S. Goorang1, L. Ausman1, R. Houser1, S.J. Whiting2
1. Tufts University Boston MA USA, 2. University of Saskatchewan Saskatoon SK Canada. Corresponding author: , Susan J Whiting, College of Pharmacy and Nutrition, 110 Science Place, University of Saskatchewan, Saskatoon SK S7N 5C9 Canada, E: susan.whiting@usask.ca, T: 1-306-9665837
Abstract
Background: Although studies have evaluated the use of vitamin and mineral supplements in the general population and community-dwelling older adults, little is known about the use of these products among long-term care (LTC) facility residents. These individuals, who tend to take more medications and are particularly at risk of undernutrition and micronutrient deficiencies, may benefit from using vitamin and/or mineral supplements. Alternatively, getting too much of these nutrients may increase risk of excessive intake or drug-supplement interactions. Thus, it is important to document supplement use among elders living in institutions. Objective: To examine the prevalence of use of different types of vitamin and mineral supplements among institutionalized elderly people in nursing homes and assisted living facilities. Design: A systematic review was conducted in July 2013 of Medline and Embase databases using key terms for LTC facilities and vitamin-mineral supplements. Filters used to narrow down the results included publication year after 1997, English language, human studies, and adult/aged population. Results: Of the 1825 publications identified, 892 were excluded after applying filters. After eliminating duplicates, 676 records were screened by either title or abstract, excluding 617. Full text of the remaining 59 articles was reviewed and 5 studies were selected. Conclusions: Very few studies have provided comprehensive information about the use of vitamin and mineral supplements among institutionalized elderly people. There appears to be some challenges associated with conducting research among this vulnerable population who have advanced age and multiple chronic diseases, and further studies are warranted.
Key words: Long-term care facility, elderly, vitamin and mineral supplements.
Introduction
Dietary supplements are widely available to consumers worldwide and use of these products has significantly increased during the past two decades. The subject of nutritional supplement usage is of interest to researchers who have examined the use of these products among different population groups. People may use these products for different reasons such as improving or maintaining overall health, illness prevention, strengthening the immune system, and a general concern about their health (1, 2).
In particular, the use of dietary supplements is prevalent in older adults, many of whom are residing in institutions. Older adults have specified their use of supplements for maintaining the health of their heart, bones, joints, and eyes (1). The institutionalized elderly people who live in nursing homes and assisted living facilities usually have multiple health problems and may need a higher level of care. Some of these individuals may benefit from the use of various categories of supplements, for example, for adults over 50 years of age, a vitamin B12 supplement (or intake of food fortified with synthetic B12) is recommended (3); for adults over 70 y, a vitamin D supplement would be needed to meet the RDA of 800 IU, and adults younger than this may have trouble meeting the RDA of 600 IU from foods alone; and calcium requirements for women over 50 y and men over 70 y, at 1200 mg, would be difficult to meet from food alone (4,5). However, there may also be some negative consequences associated with excessive use of these products including drug-supplement interactions.
There are different types of nutritional supplements. Oral nutritional supplements (ONS) are a group of nutritional supplements which are available in the market in the form of juice or milk (6), and as they contain energy and often protein in addition to micronutrients, they are prescribed to those with poor appetite, weight loss, frailty, and wound healing (7-9). Herbal remedies are another group of alternative medications used by the elderly people residing in LTC centers (10, 11). It is the vitamin and mineral supplements that are among the most popular and commonly used dietary supplements. Regular consumption of multivitamin and mineral supplements has been reported among more than 30% of the US adult population (12). Use of vitamin and mineral supplements is common in institutionalized older adults. These seniors may benefit from the use of different type of vitamin and/or mineral supplements to overcome several micronutrient deficiencies they may have; however, caution must be taken in using these products. Therefore, it is important to know the prevalence of use of different types of micronutrient supplements in this group of people. Although the number of institutionalized elderly people is increasing, information on the rate and profile of use of vitamin and mineral supplements among this group of individuals are scarce. The reason might be that obtaining information from this population is very difficult because national surveys do not examine use in institutions. The aim of the current systematic review was to assess prevalence of use of different types of vitamin-mineral supplements among residents living in LTC facilities.
Methods
The literature search was carried out utilizing the following databases: Medline (via Web of Knowledge) and Embase (via Ovid). The search was completed in July 2013.
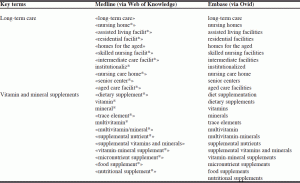
In both of the databases, search was performed in a way that at least one key term for long-term care, and one key term for vitamin and mineral supplements exist. Medline was searched for in topic and Mesh. Similarly, Embase was searched using key word and/or subject heading. The details of the searches in both databases are shown in Table 1.
As the Recommended Dietary Allowances (RDAs) have changed over the years and the latest editions of the Dietary Reference Intakes (DRIs) began in the year 1997 (3), only articles since 1997 were included. Other limiters include English language and studies of humans. Journals found in Embase were limited to adult (18 to 64) and aged (65+ years) and in Medline, excluded mesh headings were child, child preschool, adolescent, and young adults.
Results
In order to identify studies relevant to the research question, several steps were taken (13), as shown in Figure 1. After identifying the relevant publications from an initial search capturing 1825 potential titles, filters were applied on the results of both databases to obtain 933 studies, from which duplicates were excluded. Titles and abstracts were examined, and those not fitting the topic were excluded. Fifty-nine studies were examined in detail, and from these, many were excluded as outlined in Figure 1. For example, 32 were excluded because they did not provide sufficient information regarding the rate and profile of use of different types of vitamin and mineral supplements. Indeed, many of these studies had a predetermined focus, such as vitamin D and calcium, or antioxidants, and thus were excluded, as the intent of the systematic review was a full accounting of vitamin and mineral use.
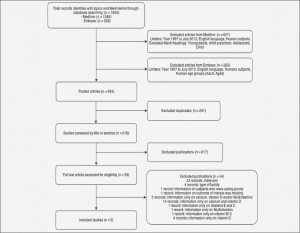
Figure 1 Flow chart of the systematic review of the prevalence of use of vitamin and mineral supplements among elderly institutionalized adults
Five studies that contained relevant information were kept for this review. Their details are shown in Table 2. The study by Viveky et al. (14), conducted in Canada, was a descriptive cross-sectional study of the prevalence of vitamin-mineral supplement usage in older adults (65 years and older) who lived in a large LTC facility. Consumption of vitamin and mineral supplements was similar among elderly people with and without dementia. Additionally, some residents consumed as many as 6 different supplements per day and were at risk for supplement overuse, which also added to the overall burden of medication use. Lam and Bradley (15) did a similar study in the United States. They found that the most commonly used product was a multiple vitamin. They also found prevalent duplicate use of multivitamins from different brands that were used as self-prescribed, over-the-counter (OTC) drugs as well as prescription products, and calcium salts that were prescribed for osteoporosis prevention and treatment, and used as an antacid.
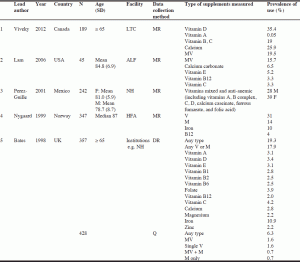
Table 2 Five selected studies in the systematic review of the prevalence of use of vitamin and mineral supplements among elderly institutionalized adults
Perez-Guille et al. (16) conducted their study in Mexico. They found that vitamin-mineral supplements were more regularly prescribed to people who suffered from CVD. Nygaard and Naik (17) conducted a study in Norway to assess drug use among elderly residents who were mentally impaired and those who were not. There were no differences in usage between these two groups except for vitamin B12. Bates et al. (18), in the United Kingdom, determined nutritional supplement usage among people ≥65 years, using data from 4-day diet records in a sample that was only 20% living in institutions. The previous four studies were conducted among institutionalized elderly only, and supplement usage was determined from medical records. In contrast to findings of the first four studies, in the last study, few people (17.9 %) ever used any vitamin/mineral supplements; however, 4-days may not capture regular use.
It should be noted that some of the selected studies only focused on examining vitamin-mineral supplements that were used in the form of tablets or capsules, while others measured vitamin and mineral that was consumed in different forms such as pills, drops, syrups, and ONS. Furthermore, in one of these studies “vitamin mixed” as a group of medication was described; thus, prevalence and quantity of different types of vitamins and/or mineral supplements used by residents could not be identified. An additional point is that four of these five studies obtained information through reviewing patients’ medical records but one study achieved the data through both questionnaire and diet records. Based on examining the five studies, determining the overall prevalence and type of supplement used by the institutionalized elderly people was not possible. These studies were conducted in five different countries each with different food habits and availability.
Discussion
The studies in this systematic review raise a number of concerns. First, the duplication in products used by some subjects suggests the medical practitioners may not have been well informed on use of products, thus safety would be an issue (19, 20). Second, older adults may not have higher need for all vitamins. A recent review suggested that older individuals may have an increased requirement for vitamins such as B6, B12, folate, and vitamin D, but there still is not enough evidence to show that these people need more of the other vitamins including thiamin, niacin, riboflavin, vitamins C and E (21). Finally, while older people who reside in LTC settings usually have multiple chronic health problems so perhaps need vitamins and minerals, there is the concern that they also use many different types of medications. The five selected studies raised concerns regarding polypharmacy, and risk of drug-supplement interactions.
In order to provide a greater level of care to institutionalized elders and improve their quality of life, more information regarding the supplement usage pattern in these individuals should be gathered to prevent these safety concerns from being realized.
Institutionalized elderly people usually have physiological decline, multiple comorbidities and underlying health conditions and take several medications. As a result, some of them may face undernutrition and require more energy, protein and micronutrients. On the other hand, with taking too many drugs as well as dietary supplements, risk of duplicative use as well as drug-nutrient interactions is high in this population. With the growing number of older adults who live in LTC centers and the potential risks and benefits of vitamin and mineral supplements usage, it is important to know about the prevalence of use of different types of vitamin and mineral supplements among these residents. It is also important to know who is most at risk so health officials could successfully target them for intervention.
Acknowledgements: None of the authors has a conflict of interest.
Funding: there were no funding sources for this work
References
1. Bailey RL, Gahche JJ, Miller PE, Thomas PR, Dwyer JT. Why US adults use dietary supplements. JAMA Internal Medicine 2013;173:355-61. doi: 10.1001 /jamainternmed.2013.2299
2. Health Canada, Ipsos-Reid (Firm). Natural Health Product Tracking Survey, 2010: Final Report. Health Canada. http://www.hc-sc.gc.ca/dhp-mps/prodnatur/index-eng.php. Accessed 26 August 2013
3. Otten JJ, Hellwig JP, Meyers LD. Dietary Reference Intakes: The Essential Guide to Nutrient Requirements. The National Academies Press, Washington DC, 2006.
4. Verbrugge FH, Gielen E, Milisen K, Boonen S. Who should receive calcium and vitamin D supplementation? Age Ageing. 2012;41(5):576-80.
5. Institute of Medicine (IOM). Dietary Reference Intakes for calcium and vitamin D. The National Academy Press, Washington DC, 2011
6. Hines S, Wilson J, McCrow J, Abbey J, Sacre S. Oral liquid nutritional supplements for people with dementia in residential aged care facilities. Int J Evid Based Healthc 2010;8:248-251. doi: 10.1111/j.1744-1609.2010.00186.x
7. Barr M, Kane M. Nutritional product use and practice in nursing and residential homes. Nursing standard (Royal College of Nursing (Great Britain) : 1987) 2002;16:33-39
8. Johnson LE, Dooley PA, Gleick JB. Oral nutritional supplement use in elderly nursing home patients. J Am Geriatr Soc 1993;41:947-952
9. Johnson S, Nasser R, Banow T, et al. Use of oral nutrition supplements in long-term care facilities. Can J Diet Pract Res 2009;70:194-198. doi: 10.3148/70.4.2009.194
10. Harms SL, Garrard J, Schwinghammer P, Eberly LE, Chang YP, Leppik IE. Ginkgo biloba use in nursing home elderly with epilepsy or seizure disorder. Epilepsia 2006;47:323-329. doi: 10.1111/j.1528-1167.2006.00424.x
11. Spoelhof GD, Foerst LF. Herbs to magnets: managing alternative therapies in the nursing home. Ann Longterm Care 2002;10:51-57
12. Marra MV, Boyar AP. Position of the American Dietetic Association: nutrient supplementation. J Am Diet Assoc 2009;109:2073-2085. doi: 10.1016/j.jada.2009.10.020
13. Khan K, Kunz R, Kleijnen J, Antes G. Systematic reviews to support evidence-based medicine. Hodder Arnold, London, England, 2011
14. Viveky N, Toffelmire L, Thorpe L, et al. Use of vitamin and mineral supplements in long-term care home residents. Appl Physiol Nutr Metab 2012;37:100-105. doi: 10.1139/H11-141
15. Lam A, Bradley G. Use of self-prescribed nonprescription medications and dietary supplements among assisted living facility residents. J Am Pharm Assoc 2006;46:574-581. doi: 10.1331/1544-3191.46.5.574.Lam
16. Perez-Guille G, Camacho-Vieyra A, Toledo-Lopez A, et al. Patterns of drug consumption in relation with the pathologies of elderly Mexican subjects resident in nursing homes. J Pharm Pharm Sci 2001;4:159-166
17. Nygaard H, Naik M. Drug use in homes for the aged. A comparison between mentally intact and mentally impaired residents. Aging (Milano) 1999;11:186-193
18. Bates C, Prentice A, van der Pols J, et al. Estimation of the use of dietary supplements in the National Diet and Nutrition Survey: People Aged 65 Years and Over. An observed paradox and a recommendation. Eur J Clin Nutr 1998;52:917-923. doi: 10.1038/sj.ejcn.1600665
19. Marinac JS, Buchinger CL, Godfrey LA, Wooten JM, Sun C, Willsie SK. Herbal products and dietary supplements: a survey of use, attitudes, and knowledge among older adults. J Am Osteopath Assoc 2007;107:13-20; quiz 21-3
20. Gardiner P, Phillips R, Shaughnessy AF. Herbal and dietary supplement-drug interactions in patients with chronic illnesses. Am Fam Physician 2008;77:73-78
21. McCormick DB. Vitamin/Trace Mineral Supplements for the Elderly. Adv Nutr 2012;3:822-824. doi: 10.3945/an.112.002956