D.A. Harris1,2, R. Youssef2*, K.D. Pelland2, N. Silva-Odom2, A.J. DaCunha2, L. McNicoll2,3
1. School of Public Health, Brown University, Providence, RI, USA; 2. Healthcentric Advisors Healthcentric Advisors, Providence, RI, USA, Providence, RI, USA; 3. Alpert School of Medicine, Brown University, Providence, RI, USA.
Corresponding author: Rouba Youssef, PhD, Healthcentric Advisors, T: 401.528.3276, 235 Promenade Street, Providence, Rhode Island, Email: ryoussef@healthcentricadvisors.org
Jour Nursing Home Res 2017;3:110-115
Published online Octobre 11, 2017, http://dx.doi.org/10.14283/jnhrs.2017.17
Abstract
Background: Antipsychotic medications (APMs) have been used to treat mood and behavior dysregulation associated with dementia. However, APMs are associated with several adverse health outcomes. Federal initiatives have successfully reduced the use of APMs in nursing homes nationally; however, from 2014 to 2017, the use of APMs in Rhode Island (RI) has increased. Objective: Delineate resident, facility and community characteristics associated with APM use in RI. Design: Cross-sectional. Setting: RI, USA. Participants: RI nursing homes (N=84). Measurements: Data for RI nursing homes were obtained from the Certification and Survey Provider Enhanced Reporting (CASPER) system. The main dependent variable was a facility’s APM use. Resident, facility and community characteristics were included in the analysis. Logit-binomial regression identified which independent variables were associated with APM prevalence. Results: APM use was at an average of 18.8% (SD: 13.0%) for residents in RI’s nursing homes. After adjustment for confounding variables, the use of antianxiety and antidepressant medications, psychiatric diagnoses, and behavioral symptoms were positively associated with APM use. Dementia and behavioral care plans were associated with lower APM use (β = -1.38 [95%CI= -2.21, -0.55]; β = -0.59 [95%CI= -0.86, -0.32], respectively). Compared to non-profit facilities, for-profit facilities had greater use of APMs (β = 0.81 [95%CI= 0.39, 1.24]). Compared to nursing homes in low-income communities, homes in middle- and high-income communities were associated with less use of APMs (β = -0.67 [95%CI= -1.30, -0.25]; β = -0.75 [95%CI= -1.30, -0.20], respectively). Conclusions: Findings assist quality improvement by identifying which nursing home characteristics are associated with APM use.
Key words: Antipsychotic medications, nursing homes, Rhode Island, quality improvement.
Introduction
Nursing homes are among the most regulated institutions in the United States. Federal legislation overseeing nursing home quality dates to the Nursing Home Reform Act (NHRA) of 1987, which requires nursing homes to meet several quality benchmarks, such as 24-hour access to nursing staff, strict nurse to patient ratios, and the surveillance of psychoactive medications (1). Importantly, the law ensures that nursing home residents have freedom from inappropriate drug use and chemical restraints (1, 2).
The Food and Drug Administration (FDA) approves antipsychotic medications (APMs) to treat schizophrenia and bipolar disorder (3). However, due to their sedative effects, APMs have been inappropriately prescribed to treat behavioral and mood dysregulation associated with dementia (4). Several studies have demonstrated associations between APMs and morbidity and mortality among patients with dementia (5).One study reported that patients with dementia taking an APM, haloperidol, had 3.8% higher mortality over 180 days of follow-up compared to nonusers (6). Additional studies have replicated these findings in this population (7). Amid rising concerns about the use of APMs among older adults, the FDA issued “black box” warnings and cautioned against inappropriate use in 2005. Other national organizations and federal agencies have implemented guidelines and quality improvement (QI) activities to counteract inappropriate use. For example, the American Geriatrics Society (AGS) Beers Criteria explicitly discourage prescribing of APMs to treat behavioral problems and in 2012, the Centers for Medicare & Medicaid Services (CMS) established the National Partnership to Improve Dementia Care in Nursing Homes, which aims to reduce APM use in nursing homes through active surveillance and public reporting (8).
In 2012, excluding nursing home residents with schizophrenia, Tourette’s, Huntington’s, Manic Depression (Bipolar disorder), hallucinations, and delusions, 23.8% of nursing home residents were receiving an antipsychotic (9).In 2016, excluding residents with schizophrenia, Tourette’s, and Huntington’s, the national percentage of nursing home residents receiving an antipsychotic medication decreased to 16.0% (10, 11). Despite the national decrease, variation exists across states. For example, from 2013 to 2014, the prevalence of RI’s nursing home resident population receiving an APM decreased from 20.3% to 16.9%, but in late 2016, the use of APMs increased to 17.6% (10).
Previous research identified associations between facility and resident characteristics and APM use (12). In a recent review, several facility and resident factors were associated with greater APM use (e.g., smaller facility size, lower staff to patient ratios, greater percentage of residents with Medicaid coverage, independent ownership type) (2). Additionally, other studies have found that behavioral problems are strongly associated with the prescription of APMs (13, 14). In a sample of Australian nursing home residents, agitation and challenging behaviors were among the strongest factors associated with nursing home residents receiving APMs. Similar findings have been reported in the United States (13).
To our knowledge, no study has focused on a sample of RI nursing homes. Due to the risks of APMs and RI’s increasing prevalence, it is imperative to delineate the facility and resident characteristics associated with APM use. Our findings will inform and tailor future QI initiatives.
Methods
Data Source
The present study used data for 84 certified nursing homes in RI, surveyed by RI state surveyors in 2016 through to March 2017. Skilled state surveyors visit all Medicare- and Medicaid-certified nursing homes annually to collect data on a variety of facility and aggregated resident measures (12, 15). Through Healthcentric Advisors, the CMS Medicare Quality Innovation Network-Quality Improvement Organization (QIN-QIO) for New England, data were obtained from the Certification and Survey Provider Enhanced Reporting (CASPER) system. All data are self-reported and represent point prevalences collected on the state survey date.
Dependent Variable
The use of APMs at the facility was the main dependent variable. APM use was calculated by dividing the total number of residents receiving an APM by the total number of residents living in the nursing home at the time of the survey. Surveyors were provided a list of APMs and worked directly with each director of nursing to identify residents taking an APM (12).
Resident Variables
The CASPER database collects resident data, aggregated to the facility, on medication use, psychiatric diagnoses, developmental disabilities, and behavioral symptoms. To obtain facility prevalence for each medication category, the number of residents receiving an antianxiety, antidepressant, or sedative-hypnotic medication was divided by the total number of residents in the facility (12, 16). Due to the low prevalence of sedative-hypnotic medications, we categorized the prevalence of residents receiving a sedative-hypnotic into two levels: 1) no residents taking a sedative hypnotic and 2) at least one resident taking a sedative-hypnotic. The number of residents with a diagnosis of schizophrenia, schizoaffective disorder, schizophreniform disorder, delusional disorder, anxiety disorder, and/or psychotic mood disorder (including bipolar disorder, psychotic depression, acute psychosis, brief reactive psychosis, and atypical psychosis) was divided by the total number of residents in the facility to obtain the prevalence of psychiatric diagnoses. Included as separate measures were the numbers of residents with documented symptoms of depression, a dementia diagnosis or intellectual disability. As with the previous variables, we divided the total number of residents with symptoms of depression, dementia, or intellectual disability by the total number of residents in the facility to obtain a prevalence for each. Due to the low prevalence of residents with intellectual disabilities across nursing homes, we categorized prevalence of residents with an intellectual disability into two levels: 1) no residents with an intellectual disability and 2) at least one resident with an intellectual disability. In addition, the prevalence of behavioral problems (e.g., wandering, verbally abusive, physically abusive, socially inappropriate and disruptive, and resistant to care) was included as a potential confounder (12, 16). Last, among the residents with these behavior problems, the prevalence of these residents on a behavioral care plan was also included.
Facility Variables
To identify facility factors associated with APM use, we included several facility characteristics in the analysis. Facility variables included the facility size (total number of beds), occupancy at the time of the state survey, ownership (for-profit or non-profit), staffing (numbers of full-time equivalent registered nurses [RNs] and certified nursing assistants [CNAs]), the percent of residents with Medicare or Medicaid, and a binary variable of the presence of an Alzheimer’s unit or other special care unit. Occupancy was calculated by dividing the total number of residents by the total number of beds in the facility. To account for differences in facility size, which may influence RN and CNA staffing, we divided the number of full time equivalent RNs and CNAs by the total number of beds in the facility.
Community variables
We used 2014 United States Census estimates to identify the median household income for each nursing home’s ZIP Code. After examining the distribution of median household income in RI, we stratified the variable into three levels: low income (a median income less than $47,700), middle income ($47,700 to $71,500), and high income (greater than $71,500).
Data Analysis
Descriptive analyses were conducted to examine the distribution of resident, facility, and community characteristics (Table 1). We then used correlations to test for multicolinearity between the independent and dependent variables. Finally, due to the proportional nature of the dependent variable, we used a logit-binomial regression to test for unadjusted and adjusted associations between the independent and dependent variables. Robust standard errors were used to protect against potential model misspecification. Due to the small number of facilities in RI, we first analyzed the resident (Table 2) and facility and community characteristics (Table 3) separately. Table 4 reports results from a final model including all of the resident, facility and community characteristics included together (12). One unit increases in the independent variable represent β changes in the log-odds in the dependent variable. All statistical analyses were performed in STATA version 14 (17).

Table 1
Resident, Facility, and Community Characteristics of Rhode Island Nursing Homes in 2016 and 2017 (N=84)
Notes: Registered nurse (RN); Certified nursing assistant (CNA); Full-time equivalent (FTE); 1. Psychiatric diagnoses included schizophrenia, schizoaffective disorder, schizophreniform disorder, delusional disorder, anxiety disorder, and psychotic mood disorder (including bipolar disorder, psychotic depression, acute psychosis, brief reactive psychosis, and atypical psychosis) and excluded diagnoses of depression and dementia. 2. The number of residents with a behavioral care plan is of the sample of residents with behavioral symptoms; 3. Median household income for the ZIP Code in which the nursing home was divided into three levels.
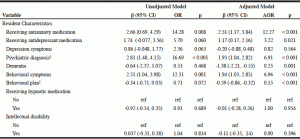
Table 2
Unadjusted and adjusted β and odds ratio estimates across resident characteristics and antipsychotic medication use (N = 84)
Notes: Confidence interval (CI); odds ratio (OR); AOR (adjusted odds ratio); 1. Psychiatric diagnoses included schizophrenia, schizoaffective disorder, schizophreniform disorder, delusional disorder, anxiety disorder, and psychotic mood disorder (including bipolar disorder, psychotic depression, acute psychosis, brief reactive psychosis, and atypical psychosis) and excluded diagnoses of depression and dementia; 2. The number of residents with a behavioral care plan is of the sample of residents with behavioral healthcare needs (direct wording from CMS-672 form)
Results
A mean of 18.8% (SD: 13.0%) of residents in our statewide sample of nursing homes were receiving an APM. Notably, 60.3% (SD: 16.2%) of nursing home residents on average were receiving an antidepressant medication. A mean of 52.2% (SD: 14.2%) of residents in RI nursing homes had a dementia diagnosis, a mean of 42.2% (SD: 4.3%) had depression symptoms, and a mean of 37.1% (SD: 15.6%) had a psychiatric diagnosis other than dementia or depression. Regarding facility characteristics, the mean number of beds across RI nursing homes was 103.8 (SD: 51.1). A majority (80.9%) of nursing homes in RI were for-profit institutions and slightly more than half (51.2%) were part of a nursing home chain. See Table 1 for a descriptive analysis of the nursing homes in RI.
Several resident characteristics were significantly associated with facility APM use (Table 2). The use of antianxiety (β = 2.56, 95%CI [1.24, 3.89]) and antidepressant medications (β = 1.13, 95%CI [0.11, 2.17]) were both associated with a greater use of APMs after adjusting for medication use, psychiatric diagnoses, behavioral symptoms, and behavioral care plans. Additionally, psychiatric diagnoses (β = 2.01, 95%CI [1.14, 2.89]) and behavioral problems (β = 1.98, 95%CI [1.07, 2.89]) were associated with greater APM use after adjustment. The percent of residents with behavioral care plans among residents with behavioral problems was significantly associated with lower APM use after adjustment (β = -0.59, 95%CI [-0.85, -0.32]). Last, dementia was found to be inversely associated with APM use in the adjusted model (β = -1.40, 95%CI [-2.24, -0.55]).
Before adjustment for the other facility characteristics, the proportion of residents paying with Medicare was associated with significantly less APM use compared with residents whose stay was not covered by Medicare (β = -4.37, 95%CI [-7.95, -0.78]). Second, a larger proportion of full-time equivalent registered nurses was also associated with significantly less APM use before adjustment (β = -5.58, 95%CI [-9.75, -1.41]). However, after adjustment, only for-profit ownership (β = 0.81, 95%CI [0.39, 1.24]) and median household income at the ZIP Code level remained significantly associated with APMs. Nursing homes in the middle- (β = -0.67, 95%CI [-1.30, -0.25]) and high-income (β= -0.75, 95%CI [-1.30, -0.20]) communities were significantly less likely to use APMs compared to nursing homes in the low- income community in the adjusted model (Table 3).
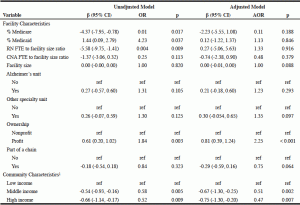
Table 3
Unadjusted and adjusted β and odds ratio estimates of association across facility and community characteristics and facility antipsychotic medication use (N = 84)
Notes: Confidence interval (CI); odds ratio (OR); AOR (adjusted odds ratio); FTE (full time equivalent); RN (registered nurse); CNA (certified nursing assistant); 1. Median household income for the ZIP Code in which the nursing home was located, divided into three levels.
When all resident, facility and community characteristics were included in one regression model, several characteristics remained statistically significant (Table 4). After controlling for all of the resident, facility and community characteristics, for-profit facilities remained more likely to use antipsychotic medication compared to non-profit facilities (β= 0.45, 95%CI [0.02, 0.88]). Compared to facilities in a low-income community, facilities in middle-income community were significantly less likely to use antipsychotic medications (β= -0.41, 95%CI [-0.76, -0.06]). The prevalence of residents with dementia was also significantly associated with less antipsychotic medication use while holding all other resident, facility and community characteristics equal (β= -1.10, 95%CI [-1.95, -0.25]).
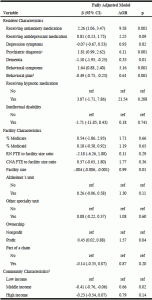
Table 4
Adjusted β and odds ratio estimates of association across all resident, facility and community characteristics and antipsychotic medication use (N = 84)
Notes: Confidence interval (CI); AOR (adjusted odds ratio); FTE (full time equivalent); RN (registered nurse); CNA (certified nursing assistant); 1. Psychiatric diagnoses included schizophrenia, schizoaffective disorder, schizophreniform disorder, delusional disorder, anxiety disorder, and psychotic mood disorder (including bipolar disorder, psychotic depression, acute psychosis, brief reactive psychosis, and atypical psychosis) and excluded diagnoses of depression and dementia; 2. The number of residents with a behavioral care plan is of the sample of residents with behavioral healthcare needs (direct wording from CMS-672 form); 3. Median household income for the ZIP Code in which the nursing home was, divided into three levels
Discussion
This study has several findings. First, among the resident characteristics, antianxiety medications, antidepressant medications, psychiatric diagnoses, and behavioral problems were significantly associated with greater APM use in the unadjusted and adjusted models. Second, use of behavioral care plans among residents with behavioral problems was associated with less APM use in after adjustment for other resident characteristics (i.e., medication use, behavioral problems, and psychiatric diagnoses). Last, the proportion of residents with a dementia diagnosis was significantly associated with less APM use in the adjusted model. Though some facility characteristics were associated with APM use in the unadjusted results, only for-profit ownership and middle- and high- median household income remained significant after adjustment.
Replicating previous research, we found that higher prevalences of antianxiety medications and antidepressants were associated with more APMs (16). This may lend insight into the prescribing culture of a nursing home facility. Interventions successfully reducing APM use have targeted physicians and pharmacists and provided tailored educational resources (16). Tailoring QI initiatives to prescribers that also consider resident factors may lead to successful reduction efforts.
As in other studies, behavioral problems and psychiatric diagnoses are among the strongest factors associated with APMs in our sample (12, 14). Despite practice guidelines advocating for the preliminary use of psychosocial interventions to treat behavioral problems, pharmaceutical interventions often come first (18). In addition to targeting prescribing practices, QI efforts should build the non-pharmacologic skill base of nursing home care workers in addressing psychiatric and behavior problems. For example, compared to control homes, one study showed a 23% reduction in APM use after an intervention implementing both physician education and skill building among direct care staff (e.g., role play, case study examples, and problem solving meetings) (19, 20).
Interestingly, unlike previous findings, our results revealed that dementia was inversely related to APM use (12, 14, 21). This may be a successful reflection of the CMS partnership aiming to reduce APM use among nursing home residents with dementia. Currently, the CMS publically reported quality measure for APMs excludes residents with Huntington’s, Tourette’s, or schizophrenia, as those diagnoses may warrant the prescription of APMs (11). Therefore, increases in APM use may not solely be among residents with dementia, but rather among residents with behavioral symptoms and psychiatric diagnoses that may be unassociated with dementia. Future research may consider examining changes in subpopulations of nursing home residents who are more likely to receive APMs as a result of federal initiatives.
Interestingly, we found that nursing home location had an impact on APM use (2). To our knowledge, our study is the first to find that compared to nursing homes in lower-income communities, nursing homes in middle- and higher-income communities use less APMs. Last, unlike previous studies, we did not find any associations between staffing variables and APM use after adjustment (2, 12). This result may be due to, in part, a small sample size. Future research may explore what community factors may explain the association between median household income and a nursing home’s APM use (2).
The present study is limited by its small sample size. This reduces our ability to generalize to other states and include a larger number of independent variables in our analysis. Additionally, the CASPER data source uses aggregated facility-level measures, which may obscure more nuanced multi-level relationships between resident, facility and community characteristics. However, this study’s primary strength is its ability to describe RI’s nursing home environment, aiding local QI initiatives.
Acknowledgements: The authors would like to acknowledge the early support of Melissa Miranda in this research.
Conflicts of Interest: The analyses upon which this report is based were performed under IDIQ contract number HHSM-500-2014-QIN0141, Task Order Number HHSM-500-TMA01, funded by the Centers for Medicare & Medicaid Services, an agency of the U.S. Department of Health and Humans Services. The content of this publication does not necessarily reflect the views or policies of the Department of Health and Human Services, nor does mention of trade names, commercial products, or organizations imply endorsements by the U.S. government. The authors assume full responsibility for the accuracy and completeness of the ideas presented.
References
1. Nursing Home Reform Law, in 42 U.S.C. §§1395i-3(a)-(h), 1396r(a)-(h) In. 1987.
2. Cioltan H, Alshehri S, Howe C, et al., Variation in use of antipsychotic medications in nursing homes in the United States: A systematic review. BMC Geriatr, 2017. 17(1): p. 32.
3. Levinson DR. Medicare atypical antipsychotic drug claims for elderly nursing home residents: US department of health and human services, office of inspector general. 2011.
4. Jeste DV, Blazer D, Casey D, et al. ACNP White Paper: update on use of antipsychotic drugs in elderly persons with dementia. Neuropsychopharmacology, 2008. 33(5): p. 957-70.
5. Schneider, LS, Dagerman KS, and Insel P. Risk of death with atypical antipsychotic drug treatment for dementia: meta-analysis of randomized placebo-controlled trials. JAMA, 2005. 294(15): p. 1934-43.
6. Maust DT, Kim HM, Seyfried LS, et al. Antipsychotics, other psychotropics, and the risk of death in patients with dementia: number needed to harm. JAMA Psychiatry, 2015. 72(5): p. 438-45.
7. Trifirò G, Verhamme KM, Ziere G, Caputi AP, Ch Stricker BH, Sturkenboom MC. All-cause mortality associated with atypical and typical antipsychotics in demented outpatients. Pharmacoepidemiol Drug Saf, 2007. 16(5): p. 538-44.
8. American Geriatrics Society. American Geriatrics Society 2015 Updated Beers Criteria for Potentially Inappropriate Medication Use in Older Adults. J Am Geriatr Soc, 2015. 63(11): p. 2227-46.
9. Centers for Medicare & Medicaid. Description of Antipsychotic Medication Quality Measures on Nursing Home Compare. 2012. https://www.cms.gov/Medicare/Provider-Enrollment-and-Certification/CertificationandComplianc/Downloads/AntipsychoticMedicationQM.pdf
10. Centers for Medicare & Medicaid. National Partnership to Improve Dementia Care in Nursing Homes: Antipsychotic Medication Use Data Report (March 2017), 2017. p. 1-3. https://www.nhqualitycampaign.org/files/AP_package_20170413.pdf
11. Centers for Medicare & Medicaid. MDS 3.0 Quality Measures User’s Manual (v10.0 03-25-2016). 2016. https://www.cms.gov/Medicare/Quality-Initiatives-Patient-Assessment-Instruments/NursingHomeQualityInits/Downloads/MDS-30-QM-Users-Manual-V10.pdf
12. Hughes, CM, Lapane KL, and Mor V. Influence of facility characteristics on use of antipsychotic medications in nursing homes. Med Care, 2000. 38(12): p. 1164-73.
13. Ott BR, Lapane KL, Gambassi G. Gender differences in the treatment of behavior problems in Alzheimer’s disease. SAGE Study Group. Systemic Assessment of Geriatric drug use via Epidemiology. Neurology, 2000. 54(2): p. 427-32.
14. Nishtala PS, McLachlan AJ, Bell JS, Chen TF. Determinants of antipsychotic medication use among older people living in aged care homes in Australia. Int J Geriatr Psychiatry, 2010. 25(5): p. 449-57.
15. Petrisek AC, Mor V.Hospice in nursing homes: a facility-level analysis of the distribution of hospice beneficiaries. Gerontologist, 1999. 39(3): p. 279-90.
16. Nørgaard A, Jensen-Dahm C, Gasse C, Hansen ES, Waldemar G. Psychotropic Polypharmacy in Patients with Dementia: Prevalence and Predictors. J Alzheimers Dis, 2017. 56(2): p. 707-716.
17. StataCorp. Stata Statistical Software: Release 14. 2015: College Station, TX: StataCorp LP.
18. Ruths S, Straand J, Nygaard HA, Aarsland D. Stopping antipsychotic drug therapy in demented nursing home patients: a randomized, placebo-controlled study–the Bergen District Nursing Home Study (BEDNURS). Int J Geriatr Psychiatry, 2008. 23(9): p. 889-95.
19. Meador KG, Taylor JA, Thapa PB, Fought RL, Ray WA. Predictors of antipsychotic withdrawal or dose reduction in a randomized controlled trial of provider education. J Am Geriatr Soc, 1997. 45(2): p. 207-10.
20. Richter T, Meyer G, Möhler R, Köpke S. Psychosocial interventions for reducing antipsychotic medication in care home residents. Cochrane Database Syst Rev, 2012. 12: p. CD008634.
21. Alessi-Severini S, Dahl M, Schultz J, Metge C, Raymond C. Prescribing of psychotropic medications to the elderly population of a Canadian province: a retrospective study using administrative databases. PeerJ, 2013. 1: p. e168.
