M.M.T.J. Broekman1, J. de Vos2, L. de Vijlder1, M. Brundel1
1. Elderly care physician, Beweging 3.0, Amersfoort, The Netherlands; 2. Department of primary and community care, Radboud University Medical Center, Nijmegen, The Netherlands. Corresponding author: Mark M.T.J. Broekman, Elderly care physician, Beweging 3.0, Beweging 3.0, Postbus 1599, 3800 BN Amersfoort, The Netherlands. E-mail: broekmanmark@gmail.com, ORCID: 0000-0001-5523-2771
Jour Nursing Home Res 2021;7:62-64
Published online September 23, 2021, http://dx.doi.org/10.14283/jnhrs.2021.10
Abstract
Purpose: In very frail nursing home residents transport to the hospital for diagnostics in case of a suspected hip fracture might be considered too burdensome or not desirable. We aimed to elucidate the prognosis and disease course for this group. Methods: We performed a retrospective cohort study between 2017 and 2020 in a nursing home in the Netherlands. All patients with a suspected hip fracture were eligible. The main exclusion criteria was transport to the hospital for diagnostics. Our primary outcome is survival after one month. Results: 23 patients fulfilled the inclusion criteria. Median age was 84 years. Almost all patients had severe dementia. After one month 20 patients (87%) had died. Median survival was 5 days (interquartile range 3-8). Conclusion: In the most frail nursing home residents with a suspected hip fracture the prognosis is very poor with a median survival of only 5 days.
Key words: Non-operative, conservative, hip fracture, long term care facility, nursing home, frailty, elderly.
Introduction
For residents of long term care facilities mortality rates after a hip fracture with surgical treatment vary between 20-55% after 6 months (1, 2). The high mortality rate follows from significant physical and cognitive comorbidity leading to an increased risk of complications after surgery (3, 4). Moreover, there is a significant decline in mobility and quality of life after a hip fracture (5).
Surgery is considered the treatment of choice. It is associated with a better prognosis and pain relief (6, 7). However, because of the poor prognosis and high complication rate of surgery, a conservative treatment is increasingly considered in frail patients with extensive comorbidity, including dementia (8). Historically, conservative treatment of a hip fracture included traction therapy, however nowadays it merely comprises the administration of sufficient painkillers and early mobilization when feasible. A large study showed a mortality of 53,8 % after six months in nursing home residents with advanced dementia and a radiological conformed hip fracture treated conservatively (9).
In daily practice, there is a significant group of very frail nursing home residents for whom even transport to the hospital for diagnostics is considered too burdensome. This group is not included in previous studies exploring mortality with conservative treatment. It would be of great value to gain more insight in their prognosis. Though not radiological confirmed, we aimed to elucidate the disease course of nursing home residents with a clinical suspicion of a hip fracture with a conservative treatment.
Methods
Design
We performed a single center retrospective cohort study in the long term care facility Beweging 3.0 in the region of Amersfoort, the Netherlands.
Patient identification
All patients with a clinical suspicion of a hip fracture as diagnosed by the treating physician for whom a conservative treatment was initiated were eligible. Patients were identified by screening the daily reports. Daily reports were screened from end 2017 till March 2020 (because from March 2020 the covid pandemic might have influenced the decision to admit a patient to the hospital.) A clinical suspected hip fracture is typically characterized by severe pain or swelling in the groin, the leg is held in external rotation and the leg appears shortened. Exclusion criteria were transport to the hospital for diagnostics with or without subsequent surgery, transfer to another care organization after the suspected hip fracture, and a fast functional recovery, which makes a fracture unlikely.
Data collection and statistics
One author (JV) extracted patient and clinical characteristics from the medical charts. In case of doubt findings were discussed with MB. Variables identified included age, sex, comorbidity, type of dementia. Data about mobility before as well as the best achieved mobility after the suspected hip fracture were retrieved. Drugs administered in the period after the suspected hip fracture (pain medication and sedative drugs) were verified, even as day of death. Our primary outcome is mortality within one month. Secondary outcomes are median time to death, death within two weeks, three months and six months. Descriptive analyses were performed. A survival curve was plotted to illustrate disease course. Statistical analyses were performed with SPSS version 25.0.0.1 (SPSS Inc.,Chicago, IL, USA). The study was approved by the Medical Ethics Review Committee of VU University Medical Center (Registration number 2020.448).
Results
Patient characteristics
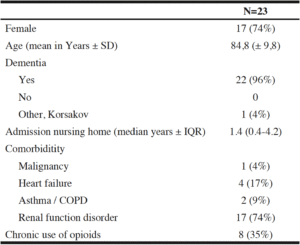
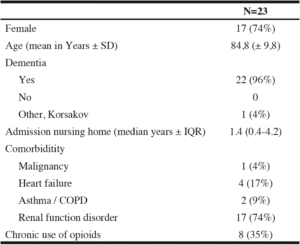
Twenty-three patients were identified with a clinical suspicion of a hip fracture treated conservatively without diagnostics in the hospital. Table 1 shows the patient characteristics. The majority of patients (three out of four) was female. All patients lived in psychogeriatric homes, because of advanced dementia (22/23) or Korsakov (1/23). One patient was recently diagnosed with metastatic lung cancer.
Mobility and clinical symptoms of the hip fracture
Three patients used no walking aid, while 19/23 used a walking aid before the incident. From 21 of 23 information about typical symptoms could be retrieved. Two out of three patients had all three typical symptoms of a hip fracture (pain, external rotation, decreased length), while one out of ten had 2 out of 3 symptoms and one out of five had one typical symptom. Most patients (19/23) became fully bedridden after the hip fracture. All patients received opioids and 14/23 received sedative drugs, during the disease course. Nine patients received a urinary catheter.
Survival
One-month mortality rate was 87% . Figure 1 shows the survival curve. Median survival after the suspected hip fracture was 5 days [IQR 3-8]. Mortality after two weeks and three months was 19/23 and 22/23, respectively. In patients who became bedridden (n=19) mortality was 100% after 10 days. More typical symptoms of a hip fracture was related to a worse prognosis.
Discussion
We showed a very poor prognosis for the most frail nursing home residents with a suspected hip fracture for whom even transport to the hospital for diagnostics is considered not desirable or too burdensome. With a median survival of 5 days and a mortality rate of 87% after one month the prognosis of this group is very poor, especially in those patients who become bedridden with a 100% mortality after 10 days.
Our findings are in contrast with recent literature evaluating the prognosis of the conservative treatment of a hip fracture.(2, 6). In a comparable patient population, patients with advan ed dementia living in a nursing home, Berry et al. showed a mortality rate of 30% after one month after a hip fracture with a conservative treatment.(9) Other studies showed an one-month mortality between 25% and 64% (10, 11). In contrast to our study, all patients were sent to the hospital for diagnostics in these studies. Therefore, an explanation for the large difference is that patients in our study were more frail, either because of more advanced dementia or more severe comorbidity, compared to those patients who are considered fit enough for transport to the hospital. Another reason might be that in those studies a conservative treatment in the hospital was preferably initiated when there was an anatomically favorable fracture, which positively influences the prognosis. This is supported by the fact that all patients who became bedridden, suggesting an evident displaced fracture, deceased within 10 days. Interestingly, a recent study, evaluating the effect of a comprehensive geriatric assessment on the number of patients being treated conservatively, also showed a median survival of five days in case a conservative treatment was preferred (12). An explanation for the very poor prognosis might be that food and fluid administration is suppressed due to a combination of an already very poor functional status in combination with the administration of opioids or sedative drugs, resulting in a rapid deterioration.
Our study is unique, because we only included patients who have not been admitted in the hospital for diagnostics or surgery. Currently, there is no literature evaluating the prognosis of this group. Some limitations are inherent to our study design. No definite diagnoses can be provided and small fractures with a better prognosis might have been missed. Approximately, 15% of hip fractures are undisplaced, which fades typical symptoms (13). As nondisplaced fractures might have been missed, our population especially consisted of patients with a displaced hip fracture with a worse prognosis. In conclusion, in nursing home residents with a suspected hip fracture who are considered as very frail the prognosis is very poor, especially when patients become bedridden.
Acknowledgements: None
Funding: No funds, grants, or other support was received
Conflicts of interest: The authors have no relevant financial or non-financial interests to disclose.
Ethical standards: Ethics approval was obtained from the medical ethics review committee of VU University Medical Center (2020.448).
References
1. van de Ree CL, Gosens T, van der Veen AH, Oosterbos CJ, Heymans MW, de Jongh MA. Development and validation of the Brabant Hip Fracture Score for 30-day and 1-year mortality. Hip Int. 2020;30(3):354-62.
2. Loggers SAI, Van Lieshout EMM, Joosse P, Verhofstad MHJ, Willems HC. Prognosis of nonoperative treatment in elderly patients with a hip fracture: A systematic review and meta-analysis. Injury. 2020;51(11):2407-13.
3. Smith T, Pelpola K, Ball M, Ong A, Myint PK. Pre-operative indicators for mortality following hip fracture surgery: a systematic review and meta-analysis. Age Ageing. 2014;43(4):464-71.
4. Berry SD, Samelson EJ, Bordes M, Broe K, Kiel DP. Survival of aged nursing home residents with hip fracture. J Gerontol A Biol Sci Med Sci. 2009;64(7):771-7.
5. Hannan EL, Magaziner J, Wang JJ, Eastwood EA, Silberzweig SB, Gilbert M, et al. Mortality and locomotion 6 months after hospitalization for hip fracture: risk factors and risk-adjusted hospital outcomes. JAMA. 2001;285(21):2736-42.
6. van de Ree CLP, De Jongh MAC, Peeters CMM, de Munter L, Roukema JA, Gosens T. Hip Fractures in Elderly People: Surgery or No Surgery? A Systematic Review and Meta-Analysis. Geriatr Orthop Surg Rehabil. 2017;8(3):173-80.
7. Neuman MD, Silber JH, Magaziner JS, Passarella MA, Mehta S, Werner RM. Survival and functional outcomes after hip fracture among nursing home residents. JAMA Intern Med. 2014;174(8):1273-80.
8. Meijer-Schafrat EC, Janssens JF, van Delden JJ, Achterberg WP. [Hip fracture in patients with dementia: surgery is not always the best alternative]. Ned Tijdschr Geneeskd. 2012;156(45):A5237.
9. Berry SD, Rothbaum RR, Kiel DP, Lee Y, Mitchell SL. Association of Clinical Outcomes With Surgical Repair of Hip Fracture vs Nonsurgical Management in Nursing Home Residents With Advanced Dementia. JAMA Intern Med. 2018;178(6):774-80.
10. Frenkel Rutenberg T, Assaly A, Vitenberg M, Shemesh S, Burg A, Haviv B, et al. Outcome of non-surgical treatment of proximal femur fractures in the fragile elderly population. Injury. 2019;50(7):1347-52.
11. Chlebeck JD, Birch CE, Blankstein M, Kristiansen T, Bartlett CS, Schottel PC. Nonoperative Geriatric Hip Fracture Treatment Is Associated With Increased Mortality: A Matched Cohort Study. J Orthop Trauma. 2019;33(7):346-50.
12. van der Zwaard BC, Stein CE, Bootsma JEM, van Geffen H, Douw CM, Keijsers C. Fewer patients undergo surgery when adding a comprehensive geriatric assessment in older patients with a hip fracture. Arch Orthop Trauma Surg. 2020;140(4):487-92.
13. Parker M, Johansen A. Hip fracture. BMJ. 2006;333(7557):27-30.