1. Nursing Science & Research, Nursing Homes ,City of Zurich, Switzerland; 2. Chief Physician of Geriatrics Department, Medical Director Nursing Homes ,City of Zurich , Switzerland. Corresponding author: Dr. med. Gabriela Bieri-Brüning, FMH Gen. Int. Med. spez. geriatrics, Chief Physician Department of Geriatrics, Nursing Homes, City of Zurich, Walchestrasse 31, P.O. Box, 8021 Zurich; Tel. 044 412 10 13; gaby.bieri@zuerich.ch
Published online July 6, 2020, http://dx.doi.org/10.14283/jnhrs.2020.8
Residents of nursing homes are generally of older age and regarded as a high risk group for contracting a SARS-CoV-2 infection. Protective measures and a consistent outbreak management are essential.
In contrast to hospitals, hygiene policies, isolation and quarantine measures are difficult to implement in nursing homes. Residents live in these institutions and move freely around their ward and the public sites of the nursing home. Adherence to strict social distancing is difficult depending on spatial factors and the cooperativeness of residents. 80 % of the residents in the Nursing Homes of the City of Zurich (German abbreviation: PZZ) suffer from dementia. They do not understand why they have to stay in their rooms. In order to avoid having to lock them in their rooms, one-to-one care is inevitable.
Prevention Measures and Outbreak Management
Protection measures have been implemented early on in all nine PZZ sites (approximately 1600 beds). Hand hygiene measures, previously already of great importance, were reinstructed and supervised by link nurses of the hygiene team. A step by step ban on visitors was enacted. From mid March, all the healthcare personnel on the wards were required to wear masks, and soon after that this measure was extended to all employees upon entering the nursing homes. Visits to the hairdresser and podiatric treatments were no longer possible and events by a third party were cancelled. Eventually activities spanning multiple nursing wards and group activities were also discontinued.
New residents had to stay in designated entry into admission and quarantine wards, where they were monitored for 14 days for the appearance of symptoms and their temperature was regularly taken. Additionally, two wards have been installed to provide a systematic cohort isolation, one of which was assigned to demented residents with specific equipment e.g. anti-wandering system.
Nurses were instructed to immediately inform the physicians about residents with any light symptoms such as coughing, fever or subfebrile temperature. Those residents were tested immediately by internal or doctors on call, every day including weekends. The residents were isolated until the test results were available. Soon we found out that a group of residents manifests less pronounced SARS-CoV-2 symptoms in the beginning. Even residents with subfebrile temperatures could be tested positive.
Isolation measures were implemented in the same manner as in the municipal hospitals by use of protective equipment for the personnel (jackets, gloves, surgical masks, glasses; FFP2 masks were provided only for tasks with higher aerosol formation). Staff with fever and/or cough had to give notice and were referred to be tested.
Outbreaks
There have so far been six Coronavirus outbreaks in the Nursing Homes of the City of Zurich. The presumptive infection sources were as follows: one index patient brought the virus from hospital; one resident who visited her sick partner at home; two employees who tested positive (before the mask obligation was implemented); two as of yet unknown infection sources. There was no spread of the virus from designated COVID-19 wards, where besides PZZ internal patients, occasionally patients with COVID-19 from retirement homes and hospitals were admitted (n= 6). In case of an outbreak, stringent cohort isolation was carried out and patients were isolated in designated COVID-19 wards or designated rooms.
At the beginning of April, there were a series of outbreaks in the nursing homes A and B, which were difficult to contain. Despite rigorous testing, quarantine and isolation, more and more residents became symptomatic and tested positive. In consultation with the head infectologist at the Triemli Municipal Hospital, the PZZ directors decided to test all asymptomatic residents in affected wards too. Additionally, all employees working in these wards were tested.
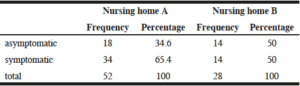
52 out of 110 respectively 28 out of 80 residents were tested positive. Evidently there was a wide spread of the virus. Particularly surprising were the results of the cohort testing (cf. table 1): 18 out of 52 residents or 14 out of 28 residents tested positive for COVID-19 had no symptoms and were identified through the cohort testing only.
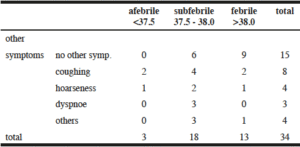
Furthermore, only approximately 41 % of infected and symptomatic residents qualified for testing with the presented symptoms according to the criteria of the Swiss Federal Office of Public Health (FOPH). Besides the approximately 40 % of asymptomatic patients, there are also many oligosymptomatic patients (cf. table 2). They most commonly show subfebrile temperatures. We can therefore conclude that there are asymptomatic patients in the high risk groups as well.
These results help to explain why isolation measures in both nursing homes were not primarily successful, due to asymptomatic patients spreading the virus undetected.
From the analysis of the SARS-CoV-2 outbreak on the cruise ship ‹Diamond Princess›, there are also known cases of elderly asymptomatic COVID-19 patients. Out of 55 COVID-19 patients between the age of 80 and 89, 24 were asymptomatic (1). Comparable results are published from a SARS-CoV-2 outbreak in an American skilled nursing home as well: more than 50 % of the residents with positive tests were asymptomatic at the time of testing (2).
Residents in nursing wards not affected by COVID-19
In consultation with the Zurich City Council and the Department of Health of the Canton of Zurich, another cohort test was conducted before Easter. The plan was to test all residents in wards that had not been affected, to evaluate if they also presented a high number of asymptomatic COVID-19-cases. However, due to the high number of residents, it was decided to go forward with a two-stage approach. In a first step, only not affected wards in nursing homes with COVID-19-cases were tested. This included 19 wards with a total of 320 residents. All results were negative. We subsequently refrained from testing the rest of the nursing homes. It can be assumed that it is highly unlikely that there will be asymptomatic carriers in wards without COVID-19-cases.
With respect to our findings of the high proportion of asymptomatic residents tested positive the Department of Health of the Canton of Zurich and the Federal Office of Public Health adapted the testing policy for elderly people living in nursing homes.
In the course of the COVID-19-pandemic we observed no further outbreak. Until mid of May only few more residents were tested positive. In total 121 out of 1600 residents have been tested positive, 51 of them died.
Since during the cohort testing beginning of April in nursing home A, 10 out of 64 staff tested positive in the cohort testing; in nursing home B, 3 out of 90 tested positive. As an immediate measure, the enforcement of social distancing measures during meals, smoking and in changing rooms were stepped up: e. g. food in the nursing homes’ restaurants is collected while wearing a mask and eaten outside with ample distance. The exact path of infection could not be determined yet. During the whole pandemic period in total 108 employees have been identified as SARS-CoV-2 positive. Three of them suffered from severe symptoms and needed hospital care.
Conclusion
In nursing homes, where social distancing can only be insufficiently implemented, the virus will spread rapidly. Only by systematic isolation of virus carriers, the spread can be contained. To this end, virus carriers have to be identified. Even among symptomatic patients, many do not meet the test criteria set out by the FOPH and many of them only present with subfebrile temperature. 40 % of virus carriers are asymptomatic upon diagnosis. Therefore, broad testing is necessary in nursing home wards in case of COVID-19 infections, in order to facilitate effective isolation measures. In that process, all possible contacts of the COVID-19-cases have to be included. In a nursing home this includes, at the minimum, all residents of the same nursing ward.
This approach is worth the effort, due to the high lethality because of the COVID-19 virus in nursing homes. Due to the highly vulnerable population in nursing homes, PZZ is regretfully showing a lethality of COVID-19 around 40 % in its institutions, which is significantly higher than that in the average general population of the same age.
For comparison: We know from Italy, that mortality significantly rises with the increase of age. In the age group between 79 and 79 years, 12.6 % die. This increases to 19.7 % with people aged 80 to 89, and to 22.9 % with the very elderly (≥90 years old) (3).
Conflict of interest: none
References
1. Mizumoto K, Kagaya K, Zarebski A, Chowell G. Estimating the asymptomatic propor-tion of coronavirus disease 2019 (COVID-19) cases on board the Diamond Princess cruise ship, Yokohama, Japan, 2020, Euro Surveill. 2020;25(10):pii=2000180.
2. Arons MM, Hatfield KM, Reddy SC, Kimball A, James A, Jacobs JR et al. Presympto-matic SARS-CoV-2 Infections and Transmission in a Skilled Nursing Facility, NEJM, DOI: 10.1056/NEJMoa2008457
3. Livingston E, Bucher K. Coronavirus disease 2019 (COVID-19) in Italy. JAMA 2020