K. El Haddad1, X. Dubusc1,2, C. Cool2, F. Nourhashémi1,2, P. De Souto Barreto1,2, Y. Rolland1,2
1. Gérontopôle, Department of Internal Medicine and Geriatrics, Toulouse University Hospital, Toulouse, F-31059, France; 2. INSERM U1027, University of Toulouse III, Toulouse, France. Corresponding author: Kamal El Haddad, Institut du Vieillissement, Gérontopôle, Université Toulouse III Paul Sabatier, 37 Allées Jules Guesde, 31000 Toulouse, France, E-mail: kamal.elhaddad@hotmail.com, Tel: +33561145657; fax: +33561145640
Jour Nursing Home Res 2018;4:5-9
Published online April 25, 2018, http://dx.doi.org/10.14283/jnhrs.2018.2
Abstract
Background: Despite comparable clinical characteristics of nursing home residents, the rate of emergency department transfer is highly variable from one nursing home to another, suggesting that structural characteristic and organizational factors may influence the rate of nursing home resident’s transfer to the emergency department. Objectives: To identify structural characteristics and medical care organization of nursing homes according to the rate of emergency department transfers of nursing home residents. Design: We conducted a cross-sectional analysis using the baseline data of the IQUARE study (Impact of a QUAlity improvement initiative on nursing practices and functional decline in NH REsidents), a non-randomized controlled multicenter trial with 175 nursing homes in south-western, France. Participants: 5926 nursing home residents. Measurement: Data on nursing home structural characteristics and medical care organization were collected by questionnaires between May and July 2011. Data concerning hospital admissions and emergency department transfers during the past year were retrieved from the residents’ medical files. Results: The rate of emergency department transfer in the last 12 months was 18.9% (±11.5): 7.4%, 18.4% and 31.4% for the low, medium and high tertile groups, respectively. Compared to the low transfer group, the high transfer group had less special care unit (RRR: 0.31, 95%CI 0.19-0.83, P: 0.018). The location of the high transfer group tends to be more urban than rural when compared to the low transfer group (RRR: 0.37, 95%CI 0.14-0.99, P: 0.047). Compared to the low transfer group, the high transfer group has less pharmacy for internal use (RRR: 0.10, 95%CI 0.03-0.38, P < 0.001). Conclusion: Our results suggest that implementing special care unit and pharmacy for internal use in nursing homes may reduce the rate of nursing home residents’ transfer to the emergency department. Geographic location seems to dissuade or encourage nursing home to transfer residents to the emergency department. Long-term interventions are needed to reduce the risk of inappropriate emergency department transfers, thus the risk and cost associated with hospitalization.
Key words: Nursing home, nursing home residents, emergency department, transfer.
Introduction
Nursing home residents (NHR) constitute a highly vulnerable group of older people in terms of medical problems. They are characterized by a high level of disability and multiple chronic illnesses thus are more prone to be transferred to the emergency department (ED). Hospitalization of this vulnerable population is however an important risk factor for complications such as confusion and further functional decline (1). The balance between benefit and risk of a transfer to an emergency room is frequently questionable in NHR. Currently, more than 25% of long-stay NHR are hospitalized during a 6-month period in France (2). Respiratory symptoms, suspected infections and falls are the most common reasons for transfer (3-5). Of those reasons, some are not determined on medical grounds, meaning that NHR care does not rely on emergency expertise and could have been managed differently without a transfer from the nursing home (NH) to the ED. According to Graverholt (6-9) et al., the NH population accounts for many potentially avoidable hospitalizations, with estimates between 19-67%. Interestingly, despite comparable clinical characteristics of residents, the rate of ED transfer (EDT) is highly variable from one nursing home to another (10), suggesting that organizational factors may influence the rate of EDT. These factors may be more easily targeted by interventions than the clinical characteristics of the residents.
It has previously been reported that factors such as the incorporation of a palliative approach, documented advanced care plans (ACP) by the physician (11), higher educational levels and competences among registered nurses (RNs) (12), or the presence of more physicians and RNs onboard (13-14) are associated with lower rate of EDT. We also reported a 26.1% decrease in the emergency department transfers of resident after integrating a global intervention comprising professional support and education for nursing home staff on quality indicators (QIs) (15).
Intrinsic structural characteristics and medical care organization among NH structure that influence the rates of EDT have been poorly investigated. One recent Swedish study showed that high transfer rate from NHs to ED was associated with for-profit ownership, less experienced RNs (those with less work experience in care of older people and had less training in care of patients with dementia) and fewer updated ACP within the past year (16).
Thus the aim of this study was to identify structural characteristics and medical care organization associated with NHs with high versus low rates of EDT.
Methods
Study procedure and population
We used the baseline database of the IQUARE (Impact of a QUAlity improvement initiative on nursing practices and functional decline in NH REsidents) study, a non-randomized controlled multicenter trial with 175 NHs in south-western, France. The methods of IQUARE (trial registration number NCT01703689) have been previously described in detail (17). In brief, IQUARE tested the effects of a global intervention including professional support and education for NH’s staff on NH quality indicators, functional decline and EDT of residents (15). For this research, we used only the cross-sectional data collected at baseline.
From the 175 NHs, recruitment of at least 30 NHR per NH, (living for more than 30 days in the institution), was selected by alphabetical order to obtain a total of 6275 residents at baseline. Baseline data on hospitalization and EDT was available for 5926 NHR (94.4% of the total NHR) which constitute our sample for this study. IQUARE was approved by the ethics committee of Toulouse University Hospital and the Consultative Committee for the Treatment of Research Information on Health (CNIL: 07–438).
Data collection
The data for this study were collected between May and July 2011.
Data on NH structural characteristics, medical care organization and residents’ health were collected from an online questionnaires twice (at baseline and at 18 months post intervention).These questionnaires were completed by NH leadership staff (NH director, the coordinating physician and the coordinating nurse).
Data concerning hospital admissions and EDT were retrieved from the resident’s medical files.
Structural factors and medical care organizational factors included:
The ownership status of each NH : (private and public), number of NH beds, the availability of a special care unit (SCU), (a closed and secured unit for the management of patients with dementia and behavioral disorders), the NH’s geographic location defined by its geographic affiliation (rural/urban) using the January 2011 INSEE (National Institute of Statistics and Economic Studies) French database and the estimation of the required timing from the NH’s to the ED (minutes), the number of full-timer staff in the NH ( coordinating nurse, physical therapist, dentist or dental surgeon, dietician, sports trainer and pedicure specialist ), GPs for 100 occupied beds, paramedics for 100 occupied beds, staff personals recruited in the last 6 months per 100 beds, and the level of geriatric training of the coordinating NH physicians ( high level if the coordinating physician has a specialized geriatric diploma). The availability (yes/no) of a Pharmacy unit for internal use (PIU) within the NH to ensure the proper preparation (pillbox), administration, safety as well as the supply of the medications, a computerized medical folder, reports and assessments of resident’s falls, and an ACP were recorded, the pillbox preparation was determined according to the operator if any (city pharmacist or the NH nurse), the requisitioning of a benzodiazepine or an antipsychotic reevaluation every month by the GP was reported (yes/ no/ N/A), the easy access to a geriatric/psychiatric advice or inpatient admission to a geriatric/psychiatric floor if needed was recorded, the availability of a psychiatrist or a psychiatric nurse visit within the NH was collected (yes/ no).
Rate of hospitalization
In IQUARE, NH staff notified for the last four hospitalizations the hospital department to which patients were addressed: ED, geriatrics service, psychiatric service, or other services. The annual rate of EDT for each NH was calculated from the number of residents who were transferred in an ED (at least one EDT) during the previous 12 months divided by the total number of residents participating in the study. NHs were categorized into three different groups (tertile distribution) according to their annual rate of EDT: low, medium, or high.
Statistical analysis
We conducted a cross-sectional analysis using the baseline data of the IQUARE study. The unit of analysis was the NH.
Descriptive statistics were obtained using means (mean ± SD) or absolute numbers (%) as appropriate. Bivariate analysis were undertaken using the Chi-2 test or the Fisher’s exact test (as appropriate) or using One-way ANOVA with Bonferroni adjustment for multiple comparisons.
Variables associated with a p value <0.25 in the bivariate analysis (table 1) were included in a multinomial logistic regression that analyzed the association of the selected independent variables with NH groups (low, medium or high transfer group).
This analysis was adjusted for the average of residents’ age, comorbidities (charlson index) (18) and dependency score for each NH.
All analysis were performed with STATA (version 14.2), and p<.05 was used to indicate statistical significance.
Results
Overall, the rate of EDT in the last 12 months was 18.9 % (±11.5): 7.4%, 18.4% and 31.4% for the low, medium and high tertile groups, respectively. Differences in the rate of hospitalization between the three groups were related to the availability of a special care unit, the number of GPs for 100 occupied beds, the availability of a PUI within the NH and the reevaluation of benzodiazepine and antipsychotic prescription by the GP (table 1).
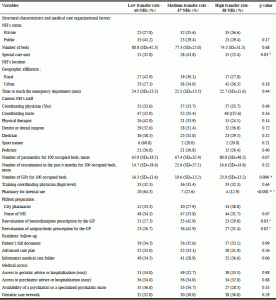
Table 1
Bivariate analysis of NHs characteristics with low, medium and high transfer rate to emergency
Notes: * significative difference between low and high group (p<0.0167); ° significative difference between medium and high group (p<0.0167); “ significative difference between low and medium group (p<0.0167); NH, Nursing Home ; GP, General Practitioner; Continuous variables : One-Way ANOVA (significances were adjusted using the Bonferroni method ; p< 0.167); Categorical variables : Chi-2 Test (significances were adjusted using the Bonferroni method ; p< 0.167)
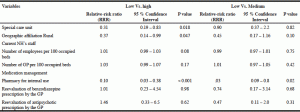
Results from the multivariate analysis are reported in the table 2. In summary, we showed that compared to the low transfer group, the high transfer group had less special care unit (RRR: 0.31, 95%CI 0.19-0.83, p: 0.018). The location of the high transfer group tended to be urban (less distant to the hospital) when compared to the low transfer group (RRR: 0.37, 95%CI 0.14-0.99, p: 0.047).
Compared to the low transfer group, the high transfer group has less pharmacy for internal use (RRR: 0.10, 95%CI 0.03-0.38, P < 0.001).
Notes: NH, Nursing Home; GP, General Practitioner; IC95%: 95% confidence interval; RRR, relative-risk ratio
Discussion
We found that NHs identified with the highest transfer rates to the ED had less SCU, were located closer to hospitals and had less PIUs than NHs with the lowest ED rates of transfer. Our research confirmed the large variation of ED rate of transfer across NHs and showed that structural characteristics and medical care organization are significant factors explaining these differences.
A higher transfer rate was observed in NH without SCU. SCU were implemented in NH to facilitate care for patients with dementia and behavioral disturbances. A previous study did not find a reduced rate of hospitalization in residents living in SCU compared to similar residents not living in a SCU (19). However, SCUs have been reported to result in better care based on higher amounts of interaction among residents, with residents more often out of their room, displaying greater mobility, fewer medications and less physical restraint (20) and potentially less hospitalization. Furthermore, volunteer and higher trained NH staff working in SCU may more often contribute to establish advanced directive for non-hospitalization. For example, a Swedish study found that registered nurses working in a low emergency transfer rate NH were better trained for care of older people with dementia compared to registered nurses working in a high emergency transfer rate NH (16).
Paradoxically, a lower transfer rate to the ED was associated with NH geographically located in a more distant rural areas compared to NH in urban areas. It is possible that safety concerns may result in lower transfer when the staff is isolated from hospital ED and when the time to organize emergency care is greater. Ease of transfer (easy access and less time to transport) to the ED in urban NHs may explain these results. This hypothesis needs further validation; if confirmed, it would suggest poorer quality management in urban NH compared to those located in rural areas. Rural NHs may also be more equipped medically knowing the deficiency of nearby hospitalized settings. These hypothesis require further investigations.
Polymedication has been reported to be an important factor associated with adverse events in NH residents (21). In our study, NHs with a low transfer rate had more pharmacy for internal use (PIU) compared to the high transfer group. This result supports the importance of medical care organization regarding prescription, proper preparation, safety as well as the supply of the medication as a relevant approach to reduce EDT. Reasons of EDT were not reported in our study but this results suggest that decreasing iatrogenic events caused by polypharmacy among NH’s resident is a relevant task to reduce EDT. According to Beuscart. et. al. (22), 24% of patients living in NHs were exposed to a prescription with high anticholinergic score. Fall, delirium, aspiration pneumonia are usual reasons of EDT and frequently relate to side effect of polymedication. The main goal of pharmacy for internal use is to improve the quality of prescription, thus reducing clinical adverse events leading to inappropriate but avoidable EDT.
The main strength of this study is the large sample size and diverse regions in which NHs were located (Urban, rural, and mountainous areas). However, our study has limitations. There is a recall bias inherent to the retrospective data collection and medical charts are not always updated which could lead to an under-estimation of EDT rate. Moreover, our data do not reveal the motives of EDT; appropriateness of the EDT was not collected. Then, the lower rate of EDT from rural NHs may also be an indicator of missed diagnosis or misevaluation of the resident’s health status requiring EDT, thus poor medical management and poor quality of care. Moreover, the time required for the transfer from urban or rural NHs to a hospital is not accurate since it does not take into account the distance and the availability of ambulance services, however these factors most likely affect the time course.
In conclusion, identifying structural and medical care organizations and optimizing them according to each resident is necessary in order to decrease inappropriate EDT (thus the risks and cost associated with hospitalization). According to Ong et. Al (23) residents transferred acutely from NH have a high mortality rate, 40% of these death occurred within the first twenty-four hours of admission. Facing and managing these acute medical cases among NH residents might overpass NH staff availability and competences and result in poor medical management and poor quality of care for other residents. Implementing organizational programs that reduced inappropriate EDT without reducing the quality of care should be an important task for NH staff.
Conflict of interest: All authors declare no conflict of interests.
Ethical standards: IQUARE was approved by the ethics committee of Toulouse University Hospital and the Consultative Committee for the Treatment of Research Information on Health (CNIL: 07–438).
References
1. Kihlgren A, Nilsson M, Skovdahl K, Palmblad B, Wimo A. Older patients awaiting emergency department treatment. Scand J Caring Sci 2004;18(2):169-176.
2. Intrator O, Castle NG, Mor V. Facility characteristics associated with hospitalization of nursing home residents: Results of a national study. Med Care 1999;37(3):228-237.
3. Ackermann RJ, Kemle KA, Vogel RL, Griffin RC Jr. Emergency department use by nursing home residents. Ann Emerg Med 1998;31(6):749-757.
4. Givens JL, Selby K, Goldfeld KS, Mitchell SL. Hospital transfers of nursing home residents with advanced dementia. J Am Geriatr Soc 2012;60(5):905-909.
5. Kihlgren A, Wimo A, Mamhidir AG. Older patients referred by community nurses to emergency departments-a descriptive cross-sectional follow-up study in a Swedish context. Scand J Caring Sci 2014;28(1):97-103.
6. Saliba D, Kington R, Buchanan J, et al. Appropriateness of the decision to transfer nursing facility residents to the hospital. J Am Geriatr Soc 2000;48(2):154-163.
7. Ouslander JG, Lamb G, Perloe M, et al. Potentially avoidable hospitalizations of nursing home residents: frequency, causes, and costs: [see editorial comments by Drs. Jean F. Wyman and William R. Hazzard, pp 760-761]. J Am Geriatr Soc 2010; 58(4):627-635.
8. Walker JD, Teare GF, Hogan DB, Lewis S, Maxwell CJ. Identifying potentially avoidable hospital admissions from Canadian long-term care facilities. Med Care 2009;47(2):250-254.
9. Grabowski DC, O’Malley AJ, Barhydt NR. The costs and potential savings associated with nursing home hospitalizations. Health Aff (Millwood) 2007;26(6):1753-1761.
10. Kirsebom M, Hedström M, Wadensten B, Pöder U. The frequency of and reasons for acute hospital transfers of older nursing home residents. Arch Gerontol Geriatr 2014;58(1):115-120.
11. Kirsebom M, Wadensten B, Hedström M. Communication and coordination during transition of older persons between nursing homes and hospital still in need of improvement. J Adv Nurs 2013;69(4):886–895.
12. Aiken LH, Sloane DM, Bruyneel L, et al. Nurse staffing and education and hospital mortality in nine European countries: A retrospective observational study. Lancet 2014;383(9931):1824-1830.
13. Lisk R, Yeong K, Nasim A, et al. Geriatrician input into nursing homes reduces emergency hospital Admissions. Arch Gerontol Geriatr 2012;55(2):331-337.
14. Konetzka RT, Spector W, Limcangco MR. Reducing hospitalizations from long-term care settings. Med Care Res Rev 2008;65(1):40-66.
15. Rolland Y, Mathieu C, Piau C, et al. Improving the Quality of Care of Long-Stay Nursing Home Residents in France. J Am Geriatr Soc 2016;64(1):193-199.
16. Kirsebom M, Hedström M, Pöder U, et al. Transfer of nursing home residents to emergency departments organizational differences between nursing homes with high vs. low transfer rates. Nurs open 2016;4(1):41-48.
17. de Souto Barreto P, Lapeyre-Mestre M, Mathieu C, et al. A multicentric individually-tailored controlled trial of education and professional support to nursing home staff: Research protocol and baseline data of the IQUARE study. J Nutr Health Aging 2013;17(2):173-178.
18. Charlson ME, Pompei P, Ales KL, MacKenzie CR. A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 1987;40(5):373-383.
19. Coleman EA, Barbaccia JC, Croughan-Minihane MS. Hospitalization rates in nursing home residents with dementia. A pilot study of the impact of a special care unit. J Am Geriatr Soc 1990;38(2):108-112.
20. McCracken AL. Special care units: meeting the needs of cognitively impaired persons. J Gerontol Nurs 1994;20(4):41-46.
21. Cool C, Cestac P, Laborde C, et al. Potentially inappropriate drug prescribing and associated factors in nursing homes. J Am Med Dir Assoc 2014;15(11):850.e1-9.
22. Beuscart JB, Dupont C, Defebvre MM, Puisieux F. Potentially inappropriate medications (PIMs) and anticholinergic levels in the elderly: a population based study in a French region. Arch Gerontol Geriatr 2014;59(3):630-635.
23. Ong AC, Sabanathan K, Potter JF, Myint PK. High mortality of older patients admitted to hospital from care homes and insight into potential interventions to reduce hospital admissions from care homes: The Norfolk experience. Arch Gerontol Geriatr 2011;53(3):316–319.