K. Salminen1,2, U. Aalto3, M. Suominen1, H. Kautiainen1, K. Pitkälä1,4, H.-M. Roitto5,6,7
1. University of Helsinki, Department of General Practice and Primary Health Care, Helsinki, Finland; 2. Vantaa Social Welfare and Health Care, Vantaa, Finland; 3. Dept of Social Services and Health Care, Helsinki Hospital, Home-care Services, City of Helsinki, Finland; 4. Helsinki University Hospital, Unit of Primary Health Care, Helsinki, Finland; 5. University of Helsinki, Department of Neurosciences, Finland; 6. Helsinki University Hospital, Internal medicine and rehabilitation, Division of Geriatrics, Finland; 7. Finnish Institute for Health and Welfare, Population health unit, Finland
Corresponding author: Karoliina Salminen, MHC, Department of General Practice and Primary Health Care, POB 20, 00014, Helsinki, Finland, Tel.: +358405400675, Email: karoliina.salminen@helsinki.fi, ORCID: https://orcid.org/0000-0003-4704-3211
Dear editor
Older nursing home residents have high risk of falls and half of nursing home residents fall annually (1). Previous studies have reported that vitamin D supplementation might reduce the risk of falls in long-term care (LTC) settings (2). However, the findings have been contradictor and optimal dose of vitamin D for institutionalized older people remains unclear. The aim of this study was to explore the association between total vitamin D intake and annual number of falls among older LTC residents.
Methods
Overall, 352 LTC residents living in Helsinki had information available to this study. Residents were thoroughly assessed in 2018 (3, 4). The use of vitamin D supplementation was retrieved from medical records and the vitamin D intake from nutrition was evaluated by one- or two-day food records. The number of falls was collected from medical records over 12 months. Residents who were bed-ridden and unable to move were excluded from this study. The Ethics Committee of Helsinki University Central Hospital has approved all study the protocols. Informed consent was obtained for all participants. The informed consent included access to the social and medical records. If the resident was not able to give the informed consent (MMSE <20), the closest proxy gave consent.
Crude and standardized estimates of falls incidence was calculated using Poisson regression models.
A possible nonlinear relationship between falls and the vitamin D daily integer age was assessed by using a 4-knot-restricted cubic spline Poisson regression model; model adjusted for age, sex, Charlson comorbidity (5) index and frailty (6 ).
Results
The residents mean age was 83 and 80% were females. Of residents, 86% suffered from dementia and 61% were frail, 38% prefrail and only 1% robust according to Fried’s phenotype (6) 42% needed another person’s help while moving. The mean Charlson comorbidity index (5) was 2.0.
There were 450 falls and 17 fractures in our population during one year follow-up. The incidence of falls was 1.52 (95% CI 1.38-1.67). Of residents, 89% used vitamin D supplementation. When counting the vitamin D total intake from food and supplements, the incidence rate of falls started linearly decreasing after the total vitamin D intake was ≥1200 IU/day (Figure 1). Of those receiving <1200IU/day there were 15 fracture whereas the respective figure among those with ≥1200 IU/day was two fractures. The results were essentially the same, when adjusted for dementia, mobility, protein intake or use of psychotropics (data not shown).
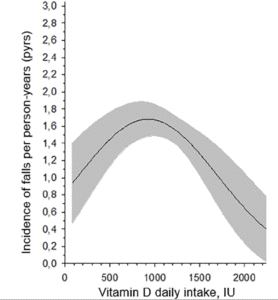
Figure 1
Association between vitamin D daily intake (IU)
and incidence of falls per person-years (pyrs)
Discussion
In our study among old, frail nursing residents the incidence of falls decreased linearly with vitamin D intake over 1200 IU/day. The low number of fractures among those with higher doses supports the finding that this frail population benefits from vitamin D doses 800IU or more.
Some earlier studies have reported that high vitamin D dose might be associated with higher risk of falls and fracture risk in community-dwellers (7). In one-year randomized, controlled trial 60 000 IU monthly vitamin D dose or 24 000 IU vitamin D dose plus calcifediol increased proportion of fallers and number of falls compared to 24 000 IU group (8). However, according to a pooled analysis including 11 RCT studies including both home-dwellers and people in institutions, higher vitamin D doses (792-2000IU/day) prevented hip fractures and decrease the risk of nonvertebral fractures among older people compared to lower doses (9).
Meta-analysis showed that vitamin D supplement over 800IU combined with calcium supplement decreased fracture risk compared to doses less than 800IU (10). The institutionalized residents benefitted relatively more than community-dwellers. The RCT study among nursing home residents showed that vitamin D supplement 800IU decreased the number of fallers and incidence of falls compared lower dose groups (2).
Thus, it seems that community-dwelling and institutionalized older people differ in their needs for vitamin D. Our study population was living in nursing homes being frail, having impaired cognition and mobility limitations. Our vitamin D intake included both supplement and vitamin D obtained from nutrition. Institutionalized people in Finland do not spend very much time outdoors and most of falls happens indoors.
In Finland vitamin D supplementation 400-800 IU/day has been recommended for people over 75 years. This recommendation has well been implemented to LTC facilities, as 89% of the residents used the vitamin D supplementation.
It seems that, the association between vitamin D3 supplementation dose and falls may vary depending on the frailty status of older people.
Conflicts of Interest: Authors declare no conflict of interest.
References
1. Rubenstein LZ. Falls in older people: epidemiology, risk factors and strategies for prevention. Age Ageing. 2006;35 Suppl 2:ii37-ii41. doi: 10.1093/ageing/afl084
2. Broe KE, Chen TC, Weinberg J, Bischoff-Ferrari HA, Holick MF, Kiel DP. A higher dose of vitamin d reduces the risk of falls in nursing home residents: a randomized, multiple-dose study. J Am Geriatr Soc. 2007;55(2):234-9. doi: 10.1111/j.1532-5415.2007.01048.x
3. Salminen K, Willman M, Kautiainen H, Pitkälä K, Roitto H-M, Suominen M. Temporal trends in nutrition intake among older long-term care residents. Clinical Nutrition. 2021;40(6):3793-7. doi: https://doi.org/10.1016/j.clnu.2021.04.048
4. Roitto H-M, Öhman H, Salminen K, Kautiainen H, Laurila J, Pitkälä KH. Neuropsychiatric Symptoms as Predictors of Falls in Long-Term Care Residents With Cognitive Impairment. 2020. doi: 10.1016/j.jamda.2020.04.003
5. Charlson ME, Pompei P, Ales KL, MacKenzie CR. A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. Journal of chronic diseases. 1987;40(5):373-83. doi: 10.1016/0021-9681(87)90171-8
6. Fried LP, Tangen CM, Walston J, Newman AB, Hirsch C, Gottdiener J, et al. Frailty in older adults: evidence for a phenotype. The journals of gerontologySeries A, Biological sciences and medical sciences. 2001;56(3):146. doi: 10.1093/gerona/56.3.m146.
7. Wanigatunga AA, Sternberg AL, Blackford AL, Cai Y, Mitchell CM, Roth DL, et al. The effects of vitamin D supplementation on types of falls. Journal of the American Geriatrics Society (JAGS). 2021;69(10):2851-64. doi: 10.1111/jgs.17290
8. Bischoff-Ferrari HA, Dawson-Hughes B, Orav EJ, Staehelin HB, Meyer OW, Theiler R, et al. Monthly High-Dose Vitamin D Treatment for the Prevention of Functional Decline: A Randomized Clinical Trial. JAMA Intern Med. 2016;176(2):175-83. doi: 10.1001/jamainternmed.2015.7148
9. Bischoff-Ferrari HA, Willett WC, Orav EJ, Lips P, Meunier PJ, Lyons RA, et al. A Pooled Analysis of Vitamin D Dose Requirements for Fracture Prevention. New England Journal of Medicine. 2012;367(1):40-9. doi: 10.1056/NEJMoa1109617
10. Tang BM, Eslick GD, Nowson C, Smith C, Bensoussan A. Use of calcium or calcium in combination with vitamin D supplementation to prevent fractures and bone loss in people aged 50 years and older: a meta-analysis. Lancet (London, England). 2007;370(9588):657-66. doi: 10.1016/s0140-6736(07)61342-7
