J.M.G.A. Schols1,2, E.P. Poot3, N.M. Nieuwenhuizen3, W.P. Achterberg4
1. Maastricht University, Care and Public Health Research Institute, Department of Health Services Research and Department of Family Medicine, Maastricht, The Netherlands; 2. Living Lab in Ageing and Long-Term Care, Maastricht, The Netherlands; 3. Verenso, Dutch Association of Elderly Care Physicians, Utrecht, the Netherlands; 4. Department of Public health and Primary care, Leiden University Medical Center, Leiden, the Netherlands. Corresponding author: JMGA Schols, Maastricht University, Care and Public Health Research Institute, Department of Health Services Research and Department of Family Medicine, Maastricht, The Netherlands, jos.schols@maastrichtuniversity.nl
Jour Nursing Home Res 2020;6:30-34
Published online July 6, 2020, http://dx.doi.org/10.14283/jnhrs.2020.7
Abstract
It is absolutely no surprise that the Dutch nursing home sector with a total of 125.000 residents would be affected by COVID-19. Before the first case in the Netherlands was registered, alarming signals had already arrived from other countries, indicating that the frail and disabled, multimorbid nursing home population is an easy prey for this virus. In the meantime, despite a visitor lockdown since mid-March, a considerable amount of residents and staff have been infected and around 1700 residents have died from COVID-19 (mid-May). The future will learn what the long-term consequences of this crisis will be for residents and staff and what finally will be the main lessons learnt. This article shows that it is clear that we have some way to go, to ensure that the Dutch nursing home sector, despite its good infrastructure, will be sustainably and proactively recognized, resourced and equipped to fulfil its unique role in long-term care. Moreover the sector has to find its way in preparing itself for the temporary future 1,5 meter society.
Key words: COVID-19, nursing home, Netherlands.
Report from The Netherlands
Not unexpectedly, the Dutch nursing home sector (with a total of around 125.000 beds) has been hit by the COVID-19 pandemic as well. In this article we want to show how Dutch nursing homes actually try to deal with COVID-19. In doing so, we will generally respect the phases that are connected with handling a widely spread infection: a) phase of preparation; b) phase of outbreak; c) phase of getting control; d) phase of recovery; e) phase of evaluation. As we are still in the crisis, not all phases can be addressed completely and the focus is consecutively on the following issues:
1. Preparation – How well prepared were Dutch nursing homes for this pandemic, initially?
2. Phase of outbreak – What did Dutch nursing homes do during the outbreak phase of the virus?
3. Getting control – What happened during the outbreak phase of the virus and what are the consequences for residents, family and staff?
4. Preliminary evaluation – What are the first lessons to be learnt for the future?
Preparation – How well prepared were Dutch nursing homes for this pandemic, initially?
In general Dutch nursing homes distinguish themselves from care homes in most other countries in that sense that they have a well-developed care infrastructure and are fully part of the national health sector and not of the social sector. Dutch nursing homes employ their own multidisciplinary care teams, consisting of, amongst others, nurses, elderly care physicians, psychologists, physiotherapists, occupational therapists, speech therapists, dieticians and pastoral (spiritual) workers. Nursing home medicine, currently called elderly care medicine, has been a recognized field of medicine since 1989. In the past thirty years, these professionals and teams have professionalized to a large extent, specific trainings were developed and many diagnostic and treatment protocols targeting nursing home residents have been developed and implemented. Finally this has led to an overall high standard of care (1, 2).
Fitting in these developments, most Dutch nursing homes also have their own hygiene/infection committee, as outbreaks of flu or infections with Norovirus or MRSA regularly occur and require from personnel to pay extra attention to respecting hygiene and other anti-infective measures. These committees take care of actual hygiene and infection protocols, perform educational and supporting activities for the teams on the wards, perform audits and do advise the management regularly on developing and adapting the hygiene/infection policy and on the stock and provision of necessary materials within the institution. In addition, these committees are often supported by a hygienist or clinical microbiologist from the hospital and they are in close contact with public health services, with regard to obliged registration procedures of some infection types and the start of adequate preventive activities, if needed (3).
In case of larger outbreaks, each nursing home or nursing home organization (in case of more locations) also installs an internal crisis team, consisting of representatives from the management, the professionals, cleaning services, communication department and their own hygiene/infection committee. This also happened when the COVID-19 crisis emerged and signals of its expression in nursing homes in other European countries, especially Italy and Spain, reached the country. The internal crisis team is responsible for 1) optimizing communication, 2) reviewing infection control practices and Personal Protective Equipment (PPE) utilization, 3) creating a centralized process to monitor residents and staff 4) implementing protocols for staff and others and 5) having and executing a plan for an outbreak.
Speeding up occurred after the first cases in Dutch nursing homes were diagnosed in the beginning of March. Since then, the nursing home sector has followed the national directives as given by the National Institute for Public Health and the Environment (RIVM), which in the case of a nation-wide outbreak of a new infectious disease, such as the novel coronavirus, coordinates all efforts to control the disease (4).
RIVM convened the national Outbreak Management Team (OMT – Outbreak Management Team) consisting of specialists from various backgrounds who know a great deal about infection prevention, although the disease in question is new and therefore the knowledge, especially in the beginning at a low level. They continuously advise the Ministry of Health, Welfare and Sport (VWS) and the responsible Ministers. The government ultimately decides which measures are implemented. In each province and region these measures are executed under supervision of the Area Health Authority (GGD).
The most important national measures taken initially, and into action at this moment, were (4):
– Stay at home and work at home as much as possible; leave home only for shopping or a bit of fresh air
– Health care workers, were initially allowed to work if they suffered from a mild cold without fever
– Stay 1.5 meters (2 arms lengths) away from other people
– Do not shake hands
– Wash your hands regularly with soap and water
– Cough and sneeze into your elbow
– Use paper tissues to blow your nose and discard them after use
– Schools and other educational institutes closed
– Sports facilities closed and also gyms, fitness centers
– Restaurants/Eating and drinking establishments closed; take away services allowed.
– Museums, concert venues, theatres etc. and libraries closed
– Contact base jobs not allowed to perform
– Gatherings and events banned.
– Lock down of long-term care facilities for visitors ( family) (since March 20th).
Phase of outbreak – What did Dutch nursing homes during the outbreak phase of the virus?
As stated above, Dutch nursing homes could start from a relatively strong intrinsic basis when the disease entered our country. In line with national measures, Verenso, the Dutch Association of Elderly Care Physicians developed well designed and regularly updated directives as how to act in the nursing home if a (suspected) case of COVID-19 might occur. The dissemination and implementation of these measures occurred in most nursing homes via the internal crisis team, partly delegated to the internal hygiene/infection committee (5)
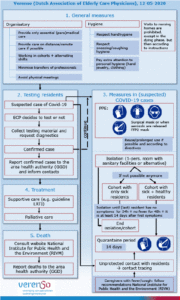
Figure 1 shows a flow-chart with an overview of measures that have to be taken in the nursing home. These measures involve general measures, that built upon activating the internal crisis team and stress the importance of adhering to general hygiene and preventive measures within the institution. Nursing homes were also asked to participate in a country wide registration of COVID-19 (suspect) cases and symptoms, via a module incorporated in the mostly used Electronic Patient Records. Furthermore, the general measures include directives on the logistics of internal care services, meaning to avoid personal contact as much as possible and demand to respect and control the nationally imposed lock down of nursing homes for visitors (family).
In addition to the general measures, there are also directives on diagnosis and testing and measures in case of (suspect) COVID-19 infections and finally treatment directives and instructions on what to do if a resident dies from COVID-19.
Regarding testing, a deciding role has been given to the elderly care physician whether to test the resident or not. For this, a case definition was made: COVID-19 suspect means minimally 1 (formerly 2) of the following symptoms: fever or feeling feverish, coughing, dyspnea OR suspect because of the clinical impression of the physician as COVID-19 may present atypically in nursing home residents. Other symptoms like diarrhea, fatigue and delirium may be present before or without respiratory symptoms. Finally instructions on how to arrange testing by using nasopharyngeal swabs are given.
Measures in case of (suspect) COVID-19 infection do first involve isolation measures; if possible, residents are managed in their rooms as much as possible throughout the pandemic. If that is not possible, a strategy of zoning care homes into COVID-19 positive and negative areas and even mixed is indicated, because the decision to isolate people in their rooms raises considerable practical challenges in residents with dementia, which requires a lot of creativity to find an acceptable and ethical solution. Isolation can be ended if a resident in single isolation or the last patient in an infected cohort is symptom free for at least 24 hrs AND free of fever for 48 hrs AND the start of first symptoms was at least 14 days ago. Quarantine is not only indicated for residents of a mixed area and lasting 14 days after the last resident has been symptom free for 24 hrs, but it also counts for team members, suffering from cough/fever who have had unprotected contact with residents. If they must continue working, they follow the recommendations of the National Institute for Public Health and the Environment (RIVM). Next to isolation procedures, nursing team members must wear Personal Protective Equipment (PPE) (mask, goggles, gown and gloves) when they take care of residents suspect for or with COVID-19. In case of quarantine mask and gloves are sufficient.
Regarding treatment of residents with COVID-19, it is clear that there is no curable intervention available, meaning that the approach has to be one of supportive care, following regular guidelines with regard to viral respiratory tract infections. However it appears to be rather characteristic that a considerable number of residents, suffering from this infection, require oxygen supply and that extra attention must be paid to the nutritional and hydration status and also to the prevention of complications such as pressure ulcers because in more severe cases, residents become completely bed bound. Additionally, in the nursing home, teams can apply the triage directives with regard to older people with COVID-19 at home, nursing home or in the hospital, which have been developed nationally (6). In Dutch nursing homes the attention for adequate Advance Care Planning has already become more important during the last decade and discussions about treatment preferences (including whether or not to undergo reanimation procedures, curative treatments and or referrals to hospitals) are more common now than in the past. This is important as in this COVID-19 period we must avoid ACP becoming ‘fast track ACP’, which in addition is difficult to execute because face-to-face discussions are extremely difficult because of protective shielding measures affecting residents or their family. It will be clear that the use of PPE also hinders the execution of dedicated warm and tender loving end of life care, especially because only 1 or 2 close family members are allowed to visit the resident during the last couple of days.
However, at the time of writing of this article, many care home residents and relatives will by now have reflected on what COVID-19 means for them and that makes it more feasible to discuss issues around future care plans in the context of a pandemic which preferentially affects frail older people. Nevertheless, it is clear that a considerable number of residents do not survive COVID-19. Figure 1 ends with the instruction to report each death case to the regional Area Health Authority (GGD)
Getting control – What happened during the outbreak phase of the virus and what are the consequences for residents, family and staff?
Currently we are in the midst of this 2020 pandemic crisis. At the beginning of May around 9000 residents have been infected with COVID-19 (confirmed as well as suspected cases) country wide, of which 1700 have died already (7). In the meantime, nursing home staff tries to find its way in this new reality and the overall vulnerability of the nursing home environment has led to a visitor lockdown since mid-March, which of course has an enormous negative impact on both the residents and their families.
Even, if all information above may indicate ‘well-preparedness’ of the Dutch nursing home sector, in the period of March until mid-April, paradoxically the national shortages of personal protective equipment (PPE), the restrictive testing policy, which was also related to a low test capacity and the initial sick leave instructions have put an extra strain on nursing homes and their staff. It appeared that, after 2-3 weeks of nursing home lockdown, which is along the incubation time (14 days), still a considerable amount of residents got infected. Some media reported about a silent drama taking place in nursing homes (8, 9). Obvious explanations may be, first, that once the virus is in the building, it is difficult to control. Second, residents may transmit the disease already in the presymptomatic stage and third, the difficulties in respecting complete isolation, especially in demented residents may have contributed as well. But it should not be excluded that the initial sick leave policy for nursing home staff, meaning that staff members were initially allowed and asked to work if they suffered from a mild cold without fever, may have contributed to a rise in infections as well. The more, because there was a general lack of PPE, making the use of PPE only possible when providing direct care to COVID-19 (suspect) residents in their own rooms or created zones and not in the rest of the building. In addition it was difficult to monitor the spread of COVID-19 within the nursing homes as initially the test policy was to stop testing after 2 positive cases had been established in the ward respectively home. Currently, it is not up for debate anymore that the virus has entered nursing homes partly through employees and that some infections may have been avoided, but it must be clear that those caregivers may absolutely not be blamed for this (10, 11).
Because nursing homes, together with other long-term care sectors, were at the very end of the line in the national allocation of tests and protective equipment, employees had to work without protection with very vulnerable residents, who had not been tested themselves, while everyone knows how complicated it is to prevent or combat outbreaks of infectious diseases in nursing homes. This not only has increased the psychological impact of COVID-19 on staff, which works tremendously hard to control the infection within the homes and wants to take care as best as possible for the residents, but it also caused extra stress for families who were not allowed anymore to visit their relatives in the nursing home.
Preliminary evaluation – What are the first lessons to be learnt for the future?
At the end of April and the beginning of May, national awareness rose that the attention for COVID-19 initially had focused mainly on the hospitals and the cueing of their ICUs and not on the long-term care sector (LTC-sector). Therefore, one of the first lessons was that the LTC sector should be included in the national distribution of PPE as soon as possible and that test facilities for COVID-19 should be increased. At this moment, the allocation mechanism for PPE has been amended in order to improve the distribution of PPE to LTC facilities. Testing capacity has increased for both residents and staff. Informal care-givers will be allowed to access testing in June. Finally the sick leave instructions have been adapted as well: employees with or without a fever and other symptoms have to stay at home now (since end of April).
Currently, there is a promising downward trend in the overall number of COVID-19 cases in the Netherlands and it seems that we see the ‘flatten the curve-principle’ also gradually occurring in nursing homes. The most important societal question now is when, and how, we can lift the ban on family visits to nursing homes again. It is known that restricting movements for residents and their families represents a significant loss of autonomy, with psychological and physical harms associated with social isolation and immobility. Of course, these need to be weighed against potential harms to the residents and others if more free movements will be allowed, but seeking for a safe balance is the least we can do now. The government has initiated several pilots on this, which started may 11th, and tries to learn from other countries, like France, Germany and Belgium. The pilots are monitored on possible spread of SARS-CoV-2. The near future will show how this works out (12, 13).
For some people outside the long-term care sector, the nursing home environment may seem a rather unsafe place now, as in regions in which there were many fatal cases of COVID-19 in nursing homes, residents on the waiting list for admission, seem rather reluctant of being admitted at this moment. Moreover, this is enforced directly by the fact that their relatives are not able to visit them after admission. This stresses the need to provide good supportive care to future residents and their families and also adequate and prolonged aftercare to families who lost a resident because of COVID-19.
Another lesson is that much attention must been given to support the mental health of nursing home staff. They have been exposed to high-stress environments during this pandemic and this might cause serious mental health issues. A pro-active approach should be considered here as a high priority, to address these mental health concerns.
Finally, it is important that the pandemic is evaluated nationally in all health care settings.
Conclusion
Overall, we can conclude that despite the well-developed care infrastructure of Dutch nursing homes, it has become clear that in the national COVID-19 prevention policy this sector and other chronic care sectors have been too long a blind spot in the national COVID-19 policy. This must never happen again. Until a vaccine has been found, the new challenge will be how to anticipate and manage new waves of COVID-19 outbreak and to adapt the nursing home environment and all its related processes to a temporary 1,5 meter society to manage spread of SARS-CoV-2.
Conflict of Interest: NO COI of all authors.
References
1. Schols JMGA, Crebolder HF, van Weel C. Nursing home and nursing home physician: the Dutch experience. J Am Med Dir Assoc. 2004 May-Jun;5(3):207-12. Review.
2. Koopmans RT, Lavrijsen JC, Hoek JF, Went PB, Schols JMGA. Dutch elderly care physician: a new generation of nursing home physician specialists. J Am Geriatr Soc. 2010 Sep;58(9):1807-9. doi: 10.1111/j.1532-5415.2010.03043.x.
3. https://www.zorgvoorbeter.nl/hygiene/inspectie-gezondheidszorg
4. https://www.rivm.nl/en
5. file:///C:/Users/jossc/Documents/Documents/ENVIDA/2020/corona%20uitvoering/12%20mei/200512-18-00-COVID-19-behandel-advies-update-herstructurering-DEFINITIEF-huisstijl.pdf
6. https://www.verenso.nl/_asset/_public/Dossiers/Leidraad-triage-thuisbehandeling-versus-verwijzen-COVID-19-def-versie-3-0-07052020-002.pdf
7. https://www.verenso.nl/nieuws/update-registratie-verpleeghuizen-12-mei-2020
8. https://www.volkskrant.nl/columns-opinie/opinie-coronadrama-in-verpleeghuizen-iedereen-keek-de-verkeerde-kant-op~bf4ac2e8/
9. https://www.venvn.nl/nieuws/v-vn-stil-drama-in-wijk-en-verpleeghuizen-door-tekort-beschermende-middelen/
10. https://ltccovid.org/2020/04/26/covid-19-policy-responses-affecting-nursing-homes-in-the-netherlands/
11. Chris Klomp, Hanneke van Houwelingen, Tonny van der Mee. Sterfte onder bewoners verpleeghuizen en instellingen bijna verdubbeld [Deaths amongst residents of nursing homes almost doubled]. AD. 2020.
12. https://www.rijksoverheid.nl/ministeries/ministerie-van-volksgezondheid-welzijn-en-sport/nieuws/2020/05/11/deelnemende-instellingen-versoepeling-bezoekregeling-verpleeghuizen-bekend
13. https://www.actiz.nl/nieuws/handreiking-bezoekregeling-verpleeghuizen-gereed