V. Guion1,2,3, P. Riba Bremerch4, Y. Rolland1,5
1. Gerontopole of Toulouse, Institute on Aging, Toulouse University Hospital (CHU Toulouse), Toulouse, France; 2. Département douleur – Soins Palliatifs, Pôle autonomie – handicap, CHU de Besançon, Besançon, France; 3. INSERM CIC 1431, Université de Bourgogne Franche-Comté, Besançon, France; 4. Département Universitaire de Médecine Générale, Faculté de Médecine Toulouse Rangueil, Université Paul Sabatier Toulouse III, France; 5. CERPOP Centre d’Epidémiologie et de Recherche en santé des POPulations UPS/INSERM UMR 1295, Toulouse, France
Corresponding author: Vincent Guion, Gerontopole, Cité de la Santé, CHU de Toulouse, 20 rue du Pont Saint-Pierre, 31059 Toulouse, France, Phone: (+33) 561 145 664, e-mail: vincent.guion@gmail.com, ORCID ID : 0000-0001-5144-4419
Jour Nursing Home Res 2022;8:20-23
Published online July 1, 2022, http://dx.doi.org/10.14283/jnhrs.2022.6
Abstract
The purpose was to investigate the association between mortality in nursing home residents (NHR) and multimorbidity, dependence and their interaction. This study was an 18-month prospective, observational study, that included a subgroup of 5527 NHR residing in 163 nursing homes located in France between May and July 2011. A Cox proportional hazard model was used to perform multivariate survival analysis. Independent variables of interest were baseline multimorbidity, baseline dependence, and the interaction between multimorbidity and dependence. NHR were very dependent at baseline and the median Charlson Index score was 2. In multivariate survival analysis, multimorbidity and dependence were both significantly associated with an increased 18-month mortality (HR=1.10; CI 95% [1.04 – 1.17] and HR=1.30; CI 95% [1.22 – 1.38], respectively). Higher multimorbidity and higher dependence were both independently associated with a higher 18-month mortality in NHR. Clinicians could use these two simple indicators to identify NHR requiring palliative care.
Key words: Nursing homes, multimorbidity, functional status.
Introduction
Nursing home residents are a vulnerable population, with a limited lifespan (1), life-limiting diseases and are at risk for potentially life-limiting acute events. Yet, one nursing home resident in four have very limited access to palliative care at the end of their life, with insufficient symptom relief and respect for privacy (2). External palliative care resources are available but under-solicited and internal resources are scarce (2). Early initiation of palliative care could improve residents’ quality of life by identifying care needs and facilitating palliative care provision at early stages (3).
Identifying nursing home residents requiring palliative care is a pre-requisite to their effective access to palliative care. Existing tools to identify palliative situations are either derived from prognosis estimation (4, 5) or from multimorbidity evaluation (6) and are seldom specific to nursing home residents (7). But existing identification tools lack sensitivity and often identify nursing home residents in very advanced or terminal stages, when care planning is limited to short-term goals of care, whereas earlier identification would be required in nursing home residents often presenting terminal declines over several years (8).
Multimorbidity and dependence are routinely evaluated in nursing home residents. Their use in daily practice to identify nursing home residents requiring palliative care could be easier than the use of research-purposed identification tools, and thus ensure broader access to palliative care in nursing home residents. The aim of this study was to investigate the association between 18-month mortality in nursing home residents and multimorbidity, dependence and their interaction.
Methods
Participants and setting
Data of the IQUARE study were used. Briefly, IQUARE was an interventional study performed in southwest France from 2011 to 2013 that included 6275 nursing home residents to improve quality of care and reduce nursing home residents’ functional decline (9). Quality indicators were compared before and after an 18-month follow-up, during which two types of interventions (light or strong) were implemented in participating facilities. Nursing homes in the strong intervention group were assigned individual support by a hospital geriatrician and collective support by the regional health agency. Nursing homes in the light intervention group were only presented their performance on quality indicators before and after follow-up (10). Data from both intervention groups were pooled in this study. The ethics committee of Toulouse University Hospital and the Consultative Committee for the Treatment of Research Information on Health approved IQUARE (CNIL: 07–438).
Outcome measures
The main outcome was death. Follow-up time was calculated from the date of inclusion to the date of death for decedents, and from the date of inclusion to the date of final assessment for survivors.
Independent variables of interest were baseline multimorbidity, as indicated by the Charlson Comorbidity Index, baseline dependence as indicated by the Groupe Iso Ressource (GIR, ranging from 1: totally dependent, to 6: no dependence) and the interaction between multimorbidity and dependence. Multimorbidity and dependence were used as continuous variables.
Covariates included age, gender, provenance before admission to NH, hospitalizations in the last year, body mass index (BMI), any weight loss in the last two months, oral nutritional supplements intake, falls in the last year, dementia, screams, depression, physical restraint, pain, and polypharmacy (number of drugs prescribed, continuous).
Statistical analysis
A Cox proportional hazard model was used to perform multivariate survival analysis. Proportional hazards assumption was verified using Shoenfeld residuals method and the absence of multicollinearity was verified using the variance inflation factor. Analyses were performed by STATA, version 16.1. (StataCorp, College Station, Texas, USA). Statistical significance was assumed when p<.05.
Results
A total of 5527 residents from 163 nursing homes were included, among which 1554 died during follow-up. Nursing home residents’ characteristics were presented in Table 1. The median age was 87.5 years, and most nursing home residents were women (73.8%). The median GIR was 2 and the median Charlson Index score was 2; 42.7% of nursing home residents had dementia.
*GIR: Groupe Iso-Ressources, inversely reflecting dependency for activities of daily living
The results of the survival model were presented in Table 2. Multimorbidity and dependence were both significantly associated with an increased 18-month mortality (Hazard Ratio (HR)=1.10; CI 95% [1.04 – 1.17] and HR=1.30; CI 95% [1.22 – 1.38], respectively), whereas their interaction was not (HR= 0.99; CI 95% [0.98 – 1.01]).
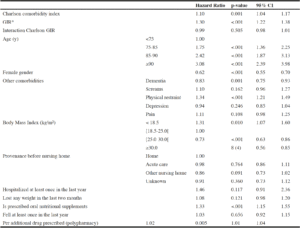
Table 2
Cox model: 5527 observations, 163 nursing homes, 1554 deaths, time at risk 88,984.1 months, p value <.001
*:GIR: Groupe Iso-Ressources, inversely reflecting dependency for activities of daily living. This variable was inverted to directly reflect dependency (e.g. GIR 6 was transformed into 1, GIR 5 into 2, etc.); Note: Age and body mass index were significantly associated with the risk of death (p-value <.001) whereas provenance before nursing home was not (p-value 0.31).
Female gender, BMI 25–29.9, BMI ≥30 and dementia were significantly associated with a decreased risk of 18-month mortality in nursing home residents (HR=0.62; IC [0.55-0.70], HR=0.73; IC [0.63-0.86], HR=0.69; IC [0.56-0.85] and HR=0.83; IC [0.75-0.93] respectively). Conversely, age (categorical covariate), BMI ≤18.5, oral nutritional supplements intake, physical restraint and polypharmacy were significantly associated with an increased risk of 18-months mortality in nursing home residents (p<.001, HR=1.31; IC [1.07-1.60], HR=1.33; IC [1.15-1.55], HR=1.34; IC [1.21-1.49], HR=1.02; IC [1.01-1.04] respectively).
Discussion
Higher multimorbidity and higher dependence were both independently associated with a higher 18-month mortality in nursing home residents. Yet, the size effect of dependence on mortality was not affected by multimorbidity, and the size effect of multimorbidity on mortality was not affected by dependence, as informed by a non-significant association of the interaction term with mortality.
This study provided clinicians with two simple indicators, i.e. higher multimorbidity and higher dependence, which could be used in routine by primary care providers to identify nursing home residents requiring palliative care. Beyond their identification, prioritizing these nursing home residents for advance care planning would more effectively give them actual access to palliative care through individually tailored goals of care.
In France, primary care physicians and nursing home medical directors are respectively responsible for individual and collective care decisions, including palliative care provision. In some situations, medical directors could implement strong facility-wide palliative care policies that will remain inaccessible to nursing home residents in a palliative situation until their primary care physician identifies the situation as such. Joint evaluation through consensual measurable indicators like multimorbidity and dependence could help solve these situations and give more nursing home residents access to palliative care.
Further research could include interventional studies to evaluate prospectively this simple identification strategy on patient-reported outcomes.
The literature on palliative care for nursing home residents and particularly on the identification of nursing home residents requiring palliative care is very scarce despite the growing prevalence of these situations. To our knowledge, this study is the first on this issue that was performed on a French population.
The large number of participants in this multicenter study and their characteristics suggest the participants were a representative sample the French population living in nursing homes. nursing home residents were similar in terms of age (median of 87.5 years in our sample and in nursing home residents in France in 2015), proportion of female gender (73.8 vs 73.6% respectively) and level of dependence (51.7% of were GIR 1 or 2 vs 54% in nursing home residents in France in 2015) (11).
Results on covariates in the multivariate survival model concur with known risk factors for mortality in nursing home residents, including age (8, 12), gender (8, 13), BMI ≤ 18.5 (14), BMI ≥ 25 (14), dementia (15) and polypharmacy (13).
A confounding bias could have been introduced in the interpretation of results due to the exclusion of some variables from the survival model, despite a rationale in the literature for including them. These variables, like recent transfer to an emergency department or pressure ulcers, were excluded after they were found to violate proportional hazards assumption.
Acknowledgments: We would like to thank Christine Piau, MD, Catherine Bouget, PhD, Françoise Cayla, MD, and Céline Mathieu, MSc for their valuable contribution in the study design and data collection. We also thank the members from the IQUARE Research Group (members from COPIL: Dr Jean-Jacques Morfoisse, Gwenaelle Buatois, Dr Catherine Marchal, Pascal Degauque, Sabine Pi; and all 57 members of the Technical Committee) for their work.
Conflicts of Interest: The authors have no conflict of interest to disclose.
Funding: The IQUARE study was funded by a grant from the Regional Agency of Health of the Midi-Pyrénées region (Agence Régionale de Santé – Midi-Pyrénées). The funder contributed to data collection. The funder had no influence on the analysis and interpretation of data, or on the preparation, review, or approval of the manuscript.
Open Access: This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits use, duplication, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license and indicate if changes were made.
References
1. Mack DS, Tjia J, Lapane KL. Defining Life-Limiting Illness in the Nursing Home Population: Identifying a Population to Benefit from Palliative Care Services. J Nurs Home Res Sci [Internet]. 2022 [cited 2022 May 16]; Available from: https://www.jnursinghomeresearch.com/all-issues.html?article=350
2. Observatoire National de la Fin de Vie. La fin de vie en EHPAD. Premiers résultats d’une étude nationale [Internet]. 2013. Available from: https://sites.google.com/site/observatoirenationalfindevie/EHPAD
3. Haun MW, Estel S, Rücker G, Friederich HC, Villalobos M, Thomas M, et al. Early palliative care for adults with advanced cancer. Cochrane Database Syst Rev. 2017 Jun 12;6:CD011129.
4. White N, Kupeli N, Vickerstaff V, Stone P. How accurate is the ‘Surprise Question’ at identifying patients at the end of life? A systematic review and meta-analysis. BMC Med. 2017 Aug 2;15:139.
5. Prompantakorn P, Angkurawaranon C, Pinyopornpanish K, Chutarattanakul L, Aramrat C, Pateekhum C, et al. Palliative Performance Scale and survival in patients with cancer and non-cancer diagnoses needing a palliative care consultation: a retrospective cohort study. BMC Palliat Care. 2021 May 26;20(1):74.
6. De Bock R, Van Den Noortgate N, Piers R. Validation of the Supportive and Palliative Care Indicators Tool in a Geriatric Population. J Palliat Med. 2018 Feb 1;21(2):220–4.
7. Flacker JM, Kiely DK. A practical approach to identifying mortality-related factors in established long-term care residents. J Am Geriatr Soc. 1998 Aug;46(8):1012–5.
8. Cohen-Mansfield J, Marx MS, Lipson S, Werner P. Predictors of Mortality in Nursing Home Residents. J Clin Epidemiol. 1999 Apr;52(4):273–80.
9. de Souto Barreto P, Lapeyre-Mestre M, Mathieu C, Piau C, Bouget C, Cayla F, et al. A multicentric individually-tailored controlled trial of education and professional support to nursing home staff: Research protocol and baseline data of the IQUARE study. J Nutr Health Aging. 2013 Feb;17(2):173–8.
10. Rolland Y, Mathieu C, Piau C, Cayla F, Bouget C, Vellas B, et al. Improving the Quality of Care of Long_Stay Nursing Home Residents in France. J Am Geriatr Soc. 2016 Jan 1;64(1):193–9.
11. Muller M. 728 000 résidents en établissements d’hébergement pour personnes âgées en 2015. Drees Études Résultats. 2017 Jul;(1015).
12. Vossius C, Selbæk G, Šaltytė Benth J, Bergh S. Mortality in nursing home residents: A longitudinal study over three years. PloS One. 2018;13(9):e0203480.
13. Dale MC, Burns A, Panter L, Morris J. Factors affecting survival of elderly nursing home residents. Int J Geriatr Psychiatry. 2001 Jan 1;16(1):70–6.
14. de Souto Barreto P, Cadroy Y, Kelaiditi E, Vellas B, Rolland Y. The prognostic value of body-mass index on mortality in older adults with dementia living in nursing homes. Clin Nutr Edinb Scotl. 2017 Apr;36(2):423–8.
15. Porock D, Parker Oliver D, Zweig S, Rantz M, Mehr D, Madsen R, et al. Predicting Death in the Nursing Home: Development and Validation of the 6-Month Minimum Data Set Mortality Risk Index. J Gerontol A Biol Sci Med Sci. 2005 Apr 1;60(4):491–8.

