H. Jia1, Q. Pei1,2, C.T. Sullivan1, D.C. Cowper Ripley1, S.S. Wu1,2, W.B. Vogel1,3, X. Wang1, J. Hale Gallardo1, B.E. Bates4
1. Center of Innovation on Disability and Rehabilitation Research, North Florida/South Georgia Veterans Health System, U.S. Department of Veterans Affairs, Gainesville, FL USA; 2. Department of Biostatistics, University of Florida, Gainesville, FL, USA; 3. College of Medicine, University of Florida, Gainesville, FL, USA; 4. Aleda E. Lutz VA Medical Center, Saginaw, MI, USA. Corresponding author: Huanguang Jia, PhD, Center of Innovation on Disability and Rehabilitation Research (151b), North Florida/South Georgia Veterans Health System, U.S. Department of Veterans Affairs, Gainesville, FL 32608, E-mail: Huanguang.Jia@va.gov, Fax: 352-271-4540, Phone: 352-376-1611 ext. 4926
Jour Nursing Home Res 2017;3:103-109
Published online Octobre 10, 2017, http://dx.doi.org/10.14283/jnhrs.2017.16
Abstract
Background: Department of Veterans Affairs (VA) community living centers (CLCs) and community nursing homes (CNHs) are the two major sources of institutional postacute care for Veterans with stroke. However, information about Veterans’ functional outcomes in these facilities is limited. Objectives: This study was to evaluate the activities of daily living (ADL) performances between Veterans at CLCs and Veterans at VA-contracted CNHs by comparing the change in ADL scores between baseline and various follow-up time points. Design: This is a retrospective, observational study. Setting: The study included all Veterans diagnosed with stroke, admitted to CLCs or VA-contracted CNHs during the study period, and had at least 2 ADL assessments completed post-admission. Measurements: ADL change score was the ADL scale sum score difference between the baseline and 3-month, 6-month, 9-month and 12-month follow-up time points. Statistical Analysis: Generalized linear mixed model with repeated ADL change scores were fitted to assess the effects of time-dependent facility type adjusting for propensity score, rehabilitation utilization, and regional districts. Results: Our pared comparison results showed that CLC (vs. CNH) Veterans had significantly better ADL performance at 3 month, but significantly worse ADL performance at 9 month and 12 month. Our risk-adjusted longitudinal analysis results demonstrated that at the 12-month follow-up CLC Veterans had developed better ADL performance (Coefficient±SD: -0.71±0.18, p<0.001) than the CNH Veterans. Conclusions: Significant differences in the changes of ADL score within the 12-month follow-up time were observed between the CLC Veterans and CNH Veterans. These longitudinal analytical findings suggest that the CLC Veterans experienced more positive changes in their ADL score compared with their counterpart CNH Veterans, even after adjusting for potential risk factors. As CNHs are more likely to provide longer term care of older Veterans, further investigation is warranted to compare other related outcomes between the two types of facilities.
Key words: Physical function, independent living, stroke, quality and outcomes.
Introduction
Within the U.S. Department of Veteran Affairs’ (VA) healthcare system, approximately 6,000 Veterans receive acute ischemic stroke care annually (1). About one-half of stroke survivors live with moderate to severe impairments (2), and these individuals need rehabilitation care to enhance their functional recovery, regain skills for activities of daily living, and increase strength, flexibility, and endurance (3).
VA community living centers (CLCs, formerly known as VA nursing homes) and community nursing homes (CNHs) are the two major sources of postacute care for Veterans with stroke. Within the VA healthcare system, there are 133 CLCs serving approximately 49,000 Veteran residents annually (4). Additionally, the VA also refers Veterans to CNHs for postacute care. This referral is under a per diem contractual agreement between local VA Medical Centers (VAMC) and local CNHs. Each year, the VA contracts with over 2,500 CNHs (5). Veteran placement in a CLC or CNH is based upon an individual needs assessment for nursing home care. This assessment is conducted by a local VAMC interdisciplinary professional team typically including a clinical nurse, social worker, and rehabilitation therapist. The team members identify each patient’s clinical needs, determine patient placement, and decide on the duration of nursing home stay (6). Veteran CNH placement is based upon local CLC bed availability, patient long-term care needs, priority for VA healthcare (e.g., service connected disabilities status, level of disability, and income), and patient preferences (e.g., proximity to Veterans’ home or family) (7). VA Handbook 1143.2, VA Community Nursing Home Oversight Procedures, outlines the per diem program and specific requirements for a CNH qualifying for a contract (8). All VA-contracted facilities are certified by U.S. national Medicare and/or Medicaid programs.
In 2004, the U.S. General Accountability Office reported that the VA lacked a systematic mechanism to evaluate the quality of care for the Veterans at CNHs (8). Several studies have evaluated the quality of care for Veteran residents at CLC and/or CNHs. Johnson et al previously reported that the CNHs with a VA contract differed from the CNHs without a VA contract: the former was more likely to be larger in certified bed numbers and for-profit; less likely to be hospital-based and to meet the minimum recommended nursing staffing; and had more residents enterally tube fed, newly catheterized, mobility restrained, and developing new pressure ulcers (9). In a recent utilization study on rehabilitation therapy and restorative nursing care, we found that CLC Veterans with stroke had fewer weekly days for rehabilitation therapy, but they had significantly more days for restorative nursing care than their counterparts at VA-contracted CNHs (10). However, information about Veterans’ functional outcomes in these facilities remains limited. For example, what are the differences in physical function outcomes between Veteran residents in CLCs versus their counterparts in CNHs? This study was to evaluate the activities of daily living (ADL) performances between Veterans at CLCs and Veterans at VA-contracted CNHs by comparing the change in ADL scores between baseline and various follow-up time points. We hypothesized that CLC Veterans have improved ADL performances than their CNH counterparts during their stay in the nursing homes.
Methods
Study Sample
This retrospective observational study included all Veterans who (1) were admitted to CLCs or VA-contracted CNHs from January 1, 2006 through December 31, 2009, (2) had stroke as a primary medical diagnosis at nursing home admission, and (3) received at least two ADL assessments: one at baseline or admission and one post-baseline. All eligible Veterans were followed for a maximum of 12 months post-admission. This study was approved by our local Institutional Review Board and VA Research and Development Committee.
Data Source
Two primary databases included the VA Minimum Dataset (MDS 2.0) for CLC information and Centers for Medicare and Medicaid Services (CMS) MDS 2.0 for CNH information. The MDS is the standardized clinical assessment tool (11). All CLCs and VA-contracted CNHs are federally mandated to conduct a resident MDS assessment at admission, after a significant change in health status, quarterly, annually, and at discharge, regardless of payment source (12). Furthermore, we also linked the CLC and CNH MDS data with VA and Medicare inpatient and outpatient data files to obtain Veterans’ relevant sociodemographic and clinical information provided inside and outside of the VA healthcare system. The Medicare Nursing Home Compare file and VA facility data were used to obtain the facility characteristic information. Details about the data sources and multiple source data linkage are published elsewhere (10).
Dependent Variable
ADL change score referred to the difference between baseline and 3-month, 6-month, 9-month and 12-month ADL scale sum score. The ADL scale was comprised of 7 MDS ADL self-performance items: bed mobility, transfer, locomotion, dressing, eating, toilet use, and personal hygiene. Each item has a 5-point rating scale ranging from “0” for independent to “4” for totally dependent. The total ADL score ranged from 0 to 28, with lower values representing higher functional status (13). This scale had a high alpha internal consistency of 0.94 (14), was validated against the Functional Independence Measure (15) and Cognitive Scale (16), and was reported to be more sensitive to ADL performances changes over time than other major MDS ADL scales (i.e., MDS ADL Short Form and MDS ADL Hierarchy) (14, 16).
During our data process, we encountered 11,196 (23.7% for CNHs and 76.3% for CLCs) observations or items with a value of “8” for “activity did not occur”. In such cases, previous studies recoded “8” to “4” (for totally dependent) with a rational that the unobservable ADL performances were due to resident inability to perform the task (17, 18). To test this assumption, we compared the average item rating values between the observations with and without a value of “8”. Our comparison showed that “8” was related to “4”, meaning when an ADL item was rated as “8”, other ADL items were most likely rated as “4” for the same Veteran. Therefore, we also recoded “8” to “4” in this study.
Independent Variable
Facility Type (CLC or CNH) specified where the Veterans resided during the study time period.
Covariates
(1) District: We adopted the VA’s regional framework grouping the CLCs and CNHs into 5 districts: North Atlantic, Southeast, Midwest, Continental, and Pacific District (19). (2) Propensity Score (PS) was used in this study as a covariate adjustment. The PS was estimated using 14 baseline facility and Veteran sociodemographic and clinical characteristics variables presented in Table 1. PS covariate method is used to balance the distribution of observed baseline covariates between CLC Veterans and CNH Veterans (20). Alternatively, we also tested the PS stratification method, but we could not use the stratification approach mainly due to unbalanced sample sizes for several quartiles (e.g., quartile 2: CLC n=3,618 vs. CNH n=15; quartile 5: CLC n=126 vs. CNH n=3,509). (3) Rehabilitation Therapy Days, (4) Restorative Nursing Care Days and (5) Depression Treatment Days referred to average weekly utilization days for these services during Veterans’ CLC or CNH stays. The VA and CMS MDS recorded the number of days for each specific type of the rehabilitation therapy, restorative nursing care and psychotherapy provided to a resident for ≥15 minutes per day in the 7 days prior to an assessment date. More details about calculating the rehabilitation therapy days and restorative nursing days are published elsewhere (10). Depression treatment days were the average weekly days for Veteran psychotherapy and antidepressant use.
Statistical Analysis
SAS version 9.4 (SAS Institute, Cary, NC) was used for all analyses. First, descriptive statistics were obtained on all the variables. Statistical inference was performed to compare the variables between the CLCs and CNHs. Second, the correlation coefficient was used to assess multicollinearity among all covariates. Consequently, we removed the patient rural/urban resident variable from our final analyses due to its strong positive correlation (r>0.5) between facility rural/urban status and rehabilitation therapy days and restorative care days. Third, the PS was estimated using backward stepwise logistic regression to regress the Facility Type variable on the facility and resident characteristic variables described in Table 1. Finally, generalized linear mixed model with repeated ADL change scores were fitted to assess the effects of time-dependent facility type adjusting for propensity score, rehabilitation utilization, and regional districts.
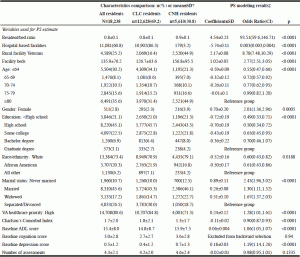
†All variables were compared between CLC group and CNH group with Chi-squared or Fisher’s exact test on discrete variables and ANOVA test on continuous variables. All comparisons were significant at p<0.001; ‡Results from logistic regression with facility type as dependent variable. The PS indicates the probability of Veterans’ CNH placement predicted by the baseline characteristic variables; SD=standard deviation, CLC=community livings center, CNH=community nursing home, CI=confidence interval, ADL=activities of daily living
Results
This study comprised 18,238 Veterans (69.2% from CLCs and 30.8% from CNHs) at 2,479 nursing homes (5.4% for CLCs and 94.6% for CNHs) during the study time period.
Table 1 shows the CLC-CNH comparison of the 14 variables used in our PS model. First, the CNHs were larger in average beds and resident/beds ratio, with more residents in rural facilities compared with the CLCs. Second, the CNH Veterans were more likely to be older, male, more educated, white, married or widowed, and have a lower VA healthcare priority compared with the CLC Veterans. Furthermore, the CNH Veterans had less burdens of comorbidity measured by the modified Charlson’s Comorbidity Index (21), worse baseline ADL and mental health performances, and more MDS follow-up assessments. All these differences were significant (p<0.001), except the baseline cognition score that was not significant (p=0.94) and excluded from the backward selection in the logistic regression.
Table 2 compares the CLC-CNH geographic distribution of Veterans and their utilization of rehabilitation therapy and restorative nursing care. CNHs differed significantly (p<0.001) from the CLCs geographically and in Veterans’ rehabilitation utilization. Specifically, the proportion of CNH Veterans in the Midwest Region was 10.8% less than the CLC Veterans in the same region. Compared with the CLC Veterans, the CNH Veterans had more average weekly rehabilitation therapy days (4.9±4.7 vs. 3.7±3.7) and depression treatment days (5.4±4.9 vs. 4.7±4.6); but they had fewer average restorative nursing care days (1.8±4.4 vs. 3.2±7.0).
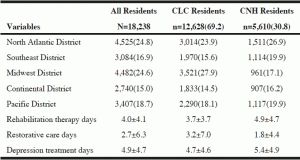
Table 2
CLC-CNH comparison of regional distribution of Veterans and rehabilitation utilization: n(%) or mean±SD†
†All variables were compared between Community Living Centers (CLCs) and Community Nursing Homes (CNHs) with Chi-squared or Fisher’s exact test on discrete variables and ANOVA test on continuous variables. All comparisons were significant at p<0.001.
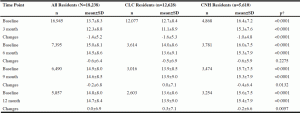
Table 3 presents Veterans’ average ADL scores and ADL change scores at different follow-up time points: 3-month, 6-month, 9-month, and 12-month. Lower ADL score represents better ADL performance. Compared with the CNH Veterans, the CLC Veterans had significantly better ADL performances at baseline (12.7±8.4 vs. 16.4±7.2, p<0.001) and more ADL change score reduction (-1.6±5.3 vs. -1.0±4.8, p<0.001) or better ADL performances at 3 month. No significant difference in the 6 month ADL change scores was observed between the two cohorts. However, the CNH Veterans showed more ADL change score reduction than the CLC Veterans at 9-month (-0.4±6.4 vs. 0.0±7.1, p<0.013) and at 12-month (-0.2±6.6 vs. 0.3±7.1, p<0.006). In addition, we also noticed that the number of CLC Veterans dropped much more than CNH Veterans at the different follow-up time points, which may be explained by the release of the healthier CLC Veterans.
†P Values were from comparisons between CLC and CNH with ANOVA test.
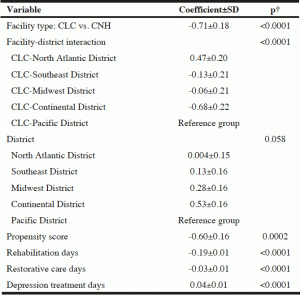
Table 4 provides the linear mixed model results. The CLC (vs. CNH) Veterans were significantly more likely to experience ADL score reduction (coefficient±SD=-0.71±0.18, p<0.001) or improved ADL performances after adjusting for the PS, effect of district and facility-district effect, and utilization factors. The mean differences in ADL change scores between the CLCs and CNHs can be further delimited by the 5 districts as follows: -0.71 for Pacific District; -0.24 (-0.71+0.47) for North Atlantic; -0.84 (-0.71+-0.13) for Southeast; -0.77 (-0.71+-0.06) for Midwest; and -1.39 (-0.71+-0.68) for Continental. Furthermore, PS (p<0.002), rehabilitation therapy days (p<0.001) and restorative care days (p<0.001) were significantly related to reduced ADL change score or improved ADL performance; but depression treatment days was significantly (p<0.001) associated with worse ADL performances over time.
†Results from linear mixed models.
Discussion
This study comprises the first comparison of 12-month ADL performances of all Veterans diagnosed with stroke at CLCs and their counterparts at VA-contracted CNHs. We hypothesized that CLC Veterans have better ADL performances than their CNH conterparts after risk adjustment.
First, without risk adjustment, we observed an ADL performance improvement for both CLC Veterans and CNH Veterans at 3-month post-admission with significantly (p<0.001) greater improvement for the CLC Veterans. Subsequently, the CNH Veterans’ ADL performance improvement continued throughout the entire follow-up time points; whereas the CLC Veterans’ ADL improved at 6-month, followed by no improvement at 9-month and deterioration at 12-month (Table 3).
Second, our longitudinal analysis of the repeated ADL change scores demonstrated that the CLC Veterans were significantly (p<0.001) more likely to have adjusted ADL performances improvement than the CNH Veterans during the study follow-up time period.
Several factors could contribute to the above unadjusted and adjusted differences in the longitudinal ADL performances change between the CLCs and CNHs. There was a significant age difference between the two study cohorts: 78.7% of the CNH Veterans were aged 65 and older as compared to 65.9% for the CLC Veterans. Although these elderly Veterans were likely to be dually eligible for VA healthcare and Medicare, the CNH Veterans could be more likely to use the dual benefit of VA and Medicare to successionally cover their continuous stay within the same facility without being discharged. However, such cases were less likely to occur for the CLC Veterans due to CLCs’ bed shortage, lack of financial motivation, and emphasis on postacute rehabilitation rather than long-term care. In this study, we were unable to calculate and compare length of Veterans’ nursing home stays due to a high missing rate in the discharge date information. Nevertheless, the number of completed assessments in Table 3 serves as a proxy for the length of stay: at 3-month, 95.6% CLC Veterans vs. 86.8% CNH Veterans completed the ADL assessments. Subsequently, there was a dramatic decline in the assessment rates for the CLC Veterans (vs. the CNH Veterans): 28.6% vs. 67.4% at 6-month; 23.9% vs. 61.9% at 9-month, and 20.6% vs. 58.0% at 12-month.
To further understand influence of age on the ADL change score, we conducted a separate analysis (not reported here) among all the Veterans who completed all the 5-time point ADL assessments (baseline, 3 month, 6 month, 9 month, and 12 month), including 1,671 or 13.2% CLC Veterans and 2,357 or 42.0% CNH Veterans. We categorized these Veterans into 3 different age groups (<65, 65-79, and >79) and compared the average ADL change scores at different follow-up time points between the two type of facilities for each age group. We found that only the “>79” age group showed a significant difference in average ADL change score between the CLCs and the CNHs at 6-month (p=0.05) and 12 month (p<0.02). These results suggested that Veterans’ aging effect can be another important effect which may cancel the ADL performance improvement associated with rehabilitation therapy.
Second, the variation in organizational characteristics between the CLC and CNH could have influenced the ADL outcome difference between the two types of facilities. For example, all the CLCs are run by the U.S. Federal Government (i.e., the Veterans Health Administration of the Department of Veterans Affairs), whereas 80% of the study CNHs were privately owned and a majority of them (65%) were for profit (22). Furthermore, compared with the CNHs, the CLCs were more likely to be hospital-based, located in urban areas, smaller in average bed numbers with lower resident-beds ratio, and provide skilled nursing restorative healthcare services (10).
Other significant factors associated with the ADL performance improvement included geographic location of the nursing homes, PS score, as well as more days for rehabilitation therapy and restorative nursing care, and fewer days for depression treatment.
We found no relevant literature to benchmark our findings above. In an early study comparing the care quality between 3,802 Veterans in 10 VA CLCs and 52,986 Veterans in 137 VA-contracted CNHs, Berlowitz et al (23) reported a worse baseline ADL functioning for the CLC Veterans than CNH Veterans. They found that the CLC Veterans were significantly (p<0.05) more likely to experience 6 month ADL functional decline than the CNH Veterans (Odds Ratio 1.6). While providing important information on the quality of care comparison between CLCs and CNHs, this study focused on only one state (New York), used data from 1997 to 1999, and limited assessment of ADL to 3 ADL items (eating, toileting and transferring).
Our study results were based upon all Veterans diagnosed with stroke residing in 133 VA CLCs and 2,346 CNHs with VA contracts from 2006 to 2009. Since our study data were from multiple sources, we were limited by availability of some important factors in the comparisons between CLCs and CNHs. For example, facility staffing level or staff hours can have a positive impact on quality of care, but these data were unavailable for the CLCs. The scope and severity is a national rating system for all certified CNHs’ deficiencies (24), however the survey was not fully implemented at VA CLCs during the study time period. Nevertheless, we linked the MDS files with VA and non-VA inpatient and outpatient data to define Veterans’ VA healthcare priority and medical comorbid conditions.
Conclusions
Our study results showed a facility difference in 12-month ADL functional outcomes between the CLCs and CNHs. Specifically, the CLC Veterans experienced more ADL improvement than their counterparts at the CNHs with a VA contract, particularly at the 3-month assessment post-index. Further investigation is warranted to compare the Veterans’ other related outcomes such cognitive functioning, mortality and rehospitalization for acute stroke between the two types of facilities. As VA continues to expand its long-term care programs to meet the increasing needs of Veterans with chronic disabilities, our findings are important for VA policy makers, clinicians, and Veterans, and will enable them make future decisions regarding the appropriate placement of Veterans in rehabilitation facilities for post-stroke care.
Acknowledgements: Support for VA/CMS data is provided by VA Information Resource Center (Project #: SDR 02-237 and 98-004).
Sources of Funding: This study was supported through the U.S. Department of Veterans Affairs Health Services Research and Development Service (VA HSR&D Grant #: IIR 11-330).
Disclosures: The opinions and contents of this paper are those of the authors and they do not represent the views of the U.S. Department of Veterans Affairs.
Ethical Standards: The authors declared no ethical issues of any type for the publication of this article.
Conflict of Interest: The authors declared no conflicts of interest of any type for the publication of this article.
References
1. Department of Veterans Affairs (VA) Stroke Quality Enhancement Research Initiative: Stroke Fact Sheet. Indianapolis, IN; July 2014
2. National Stroke Association (NSA). Rehabilitation therapy after stroke. Available at http://www.Stroke.Org/we-can-help/stroke-survivors/just-experienced-stroke/rehab. Accessed July 20, 2015
3. Duncan PW, Horner RD, Reker DM, et al. Adherence to postacute rehabilitation guidelines is associated with functional recovery in stroke. Stroke. 2002;33:167-177
4. Hojlo C. Congressional Field Hearing: Statement Before the Senate Committee on Veterans Affairs on VA Community Living Centers and State Veterans Home Clinical and Survey. Washington DC. 2008
5. VA Office of Public Affairs Media Relations. Fact sheet: VA long-term care, Washington, DC; January 2005
6. U.S. General Accountability Office (GAO). VA Long-Lerm Care: Oversight of Nursing Home Program Impeded by Data Gaps – GAO-05-65. Washington, DC. 2005
7. North Florida/South Georgia Veterans Health System. Change 2 to Appendix E, Memorandum No. 11-17: Community Nursing Home, Placement, and Follow-up. Gainesville, FL. 2005.
8. GAO. VA Long-Term Care: Oversight of Community Nursing Home Needs Strengthening – GAO-01-768. Washington, DC.2005
9. Johnson CE, Weech-Maldonado R, Huanguang J, Reker D, Buchanan R, Laberge A. Characteristics of community nursing homes serving per diem veterans, 1999 to 2002. Med Care Res Rev. 2007;64:673-690
10. Jia H, Pei Q, Sullivan CT, et al. Poststroke rehabilitation and restorative care utilization: A comparison between va community living centers and VA-contracted community nursing homes. Med Care. 2016;54:235-242
11. Centers for Medicare and Medicaid Services (CMS). Long term care minimum data set (MDS). Available at http://www.Cms.Gov/research-statistics-data-and-systems/files-for-order/identifiabledatafiles/longtermcareminimumdatasetmds.Html. Accessed December 12, 2014.
12. Morris JN, Moore T, Jones R, Mor V, Angelelli J, Berg K. CMS Report No. 500-59-0062/T.O. No. 4. Washsington, DC. 2002
13. Morris JN, Fries BE, Morris SA. Scaling ADLs within the MDS. J Gerontol A Biol Sci Med Sci. 1999;54:M546-553
14. Morris JN, Fries BE, Morris SA. Scaling ADLs within the MDS. J Gerontol. 1999;54:M546-553
15. Williams BC, Li Y, Fries BE, Warren RL. Predicting patient scores between the functional independence measure and the minimum data set: Development and performance of a FIM-MDS «crosswalk». Arch Phys Med Rehabil. 1997;78:48-54
16. Carpenter GI, Hastie CL, Morris JN, Fries BE, Ankri J. Measuring change in activities of daily living in nursing home residents with moderate to severe cognitive impairment. BMC Geriat. 2006;6:7
17. Buchanan JL, Andres PL, Haley SM, Paddock SM, Zaslavsky AM. An assessment tool translation study. Health Care Finan Rev. 2003;24:45-60
18. Jette AM, Haley SM, Ni P. Comparison of functional status tools used in post-acute care. Health care Finan Rev. 2003;24:13-24
19. VA. VA announces single regional framework under MyVA initiative. Available at http://www.Blogs.Va.Gov/vantage/16786/va-announces-single-regional-framework-under-myva-initiative/. Accessed July 20, 2015.
20. Austin PC, Grootendorst P, Anderson GM. A comparison of the ability of different propensity score models to balance measured variables between treated and untreated subjects: A monte carlo study. Stat Med. 2007;26:734-753
21. D’Hoore W, Sicotte C, Tilquin C. Risk adjustment in outcome assessment: The Charlson comorbidity index. Methods Inf Med. 1993;32:382-387
22. Jia H, Pei Q, Sullivan CT, et al. Regional variation in post-stroke multidisciplinary rehabilitation care among veteran residents in community nursing homes. J Multidisciplinary Healthcare. 2017;10:75-85
23. Berlowitz DR, Rosen AK, Wang F, Tsilimingras D, Tariot PN, Engelhardt J. Purchasing or providing nursing home care: Can quality of care data provide guidance. J Am Geriatr Soc. 2005;53:603-608
24. CMS. Nursing home data compendium 2013 edition. Available at http://www.Cms.Gov/medicare/provider-enrollment-and-certification/certificationandcomplianc/downloads/nursinghomedatacompendium_508.Pdf. Accessed December 12, 2014.