M. Fetterolf1, P. Kao2, N. Castle1
1. University of Pittsburgh, USA; 2. Department of Anthropology, Harvard University, USA. Corresponding author: Philip Kao, Harvard University, USA, philip_kao@fas.harvard.edu
Jour Nursing Home Res 2019;5:24-26
Published online June 5, 2019, http://dx.doi.org/10.14283/jnhrs.2019.5
Abstract
Across the United States, 60% of Assisted Living administrators noticed an increase in legal claims; meanwhile nearly 75% noticed an increase in lawsuits and 71% noticed an increase in settlements. This article asks whether or not the rise in legal pressure may be attributed to a higher proportion of residents with moderate to severe cognitive impairment in Assisted Living. More broadly, the findings indicate that there is a lack of consumer choice and solutions for the elderly in need of long-term services. As a short-term option to mitigate the rise in legal pressure, long-term facilities could explore ways to work with residents in defining various thresholds of care that are safe, sustainable and economically sound whilst preserving certain aspects of residents’ desired lifestyles. Over the long term, the United States needs to develop innovative options for the provision of long-term care services with a focus on redesigning care for older adults with their input. The consequences of such a positive change are examined.
Key words: Assisted Living, Nursing Homes, Consumer-Centered Healthcare, Lawsuits, Dementia.
Introduction
In the US, some attorneys are finding that after years of targeting Nursing Homes, law firms are shifting their focus toward Assisted Living. Some firms are using a “nursing home lawsuit playbook” to litigate against these expanding facilities (1). As the number of older adults in Assisted Living with moderate to severe cognitive impairment increases, facility administrators face severe challenges to care for the complex needs of residents while maintaining the values which Assisted Living was founded upon, namely: care, dignity, autonomy, and privacy.
In February 2017, the authors sent out 225 research questionnaires, by postal and electronic mail, to Assisted Living administrators in ten states across the US. Of the 225 facilities, 85% percent of them listed having “memory care units” on their websites. Our research surveys were structured to capture opinion-based, qualitative data from administrators regarding their perceptions of the number of claims, lawsuits, and settlements trending over the past five years. The methodology for collecting responses from the various facilities across the country was based on geographic spread, and the presence of a “memory care unit” in each respective Assisted Living Facility (ALF). Additionally, the majority of the facilities we targeted were medium-sized. The surveys solicited information about the types of lawsuits, prevalence of dementia in their facility, and the effects that legal pressure might have had on notions of resident choice, dignity, privacy, and safety (2). This study received 58 responses from nine states with a total 25.7% response rate overall (3).
Results
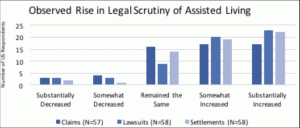
Administrators were asked to appraise the number of claims, lawsuits, and settlements over the last five years. Almost 60% of administrators noticed an increase in claims; nearly 75% of the respondents noticed an increase in lawsuits; and 71% noticed an increase in settlements.
Additionally, when asked to respond to the statement “Litigation is forcing ALFs to become more like nursing homes in terms of regulation”; 68% of administrators responded with somewhat or strong agreement; 22% neither agreed or disagreed; and 10% showed some form of disagreement.
Consumer Driven Assisted Living
The Assisted Living industry has become a target for litigation due to large variation with respect to facility size, admission policies, level of complex care needs (e.g. mobility support, eating/medication assistance) and dementia care capability (4). Growth in the Assisted Living sector across the US has been attributed to its market model of care promoting resident independence, autonomy, privacy, and dignity (5), as well as serving the primary provider for residential care for older adults with dementia (6).
As a point of clarification, ALFs offer residents assistance with the activities of daily living in a residential setting. In contrast, skilled nursing facilities (SNF) are places that can be temporary or longer term stays for people who need constant care and medical treatment from a registered nurse 24/7. Historically, the process of identifying a suitable home for a loved one has not been a consumer-driven process. Put simply, if an older adult can no longer live independently and does not require the level of support offered in skilled nursing, they are left to choose among the current supply of assisted living (or similar) facilities. In terms of care needs, this cohort accounts for the largest proportion of older adults needing supportive services. A combination of online research and touring of ALFs close to one’s current residence is the basis for a decision. There is no shortage of checklists and online resources to select a home for an older adult (most sites appeal to the son or daughter of a loved one as opposed to the actual resident). Given that 60% of assisted living residents only relocate within a 10-mile radius from their home, and 80% relocate within a 25-mile radius, this is a very narrow range to find a suitable home (7). As such, one is likely to be subject to the geographical definitions of quality and amenity; given that although the industry has rapidly expanded since its inception in the late 1970s, there has been no establishment of a threshold at or below which an ALF can provide adequate care without comprising resources and safety.
The establishment of a “threshold of care” should be an agreement between the resident and the facility in question. The facility shouldering responsibility should refer any individuals for whom they can no longer care for adequately and safely to more appropriate care settings such as SNFs. Residents with severe dementia are broadly defined as those who need non-stop assistance with daily activities and personal care. They lose awareness of recent experiences as well as of their surroundings; they also experience changes in basic physical abilities (including the ability to walk, sit, or even swallow sometimes). Furthermore, they have increasing difficulty communicating, and become vulnerable to infections, especially pneumonia (8). One memory care unit administrator from a Pennsylvania ALF said that “The population that used to be in nursing homes is now in Assisted Living”, which suggests that the industry is reacting to increasing demand, market competition, and a changing population base, instead of responding to the way they can provide services, especially with respect to medium-severe dementia. In fact, the ‘patient’ populations in both ALFs and SNFs have changed because of particular social-economic factors, but the fact remains that ALFs have to figure out how to balance when dementia related deficits have reached a tipping point.
In 2014, seven out of ten residents in ALFs exhibited some form of cognitive impairment. More specifically, 29% of residents had mild impairment; 23% have moderate impairment; and 19% have severe impairment (6). Considering that ALFs are private facilities which need to provide an economically feasible margin through staffing, overhead, and private reimbursement (that is about half of the cost of a skilled nursing home bed) questions arise regarding whether ALFs are appropriately suited to provide care to individuals with moderate to severe cognitive impairment. This is a contentious point in the industry, given that less than half of ALFs have a registered nurse on staff or licensed practical nurse hours (4). Correspondingly, hospitalization rates for moderate to severe dementia residents were 69% and 42% higher respectively in ALFs than for similar residents in nursing homes (9). This also feeds into the issue of a lack in government regulations pertaining to ALFs. Whether or not a consumer-driven model will provide an economic solution to finding appropriate care is still inconclusive. After all, ALFs are emergent models that require more research and consumer-led education, lobbying, and outreach. Still today, very little research has shown the outcomes of care for dementia patients in Assisted Living.
The US can no longer assume that an older adult will fit into one of three global/standard care models. We must begin to redesign care for our older adults by meeting older adults where they are in their life course, and with their input, design supportive care solutions that have the inherent ability to change as one’s care needs and preferences change. For example, cutting edge healthcare organizations are beginning to incorporate patient choice in one’s care plan. The creation of a care plan is multifactorial and based on one’s preferences. These preferences take into account treatment options between biomedicine and alternative medicine, one’s inclination towards pain, quality of life, risk and even types of healing that extend beyond the person, incorporating the larger family unit in the decision process. The long term care industry should facilitate autonomy. Care plans should innovate and possibly draw from artificial intelligence in order to create self-learning models that could update and predict particular changes in care needs and outcomes. Autonomy is difficult to start initiating when someone already has severe dementia. A possible solution, however, could be to rescale the ‘resident autonomy’, allowing the resident (and/or his/her family) to customize a set of services and progressive models of care in line with one’s lifestyle and the kind of future life they want to live out.
Conclusion
Assisted Living administrators across the country, are reporting that the number of claims, lawsuits, and settlements are increasing. Most administrators believe that this increased legal pressure is bound to reshape the regulatory framework of the ALF. Although this study doesn’t provide conclusive evidence to state that higher proportions of residents with moderate to severe cognitive impairment in Assisted Living is driving this trend, our results suggest that this phenomenon may be one explanation for the observed rise in litigation and worthy of further research and policy action. A broader explanation for the rise in litigation could be that the Assisted Living industry is experiencing the effects of a non-consumer driven environment exacerbated by an increasingly diverse, wide and complex population of older adults.
The ideal solution to the rising legal scrutiny would be to re-establish assisted living to allow for individualized and dynamic care planning. However, this cultural shift will take time. A short-term necessity will be to clearly define the threshold care needs that Assisted Living can safely and economically provide. According to our research, a threshold of care should be defined through individual agreements between each resident and the facility. Ideally, the facility is obligated to provide the supportive care necessary to allow the individual to preserve the kinds of autonomy they desire. Increased autonomy may result in compromised safety metrics (e.g. an uptick in the number of falls). Therefore, if a facility decides to accommodate the kinds of autonomy a person wishes to have, that facility should be afforded some meaningful legal protection.
Given the well-documented variation across the Assisted Living industry and the lack of federal regulation, Kathryn Hawes states that the effort to define quality in Assisted Living takes on a “Sisyphean cast”. Hawes goes on to say that “[…] there has been substantial progress with nursing home care, at least at a conceptual level, the rock slips and one is then faced with the uphill challenge of considering quality’s meaning in a new and different care modality— [Assisted Living] (10).” If no threshold of care standard is established and institutionally monitored, lawsuits will continue to increase which may force policy initiatives to be reactive and tip the balance disproportionately toward safety as opposed to autonomy; a criticism common to nursing homes. It is time for ALFs to set reasonable boundaries and reestablish themselves as innovative care providers. ALFs can shield themselves from legal scrutiny and reserve a place for individuals that need person-centered care by shifting the focus from developing a solution for a population to designing a dynamic solution based on the ever-changing needs and input of the consumer.
Conflict of interest: There were no identified conflicts of interest in this article.
Ethical standard: All respondents of the survey were informed how their responses would be used. There were no financial or personal relationships that would bias the findings.
References
1. Adelman, R. Esq. (2013). Assisted living lawsuits: An ounce of prevention is worth a pound of cure. Geriatric Nursing, 34(16), 6e169.
2. The survey was reviewed by two health policy lawyers and a long-term care quality expert at the University of Pittsburgh’s School of Public Health before distribution.
3. The nine states were broken down into three regions (East, Middle, and West) and included: NY, PA, FL, KY, SD, CO, TX, CA, NV. No Assisted Living facilities in OR provided a response.
4. Han, K., Trinkoff, A. M., Storr, C. L., Lerner, N., &Yang, B. K. (2016). Variation Across US Assisted Living Facilities: Admissions, Resident Care Needs, and Staffing. Journal of Nursing Scholarship.
5. Mollica, R. (1998). State regulation update: States are adopting new rules at a brisk pace. Contemporary Long Term Care, 21, 45-49..
6. Zimmerman, S., Sloane, P. D., & Reed, D. (2014). Dementia prevalence and care in assisted living. Health Affairs, 33(4), 658-666
7. 2009 Overview of Assisted Living – AHCA/NCAL
8. As defined by the Alzheimer’s Association – https://www.alz.org/alzheimers-dementia/stages
9. Sloane, P. D., Zimmerman, S., Gruber-Baldini, A. L., Hebel, J. R., Magaziner, J., & Konrad, T. R. (2005). Health and functional outcomes and health care utilization of persons with dementia in residential care and assisted living facilities: comparison with nursing homes. The Gerontologist, 45 (suppl. 1), 124-134.
10. Hawes, C., & Phillips, C. D. (2007). Defining quality in assisted living: Comparing apples, oranges, and broccoli. The Gerontologist, 47(suppl_1), 40-50.