D.S. Mack1, J. Tjia1, K.L. Lapane1
1. Division of Epidemiology, Department of Population and Quantitative Health Sciences, University of Massachusetts Medical School, Worcester, MA, USA
Corresponding author: Deborah Mack, PhD, MPH,: Department of Population and Quantitative Health Sciences, University of Massachusetts Medical School, 368 Plantation Street, Worcester, MA 01605, Deborah.Mack@umassmed.edu
Jour Nursing Home Res 2022;8:1-5
Published online February 9, 2022, http://dx.doi.org/10.14283/jnhrs.2022.1
Abstract
Patients with life-limiting conditions often benefit from palliative care to improve quality of life. There is no consensus definition of the term “life-limiting illness” for the nursing home population. The objective of this paper was to provide a framework to define life-limiting illness in the nursing home population using a narrative review. PubMed and GoogleScholar were searched for terms to define: “life-limiting illness,” “serious illness,” and “end-of-life.” Based on peer-reviewed literature, we operationalized the term “life-limiting illness” in the context of the nursing home population into five domains: (1) prognosis-based definitions (i.e. <6 months), (2) mortality risk-based (i.e. high risk vs low risk), (3) healthcare service-based (i.e. receipt of palliative care consult), (4) comorbidity index-based (e.g. the Veteran’s Health Association Palliative Care Index), and (5) composite definition (i.e. comorbidity and caregiver burden).
Key words: Life-limiting illness, end-of-life, serious illness, nursing home population, palliative care.
Introduction
Palliative care services can benefit many patients approaching the end of life (1). However there does not appear to be a standardized way to define this population among a growing cohort of older adults, particularly those residing in nursing homes. Existing definitions of terms such as “serious illness” rely on identification of conditions that carry a high risk of mortality that either negatively impacts a person’s daily function or excessively strains their caregivers (2, 3). The most common of these are cancer, heart failure, chronic obstructive pulmonary disease (COPD), advanced dementia, and end-stage renal disease (4), all of which are not uncommon in nursing home residents. Using such diagnosis-based definitions in the nursing home population may overidentify the number of residents appropriate for palliative care.
Since specialized palliative care is a limited resource not widely available to institutionalized individuals, it would be helpful for clinical and research purposes to have a nursing home specific approach when defining residents with life-limiting illness.
It is projected by 2050, 22% of the world’s population will be over 60 years of age (5). Many of the oldest adults will require extensive long term care services including nursing home care. Despite the high prevalence of nursing home use across the world, the nursing home population remains understudied. While nursing homes exist across the world, the US population of nursing home residents per capita exceeds that of other countries. One in five of all US deaths occur in a US nursing home (6) where an estimated 1.4 million people reside in at any given point in time (7). Over half of all nursing home residents die within six months of admission (8). Among those that stay at least one year, the life expectancy is less than two months (8). Frailty and functional impairment are common (7), as are conditions associated with a limited life expectancy.
Palliative care and related interventions have been shown to be effective in managing patient symptoms, while also improving a patients quality of life (9–11). Specific palliative care interventions are centered around the comfort and wellbeing of a patient rather than curative treatment. This includes medication and treatment reconciliation that reduces debilitating side effects, improves pain management (both acute and chronic), establishes goals of care, offers an array of psychosocial support to both patients and their family members, and navigates care coordination among a panoply of specialists. The goal of palliative care is not to hasten mortality, but to reduce suffering and improve quality of life (12).
Furthermore, older adults are prone to overtreatment and unnecessary spending near the end of life. Healthcare spending is concentrated among high-needs and high-cost patient populations, with 6.7% of all health care expenditures occurring in the last 12 months of life (13, 14). However, spending and more severe interventions are often not associated with better quality of care, especially for those near the end of life (15–17). Nevertheless, published literature is scarce in terms of identifying those with life-limiting illness among older adults, especially for those in nursing homes. This sub-population would likely benefit from palliative care services, but many fail to be identified.
The objective of this paper was to provide a framework to conceptually and operationally define life-limiting illness in the nursing home setting using a narrative review. Having an effective way to identify this high-needs population is critical to manage advanced stage diseases and provide quality healthcare to vulnerable populations.
Conceptual Definition of Life-Limiting Illness
Our narrative review identified a tension between definitions of patients at “end of life”, with “terminal conditions”, and with “serious illness.” They are related but subtly different, and none well described in the nursing home population. A prior systematic review defining “end of life” (18) and the clinical standard for palliative care conceptually posits that life-limiting illness centers on progressive, terminal conditions with high risk of mortality and life expectancy measured in months. This is similar to the definition of “terminal condition” from the International Association for Hospice and Palliative Care (IAHPC), where “terminal condition” was defined as “a progressive condition that has no cure and that can be reasonably expected to cause the death of a person within a foreseeable future” (19). The IAHPC definition includes both malignant and nonmalignant illness and aging, and notably is not solely based on a prognosis, which some argue can be inaccurate and may leave many seriously ill patients with inappropriate care (2) since these patients may be excluded for palliative care services without a short life expectancy. This in turn could lead to the potential for prolonged suffering and diminished quality of life near the end of life. In contrast, the term “serious illness” relies on identification of conditions that carry a high risk of mortality and either negatively impacts a person’s daily function or excessively strains their caregivers (2), but this may apply to all nursing home residents since they typically have a high reliance on formal caregivers for their daily living. Acknowledging the overlapping conceptual domains of each term, this narrative review collates the operational definitions of each term into a wholistic view of life-limiting illness that can be applied to the nursing home population collectively or individually.
Operational Definitions of Life-Limiting Illness Applied to the Nursing Home Population
Our narrative review identified multiple operational definitions of life-limiting illness that have been used in previous literature and that could be applied to the nursing home population. These are summarized below and includes five key domains: (1) prognosis-based definitions (i.e. <6 months), (2) mortality risk-based (i.e. high risk vs low risk), (3) healthcare service-based (i.e. receipt of palliative care consult), (4) comorbidity index-based (e.g. the Veteran’s Health Association Palliative Care Index), and (5) composite definition (i.e. comorbidity and caregiver burden) (20). See Figure 1 for an overview of these definitions.
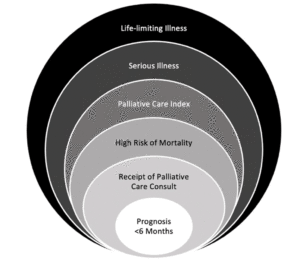
Figure 1
Summary of the operational definitions of life-limiting illness that can be applied to the nursing home population. Serious illness is the most inclusive definition, while a documented prognosis
(1) Prognosis-based operationalization
A prognosis less than six months is based on the terminal illness definition in the US federal code, 42 USC Sec. 1395x.21 In the United States, virtually all nursing homes are required to conduct a comprehensive geriatric assessment on all residents at regular intervals using the Minimum Data Set. If using the Minimum Data Set (MDS) 3.0, the variable for prognosis can be used, found in section J, sub-section 1400 “Prognosis” (22) or designation of hospice care in section O. In the MDS 2.0 use of hospice care in the last fourteen days is found in section P. While the prognosis variable is sensitive, it is not very specific. There may be more inclusive ways of identifying those near the end of life, such as the high-risk mortality score, that could have a higher predictive value overall. Nevertheless, the prognosis variable is still helpful as a start to identifying those near the end of life.
(2) Mortality risk-based operationalization
A high risk of mortality is based on mortality-related factors and one-year survival in nursing home residents based on the Flacker-Kiely (2003) (23) mortality risk score model. These factors were drawn from variables from the MDS 2.0. Other mortality risk score algorithms were not recommended (e.g., Minimum Data Set Mortality Risk Index, MMRI or the recent version, MMRI-R) as they have shown poorer performance in predicting long-term mortality of nursing home residents (24). However, it should be noted that while any of these mortality risk models will identify more people as having a life-limiting illness than simply using one variable, such as the less than six-month prognosis MDS variable, studies have shown that the performance of the MMRI, MMRI-R, and even the original and revised Flacker-Kiely models are fair at best (24). Therefore, caution should be taken if any of these models were to be used alone without any other variables or operational definitions.
(3) Health service-based operationalization
A Medicare claim for receipt of palliative care consultation is a way to identify those that were consulted for palliative care services. Medicare is the health care insurance available to Americans over aged 65 years. For those who elect Medicare Fee-for-Service, Medicare claims can be used to identify nursing home residents who have received a palliative care consultation. Palliative care or comfort treatment measures are most often offered to those with a limited life expectancy or for symptom management. If inpatient Medicare claims data are available, ICD-10 diagnosis code Z51.5 could be used to identify those that had a hospital consult for palliative care services. This hospital diagnosis code has been shown to be valid (25), with almost half of the population that received this service dying before discharge. This could be applied with a one-year or six-month lookback period. If the sample size is limited using this definition, this definition could be combined with the less than six-month prognosis variable to identify additional residents with a limited prognosis. A limitation of using this measure is that it may just reflect the relationship between the nursing home and palliative care center. The measure could thus be specific, but not very sensitive for identifying those near the end of life.
(4) Comorbidity-based operationalization
The Palliative Care Index or Veterans Health Administration Palliative Care Index (PCI) (26–28) was originally created by the Veterans Health Administration, to identify those appropriate for palliative care. Based on this index, a patient was considered eligible for these services if they had any of the following conditions: esophageal cancer, liver cancer, pancreatic cancer, broncho-tracheal-lung cancer, colon cancer, leukemia, Hodgkin’s lymphoma, multiple myeloma, metastatic breast cancer, metastatic prostate cancer, AIDS, heart failure, or chronic obstructive pulmonary disease (COPD). For heart failure and COPD, residents either had to have more than two hospitalizations, one hospitalization with an intensive care unit stay, or an active MDS diagnosis within a six-month window. These conditions could be identified with Medicare diagnostic (ICD) codes if inpatient Medicare claims are available. It should be noted that this index was created around the year 2000. In which case, some of the conditions that may have been more serious then are not as serious now given the advent of better treatment options. If using this index today, certain modifications may be necessary, such as removing early-stage colon cancer.
(5) Comorbidity and caregiver burden-based operationalization
A “serious illness,” based on the definition by Kelley et al. (2019) (20), could be identified by the presence of any diagnosis in their validated list of ICD-10 codes for the following conditions: cancer, chronic kidney disease (stage 5)/end-stage renal disease, advanced liver disease/cirrhosis, diabetes with severe complications (ischemic heart disease, peripheral vascular disease, renal disease), AIDS, hip fracture, dementia, chronic obstructive pulmonary disease (COPD) or interstitial lung disease, heart failure, neurodegenerative diseases, and stroke. This definition is particularly useful if Medicare claims with ICD codes are available to the investigators. However, it should be noted that serious illness is one of the most inclusive definitions. In one of our recent papers (29), almost all of those identified with having a life-limiting illness also were identified as having a serious illness. This more inclusive population will likely include those with a six month prognosis regardless if it is documented or not.
Translating Definitions to Administrative Codes and Datasets
These operational approaches were specifically selected based on definitions that could be translated to codes available to current researchers to operationally define life-limiting illness using administrative data sources (i.e., MDS and/or Medicare fee-for-service claims) available for most residents in US nursing homes. These definitions could also be applied to nursing homes in countries other than the US, particularly those that also use the MDS or have data available to capture the information in these definitions. This centered mostly on ICD-10 hospital discharge codes and variables from the Minimum Data Set 2.0 and 3.0. See Table 1 for a summary of these codes and the literature for which each definition was drawn. This table has been modified from some of our previous work (29–31).
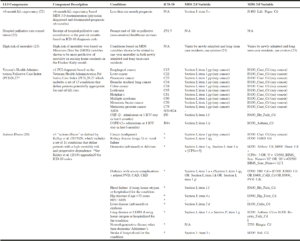
Table 1
Operational Definition for Life-Limiting Illness (LLI) including ICD-10 hospital diagnosis codes and Minimum Data Set (MDS) 2.0 and 3.0 variables
*PCI ICD-10 codes were converted from Silveira et al. (2008)26 ICD-9 codes using the AAPC Online ICD Translator Tool (2020) (34)
Applying Operational Definitions
We have demonstrated how to apply these operational definitions in some of our previous work (29, 30). For example, life-limiting illness among long-stay nursing home residents was defined by using four of the five definitions presented in this review. This included: life expectancy less than six months, receipt of palliative care consult, a palliative care index diagnosis, and a “serious illness” as defined by Kelley et al. (2019) (20). Nursing home residents were categorized into these mutually exclusive sub-conditions using a single path hierarchical modeling approach from most to least specific groups from serious illness to a prognosis <six months. In general, how life-limiting illness is operationalized and applied in any study will depend on the data resources that are available to investigators. For example, having access to the nursing home clinical information from the Minimum Data Set and/or Medicare claims data, which we were able to use to define serious illness, will influence who is identified with these algorithms.
Another application of these operational definitions would be for use in interventions. This includes using some of these criteria to determine individuals that would be appropriate for hospice, palliative care, or medication deprescribing. For hospice, a prognosis less than six months has been traditionally used to identify appropriate individuals. However, determining those appropriate for palliative care or medication deprescribing could be more nuanced (32). Thus having specific criteria available that could more broadly identify those for palliative care could be greatly beneficial, particularly for those with a high symptom burden, untreated pain, and polypharmacy in the context of a terminal condition or limited life expectancy (33).
Evidence Gaps and Future Research
The predictability of these operational definitions of life-limiting illness both individually and collectively have yet to be validated in the nursing home population. Future research should be done to validate these definitions. The importance of identifying nursing home residents with life limiting illnesses is underscored by the aging of the population. This is further emphasized by the clinical complexity of the residents, the lack of clear guidelines on when to reduce medications for which the known risks exceed the unknown benefits (e.g., statin use in those over 75 years of age), and the need for healthcare providers to initiate conversations with residents and their families to assure medical treatments are aligned with resident goals.
Conflict of Interest Disclosure: Jennifer Tjia is a consultant for CVS Health and Omnicare Long Term Care Pharmacy. The other authors have declared no conflicts of interest for this article.
Funding sources: The work was supported by the National Center for Advancing Translational Sciences, National Institutes of Health (TL1 TR001454), the National Institute of Nursing Research (R01NR016977) and the National Institute on Aging (K24AG068300).
Open Access: This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits use, duplication, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license and indicate if changes were made.
References
1. Etkind SN, Bone AE, Gomes B, Lovell N, Evans CJ, Higginson IJ, et al. How many people will need palliative care in 2040? Past trends, future projections and implications for services. BMC Med 2017 151 2017;15(1):1-10. doi:10.1186/S12916-017-0860-2
2. Kelley AS. Defining “‘Serious Illness.’” J Palliat Care 2014;17(9):985. doi:10.1089/jpm.2014.0164
3. Management Lee KC, Walling AM, Senglaub SS, Kelley AS, Cooper Z. Defining Serious Illness Among Adult Surgical Patients. J Pain Symptom Manage August 2019. https://doi.org/10.1016/j.jpainsymman.2019.08.003. Accessed August 14, 2019.
4. Kelley AS, Bollens-Lund E. Identifying the Population with Serious Illness: The Denominator Challenge. J Palliat Med 2018;21(S2):S7-S16. doi:10.1089/jpm.2017.0548
5. World Health Organization. 10 facts on ageing and health. https://www.who.int/news-room/fact-sheets/detail/10-facts-on-ageing-and-health. Published 2017. Accessed January 28, 2021.
6. Centers for Disease Control and Prevention, National Center for Health Statistics. Multiple Cause of Death 1999-2016 on CDC WONDER Online Database, released December, 2017. Data are from the Multiple Cause of Death Files, 1999-2016, as compiled from data provided by the 57 vital statistics jurisdictions through the Vital Statistics Coop. http://wonder.cdc.gov/mcd-icd10.html. Accessed March 7, 2018.
7. US Centers for Medicare & Medicaid Services (CMS). Nursing Home Data Compendium 2015 Edition.; 2015. https://www.cms.gov/Medicare/Provider-Enrollment-and-Certification/CertificationandComplianc/Downloads/nursinghomedatacompendium_508-2015.pdf. Accessed August 21, 2017.
8. Kelly A, Conell-Price J, Covinsky K, Cenzer IS, Chang A, Boscardin WJ, et al. Length of Stay for Older Adults Residing in Nursing Homes at the End of Life. J Am Geriatr Soc 2010;58(9):1701-1706. doi:10.1111/j.1532-5415.2010.03005.x
9. Smith S, Brick A, O’Hara S, Normand C. Evidence on the cost and cost-effectiveness of palliative care: A literature review. Palliat Med 2014;28(2):130-150. doi:10.1177/0269216313493466
10. Kelley AS, Morrison RS. Palliative Care for the Seriously Ill. Campion EW, ed. N Engl J Med 2015;373(8):747-755. doi:10.1056/NEJMra1404684
11. Jordhøy MS, Fayers P, Loge JH, Ahlner-Elmqvist M, Kaasa S. Quality of life in palliative cancer care: Results from a cluster randomized trial. J Clin Oncol 2001;19(18):3884-3894. doi:10.1200/JCO.2001.19.18.3884
12. Hall S, Kolliakou A, Petkova H, Froggatt K, Higginson I. Interventions for improving palliative care for older people living in nursing care homes (Review). Cochrane Database Syst Rev 2011;(3):CD007132. doi:10.1002/14651858.CD007132.pub2
13. De Nardi M, French E, Jones JB, Mccauley J. Medical Spending of the U.S. Elderly. 2015. http://www.nber.org/papers/w21270. Accessed November 16, 2021.
14. Blumenthal D, Chernof B, Fulmer T, Lumpkin J, Selberg J. Caring for High-Need, High-Cost Patients — An Urgent Priority. NEJM 2016;375(10):909-911.
15. Teno JM, Clarridge BR, Casey V, Welch LC, Wetle T, Shield R, et al. Family Perspectives on End-of-Life Care at the Last Place of Care. JAMA 2004;291(1):88-93. doi:10.1001/JAMA.291.1.88
16. Mitchell SL, Teno JM, Kiely DK, Shaffer ML, Jones RN, Prigerson HG, et al. The Clinical Course of Advanced Dementia. http://dx.doi.org/101056/NEJMoa0902234 December 2009. doi:10.1056/NEJMOA0902234
17. Download: Dying in America: Improving Quality and Honoring Individual Preferences Near the End of Life | The National Academies Press. https://www.nap.edu/download/18748. Accessed January 21, 2021.
18. Hui D, Nooruddin Z, Didwaniya N, Dev R, De La Cruz M, Kim SH, et al. Concepts and definitions for "actively dying," "end of life," "terminally ill," "terminal care," and "transition of care": a systematic review. J Pain Symptom Manage 2014;47(1):77-89. doi:10.1016/j.jpainsymman.2013.02.021
19. Hui D, Nooruddin Z, Didwaniya N, Dev R, De La Cruz M, Kim SH, et al. Concepts and Definitions for “Actively Dying,” “End of Life,” “Terminally Ill,” “Terminal Care,” and “Transition of Care”: A Systematic Review. J Pain Symptom Manage 2014;47(1):77-89. doi:10.1016/j.jpainsymman.2013.02.021
20. Kelley AS, Ferreira KB, Bollens-Lund E, Mather H, Hanson LC, Ritchie CS, et al. Identifying Older Adults With Serious Illness: Transitioning From ICD-9 to ICD-10. J Pain Symptom Manage 2019;57(6):1137-1142. https://doi.org/10.1016/j.jpainsymman.2019.03.006. Accessed August 14, 2019.
21. 42 U.S. Code § 1395x – Definitions | U.S. Code | US Law | LII / Legal Information Institute. https://www.law.cornell.edu/uscode/text/42/1395x. Accessed October 28, 2019.
22. CMS. CMS’s RAI Version 3.0 Manual CH 3: MDS Items [J] SECTION J: HEALTH CONDITIONS. 2010. https://www.ahcancal.org/facility_operations/Documents/UpdatedFilesOct2010/Chapter 3 – Section J V1.04 Sept 2010.pdf. Accessed July 20, 2017.
23. Flacker JM, Kiely DK. Mortality-related factors and 1-year survival in nursing home residents. J Am Geriatr Soc 2003;51(2):213-221. doi:10.1016/j.jamda.2009.06.001.Religiousness
24. Kruse RL, Parker Oliver D, Mehr DR, Petroski GF, Swenson DL, Zweig SC. Using Mortality Risk Scores for Long-term Prognosis of Nursing Home Residents: Caution Is Recommended. Journals Gerontol Ser A Biol Sci Med Sci 2010;65A(11):1235-1241. doi:10.1093/gerona/glq120
25. Hua M, Li G, Clancy C, Sean Morrison R, Wunsch H. Validation of the V66.7 Code for Palliative Care Consultation in a Single Academic Medical Center. J Palliat Med 2017;20(4):372-377. doi:10.1089/jpm.2016.0363
26. Silveira MJ, Kazanis AS, Shevrin MP. Statins in the last six months of life: A recognizable, life-limiting condition does not decrease their use. J Palliat Med 2008;11(5):685-693. doi:10.1089/jpm.2007.0215
27. Kumar G, Hayes K. Hospice and Palliative Care Strategic Plan for an Inpatient Unit. In: Office of Academic Affiliations (OAA), Geriatrics and Extended Care in the Office of Patient Service, eds. A Toolkit for Developing Hospice and Palliative Care Programs in the Department of Veterans Affairs Medical Centers. Washington DC: VA Training and Program Assessment for Palliative Care (TAPC) Project; 2001:52-57. www.va.gov/oaa/flp. Accessed August 13, 2019.
28. Department of Veterans Affairs, Veterans Health Administration. Journey of Change III. Washington DC: Office of Planning and Policy; 2000. http://www.va.gov/vhareorg/. Accessed November 25, 2019.
29. Mack DS, Tjia J, Hume AL, Lapane KL. Prevalent Statin Use in Long-Stay Nursing Home Residents with Life-Limiting Illness. J Am Geriatr Soc February 2020:1-9. doi:10.1111/jgs.16336
30. Mack DS, Baek J, Tjia J, Lapane KL. Statin Discontinuation and Life-Limiting Illness in Non–Skilled Stay Nursing Homes at Admission. J Am Geriatr Soc August 2020:jgs.16777. doi:10.1111/jgs.16777
31. Mack DS, Baek J, Tjia J, Lapane KL. Geographic Variation of Statin Use among US Nursing Home Residents with Life-limiting Illness. Med Care 2021;59(5):425-436. doi:10.1097/MLR.0000000000001505
32. O’connor NR, Casarett DJ. Editorial Which Patients Need Palliative Care Most? Challenges of Rationing in Medicine’s Newest Specialty. doi:10.1089/jpm.2016.0080
33. Rome RB, Luminais HH, Bourgeois DA, Blais CM. The Role of Palliative Care at the End of Life.
34. AAPC. Online ICD Code Translator Tool. https://www.aapc.com/icd-10/codes/. Published 2020. Accessed February 3, 2020.
