E. Watanabe1,2, M. Maeno2,3, M. Kamon2, J. Kayashita4, K. Miyamoto1, M. Kogirima2
1. Graduate School of Nutrition and Bioscience, Tokushima University, 3-18-15 Kuramoto-cho, Tokushima 770-8503, Japan; 2. Department of Food Science and Nutrition, Doshisha Women’s College of Liberal Arts, Imadegawa Teramachi, Kamigyo-ku, Kyoto 602-0893, Japan; 3. Long-term Care Health Facility Nukumorinosato, Shimogyo-ku, Kyoto 600-8876, Japan; 4. Department of Health Sciences, Prefectural University of Hiroshima, 1-1-71 Ujina-Higashi, Minami-ku, Hiroshima 734-8558, Japan. Corresponding author: Miho Kogirima, Department of Food Science and Nutrition, Doshisha Women’s College of Liberal Arts, Imadegawa Teramachi, Kamigyo-ku, Kyoto 602-0893, Japan, E-mail: mkogirim@dwc.doshisha.ac.jp, Tel & Fax: +81-75-251-4227
Jour Nursing Home Res 2018;4:10-14
Published online April 25, 2018, http://dx.doi.org/10.14283/jnhrs.2018.3
Abstract
Objectives: The elderly generally experience low occlusal force, which leads to decreased food intake. In this population, a soft diet with high protein content is necessary to avoid undernutrition. Here, we developed a novel texture-modified chicken using yogurt, with a hardness lower than 40,000 N/m2. Design: We applied a crossover design. Setting: Nursing home (long-term care health facility) in Kyoto, Japan from 12 to 24 June 2016. Participants: A total of 34 participants (mean age 89.7 years old, 82% female). Measurements: The proportions of minced chicken, yogurt, water, and potato starch in the texture-modified chicken were measured. The hardness and intake rate of teriyaki chicken using texture-modified chicken and conventional chicken thighs were also measured. Results: The amount of minced chicken, yogurt, water, and potato starch in the texture-modified chicken provided in the nursing home was 49.0 g, 16.2 g, 2.4 g, 2.4 g, respectively. The hardness was approximately 30,000 N/m2, which was lower than that of teriyaki chicken using conventional chicken thigh (> 63,000 N/m2). The intake rates of teriyaki chicken using texture-modified chicken and conventional chicken thigh were 75.3% and 60.0%, respectively. Conclusions: We developed a novel texture-modified chicken for a soft diet using yogurt. The texture-modified chicken had both softness and high nutrient content. Continuance of efforts such as that described in this study will lead to the prevention of undernutrition in the elderly.
Key words: Soft diet, food texture, elderly, intake amount, nursing home.
Introduction
The aging population in developed countries is advancing. In Japan, the aging population accounts for 26.6% in 2015, which was the highest in the world (1, 2). As a result, how Japan handles its aged society is being watched by the world. A major issue is maintaining the long-term care insurance system. The number of people certified for long-term care and support in 2015 was 6.2 million, which was approximately 5% of the total population (2, 3). Major conditions requiring the need of assistance or care were dementia (18.0%), cerebrovascular (16.6%), asthenia due to a ripe age (13.3%), and fracture (12.2%) in 2016 (4). Because asthenia and fracture are caused by frailty, it is important to slow its progression. Weakness, slowness, low activity, exhaustion, and weight loss are considered components of frailty, creating a self-perpetuating cycle, with malnutrition being a part of this cycle (5, 6).
Elderly individuals with poor dentition have difficulties eating a variety of foods such as fruits (7), vegetables (8, 9), fish and shellfish (8), as well as meat (9). In addition, their intake of protein, calcium, and dietary fiber is low (8-10). The Mini Nutritional Assessment-Short Form score of elderly individuals with non-functional occlusal support is lower than that of those with functional occlusal support (11). The number of present teeth and occlusal force of the elderly with frailty are lower than robust elderly individuals (12). Therefore, it is necessary to develop texture-modified foods for the purpose of maintaining the dietary intake of elderly individuals with masticating issues.
Texture-modified foods for patients with dysphagia have been studied since the 1990s, and have been standardized in some countries (13-16). In 2016, the International Dysphagia Diet Standardization Initiative developed international terminology and definitions for texture-modified foods (17). It is possible to use the highest class of these criteria for preparing texture-modified foods for elderly individuals with masticating problems. Although some criteria recommend foods cut into bite-sized or smaller pieces, these foods tend to be unappetizing, thereby contributing to decreased food intake in the elderly. Therefore, we focused on creating soft diet cooked foods. To evaluate the texture adequacy of a soft diet objectively, a physical measurement method is necessary. The Dysphagia Diet Pyramid (18) is a well-known physical assessment method for food texture in Japan. Therefore, we referred to the Dysphagia Diet Pyramid in this study. It is classified into six steps: a diet composed of jelly with less than 2 g of protein per 100 g of food is used to initiate rehabilitation of dysphagia patients who suffered a stroke (Level 0: L0), diet consisting of jelly, pudding, or mousse containing protein (L1, L2), a diet made of puree or paste (L3), soft diets (L4), and ordinary diets (L5), depending on the values obtained from the texture measurement (19). The standard physical properties of the Dysphagia Diet Pyramid were determined by texture measurement of gradual meals depending on the level of dysphagia those were provided by the Seirei Mikatahara hospital (18,19).
To prevent the decrease in food intake of elderly individuals with weak masticatory skills, it is essential to set quantitative standards of soft diet textures and share cooking methods that allow meeting these standards. Moreover, to maintain the nutritional level of the elderly, soft diets should have similar nutrition values to ordinary diets.
We studied soft diet cooking methods that could yield hardness below 40,000 N/m2, corresponding to level 4 (L4) of the Dysphagia Diets Pyramid. Moreover, we focused on main dishes, which provide high protein intake. We selected chicken, a meat that is more difficult to soften through cooking compared to pork and beef, and that can be sliced.
To soften the meat, the freeze impregnation method using protease, which is well known in Japan (20) is needed. However, this requires a vacuum packaging machine. We attempted to soften chicken using a commercially available softening agent for meat without a vacuum packaging machine, but the chicken did not become softer and was consequently not suitable for a soft diet. Therefore, we used minced chicken whose connective tissues were cut. Because the dumpling made from minced chicken only was hard, foodstuff was added to soften the meat. We selected baked wheat gluten called “yakifu,” a Japanese traditional food to maintain the same amount of protein as conventional chicken. The intake rate of the texture-modified chicken whose hardness was under 40,000 N/m2 was significantly higher than that of the conventional chicken whose hardness was over 63,000 N/m2. However, the provided weight of the texture-modified chicken including water-soaked yakifu was approximately twice that of the conventional chicken thigh. According to the interviews with some participants, the provided amount of the texture-modified chicken was too much (21).
In this study, we tried to develop a novel texture-modified chicken whose weight was lower than that including yakifu. We carried out preliminary studies to decide which food additive to use for softening chicken. Baking soda, eggs, mayonnaise, and yogurt were tested. We ultimately selected yogurt because texture-modified chicken with yogurt was soft, tasty, and easy to handle. The proportions in the texture-modified chicken were decided, and then the intake amount by elderly residents of the newly created texture-modified chicken was assessed and compared to that of their conventional soft diet in order to evaluate its effectiveness.
Methods
Preparation of samples for assessing proportions for texture-modified chicken
We used chicken breast for texture-modified meat, because they contain more protein than chicken thigh. Chicken breast with removed skin and fat was grounded and used in this study. Minced chicken, yogurt, water, and potato starch were mixed, divided in 70-g samples, molded into an oval shape, and boiled for 5 min ensuring they spent 1 min above 75°C.
Test method for measuring proportions in the texture-modified chicken
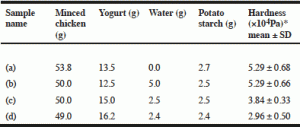
We evaluated the proportions of minced chicken, yogurt, water, and potato starch in the texture-modified chicken. We created four samples for which the textures were measured, where the minced chicken, yogurt, water, and potato starch contents were (a) 53.8 g, 13.5 g, 0 g, and 2.7 g, (b) 50.0 g, 12.5 g, 5.0 g, and 2.5 g, (c) 50.0 g, 15.0 g, 2.5 g, and 2.5 g, (d) 49.0 g, 16.2 g, 2.4 g, and 2.4 g, respectively (Table 1).
* Hardness of the texture-modified chicken was measured after boiled.
Texture measurement of samples for evaluating the proportions of texture-modified chicken
The texture measurement method was based on the Dysphagia Diet Pyramid using a creep meter RE2-33005S (Yamaden Japan). Samples were packed into a laboratory stainless dish with a diameter of 40 mm and depth of 15 mm. A 20-mm diameter cylindrical plunger was then plunged into the samples. The samples were kept at 20 ± 2°C, and a 20 N load cell was used. The distortion factor was 66.67% and the plunging rate was 1 mm/s. Hardness was calculated from the highest point on the texture curve. Each measurement was repeated five times; the highest and the lowest values were omitted, and the average was calculated using the remaining three values.
Intervention dates and participants
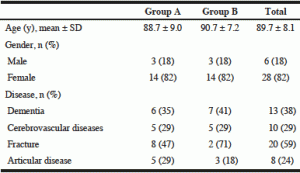
Surveys were conducted by researchers at a nursing home (long-term care health facility) in Kyoto, Japan twice in the month of June 2016. We provided teriyaki chicken for lunch using the texture-modified chicken and chicken thighs as a soft diet. All other dishes (rice, potato stew, boiled spinach, and soup) remained unchanged. The participants were composed of 34 elderly individuals (6 men and 28 women; mean age 89.7 ± 8.1 years). The study participants did not require assistance with eating. Even though thirteen of the participants had dementia, they sometimes needed for care or were independence with someone’s attention. The type of diet assigned to each participant was determined based on their eating status, their own requests, and observations made after admission by the medical doctor, physical therapist, occupational therapist, nurse, and registered dietitian of the facility. We surveyed the intake amount by crossover design. The study participants were evenly divided into two groups (Group A and Group B) based on sex and age (Table 2). Group A received the texture-modified chicken on the first survey date (12 June) and the conventional chicken thigh on the second survey date (24 June). Group B received the conventional chicken thigh on the first survey date and the texture-modified chicken on the second survey date. This study was approved by the Ethics committee of Doshisha Women’s College of Liberal Arts (No. 56). We obtained the participants’ or their family members’ consent for study participation.
Cooking method of the conventional teriyaki chicken for the intervention trial (one serving)
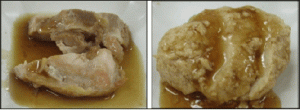
Approximately 70 g of chicken thigh was cut into bite-sized chunks and baked with 2 g of salad oil. It was then introduced into a pressure cooker along with 5 g of soy sauce, 3 g of mirin-like seasoning, 2 g of cooking sake, 1 g of sugar, and water in which all food additives were previously immersed and stewed. A mixture of 2 g of starch and 2 g of water was subsequently added into the cooker to thicken the soup. We prepared 50 servings (Figure 1).
Cooking method of teriyaki chicken using the texture-modified chicken for the intervention trial (one serving)
Minced chicken breast (57 g), 19 g of yogurt, 2.5 g of water, 0.5 g of ginger juice, 3 g of potato starch, and 1 g of soy sauce were mixed. The mixture was shaped into an oval and boiled for 5 min, ensuring they spent 1 min above 75°C. These texture-modified chicken were put into a pot with 4 g of soy sauce, 3 g of mirin-like seasoning, 2 g of cooking sake, 1 g of sugar, and water in which all food additives were immersed and stewed. A mixture of 2 g of starch and 2 g of water was subsequently added into the cooker to thicken the soup. We prepared 50 servings (Figure 1).
Texture measurement of provided samples for the intervention trial
A sample of the meal provided in the nursing home was brought back to the laboratory with refrigerant packs and the texture was measured within 4 h. The measurement method was the same as mentioned above.
Measurement of the intake amount
Before the preparation of tray service, the texture-modified chicken and the chicken thigh of the main dishes of all participants were weighed. When the participant left some texture-modified chicken or chicken thigh, the leftovers were weighed and deducted from the total weight of the served chicken. The resulting value was treated as the intake amount. The intake rate was calculated by dividing the intake amount by the served amount.
Nutritional value calculation
Nutritional values were calculated using the seventh edition of the Japanese Standard Tables of Food Composition.
Data analysis
The Wilcoxon rank sum test was carried out using the IBM SPSS Statistics v24.0 software.
Results
Analysis of the proportions in the texture-modified chicken
Table 1 shows the hardness of the samples determined by texture measurements. Although sample (c) and (d) had a hardness that was lower than 40,000 N/m2 after boiling for 5 min, the proportion of sample (d) that was softer than sample (c) was provided in the nursing home.
Hardness and weight of the texture-modified chicken
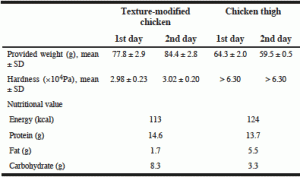
The hardness of the provided texture-modified chicken served on both study days in the nursing home was approximately 30,000 N/m2. The hardness of the provided chicken thigh was > 63,000 N/m2, which is higher than the upper limit of the measurement in these conditions. The weights of the texture-modified chicken served on both survey days were 1.2 and 1.4 times heavier than that of the chicken thigh (Table 3).
Nutritional value
Table 3 shows the energy, protein, fat, and carbohydrate values of the provided teriyaki chicken made from the texture-modified chicken or chicken thigh. Because the texture-modified chicken was made from chicken breast, yogurt, and potato starch, the energy levels and the fat content were lower, and the carbohydrate content was higher than those of the chicken thigh.
The numbers of the participants whose intake rates of both chicken thigh and texture-modified chicken were 100% were 8 in group A and 4 in group B
Survey of intake amount
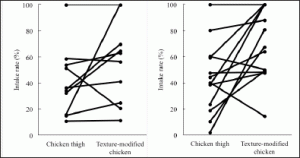
The number of participants whose intake rate of the conventional chicken thigh was 100% was 8 in group A and 4 in the group B. The intake rate of the texture-modified chicken of participants whose intake rate of the conventional chicken thigh was 100% in all groups was also 100%. The number of participants whose intake rate of the texture-modified chicken was higher than that of the conventional chicken thigh was 7 in group A and 11 in group B. The number of participants whose intake rate of the texture-modified chicken was lower than that of the conventional chicken thigh was 2 in both groups (Figure 2). Table 4 shows the mean intake rates. The intake rate of the texture-modified chicken of group B and all participants was significantly higher (p < 0.05, p < 0.01) (Table 4).
Discussion
The average of the intake rate of the teriyaki texture-modified chicken using yogurt was higher than that of the chicken thigh (Table 4). In this study, we surveyed the intake amount by crossover design. Because it was assumed that the intake amount of the first survey day did not affect that of the second day, it was not necessary to consider carryover effect. We however considered the period effect, which was defined as the difference between the intake rate of the texture-modified chicken and the chicken thigh of the two groups. Consequently, there was no significant period effect between groups A and B.
In this study, both the texture-modified chicken and the chicken thigh were cooked with same seasonings. According to the interviews with some participants, they felt that the texture-modified chicken was easier to eat than the chicken thigh. Therefore, chicken with a hardness of less than 40,000 N/m2 is suitable for a soft diet. Although the intake rate of the teriyaki chicken made from the texture-modified chicken using yakifu was also higher than that of the chicken thigh (21), the texture-modified chicken was approximately twice as heavy as chicken thigh with similar protein content. This is because yakifu absorbed a significant amount of the seasoning soup. According to the interviews with some participants, the provided amount of the texture-modified chicken using yakifu was too much. Many participants left more of the other side dishes than those at the time of providing the chicken thigh.
It is necessary to add water in order to soften food. As an example, mousse-formed and blended foods are cooked with a lot of water (22). Therefore, the intake energy and protein content of elderly individuals who ate the soft diet were less than that of those maintain a normal diet (23, 24). Increasing nutrient content is a big problem with cooking a soft diet. In this study, we used yogurt as an additive to mince the chicken. Using this method, we achieved softness and high nutrient content. Therefore, the intake rates of other side dishes were same as those at the time of providing the chicken thigh.
The cooking of softened texture-modified meat has been previously reported. Kuroda et al. (25) and Takahashi et al. (26) developed texture-modified meat using minced chicken thigh with onion, and minced pork with some types of tuber, respectively. We estimated the protein contents of the texture-modified meats obtained using onion or potato, which contain a lot of carbohydrate and very little protein. Because we focused on the main dishes that provide high protein intake, we did not try to use onion or potato as additives in this study.
Furthermore, we focused on 22 participants whose intake rate of conventional chicken thigh was not 100%, to prevent undernutrition. The average intake rate of the chicken thigh was 38.2%, and that of the texture-modified chicken using yogurt was 61.8%. The energy and protein of the texture-modified chicken were similar to those of the chicken thigh. The 18 participants, whose intake rate of the texture-modified chicken was greater than that of the chicken thigh, could ingest more energy and protein from the texture-modified chicken.
This study however has several limitations. Texture measurements should be done at the temperature at which the food is provided. Indeed, physical properties of cooked meat are affected by its temperature (22). However, we measured the textures of the samples at 20°C, when they would have been softer than at the provided temperature.
In this study, our intervention was short. We should provide texture-controlled soft diet continuously and assess long-term nutritional status of the participants. Furthermore, we did not measure the occlusal force of the participants, as low masticatory performance limit food intake. Therefore, this is a major cause of undernutrition in the elderly (7-12). Future studies will need to account for the relationship between occlusal force and the hardness of the food being evaluated.
It was difficult to uniform the weight of the cooked teriyaki chicken under the ordinary running of lunch service in the nursing home. Therefore, we considered period effect to account for this limitation, and determined that there was no significant period effect between groups A and B. There was also no effect related to the difference in weight.
In conclusion, we developed a novel texture-modified chicken for a soft diet using yogurt. The texture-modified chicken had both softness and high nutrient content. According to the survey in the nursing home, the intake rate of the texture-modified chicken was higher than that of the chicken thigh. Continuance of efforts such as that described in this study will lead to the prevention of undernutrition in the elderly.
Acknowledgment: We are deeply grateful to the staff and residents of the nursing home for participating in this study. We would like to thank Ms. Ririka Abo, Ms. Sayaka Kawahito, Ms. Nana Kohno, Ms. Yuna Fujino, Ms. Yukiko Fukuyama, and Ms. Ayumi Kihara for cooking teriyaki chicken in the laboratory and surveying intake amounts.
Conflict of Interest: The authors declare that they do not have any conflict of interest.
Ethical Standards: The study was conducted in accordance with the principles of the Declaration of Helsinki.
References
1. Cabinet Office, Government of Japan. Annual Report on the Aging Society. 2016. http://www8.cao.go.jp/kourei/english/annualreport/2016/2016pdf_e.html. Accessed 27 September 2017
2. Statistics Bureau, Ministry of Internal Affairs and Communications. 2015 Population Census. http://www.stat.go.jp/english/info/news/20161227.htm. Accessed 27 September 2017
3. Ministry of Health, Labour and Welfare. Report on Project of Long-term Care Insurance. 2015. http://www.mhlw.go.jp/topics/kaigo/osirase/jigyo/15/dl/h27_gaiyou.pdf. Accessed 27 September 2017
4. Ministry of Health, Labour, and Welfare. Comprehensive Survey of Living Conditions 2016. http://www.mhlw.go.jp/toukei/saikin/hw/k-tyosa/k-tyosa16/dl/06.pdf. Accessed 27 September 2017
5. Fried LP, Tangen CM, Walston J, et al. Frailty in older adults: Evidence for a phenotype. J Gerontol Med Sci 2001; 56A:M146-M156. doi: 10.1093/gerona/56.3.M146.
6. Xue QL, Bandeen-Roche K, Varadhan R, Zhou J, Fried LP. Initial manifestations of frailty criteria and the development of frailty phenotype in the women’s health and aging study II. J Gerontol Med Sci 2008; 63A:984-990. doi: 10.1093/gerona/63.9.984.
7. Sahyoun NR, Lin CL, Krall E. Nutritional status of the older adult is associated with dentition status. J Am Diet Assoc 2003; 103:61-66. doi: 10.1053/jada.2003.50003.
8. Iwasaki M, Taylor GW, Manz MC et al. Oral health status: relationship to nutrient and food intake among 80-year-old Japanese adults. Community Dent Oral Epidemiol 2014; 42:441-450. doi: 10.1111/cdoe.12100.
9. Iwasaki M, Yoshihara A, Ogawa H et al. Longitudinal association of dentition status with dietary intake in Japanese adults aged 75 to 80 years. J Oral Rehabil 2016; 43:737-744. doi: 10.1111/joor.12427.
10. Saarela RK, Lindroos E, Soini H et al. Dentition, nutritional status, and adequacy of dietary intake among older residents in assisted living facilities. Gerodontology 2014; 33:225-232. doi: 10.1111/ger.12144.
11. Wakabayashi H, Matsushima M, Ichikawa H et al. Occlusal support, dysphagia, malnutrition, and activities of daily living in aged individuals long-term care: a path analysis. J Nutr Health Aging 2017. doi: 10.1007/s12603-017-0897-0.
12. Watanabe Y, Hirano H, Arai H et al. Relationship between frailty and oral function in community-dwelling elderly adults. J Am Geriatr Soc 2017; 65:66-76. doi: 10.1111/jgs.14355.
13. Cichero JAY, Steele C, Duivestein J et al. The need for international terminology and definitions for texture-modified foods and thickened liquids used in dysphagia management: foundations of a global initiative. Curr Phys Med Rehabil Rep 2013; 1:280-291. doi: 10.1007/s40141-013-0024-z.
14. National Dysphagia Diet Task Force. National Dysphagia Diet: Standardization for Optimal Care. 2002. Chicago, IL, American Dietetic Association.
15. Atherton M, Bellis-Smith N, Cichero JAY, Suter M. Texture-modified foods and thickened fluids as used for individuals with dysphagia: Australian standardised labels and definitions. Nutr Diet 2007; 64:53-76. doi: 10.1111/j.1747-0080.2007.00153.x.
16. The dysphagia diet committee of the Japanese Society of Dysphagia Rehabilitation. The Japanese Dysphagia Diet 2013. Jpn J Dysphagia Rehabil 2013; 17:255-267.
17. Cichero JAY, Lam P, Steele C et al. Development of international terminology and definitions for texture-modified foods and thickened fluids used in dysphagia management: the IDDSI framework. Dysphagia 2017; 32:293-314. doi: 10.1007/s00455-016-9758-y.
18. Yamagata Y. Physical property of meals. In: Kayashita J (ed) 100 recipes for dysphagia patients based on the Dysphagia Diets Pyramid for hospitals and facilities. 2009. Ishiyaku Publishers, Tokyo, pp 13-18 (in Japanese).
19. Sakai M, Egashira F, Kanaya S, Kayashita J. Staged physical property assessment of dysphagia diet. Nihon Byoutai Eiyo Gakkaishi (J Metabolism Clinical Nutr) 2007; 10:269-279 (in Japanese).
20. Sakamoto K, Shibata K, Ishihara M. Decreased hardness of dietary fiber-rich foods by the enzyme-infusion method. Biosci Biotechnol Biochem 2006; 70:1564-1570. doi: 10.1271/bbb.50562.
21. Watanabe E, Maeno M, Kayashita J, Miyamoto K, Kogirima M. Cooking methods for a soft diet using chicken based on food texture analysis. J Nutr Sci Vitaminol 2017; 63:256-262.
22. Yamagata Y, Sakai M, Kayashita J. Current status and issues of modified diet for dysphagia persons by researching physical properties. Jpn J Dysphagia Rehabil 2012; 16:140-147 (in Japanese).
23. Nowson CA, Sherwin AJ, McPhee JG, Wark JD, Flicker L. Energy, protein, calcium, vitamin D and fibre intakes from meals in residential care establishments in Australia. Asia Pac J Clin Nutr 2003; 12:172-177.
24. Wright L, Cotter D, Hickson M, Frost G. Comparison of energy and protein intakes of older people consuming a texture modified diet with a normal hospital diet. J Hum Nutr Dietet 2005; 18:213-219. doi: 10.1111/j.1365-277X.2005.00605.x.
25. Kuroda R, Ahhmed AM, Namba Y et al. The improvement of textural properties of chicken meat loaf manufactured for elderly people. J Warm Regional Soc Animal Sci Jpn 2009; 52:23-28 (in Japanese).
26. Takahashi T, Kim Y, Iwasaki Y, Ogoshi H. Ease of eating of pork meat prepared by adding mashed tubers evaluated by physical properties, masseter muscle activities, and sensory tests. Home Economics Jpn 2010; 61:147-154 (in Japanese).