H.Y.K. Tong1,2,4, S.Y.C. Yue5, J. Woo2,3,7, H.H. Fung5, Y. Cheng6, H. Chen1, A. Kleinman1
1. Social Technology for Global Ageing Research Initiative, Harvard University, USA; 2. Faculty of Medicine, The Chinese University of Hong Kong, Hong Kong; 3. Department of Medicine and Therapeutics, Prince of Wales Hospital, Hong Kong; 4. Department of Clinical Oncology, Prince of Wales Hospital, Hong Kong ;
5. Department of Psychology, The Chinese University of Hong Kong, Hong Kong; 6. Department of Medical Humanities, School of Medicine, Sun Yat-Sen University, Chine; 7. Jockey Club Institute of Aging, The Chinese University of Hong Kong, Hong Kong.
Corresponding Author: H.Y.K. Tong, Department of Clinical Oncology, Prince of Wales Hospital, Hong Kong, kimberley.tong67@gmail.com; Tel: +852-92643191
Jour Nursing Home Res 2026;12:11-15
Published online April 10, 2026, http://dx.doi.org/10.14283/jnhrs.2026.2
Abstract
BACKGROUND: Body odour in older adults is a complex phenomenon that remains under-explored in nursing home and geriatric care settings. While age-related odour cues are biologically and socially significant, their implications for caregiving practice, resident dignity, and care quality require further investigation.
METHODS: A qualitative descriptive study was conducted between August and November 2023 in a licensed private nursing home in Hong Kong. Ten female caregivers were purposively sampled, and participated in individual semi-structured interviews covering four domains: odour perception, association with medical conditions, association with functional status, and management strategies. Caregivers rated separately the odour intensity (1-10) of residents with reference to the Katz Index of Independence in Activities of Daily Living. Data were analysed using deductive thematic analysis, and ratings were summarized descriptively.
RESULTS: Caregivers described residents’ body odour as noticeable with words such as “strong” or “musty”, yet did not express dehumanising or rejecting attitudes, reflecting professional habituation and emotional coping. Odour intensity was closely linked to functional dependency, particularly limitations in bathing and continence, and was interpreted as a clinical cue for conditions such as diabetes, chronic wounds, and poor oral hygiene. In the absence of formal training or institutional protocols, odour management relied on routine hygiene care and peer support. Caregivers also perceived that body odour contributed to stigma and ageist stereotypes among visitors and the wider community.
CONCLUSIONS: Frontline female caregivers in Hong Kong use body odour as a non-verbal indicator of health and functional status in older residents, despite limited organisational recognition or guidance. Findings support the integration of olfactory assessment and evidence-based odour management into geriatric training and care policies to promote dignified and age-inclusive care.
Key words: Older adults, body odour, residential care, caregivers, geriatrics care.
Introduction
Olfactory cues, including body odour, are an important but often over-looked dimension of residential long-term care. In nursing homes, complex interactions between ageing physiology, chronic diseases, and environmental factors can influence residents’ body odour, shaping both caregiving experiences and resident dignity. The compound 2-nonenal, an unsaturated aldehyde produced through oxidation of omega-7 unsaturated fatty acids, has long been associated with age-related body odour in adults aged over 40 years (1). However, more recent studies have reported inconsistent detection of 2-nonenal in older populations (2), suggesting that body odour in later life may be better understood through a multi-factorial model encompassing changes in skin barrier function, lipid composition, microbial communities and systemic health. Metabolites such as trimethylamine (TMA) and trimethylamine-N-oxide (TMAO), which can accumulate in individuals with altered microbiomes or renal impairment, may contribute to distinctive ammonia- or fish-like odours in some (3). In addition, systemic conditions, such as diabetes mellitus, hepatic dysfunction and chronic kidney disease, can generate characteristic volatile organic compounds (e.g., acetone and sulphur-containing compounds) that may further modify body and breath odour (4,5).
In nursing home settings, odour encompasses both biological and sociocultural dimensions. The body odour of older adult is frequently perceived as indicative of dependency, suboptimal hygiene, or neglect, which may influence the psychosocial well-being of residents and the professional experiences of caregiving staff. Incontinence-related odours, in particular, have been linked to shame, social withdrawal, and devaluation of caregiving service (6). Gender difference in olfactory sensitivity may further influence how frontline caregivers perceive and respond to odour within daily care routines (7). In Hong Kong, where roughly three-quarters of informal carers and the majority of institutional care staff are women (8), understanding these sensory and emotional dimensions of care is essential for improving resident quality of life and staff well-being.
This study aims to explore the experience the perceptions and management strategies of female caregivers regarding body odour among older adults in nursing homes in Hong Kong. Within the context of the city’s ageing population and high-density urban environment, the sensory characteristics of long-term care setting pose both operational and psychosocial challenges for caregiving staff. By understanding the perspectives and experiences of caregivers, this study hopes to inform geriatric practice and geriatric care policies, with an emphasis on integrating sensory considerations into personalised approaches that uphold resident dignity and promote supportive age-friendly institutional care environments.
Methods
Study Design and Setting
This study employed a qualitative and descriptive design to explore the perception of body odour among female caregivers working in a private residential care facility for older adults in Hong Kong. Data were collected between August and November 2023 in a licensed private residential care home in Shatin District (Sun Man Fook Aged Home, Shatin Branch; LORCH number L1016). A single-site design reduced variability in environmental factors, such as ventilation, building layout and hygiene infrastructure, which can influence odour production and perception in institutional settings. This allowed us to strengthen the internal validity of findings relating specifically to the perceptions and experiences of the caregivers.
Participants and Sampling
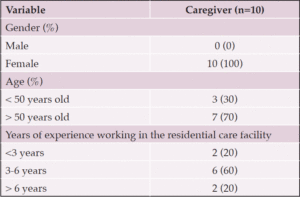
Ten female caregivers were recruited via purposive sampling to ensure variation in age, years of experience and direct care responsibilities. Inclusion criteria were: (1) female gender, (2) age >/= 18 years, (3) employment or volunteer status, and (4) provision of personal care to older adults. Individuals with self-reported or medically diagnosed olfactory impairment were excluded. All participants provided informed consent and received a HKD $100 supermarket voucher as compensation for their time. All data were anonymized and handled according to the institutional and international ethical guidelines. Sample size was guided by the concept of information power, whereby focused research questions, high-quality interview data and participant specificity can justify smaller qualitative samples (9).
Data Collection
Individual semi-structured interviews were conducted in private settings within the facility to ensure confidentiality and minimise interruptions. An interview guide that was structured around four domains (odour perception, association with medical conditions, association with functional status and management strategies), was developed with reference to the Standards for Reporting Qualitative Research (SRQR) guidelines (10). The interviews were conducted in Cantonese, lasted 45-60 minutes, were audio-recorded with consent and transcribed verbatim. After the interview, caregivers were also asked to rate the typical body odour intensity of residents on a 10-point numeric scale (1 = barely perceptible, 10 = extremely strong), considering their functional status assessed using the Katz Index of Independence in Activities of Daily Living (bathing, dressing, continence, transferring and feeding) (11).
Data Analysis
Data analysis followed a deductive, domain-specific thematic approach. Two researchers independently coded the transcripts against the four predefined domains using principles of thematic analysis (12). Coding was performed independently by researchers, with discrepancies resolved through discussion to minimize interpretive drift and ensure alignment with study’s objectives. Descriptive statistics were used to summarise odour intensity ratings by functional status; no inferential analyses were performed given the small sample and exploratory design.
Results
Perception of Body Odour
Caregivers uniformly reported that many of the residents had noticeable body odours, often described as “strong”, “musty” or “sour”. Participants acknowledged that these odours could provoke initial disgust or nausea, particularly when they first started working in the residential care industry, but described a process of habituation in which odour became an expected part of their occupational environment. Several participants reported that such odours contributed to a social stigma within care settings, reinforcing stereotypes or negative perceptions associated with ageing.
“ I assumed it was normal for elderly homes to have such noticeable odours.” #4
“I still find the smell unpleasant, but it’s part of my job. I try my best to adapt to it.” #7
“I lost 18 pounds in the first two months because I struggled to eat. The smell reminded me of rotten eggs, and I was nauseous all the time. I kept reminding myself that I had to push through.” #3
Association with Medical Condition
Most caregivers perceived distinct odour profiles associated with specific medical conditions. Diabetes, chronic wounds and poor oral hygiene were frequently cited as contributors to stronger odours, particularly breath odour. These observations parallel evidence that certain medical conditions are associated with characteristic volatile compounds. Some caregivers reported using changes in odour as a prompt to request medical review, adjust monitoring frequency or encourage hydration and oral care.
“When you stand close to them, the smell you notice often doesn’t come from incontinence; it actually comes from their mouth. I ask them to drink more water when I notice the smell because I believe they might be dehydrated.” #4
“I would say that the odour from the mouth is stronger than that from wounds, followed by the pubic area. Wounds are covered by dressings and the pubic area is covered with diapers, but the mouth cannot be covered so the bad breath is emitted directly”. #10
Association with Functional Status
Caregivers linked higher odour intensity ratings to greater functional dependency, particularly in bathing and continence. Descriptive analysis of odour ratings suggested higher mean scores among residents with dependence in Katz bathing and continence domains, although no formal statistical tests were conducted. Interestingly, one caregiver described cases in which more independent residents had stronger odour due to inconsistent bathing, re-wearing clothes or impaired memory for hygiene routines.
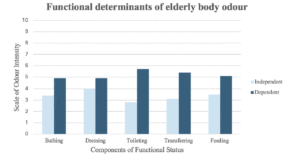
Figure 1. Graphical presentation of average odour intensity scores in relation to components of functional status based on the Katz Index of Independent Activities of Daily Living
“There was an elderly man who removed his shorts and placed them in the wardrobe before showering, but when I saw him afterwards, he was wearing the same pair. He had forgotten he had worn those shorts all day, which naturally resulted in a stronger odour. For those require assistance, we ensure that they are dressed and cleaned properly. However, for those who are capable of caring for themselves, we cannot be certain if they have cleaned themselves correctly, and they may not even realize it” #6
Management Strategies
In the absence of formal institutional policies or specific training on odour management, caregivers relied primarily on standard hygiene measures. Several participants emphasised peer support and informal knowledge sharing as their main sources of guidance. Caregivers described efforts to protect the dignity of residents when addressing odour-related issues that caused embarrassment or shame.
“When I notice a smell, I will try to clean them. This can involve bathing them, wiping their bodies with a wet towel, or changing their diapers. I will continue until the smell is gone. It doesn’t affect my relationship with them because manging body odour is part of my job.” #3
“Some elderly individuals are aware of changes in their body odour and often apologize to me when I assist with cleaning or changing their diapers. They feel embarrassed because they feel unable to care for themselves. I frequently reassure them that this is a normal aspect of ageing and that growing old is a universal experience we all must face.” #7
Discussion
This qualitative study provides valuable insights into how female caregivers in a Hong Kong private nursing home perceive, interpret, and manage body odour among older residents. Caregivers’ descriptions of “strong” and “musty” odours echo experimental work on age-related changes in volatile organic compounds, including increased levels of aldehydes such as 2-nonenal and alterations in skin lipid oxidation. Importantly, participants did not express overtly dehumanising or rejecting attitudes towards residents with strong odours; instead, they described professional habituation, emotional coping, and continued commitment to care. This contrasts with public stereotypes that equate “old people smell” with neglect and aligns with ethnographic accounts showing that caregivers actively negotiate the stigma attached to “dirty work” while maintaining a positive care identity.
The confidential, non-anonymous interview setting likely shaped how caregivers articulated these experiences. Under such conditions, professional norms of loyalty to the organisation and expectations of emotional self-control may have constrained the explicit expression of anger, disgust, or criticism of institutional practices. It is plausible that anonymous or off-site interviews may elicit more candid accounts of moral distress or negative emotions towards residents, and more detailed descriptions of coping behaviours such as avoidance or informal complaints. The relatively muted accounts of conflict and blame, together with emphasised narratives of adaptation and duty in the study, should therefore be interpreted not as the absence of ambivalence, but as reflections of what caregivers felt was professionally appropriate to disclose in a non-anonymous research encounter. Future studies using anonymous survey methods or focus groups on neutral settings could complement these findings by probing perceptions and emotions that may be more difficult to voice out when one’s professional identity and workplace are recognisable.
Caregivers in this study used odour as a non-verbal clinical cue and highlighted the potential role of olfactory assessment in geriatrics care by associating particular smells with medical conditions and adjusting care accordingly (13). These observations are consistent with evidence that metabolic and infectious conditions that are common in later life produce distinctive breath and wound odours that can support clinical assessment. Within nursing homes, caregivers’ ability to interpret such olfactory cues may facilitate early recognition of changes in health status, particularly where residents have cognitive impairment or communication difficulties. Caregivers linked odour intensity with frailty, dependency in activities of daily living, and incontinences, which are domains that are strongly associated with psychosocial consequences such as embarrassment, withdrawal, and reduced dignity. These findings underscore the value of addressing body odour as both a physiological phenomenon and a psychosocial stressor. Comprehensive odour management strategies that integrate physical hygiene, skin integrity, continence care, and emotional support may therefore help preserve quality of life and staff-resident relationships in long-term care.
In terms of odour management, caregivers primarily relied on standard hygiene practices rather than on specialised products. Caregivers did not report use of deodorising sprays or fragranced products to neutralise odours, and this may reflect their considerations regarding residents’ skin sensitivity, awareness of co-morbidities or cost limitations in resource-constrained settings. It may also indicate an underlying professional ethic in which odour control is understood primarily as restoring cleanliness and bodily integrity, rather than cosmetically masking smells. Caregivers also implicitly linked residents’ body odour to their own sense of professional performance and to perceptions of care quality. Some participants expressed determination to continue cleaning “until the smell is gone”, indicating that the absence of malodour was experienced as both a marker of residents’ dignity and an indicator that they had fulfilled their caregiving responsibilities. Persistent odours were viewed as a source of embarrassment and as a potential trigger for external judgements that the environment was unclean, reinforcing ageist stereotypes about institutional care. Therefore, body odour becomes an olfactory proxy for quality of care, used not only by visitors but also by caregivers themselves as a form of self-assessment and validation.
Despite these insights, odour management remained an under-recognised and under-resourced domain of practice. Caregivers reported no structural training or environmental interventions tailored to addressing body odour, although international geriatric nursing guidelines have increasingly emphasized the sensory qualities of care environments as key to maintaining residents’ dignity and quality of life (14). In Hong Kong’s high-density and resource-limited residential care sector, integrating olfactory considerations into standard guidelines could include training modules on clinical significance of odour changes, hygiene routines tailored to different levels of depends and communication stratifies for discussing odour sensitively with residents and families. Such measures could support caregivers in applying olfactory information consistently and safely, and distribute responsibility at an organisational rather than solely an individual level.
This study has several limitations. The single-site, private sector setting limits transferability to public facilities, other regions and community-dwelling older adults with different cultural norms and environmental conditions. The small, all-female sample, although justified by information power for an in-depth qualitative study, precluded comparisons by gender, role or cultural background. Conducting interviews in a non-anonymous workplace context increases the likelihood of social desirability bias, including the downplaying of negative emotions towards residents or explicit criticism of organisational policies. Future research should include multi-site samples, incorporate male caregivers and residents’ own perspectives, and link qualitative accounts with objective assessment of environmental and body odours to further clarify the relationships between biological, sensory, and social dimensions of body odour in later life.
Authorship / CRediT authorship contribution statement: All authors designed the study, acquired the data, analysed the data, drafted the manuscript and critically revised the manuscript for important intellectual content. All authors had full access to the data, contributed to the study, approved the final version for publication, and take responsibility for its accuracy and integrity.
Declaration of Conflicting Interest: All authors have disclosed no conflicts of interest.
Funding: This study received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Declaration of the use of generative AI and AI-assisted technologies in scientific writing and in figures, images and artwork: Artificial Intelligence played no role in the analysis of the data, the authors’ preparation or internal review of this manuscript.
Ethical standards: The study protocol and the above-mentioned consent procedures received approval from the Survey and Behavioural Research Ethics Board of Chinese University of Hong Kong (#S06906834) and the Institutional Review Board of the Anthropology Department at Sun Yat-Sen University (#86-20-84114275).
Data statement: All data generated or analysed during the present study are available from the corresponding author on reasonable request.
Acknowledgements: None.
Open Access: This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits use, duplication, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license and indicate if changes were made.
References
1. Haze S, Gozu Y, Nakamura S, Kohno Y, Sawano K, Ohta H, et al. 2-Nonenal newly found in human body odor tends to increase with aging. J Invest Dermatol. 2001;116(4):520-4
2. Gallagher M, Wysocki CJ, Leyden JJ, Spielman AI, Sun X, Preti G. Analyses of volatile organic compounds from human skin. Br J Dermatol. 2008;159(4):780-91.
3. Heinrich-Sanchez Y, Vital M. Trimethylamine-N-oxide formation, the bacterial taxa involved and intervention strategies to reduce its concentration in the human body. Ann Med. 2025; 57(1): 2525403
4. Wang Z, Wang C. Is breath acetone a biomarker of diabetes? A historical review on breath acetone measurements. J Breath Res. 2013;7(3):037109.
5. Van den Velde S, Nevens F, Van Hee P, van Steenberghe D, Quirynen M. GC–MS analysis of breath odor compounds in liver patients. J Chromatogr B Analyt Technol Biomed Life Sci. 2008;875(2):344-8.
6. Dugan E, Cohen SJ, Robinson D, Bogart LM, Ake CF, Streuber P, et al. Urinary incontinence and psychological distress in community-dwelling older adults. J Am Geriatr Soc. 2002;50(3):489-95.
7. Sorokowska A, Schriever VA, Gudziol V, Hummel C, Hähner A, Iannilli E, et al. Sex differences in human olfaction: a meta-analysis. Front Psychol. 2019;10:242.
8. Wong SY, Chan AW, Chen H. Workforce challenges in Hong Kong’s elderly care sector: a gender perspective. Asia Pac J Soc Work Dev. 2019;29(4):287-302.
9. Malterud K, Siersma VD, Guassora AD. Sample size in qualitative interview studies: guided by information power. Qual Health Res. 2016;26(13):1753-60.
10. O’Brien BC, Harris IB, Beckman TJ, Reed DA, Cook DA. Standards for reporting qualitative research: a synthesis of recommendations. Acad Med. 2014;89(9):1245-51.
11. Katz S, Ford AB, Moskowitz RW, Jackson BA, Jaffe MW. Studies of illness in the aged. The index of ADL: a standardized measure of biological and psychosocial function. JAMA. 1963;185:914-9.
12. Braun V, Clarke V. Using thematic analysis in psychology. Qual Res Psychol. 2006;3(2):77-101.
13. Shirasu M, Touhara K. The scent of disease: volatile organic compounds of the human body related to disease and disorder. J Biochem. 2011;150(3):257-66.
14. Backman C, Demery-Varin M. Impact of sensory interventions on the quality of long-term care residents: a scoping review. NMJ Open. 2021;11(3): e042466
The Author(s) 2026