L. Bavelaar1, H.T.A. van der Steen2,3, H. de Jong1, G. Carter4, K. Brazil4, W.P. Achterberg1, J.T. van der Steen1,5
1. Department of Public Health and Primary Care, Leiden University Medical Center, Leiden, the Netherlands; 2. Department of Radiology, Leiden University Medical Center, Leiden, the Netherlands; 3. Faculty of Science, University of Amsterdam, Amsterdam, the Netherlands; 4. School of Nursing and Midwifery, Queen’s University Belfast, Belfast, Northern Ireland, United Kingdom; 5. Department of Primary and Community Care, Radboud university medical center, Nijmegen, the Netherlands. Corresponding author: Jenny T. van der Steen, Department of Public Health and Primary Care, Leiden University Medical Center, Leiden, the Netherlands, jtvandersteen@lumc.nl
Jour Nursing Home Res 2021;7:23-31
Published online June 18, 2021, http://dx.doi.org/10.14283/jnhrs.2021.5
Abstract
Background: The literature indicates that palliative care for people with dementia needs to be enhanced. Objectives: To assess barriers to providing high-quality palliative dementia care and potential solutions to overcome these barriers, as perceived by physicians responsible for end-of-life care with dementia. Design: Cross-sectional study. Setting: The Netherlands. Participants: A representative sample of 311 elderly care physicians of whom 67% (n=207) responded. Measurements: A postal survey in 2013 containing open-ended items probing for barriers in the elderly care physicians’ practices and possible solutions. Answers were coded and grouped using qualitative content analysis and presented to expert physicians in 2021. Results: Barriers to palliative care in dementia were (1) beliefs held by family, healthcare professionals or the public that are not in line with a palliative care approach, (2) obstacles in recognizing and addressing care needs, (3) poor interdisciplinary team approach and consensus, (4) limited use or availability of resources, and (5) poor family support and involvement. Suggested solutions were improving communication and information transfer, and educating healthcare staff, families and the public about palliative care in dementia. Timely and frequent communication with the family, including advance care planning, and more highly skilled nursing staff were also proposed as solutions. Conclusions: The results suggest a strong need for ongoing education for healthcare professionals about palliative dementia care. Strengthening interprofessional collaboration and shared responsibility for advance care planning is also key. Increasing public awareness of the dementia trajectory and the need for a proactive approach call for a broader societal agenda setting.
Key words: Dementia, geriatrics, nursing homes, palliative care.
Introduction
As the number of people living and dying with dementia increases, dementia has been declared a public health priority (1). Because dementia is a terminal disease, a palliative care approach is appropriate in principle. In 2014, the European Association for Palliative Care (EAPC) published a white paper (2) that provided evidence- and expert consensus-based recommendations to guide clinical practice and policy in shaping palliative care in dementia. However, palliative and end-of-life care in dementia are still perceived to be suboptimal according to family and healthcare professionals because the recommendations are not always implemented (3-5). Improving care and services for people with dementia and their families is thus necessary.
The majority of people with dementia in the Netherlands die in nursing homes, estimates vary by setting of sampling between 70% (6) and 93% (7). Nursing home teams in the Netherlands are multidisciplinary teams, supervised by elderly care physicians who carry the primary responsibility for the care of nursing home residents (8, 9). The Netherlands is unique in having these care (instead of cure) oriented physicians as staff who have received specialist education in geriatrics, dementia and palliative care (8). Compared to, for example, the United States, it is more common in the Netherlands that physicians decide, together with the family, to withhold curative treatment and focus on achieving a goal of comfort for nursing home residents with dementia (10). Specialized palliative care teams are mostly serving hospital and hospice settings and are rarely called upon for nursing home residents with dementia (11).
Due to their significant role and expertise in providing end-of-life care for people with dementia, elderly care physicians are key informants as to why implementation of palliative care in dementia is still suboptimal and how to address these barriers. The main question we address in this study is: What are the barriers to providing high-quality palliative care in dementia in the Netherlands according to elderly care physicians, and what solutions do they propose to address these barriers?
Methods
Participants and procedure
This study was part of a larger cross-sectional survey in the Netherlands and Northern Ireland (12-14) from which we present the Dutch qualitative data. A representative sample of elderly care physicians in the Netherlands participated in a postal survey in 2013. We used systematic random sampling by e-mailing a self-administered postal survey to every fourth elderly care physician from an alphabetical list of the 1248 members of the Dutch Association of Elderly Care Physicians and Social Geriatricians (Verenso). This member list includes more than 80% of Dutch registered elderly care physicians. The inclusion criteria were: (i) experience with end-of-life care for people living with dementia and (ii) practicing at Autumn 2012. Two reminders and a prize draw to win a 100-euro gift card were used to maximize responses.
The survey contained a quantitative evaluation of the priorities of elderly care physicians in the end-of-life care for people with dementia (see Additional file 1). Its components were based on the EAPC white paper recommendations domains (Box 2 in (2)). Additionally, the survey included an open-ended item, asking:
“Finally, in your opinion, what are the three most significant barriers to providing good quality palliative care in dementia in your practice, and importantly, how would you suggest these barriers are best addressed?”.
In February 2021, we presented the most frequent pairs of barriers and solutions that emerged from this survey to expert elderly care physicians with a minimum of three years of experience in caring for people living with dementia, and who were affiliated with an academic center in the role of teacher, supervisor or researcher. They were asked to indicate whether the results were still relevant and up-to-date, soliciting for additional comments.
Data management and analysis
The responses were analysed using conventional content analysis (15, 16) in Atlas.ti (version 7.5.10, 2015) and Excel. First, all responses were read and reread to gain familiarization with the barriers and solutions mentioned by the respondents. Next, codes were created from the data based on the specific barriers and solutions identified. Because there was no one-to-one relation, proposed solutions were coded separately from the barriers to maintain meaningful differentiation between the categories and codes for both solutions and barriers. To ensure validity and rigor (17), codes developed by LB (PhD student trained in quantitative and qualitative methods) were peer checked by HJ (elderly care physician) and HS (BSc student trained in quantitative and qualitative methods). Finally, codes were reviewed and grouped into larger categories inspired by the literature (14, 18) and based on discussions between the researchers (LB; HS; JS, associate professor in end-of-life care). Codes were quantified to describe the frequency of their occurrence.
Codes were developed in the original language (Dutch) and translated to English for reporting. Quotations used to support findings were translated to English by a professional translator as recommended (19).
Ethical procedure
The Medical Ethics Review Committee of the VU University Medical Center approved the survey as part of series of studies on end of life in nursing homes (2010/157; 14 June 2010). Consent was implied with receiving a completed questionnaire. Returned surveys were pseudonymized with a numbering system. The expert physicians were informed of the purpose of the study and consented to use their evaluation and relevant demographics (gender and experience) for publication while not personally identifiable in the report.
Results
Characteristics of respondents
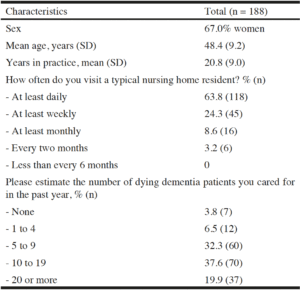
A response rate of 67% was achieved with 207 out of 311 self-complete postal surveys returned. Nineteen were excluded from analysis because the physicians did not meet the inclusion criteria of experience with end-of-life care (n = 13) or currently practicing (n = 6). Of the included 188 respondents, 171 mentioned one to four barriers and associated solutions. The majority of the elderly care physicians was female, visited their residents daily and had lost more than one resident with dementia in the past year (Table 1). The demographics of the respondents correspond with the entire population of elderly care physicians in the Netherlands (mean age: 48.4, percentage women: 64%; (20)) and we assume that the respondents are geographically representative of the entire population, as this was the case in a study conducted at the same time using the same sampling approach (21).
Barriers
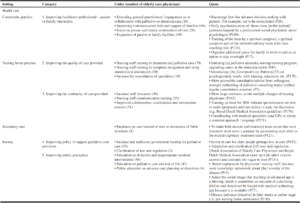
The barriers to providing good quality palliative care in dementia were clustered into five categories (cf. (14)) and are listed in Table 2 in order of frequency together with the underlying codes and example quotes.
1. Beliefs and lack of knowledge, awareness or understanding. A perceived lack of knowledge about dementia and palliative care appeared to be the most prominent barrier according to the elderly care physicians. Consequently, families, hospital doctors, nursing staff, and the public did not see the need for a palliative approach for people with dementia.
2. Obstacles in recognizing and addressing care needs. The respondents mentioned difficulties in identifying and managing decline, discomfort, and diagnosing and managing dementia in general. The start of the palliative phase was often recognized late. Additionally, care goals or treatment plans were not documented or vague.
3. Poor interdisciplinary team approach and consensus. The elderly care physicians indicated that care was not continuous because of high staff turnover, poor information transfer, and poor collaboration between healthcare professionals. This could delay starting palliative care. Moreover, the respondents stated that palliative care terminology was used inconsistently, and uncertainty remained about what a palliative care approach entailed.
4. Limited use or availability or resources. The next most frequently mentioned barrier was limited staff resources. Elderly care physicians often mentioned a lack of time and poor staffing to negatively impact the care provided.
5. Poor family support and involvement. The respondents indicated that frequently family did not feel ready to part with their relative-hence resisting palliative care. Underlying this resistance was insufficient support for families, as elderly care physicians and the nursing staff were not able to timely discuss the end of life. Further, family and nursing home staff sometimes disagreed about the quality of life of the person with dementia.
Proposed solutions
Table 3 shows five clusters of solutions that the respondents proposed for various barriers. First, we discuss three clusters in chronological order of patient transitions across care settings. Next, we present two clusters that address barriers at a broader, societal level.
Healthcare
Improving healthcare professional – patient or family interaction
Starting in community practice, the elderly care physicians proposed a stronger involvement of general practitioners (GPs) in palliative or dementia care. The respondents called for an early start of patient support, dementia diagnosis and advance care planning (ACP), to prevent emergency actions in nursing homes. This was most frequently mentioned as a solution for a lack of continuity of care, palliative care or dementia knowledge, and resources.
Transitioning to nursing home practice, the respondents stated that improved communication and family support could be a solution to the suggested barriers. Nursing home staff needed to increase the frequency of their conversations with family and provide counseling (“psychoeducation”). Together with timely conversations about end of life and an early start of ACP, this could assist families in accepting or understanding their relative’s prognosis, and to recognize palliative care as an appropriate approach. Potentially, this would ameliorate disagreements between family and nursing home staff.
Further, nursing home staff should focus more on person and family-centered care. This includes attention for spiritual care and providing compassionate care, with an emphasis on social and emotional bonding, and less on a medical approach. It was suggested that nursing home staff should engage family in daily care tasks and improve their interaction with other cultures. This was highlighted in case of limited resources, obstacles in recognizing and addressing care needs and poor family involvement. Finally, respondents proposed to expand facilities, activities or services for patients and families to facilitate family support and involvement.
Improving the quality of care provided
In nursing home practice, barriers to palliative dementia care could by countered by nursing staff receiving specific training in palliative care. Many respondents suggested that multidisciplinary training could enhance palliative care knowledge and overcome several barriers related to limited staff resources and a lack of consensus about palliative care terminology.
Another important solution proposed by many elderly care physicians was to train nursing staff in symptom recognition and in using standardized instruments, such as pain observation scales and the Liverpool Care Pathway (22). If correctly used as a supportive tool and not as a ‘protocol’, the respondents believed that this could help improve recognizing and addressing care needs, and increase staff knowledge about dementia and palliative care.
Both barriers could also be countered if nursing staff were able to consult a specialist, and if elderly care physicians consulted peers. The respondents further suggested that consulting a specialist or specializing staff could improve continuity in practice, although some, both in the survey and expert consultation, regarded themselves palliative care specialists.
Improving the continuity of care provided
To improve the continuity of care in the nursing homes, many elderly care physicians suggested to increase staff resources. More staff and decreased (administrative) workload would reduce lack of time. Additionally, investing in having the same healthcare professional attending the same patient and family would facilitate relationships and improve acceptance of dementia diagnosis or prognosis.
Another proposed solution to increase continuity was to provide further training for nursing home staff in communication to facilitate initiating or conducting end-of-life conversations and ACP. This would also help connect with family and enhance the quality of information transfer between healthcare professionals. Specifically, a clear use of terminology was needed. This could improve families’ and staff’s knowledge and acceptance of appropriateness of palliative care in dementia.
Many respondents proposed improved collaboration, coordination and information transfer, both within nursing home practice and in transfers to and from secondary care. This could address barriers related to lack of continuity in care or personnel, misunderstandings between healthcare professionals, and to obstacles in recognizing and addressing care needs. In particular, multidisciplinary meetings and collaboration were considered key, also to support ACP. Respondents also suggested to specifically improve collaboration between nursing home staff and medical specialists. Hospital doctors (and GPs) were suggested to benefit from nursing home staff’s expertise in providing good care for people living with dementia. This could foster continuity in care and ameliorate problems with overtreatment.
In relation to the latter, the elderly care physicians proposed to have more discussions about futile treatment and focus on care rather than cure. This could also help overcome disagreements about care goals between healthcare professionals, within the nursing home and in the interaction with hospital doctors.
Society
In addition to specific changes of healthcare, the elderly care physicians proposed more general solutions to address barriers for palliative dementia care at a broader, societal level.
Improving policy to support palliative care provision
The respondents suggested that an increase and reallocation of government funding for palliative care could address barriers such as poor staffing and a lack of time, and support the enhanced education of nursing staff to increase their knowledge in palliative and dementia care. Funding could support the provision of palliative care in practice by enabling more facilities, activities or services for the patient or family.
Another policy improvement was clarification of law and regulation. This was proposed to help resolve perceived ambiguity in legislation regarding (foregoing) treatment.
Improving public perception
The elderly care physicians expressed a need for public education on palliative care and end of life. This could help address barriers to providing high-quality palliative care in dementia such as the perceived unrealistic public image of prolonging or ending life, the denial of dementia diagnosis or prognosis by some families, and the difficulties in recognizing and addressing care needs.
The respondents also proposed that public education to increase awareness around the medical futility of life-prolonging treatment in people with advanced dementia could solve a variety of barriers related to overtreatment and a lack of knowledge and acceptance. It could also diminish the stigma around dementia and myths around prolonging or ending life. Finally, public education on ACP or advance directives could be a solution for the lack of clear guidance for their practice.
Expert checking
These results from the 2013 survey were presented to 26 expert physicians in 2021, ten of whom were men and the average years of experience in caring for people living with dementia was 19.6 years. All barriers and solutions were indicated to still be relevant by at least 12 physicians (range: 12-25 confirmations per barrier and solution). The barriers and solutions related to the availability of resources, information transfer, and symptom recognition and control were endorsed by the lowest numbers of physicians (13, 16 and 12, respectively). Nearly all physicians endorsed the barriers and solutions related to palliative dementia care knowledge (n = 25) and family support (n = 22).
Discussion
Dutch elderly care physicians see most people living with dementia in the last phase of their life as they are responsible for providing nursing home care and most people with dementia in the Netherlands die in a nursing home. Specialist training supports their competency; the Netherlands is a country where withholding curative treatment based on quality-of-life care goals is more common than elsewhere (10). Therefore, we expected this particular setting to be promotive of palliative and end-of-life care provision to person with dementia. Yet, this representative sample of elderly care physicians raised a variety of barriers to providing high-quality palliative care in dementia.
Interestingly, the barriers perceived by the elderly care physicians mirror the barriers reported in international literature (e.g. (18)). Apparently, having a skilled elderly care physician on the staff of nursing homes is not enough to overcome these barriers to high-quality palliative care. Families having insufficient awareness of the terminal nature of dementia and a poor understanding of palliative care (23-25) still remain as barriers, causing families to resist a palliative approach and insisting on curative treatment. Also continuity of care is not assured. A strong upstream orientation to palliative care that addresses palliative care early on is missing (26). GPs would not usually discuss palliative care and ACP when their patients with dementia were still able to contribute. Living wills that elderly care physicians can use to guide treatment and thus provide continuity in care remain uncommon. In addition, the extended palliative phase in dementia is not being recognized by all healthcare professionals (27). The elderly care physicians reported that hospital doctors did not consider the dementia of their patients in the treatment plans. Continuity of palliative care was therefore disrupted upon hospitalization.
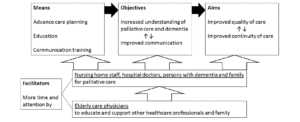
A broader support base for palliative care is thus required and this refers to all involved in caring for people living with dementia: families, GPs, hospital doctors and nurses. Figure 1 visualizes the solutions that the elderly care physicians proposed to overcome these barriers. To improve the quality and continuity of palliative care in dementia (overall aims), increased understanding of palliative care and dementia and improved communication is needed (objectives). The means necessary to achieve increased understanding and improved communication are ACP, education and communication training. With their expertise, elderly care physicians function as the key consultants to facilitate this process, supported by palliative care specialists. Rather than have healthcare professionals refer cases to the elderly care physician or palliative care specialists, this means that elderly care physicians and palliative care specialists need to support GPs, hospital doctors and nursing staff in providing palliative dementia care themselves. It is thus important that consulting a specialist in palliative dementia care does not reinforce the lack of support for palliative dementia care in certain healthcare settings.
Public education on palliative care has been labeled a key priority by international experts to support integrated palliative care (28) and several studies found a positive effect on palliative care delivery (29-31). The effectiveness of education on dementia, however, remains unclear (32). This is why improving communication that was frequently proposed is an important solution. Families want more information about dementia, preferably provided by healthcare professionals that follow-up on this information (33). Communication between healthcare providers and families is thus important to educate families. In addition, ACP, if perceived as an ongoing dialogue, can serve as a means to support education and communication. This ongoing dialogue is further important as families need repeated information about their relative’s condition and palliative care options to foster acceptance (34). Timely discussions of death and dying are important in orienting families to palliative care (35). To support an early start of ACP, the physicians called for public education on ACP or advance directives, end of life and the lack of added value of curative medical treatments in advanced dementia. Moreover, families, nurses and physicians should use consistent language in ACP.
In addition to pointing to complexities around families not being on the same page, many solutions targeted nursing staff. Nurses are especially important to address barriers to providing high-quality palliative care that are specific to dementia: difficulties in assessing discomfort and the start of the dying phase (36). Having an elderly care physician on the staff does not suffice, as proper assessment involves continuous monitoring. Nursing staff are in a better position to perform this. Continuous monitoring requires time, training and communication with team members. However, the elderly care physicians stated that there was a lack of time and poor staffing levels, as frequently observed before (18), causing high workload. In addition, they expressed a lack of trust in nursing staff being sufficiently equipped to deliver high-quality palliative care. Nurses indeed express difficulties in recognizing and addressing care needs (37). Training in using tools is therefore necessary (38) and was often suggested by the elderly care physicians. This training should underline the use of the tools as supportive instruments and not as standardized protocols or as a tick box approach, to retain a person-centered approach. This specific issue was also raised by one of the respondents.
There are some limitations of this study. Brief answers to the open-ended survey items complicated interpretation and elaboration could not be sought. Another limitation is the time between data collection (2013) and reporting. This could affect the relevance of the results. However, the findings were considered to be relevant-and the interpretation of answers appropriate-as the perceived barriers and proposed solutions were confirmed by expert physicians in 2021. Additionally, developments in nursing home care in the years following data collection (39) lead us to believe that the barriers were stable or even increasing. For example, nursing home staff was found to feel less competent. A strength of this study is the inclusion of a large and representative sample of elderly care physicians and the two-stage approach, adding expert views. The representative sample led to the inclusion of more women than men in this study, as the proportion of women working in nursing home care in the Netherlands is higher than in medical specialist care (40). Future research could investigate if men and women in healthcare experience different barriers to palliative dementia care.
In conclusion, elderly care physicians in the Netherlands experience several barriers to providing high-quality palliative care in dementia. The current study suggests a strong need for specialist training of nursing staff, stronger networks between healthcare professionals to ensure continuity of care, and raising public awareness in the domains of dementia, palliative care, ACP and end of life. Palliative dementia care is shared care as families, nurses and physicians all have a role to play. Better education could overcome barriers in several contexts: both in nursing homes and in society.
Funding: The study in the Netherlands was supported by the Aspasia supplement to a career award for JS provided by the Netherlands Organization for Scientific Research (NWO; Innovational Research Incentives Scheme) Vidi grant number 91711339. Analyses were part of an EU Joint Programme – Neurodegenerative Disease Research (JPND) project. This project is supported in the Netherlands through the Netherlands Organisation for Health Research and Development (ZonMw) program Memorabel grant number 733051084 under the aegis of the EU Joint Programme – Neurodegenerative Disease Research (JPND) – www.jpnd.eu. The sponsors had no role in the design and conduct of the study; in the collection, analysis, and interpretation of data; in the preparation of the manuscript; or in the review or approval of the manuscript.
Acknowledgements: Special thanks to the elderly care physicians who completed the surveys and the expert physicians who checked the results. The authors would like to thank Dr. Tamara Sussman for reviewing an earlier version of the manuscript.
Conflict of interest: The authors declare that they have no competing interests.
References
1. World Health Organization (WHO). Dementia: a public health priority. Report. Alz Dis Int, 2012.
2. Van der Steen, J.T., Radbruch, L., Hertogh, C.M.P.M., et al. White paper defining optimal palliative care in older people with dementia: a Delphi study and recommendations from the European Association for Palliative Care. Palliat Med 2014; 28: 197-209.
3. Ten Koppel, M., Onwuteaka-Philipsen, B.D., Van Den Block, L., et al. Palliative care provision in long-term care facilities differs across Europe: results of a cross-sectional study in six European countries (PACE). Palliat Med 2019; 33: 1176-1188.
4. Cohen, L.W., van der Steen, J.T., Reed, D., et al. Family perceptions of end-of-life care for long-term care residents with dementia: Differences between the United States and the Netherlands. J Am Geriatr Soc 2012; 60: 316-322.
5. Miranda, R., Bunn, F., Lynch, J., Van Den Block, L., Goodman, C. Palliative care for people with dementia living at home: a systematic review of interventions. Palliat Med 2019; 33: 726-742.
6. Joling, K., van der Heide, I., Verheij, R., Francke, A., van Hout, A. Infographic. Zorgtrajecten van mensen met dementie in kaart: resultaten van het BESIDE project [Infographic. Mapping care trajectories of people with dementia: results of the BESIDE project]. 2019. Nivel, Utrecht.
7. Houttekier, D., Cohen, J., Bilsen, J., Addington-Hall, J., Onwuteaka-Philipsen, B.D., Deliens, L. Place of death of older persons with dementia. A study in five European countries. J Am Geriatr Soc 2010; 58: 751-756.
8. Koopmans, R.T.C.M., Pellegrom, M., Van der Geer, E.R. The Dutch move beyond the concept of nursing home physician specialists. J Am Med Dir Assoc 2017; 18: 746-749.
9. Schols, J.M.G.A.; Crebolder, H.F.J.M.; Van Weel, C. Nursing home and nursing home physician: the Dutch experience. J Am Med Dir Assoc 2004; 5: 207-212.
10. Van der Steen, J.T., Kruse, R.L., Ooms, M.E., et al. Treatment of nursing home residents with dementia and lower respiratory tract infection in the United States and The Netherlands: an ocean apart. J Am Geriatr Soc 2004; 52: 691-699.
11. Van der Steen, J.T., Deliens, L., Koopmans, R.T.C.M., Onwuteaka-Philipsen, B.D. Physicians’ perceptions of suffering in people with dementia at the end of life. Palliat Support Care 2017; 15: 587-599.
12. Van der Steen, J.T., Galway, K., Carter, G., Brazil, K. Initiating advance care planning on end-of-life issues in dementia: Ambiguity among UK and Dutch physicians. Arch Gerontol Geriatr 2016; 65: 225-230.
13. Brazil, K., Galway, K., Carter, G., Van der Steen, J.T. Providing optimal palliative care for persons living with dementia: a comparison of physician perceptions in the Netherlands and the United Kingdom. J Palliat Med 2017; 20: 473-477.
14. Carter, G., Van der Steen, J.T., Galway, K., Brazil, K. General practitioners’ perceptions of the barriers and solutions to good-quality palliative care in dementia. Dementia 2017; 16: 79-95.
15. Hsieh, H.F., Shannon, S.E. Three approaches to qualitative content analysis. Qual Health Res 2005; 15: 1277-1288.
16. Crowe, M., Inder, M., Porter, R. Conducting qualitative research in mental health: Thematic and content analyses. Aust N Z J Psychiatry 2015; 49: 616-623.
17. Morse, J.M. Critical analysis of strategies for determining rigor in qualitative inquiry. Qual Health Res 2015; 25: 1212-1222.
18. Mataqi, M., Aslanpour, Z. Factors influencing palliative care in advanced dementia: a systematic review. BMJ Support Palliat Care 2020; 10: 145-156.
19. Van Nes, F., Abma, T., Jonsson, H., Deeg, D. Language differences in qualitative research: is meaning lost in translation? Eur J Ageing 2010; 7: 313-316.
20. Capaciteitsorgaan. Capaciteitsplan 2013. Deelrapport 5, Specialist Ouderengeneeskunde. [Advisory Committee on Medical Manpower Planning 2013. Sub-report 5, Elderly Care Physicians]. 2013. Capaciteitsorgaan, Utrecht.
21. Gijsberts, M-HJE, van der Steen, J.T., Hertogh, C.M.P.M., et al. Spiritual care provided by nursing home physicians: a nationwide survey. BMJ Support Palliat Care 2019; 0: 1-9.
22. Klapwijk, M. S., Dekker, N. L., Caljouw, M. A., et al. Experiences with the Liverpool care pathway for the dying patient in nursing home residents: a mixed-method study to assess physicians’ and nurse practitioners’ perceptions. BMC Palliat Care 2020; 19: 1-11.
23. Gabbard, J., Johnson, D., Russell, G. et al. Prognostic awareness, disease and palliative understanding among caregivers of patients with dementia. Am J Hosp Palliat Care 2020; 37: 683-691.
24. Robinson, A., Eccleston, C., Annear, M., et al. Who knows, who cares? Dementia knowledge among nurses, care workers, and family members of people living with dementia. J Palliat Care 2014; 30: 158-165.
25. Van der Steen, J.T., Onwuteaka-Philipsen, B.D., Knol, D.L., Ribbe, M.W., Deliens, L. Caregivers’ understanding of dementia predicts patients’ comfort at death: a prospective observational study. BMC Med 2013; 11: 1-12.
26. Sawatzky, R., Porterfield, P., Lee, J., et al. Conceptual foundations of a palliative approach: a knowledge synthesis. BMC Palliat Care 2016; 15: 1-14.
27. Hanson, E., Hellström, A., Sandvide, A., et al. The extended palliative phase of dementia–An integrative literature review. Dementia 2019; 18: 108-134.
28. Payne, S., Hughes, S., Wilkinson, J. Hasselaar, J., Preston, N. Recommendations on priorities for integrated palliative care: transparent expert consultation with international leaders for the InSuP-C project. BMC Palliat Care 2019; 18: 32.
29. Brazil, K., Carter, G., Cardwell, C., et al. Effectiveness of advance care planning with family carers in dementia nursing homes: a paired cluster randomized controlled trial. Palliat Med 2018; 32: 603-612.
30. Di Giulio, P., Finetti, S., Giunco, F., et al. The impact of nursing homes staff education on end-of-life care in residents with advanced dementia: a quality improvement study. J Pain Symptom Manage 2019; 57: 93-99.
31. Arcand, M., Monette, J., Monette, M., et al. Educating nursing home staff about the progression of dementia and the comfort care option: impact on family satisfaction with end-of-life care. J Am Med Dir Assoc 2009; 10: 50-55.
32. Moore, K.J., Lee, C.Y., Sampson, E.L., Candy, B. Do interventions that include education on dementia progression improve knowledge, mental health and burden of family carers? A systematic review. Dementia 2019, 1471301219831530.
33. Thompson, G., Hack, T., Rodger, K., St John, P., Chochinov, H., McClement, S. Clarifying the information and support needs of family caregivers of nursing home residents with advancing dementia. Dementia 2020, 1471301220927617.
34. Gonella, S., Basso, I., Dimonte, V., et al. Association between end-of-life conversations in nursing homes and end-of-life care outcomes: A systematic review and meta-analysis. J Am Med Dir Assoc 2019; 20: 249-261.
35. Stirling, C., McInerney, F., Andrews, S., et al. A tool to aid talking about dementia and dying–development and evaluation. Collegian 2014; 21: 337-343.
36. Sachs, G.A., Shega, J.W., Cox-Hayley, D. Barriers to excellent end-of-life care for patients with dementia. J Gen Intern Med 2004; 19: 1057-1063.
37. Bolt, S.R., van der Steen, J.T., Schols, J.M.G.A., Zwakhalen, S.M.G., Pieters, S., Meijers, J.M.M. Nursing staff needs in providing palliative care for people with dementia at home or in long-term care facilities: A scoping review. Int J Nurs Stud 2019; 96: 143-152.
38. De Witt Jansen, B., Brazil, K., Passmore, P., et al. “A tool doesn’t add anything”. The importance of added value: Use of observational pain tools with patients with advanced dementia approaching the end of life—a qualitative study of physician and nurse experiences and perspectives. Int J Geriatr Psychiatry 2018; 33: 1346-1354.
39. Prins, M., Heijkants, C., Willemse, B. Trends in de verpleeghuiszorg voor mensen met dementie. Monitor Woonvormen Dementie 2008-2017. [Trends in nursing home care for people with dementia. Monitor Residency Types Dementia 2008-2017]. 2018. Trimbos-instituut, Utrecht.
40. Velden, L.F.J. van der, Hingstman, L., Heiligers, P.J.M., Hansen, J. Toenemend percentage vrouwen in de geneeskunde: verleden, heden en toekomst. [Increasing percentage of women in medicine: past, present and future]. Ned Tijdschr Geneeskd; 2008, 152: 2165- 2171.