P. de Souto Barreto1, V. Zanandrea1,2, M. Lapeyre-Mestre3,4, M. Cesari1,3, B. Vellas1,3, Y. Rolland1,3
1. Gérontopôle de Toulouse, Institut du Vieillissement, Centre Hospitalo-Universitaire de Toulouse, France; 2. Clinica Geriatrica, University of Verona, Italy; 3. Inserm U1027, University of Toulouse III, Toulouse, France; 4.Department of Clinical Pharmacology, Toulouse University Hospital (CHU Toulouse), Toulouse, France. Corresponding author: Dr. Philipe de Souto Barreto. Gérontopôle de Toulouse, Institut du Vieillissement. 37, Allées Jules Guesde, 31000 Toulouse, France. Telephone number: (+33) 561 145 668, Fax: (+33) 561 145 640, e-mail: philipebarreto81@yahoo.com.br
Abstract
Background: Obesity in older people is a growing health problem in developed countries including among nursing home (NH) patients. However, little is known about the characteristics of obese NH residents and the specific organization of care devoted for these patients. Methods: Data are from 4168 patients recruited among the 175 NHs from Midi-Pyrénées, South-Western, France. Patient’s characteristics (e.g., demographics, weight changes, comorbidities, treatments, diet) are explored according to the body mass index (BMI) groups and NH specificities (e.g., ownership, number of beds, number of NH staff). Results: About 18.5% of NH residents were obese. Obese patients were significantly younger and less disabled than non-obese. They had a significantly higher prevalence of hypertension, diabetes, peripheral vascular disease, psychiatric diseases and pain than non-obese residents, and had a lower prevalence of dementia and stroke. No weight change and weight gain in the past two months were significantly more prevalent in the obese group than in the non-obese one, despite of the higher rate of low salt, diabetic and hypo-caloric diet among obese people. Higher prevalence of obesity was found in NHs who less often had both dietitian and physical activity professional as a member of the staff. Conclusions: Very old and obese people living in NHs are a particular population, with specific care needs. Further studies are needed in order to define the optimal management of obesity in the NH resident.
Key words: Obesity, BMI, elderly, institutionalized, older adults.
Introduction
Older persons represent about 15% of the population in Western European countries and United States. This proportion is projected to increase to 25% by 2025 (1). The prevalence of overweight and obesity is simultaneously growing. In the National Health and Nutrition Examination Survey III (NHANES III), the age-adjusted prevalence of obesity in the United States increased from the beginning to the end of the Nineties from 22.9% to 30.5% (2); this same trend is also documented in older adults. In Europe, the prevalence of obesity in people 50 years and older varied across countries, reaching the prevalence of up to 20.2%.among men, and 25.6%among women (3).
In industrialized countries, between 2% and 5% of older persons resides in nursing homes (NH) (4). This population does not escape from such increasing prevalence of obesity, consequently raising a specific public health issue with more global economic implications (5,6). In the United States, only 15% of newly admitted NH residents were obese in 1992, but they were more than 25% in 2002 (5). Moreover, weight gain in overweight subjects is associated with an increased relative risk of institutionalization (7).
Obesity in community-dwelling adults and older persons (especially as a comorbid condition exposing to negative health-related events) has been widely-studied (8). Consensual guidelines about diet, exercise, surgical, and pharmacological treatment of obesity are available in literature (9,10). However, such recommendations were generally developed for the general population and may not be easily applicable or appropriate to the NH population. In fact, only few studies documented the characteristics of obese NH residents and the characteristics of NHs (e.g., structure and internal organization) that take care of this population (11, 12).
The purpose of this study is to report the prevalence and describe the characteristics of the NH residents according with obesity status. The study also examines the possible relationships between specific characteristics of the NHs and the prevalence of obesity in the NH.
Methods
This cross-sectional analyses are from the baseline assessments of the IQUARE (Impact d’une démarche QUAlité sur l’évolution des pratiques et le déclin fonctionnel des Résidents en Ehpad) study. The research protocol of IQUARE (trial registration number: NCT01703689) has been previously described (13). Briefly, IQUARE is a multi-centric, individually-tailored controlled trial conducted among 175 NHs in the Midi-Pyrénées region (South-Western France) (trial registration number: NCT01703689). IQUARE started in May 2011. The trial is aimed at improving quality indicators related to frequent medical problems faced by NH staff (e.g., obesity, polypharmacy, nutrition). Participating NHs were allocated to one of two groups:
1. Intervention group: consisting of an audit with following feedback and specific working groups (between university hospital geriatricians and the NH staff) in order to improve the NH quality indicators;
2. Control group: consisting of an audit with following feedback only.
IQUARE follows the principles of the Declaration of Helsinki and complies with ethical standards in France. Study protocol was approved by the Ethic Committee of the Toulouse University Hospital and the Consultative Committee for the Treatment of Research Information on Health (CNIL: 07-438).
Participants
A total of 6275 residents from the 175 NHs participate in the IQUARE study. Residents were randomly selected (excepted for NHs that had ≤ 30 potential participants, in which all residents were included in the study) on the basis of alphabetical order within each NH: NHs having 31 to 90 residents had to randomly select, according to alphabetical order (at a pace of 1 / 2 persons), from 30 to 45 participants; NHs with > 90 residents had to randomly select from 45 to 60 participants (at a pace of 1 / 3 persons). Two on-line questionnaires were completed by the NH staff: one questionnaire on the characteristics and health status (recorded by the NH medical staff, mainly coordinating physicians) of participating residents, the other on the NH structure and internal organization (recorded by the NH administrative staff, mainly the NH director). All drug prescribed to participants during the week of their inclusion in the IQUARE study were sent by the NH staff to the research team. The present analyses are based on the 4,168 participants with valid data for weight and height, and then, body mass index (BMI).
Obesity variable
Obesity is defined according to subject’s BMI, i.e., body weight (in kg) divided by squared height (in meters). Participants were categorized into the following groups: underweight (BMI < 18.5 kg/m2), normal weight (BMI between 18.5 kg/m2 and 24.9 kg/m2), overweight (BMI between 25.0 kg/m2 and 29.9 kg/m2), and obese (BMI ≥ 30 kg/m2).
Information on the current weight of participants and their weight two months before the recruitment was recorded. This gave the opportunity to create a variable measuring weight changes in the last two months. A relevant weight change was defined as a change higher than 1kg (14) and ≥2.5% of participants’ body weight .
NHs (n = 99) that measured weight and height in ≥ 80% of the residents were divided into quartiles according with the prevalence of obesity in the institution. From this, we grouped together the second and third quartiles. Since the absence of weight/height records in the NH may suggest organizational dysfunctions in the care of patients, a fourth category was created by grouping together the NHs (n = 25) that did not measure weight and height in any patient with those (n = 51) that measured weight and height in less than 80% of the residents. Therefore, NHs were grouped as follows: low prevalence of obesity (first quartile), medium prevalence of obesity (second and third quartiles), high prevalence of obesity (fourth quartile), and missing/incomplete data for BMI.
Other variables
The following individual-related variables were recorded from patients’ medical charts: age, sex, disability in feeding, disability in walking, diabetes, hypertension, congestive heart failure, myocardial infarction, stroke, peripheral vascular disease, psychiatric diseases (other than depression), dementia, cancer, Charlson Comorbidity Index (15), pain complaints, hospitalization during the last 12 months, wandering behavior, number of drugs, antipsychotics, antidiabetic drugs, and current specific diets (i.e., poor/without salt diet, hypocaloric diet, hypercaloric diet, diabetic diet).
The following NH-related variables were recorded and are considered in the present analyses: ownership of the NH (i.e., public, private non-profit, or private for-profit), number of beds, full-time equivalent (FTE) for the NH coordinating physician, for nurses, for nurses’ aide, presence of a dietitian, availability of a physical activity professional (e.g., physical therapist, instructor of physical activity), presence of physical activity classes ≥ once a week vs. < once a week or no physical activity, and a NH global disability score (measured by the French AGGIR grid, ranging from 70 to 1.000 with higher scores indicating higher general disability).
Statistical Analysis
Chi-square tests was used to analyze differences between categorical variables, whereas Kruskall-Wallis’ tests examined differences regarding discrete and continuous variables across obesity categories at the residents’ level and at the NH level (prevalence of obese residents). All the bivariate tests were adjusted for multiple comparisons using the False Discovery Rate (FDR) developed by Benjamini and Liu (16,17). Analyses were performed using Stata version 11 (College Station, TX: StataCorp LP).
Results
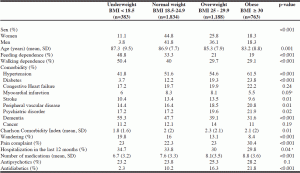
Table 1 shows the main characteristics of the 4168 NH residents with available data on BMI. About 18% of participants (n=763) were obese. Obese residents were significantly younger and had a lower prevalence of feeding and walking disability compared to the non-obese groups. Moreover, they had a significantly higher prevalence of hypertension, diabetes, psychiatric disorder and peripheral vascular disease, and more frequently reported pain. Obese residents had lower prevalence of stroke and dementia compared to the other BMI groups. Obese NH residents took more medications than other BMI groups, especially antidiabetic drugs, and were less often wanderers.
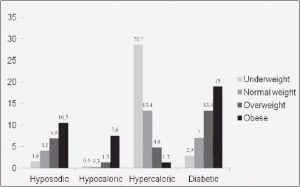
With regard to diet types, overall 1276 (30.6%) of the 4168 residents with available data on BMI had a specific diet: among them, 244 (5.8%) patients followed a hyposodic diet, 81 (1.9%) a hypocaloric diet, 423 (10.1%) a hypercaloric/high protein diet and 444 (10.6%) a diabetic diet. Obese NH residents were significantly more likely to follow a hyposodic, hypocaloric, and diabetic diet compared to non-obese groups, whereas underweight residents were more often following hypercaloric/hyperproteic diets compared to the other groups. Data about specific types of diet according to classes of BMI are shown in Figure 1.
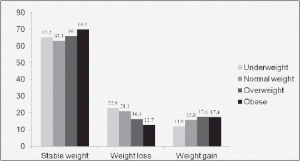
The 2-month weight change across BMI categories are shown in Figure 2. Information about weight change was available for 3789 patients. About 65.4% of these patients (n=2478) remained stable over time. Among those experiencing a weight change, 696 (18.4%) and 615 (16.2%) participants lost and gained weight, respectively. Weight change significantly differed across BMI categories (p<0.001). Underweight residents more often lost further weight, whereas overweight/obese people tended to further gain weight.
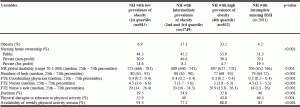
Regarding NH classification according with the prevalence of obesity, 99 NHs measured weight and height in ≥ 80% of their residents: 27 NHs (n = 983) had a low prevalence of obesity, 48 NHs (n = 1749) had an intermediate prevalence of obesity, and 24 NHs (n = 852) had a high prevalence. 25 NHs (n = 845) did not measure weight and height in any resident and 51 NHs (n = 1846) measured these variables in less than 80% of the residents (overall, only 41.9% of people from these 51 NHs had data on BMI); the 76 NHs with no/incomplete data on BMI constituted the category “NH with incomplete/missing BMI”. Table 2 shows the main characteristics of NHs according to their prevalence of obesity. Of note, high prevalence of obesity was found in public NHs, NHs with lower number of beds, and NHs that less frequently had in their staff both a dietitian and a physical activity professional.
Discussion
This study described for the first time in a large population of people living in NHs the characteristics of obese NH residents as well as the prevalence of obesity in this institutional setting. Another strength of this study is that it described how obese residents are cared in terms of diet and selected medications.
Despite low salt, low calories and diabetes diet were more prescribed in the obese residents, they significantly gained weight more frequently, compared to normal and underweight patients. NH ownership was related to the quantity of obese patients and public NHs had more frequently a higher obesity rates.
Some studies reported the negative effect of high BMI on cardiovascular diseases (8) and survival (18,19). For this reason obese people living in NHs, a population characterized by a very old age, can be considered as survivors to their own obesity. This may mean that obese people who have had myocardial infarction or stroke, diseases less prevalent among obese residents, probably died before becoming old, even though we cannot exclude the possibility that people became obese in their late-life.
The high prevalence of anti-diabetic treatment is not surprising in obese residents since these people also had a higher prevalence of diabetes compared with non-obese people. The use of antidiabetics may also have contributed to weight gain in overweight and obese NH residents; indeed, the association of these drugs with weight gain is well-established (20). Obese people also had the highest rate of antipsychotic treatment (non-significant), a drug associated with weight gain. Interestingly, weight gain occurred despite obese residents have been more often under both caloric and salt restriction. . However, diet alone is probably not an effective way to reduce weight and improve health in older people, if it is not combined with physical activity (9). It is noteworthy that NHs with lower rates of obesity had the highest percentages of weekly physical activity sessions and physical activity staff.
Finally more than half of NHs with high rates of obese residents were public and only very few were private for-profit. We may suggest that private NHs prefer to take care of normal weight or underweight patients, since taking care of obese people asks for more staff, and then higher costs. In fact, although French NHs receive financial support from the government according, for example, with the global disability score of the institution, weight and obesity are not taking into account for funding purposes. However, for the same level of disability, obese residents require more human assistance than non-obese residents (11,12). They usually require additional staff to be moved or lifted, receive multiple medications and suffer from numerous metabolic complications (12). The concerns about additional costs related to obesity may lead some NHs to consider obese patients ineligible for admission in the institution (12).
One limitation of this study is the impossibility to distinguish if weight changes were unintentional (related to anorexia, dehydration, infection, chronic disease and fluid retention or other reasons), or intentional. For this reason it is difficult to interpret changes in weight in relation only to physical activity and diet. Our results may have been biased by the high rate (33.6%) of missing data concerning BMI.
The present study provides a comprehensive update on practices regarding obesity in NH. Available data describing the NH population are still limited. Very few data are currently available about care offered to treat obesity among NH residents (11,12). To our knowledge, this is the first large-scale study of obesity in NH.
In conclusion, our study represents a first step in the understanding of the clinical phenomenon of obesity in the institutionalized older adult population. Optimal management of obesity in NH residents remains to be defined due to the lack of data on the topic for this specific population. Further studies are needed to improve our knowledge of this public health priority and to create the foundations for generating specific clinical guidelines and recommendations to treat obesity in the NH setting.
Conflict of interest: All authors declare no conflict of interests.
Ethical standard: IQUARE follows the principles of the Declaration of Helsinki and complies with ethical standards in France. Study protocol was approved by the Ethic Committee of the Toulouse University Hospital and the Consultative Committee for the Treatment of Research Information on Health (CNIL: 07-438).
References
1. Elia M. Obesity in the elderly. Obes Res 2011;9:244S-248S.
2. Flegal KM, Carroll MD, Ogden CL, Johnson CL. Prevalence and trends in obesity among US adults, 1999-2000. JAMA. 2002;288(14):1723-7.
3. Andreyeva T, Michaud PC, van Soest A. Obesity and health in Europeans aged 50 years and older.. Public Health. 2007;121(7):497-509.
4. Ribbe MW, Ljunggren G, Steel K, Topinková E, Hawes C, Ikegami N, et al. Nursing homes in 10 nations: a comparison between countries and settings. Age Ageing. 1997;26 Suppl 2:3-12.
5. Lapane KL, Resnik L. Obesity in nursing homes: an escalating problem. J Am Geriatr Soc. 2005;53(8):1386-91.
6. Lakdawalla DN, Goldman DP, Shang B. The health and cost consequences of obesity among the future elderly. Health Aff (Millwood). 2005;24 Suppl 2:W5R30-41.
7. Zizza C, Herring A, Domino M, Haines P, Stevens J, Popkin BM. The effect of weight change on nursing care facility admission in the NHANES I Epidemiologic Followup Survey. J Clin Epidemiol. 2003;56(9):906-13.
8. Salihu HM, Bonnema SM, Alio AP. Obesity: What is an elderly population growing into? Maturitas. 2009; 20;63(1):7-12.
9. Mathus-Vliegen EM; Obesity Management Task Force of the European Association for the Study of Obesity. Prevalence, pathophysiology, health consequences and treatment options of obesity in the elderly: a guideline. Obes Facts. 2012;5(3):460-83.
10. Han TS, Tajar A, Lean ME. Obesity and weight management in the elderly.Br Med Bull. 2011;97:169-96.
11. Felix HC. Personal care assistance needs of obese elders entering nursing homes. J Am Med Dir Assoc. 2008;9(5):319-26.
12. Rotkoff N. Care of the morbidly obese patient in a long-term care facility. Geriatr Nurs. 1999;20(6):309-13.
13. P. De Souto Barreto, M. Lapeyre-Mestre, C.Mathieu, C.Piau, C. Bouget, F.Cayla, B.Vellas, Y.Rolland. J Nutr Health Aging. A multicentric individually-tailored controlled trial of education and professional support to nursing home staff: research protocol and baseline data of the IQUARE study. In press.
14. Beck A.M., Damkjær K., Simmons S.F.. The relationship between weight status and the need for health care assistance in nursing home residents. Journal of Aging Research & Clinical Practice. 2012; 1(2): 173-177.
15. McGregor JC, Kim PW, Perencevich EN, Bradham DD, Furuno JP, Kaye KS, Fink JC, Langenberg P, Roghmann M-C, Harris AD Utility of the Chronic Disease Score and Charlson Comorbidity Index as comorbidity measures for use in epidemiologic studies of antibiotic-resistant organisms. Am J Epidemiol. 2005; 161:483–493.
16. Benjamini Y, Drai D, Elmer G, Kafkafi N, Golani I. Controlling the false discovery rate in behavior genetics research. Behav. Brain Res. 2001; 125(1-2):279-284.
17. Benjamini Y, Liu W. A distribution-free multiple test procedure that controls the false discovery rate. Tel Aviv. RP-SOR-99-3: Department of Statistics and O.R., Tel Aviv University, 1999. Accessed on December 12th 2012. Available at: http://www.math.tau.ac.il/~ybenja/BL2.pdf
18. Dyer AR, Stamler J, Garside DB, Greenland P. Long-term consequences of body mass index for cardiovascular mortality: the Chicago Heart Association Detection Project in Industry study. Ann Epidemiol. 2004;14(2):101-8.
19. Hu FB, Willett WC, Li T, Stampfer MJ, Colditz GA, Manson JE. Adiposity as compared with physical activity in predicting mortality among women. N. Engl. J. Med. 2004 23;351(26):2694-703.
20. Bailey CJ: The challenge of managing coexistent type 2 diabetes and obesity. BMJ 2011; 342:d1996.
21. Rolland Y, Kim MJ, Gammack JK, Wilson MM, Thomas DR, Morley JE. Office management of weight loss in older persons. Am J Med. 2006;119(12):1019-26).
22. Rolland Y, Abellan van Kan G, Hermabessiere S, Gerard S, Guyonnet Gillette S, Vellas B. Descriptive study of nursing home residents from the REHPA network. J Nutr Health Aging. 2009;13(8):679-83.