J. Robles-Suarez1, L.D. Sinvani1, L. Rosen2, C.N. Nouryan3, G. Wolf-Klein1,4,5
1. Division of Geriatric Medicine, North Shore-LIJ Health System, Manhasset, NY; 2. Biostatistics Division, Feinstein Institute for Medical Research, Manhasset, NY; 3. Division of Health Services Research, North Shore-LIJ Health System, Great Neck, NY; 4. Division of Geriatrics, Department of Medicine, Albert Einstein College of Medicine, Bronx, NY;5. Department of Medicine, Hofstra North Shore-LIJ School of Medicine, Hofstra University, Hempstead, NY. Corresponding author: Christian Nouryan, NSLIJ Health System, 175 Community Drive 2nd Floor, Great Neck, NY 11021, cnouryan@nshs.edu
Abstract
Background: Today, up to 90% of rehospitalizations from long term care (LTC) facilities appear to be unplanned. Studies have found laboratory values indicating low levels of hydration in as many as 48% to 60% of subjects in both hospitalized and community-dwelling older adults. Objectives: This study’s objective was to identify the prevalence of low hydration, a potentially treatable condition, in patients who were rehospitalized from a LTC facility. Design: This was a retrospective chart review of patients rehospitalized within 30 days of LTC facility admission. For this study, low hydration was defined as a Serum Na >145 mg/dl or a blood urea nitrogen to creatinine (BUN:Cr) ratio of > 20:1. Setting: A hospital and a nearby LTC facility in the metropolitan New York area. Participants: Any patient over age 65 who was sent back to the hospital for any reason within 30 days of entering the LTC facility. Measurements: demographics, admission diagnosis, co-morbid conditions, electrolyte changes (Na, BUN, and Cr), and reason for transfer. Results: There were 261 subjects rehospitalized during the six-month study period. Average age was 79 years, and 42% were male. The principal diagnoses at LTC admission were: cardiovascular (34%), infection (20%), neurological (14%), gastrointestinal (13%), gynecological (4%), pulmonary (3%), fall (2%), electrolyte abnormality (including documented dehydration, 2%), hematology (1%) and other (6%). For these subjects, the prevalence of low hydration at time of LTC facility admission was 60.5% (95% CI: 54.3% to 66.5%), at time of rehospitalization, low hydration prevalence had increased to 67.4% (95% CI: 61.4% to 73.1%). Conclusion: Low hydration appears to be an unrecognized clinical issue for older adults requiring LTC and hospital readmission. Increasing awareness of this condition might assist in improving the patient’s fluid status prior to discharge from the hospital thereby potentially preventing avoidable readmissions.
Key words: Dehydration, long term care, rehospitalization.
Introduction
In the United States, it has been estimated that as many as 20% of Medicare beneficiaries are rehospitalized within 30 days of discharge, either from the community, or from long term care (LTC) facilities (1-3). The Centers for Medicare and Medicaid Services health system reform law created the Hospital Readmissions Reduction Program, aiming at reducing these readmissions (4). As of October 2012, about two-thirds of US hospitals have faced potential penalties with a impending loss of $300 million in Medicare payments for 2013 alone (5). Of importance, 90% of these rehospitalizations are non-elective, and up to one third are thought to be potentially avoidable (6, 7). It should be noted, however, that a concrete definition of an avoidable rehospitalization has not been established – estimates in one review were found to vary between 5% and 79% (8).
Low hydration in the frail elderly is a well-established phenomenon, especially for those who have recently had surgery, are hospitalized, or are living in LTC facilities (9-11). Past studies have identified specific factors that are associated with low hydration in elders including decreased thirst, medications (such as diuretics), dysphagia, delirium, dementia, depression, sedation and diarrhea (12, 13).
Despite its prevalence, few studies have specifically examined the role of low hydration in the rehospitalization process of older adults (14-16). A search of PubMed.Gov performed in June 2013 returned no results for “hypernatremia rehospitalization” and only ten results for “dehydration rehospitalization” – five of which refer to newborns (17).
It has been established that a sizeable number of hospitalized patients are malnourished or at risk of malnutrition (18). The literature has demonstrated that low levels of hydration are common among the elderly and have been associated with morbidity and mortality (19-22). Poor hydration has also been shown to adversely affect mood and cognitive function (23, 24). The frequency of comorbidities in the elderly population has elicited the recommendation of routine screening of older hospitalized patients (>70 years) for six risk factors including dehydration (25). Some have gone as far as suggesting that the frail elderly receive prescriptions for drinking water (26).
Identifying an agreed upon set of parameters to define clinical dehydration has proven to be elusive. The diagnosis of dehydration usually rests on assessment of patient history, physical examination and laboratory tests weighed together – similar to most clinical diagnostics. As numerous manuscripts state, in various forms, no single laboratory value can accurately determine that a patient is dehydrated, however, Riccardi et al (2013) state that Blood Urea Nitrogen:Creatinine (BUN:Cr) ratio is the most reliable parameter (27, 28). While some studies agree that a BUN:Cr ratio of greater than or equal to 25 is a reliable indicator, others point out that patient history and physiological disease processes must be taken into account when assessing dehydration (29). Additionally, BUN, in general is usually higher in older subjects (30, 31).
Studies have found laboratory values indicating low levels of hydration in as many as 48% to 60% of subjects in both hospitalized and community-dwelling older adults (32, 33). Despite this, knowledge by health care staff members of nutritional needs was found to be surprisingly low, especially in the category of fluid requirements (34).
The suggested intake of water for all adults (including water derived from foods and other beverages) is 2.7 Liters per day for women over 18 and 3.7 Liters per day for men (35). A separate stipulation for seniors does not exist, but most LTC residents consume between 1.5 and 2 liters per day (36-39).
In this study, laboratory data were used to evaluate the hydration status of patients who were rehospitalized within 30 days of admission to a LTC facility. It was hypothesized that many of these patients would show low levels of hydration.
Methods
The study design utilized a retrospective chart review exploring the hydration status of Medicare patients who were rehospitalized within 30 days of admission to a LTC facility during a six month period from January 2012 to June 2012. After Institutional Review Board approval, paper LTC charts were reviewed for epidemiologic information including demographics, admission diagnosis, co-morbid conditions, electrolyte levels and reason for transfer to the hospital. Hospital electronic medical record (EMR) data were accessed to determine emergency department (ED) diagnosis and hydration levels from initial laboratory results from blood measurements. Data were collected at LTC admission and at hospital readmission.
Hydration level data included: Serum Sodium (Serum Na), blood urea nitrogen (BUN), Creatinine (Cr), and BUN:Cr ratio. For the purposes of this study, low hydration was defined as a Serum Na>145 mg/dl or a BUN:Cr ratio of >20:1 (33, 40, 41).
To analyze admission diagnoses, the study team created the following general categories: infectious, cardiovascular, pulmonary, neurological, gastrointestinal, electrolyte abnormality (including dehydration), falls, genitourinary and gynecologic, hematological, and other.
Statistical Analysis
Descriptive statistics (mean, standard deviation (SD), median, first quartile (Q1), third quartile (Q3) frequencies and percentages) were used to report levels of laboratory tests. Standard methods for estimating proportions with their respective 95% confidence intervals (CI) were used to calculate the prevalence of low hydration at LTC admission and at hospital readmission.
Results
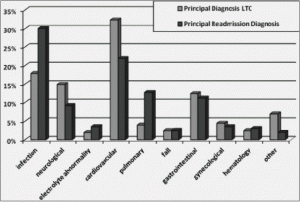
In the 261 subjects studied, average age was 79 years (± 10.4) and 42% were male. The principal diagnoses at time of admission to LTC facility were cardiovascular (34%), infection (20%), neurological (14%), gastrointestinal (13%), gynecological (4%), pulmonary (3%), fall (2%), electrolyte abnormality (including dehydration, 2%), hematology (1%) and other (6%, Figure 1).
The principal diagnoses recorded in the ED at time of hospital readmission were infection (31%), cardiovascular (23%), pulmonary (12%), gastrointestinal (11%), neurological (9%), hematology (3%), gynecological (3%), electrolyte abnormality (including dehydration, 3%), fall (2%), and other (2%, Figure 1).
Among all subjects, at time of LTC admission the prevalence of low hydration was 60.5% (95% CI: 54.3% to 66.5%), at time of rehospitalization, low hydration prevalence was 67.4% (95% CI: 61.4% to 73.1%). Median changes in lab values from LTC admission to rehospitalization are displayed in Table 1.

Table 1 Laboratory Values for Serum Na, BUN, Creatinine and BUN:Cr at Admission to Long Term Care, Readmission to the Hospital and the Difference Between the Two
Serum Na=serum sodium; BUN=blood urea nitrogen; BUN:Cr=blood urea nitrogen:creatinine ratio; LTC=Long Term Care. P-values are based on a Wilcoxon signed-rank test.
Discussion
Almost 70% of the subjects studied met or exceeded at least one study parameter for low hydration across the continuum of care from hospitalization to readmission. Yet, clinical dehydration was identified only 2% and 3% of the time as a diagnosis. These percentages are similar to previous studies which have evaluated dehydration and poor nutritional status across this population (32, 33, 42-44). Further, hospitalized patients may be kept without oral food or fluids for procedures, or may be unwilling or unable to tolerate nutrition. Additionally, the hospitalized elderly may not have the capacity or awareness to request the fluids they need, as thirst may be impaired due to acute illness, decreased appetite, inability to ambulate or obtain water on their own and altered mental status. Infections, sepsis and gastrointestinal illness may further contribute to low hydration.
The frequency of low hydration among these subjects indicates a need for careful vigilance of the nutritional status of all older hospitalized and LTC patients. Perhaps LTC facilities need to initiate nutritional consults to better identify and treat those at highest risk and prevent further clinical deterioration. An individualized hydration and nutrition program geared towards the vulnerable elderly might help alleviate this phenomenon. Such a program might also follow subjects to track changes to develop markers which might indicate risk level for readmission due to a lack of improvement in status – as seen in this study.
While it remains unclear if lab results showing low hydration correspond with clinical dehydration and if improving hydration status prevents rehospitalization, this study seeks to show an ancillary result of clinical deterioration that may be reversible and may help the patient’s overall condition. Therefore, patients may benefit if providers can attend to this common issue while still maintaining a high level of care addressing the most salient issues for each individual patient.
This study had several limitations including a small sample size derived from a single LTC facility, and a single hospital. Dehydration in the elderly is difficult to discern given the fact that many older patients have diminished muscle mass, renal disease, congestive heart failure and other medical conditions. Additionally, it is not known if the staff of the LTC facility or the hospital was aware of the hydration status of patients. Finally, due to the retrospective nature of the study it is not known whether an improved hydration status would have prevented readmissions.
In this study, low hydration levels appear to be an unrecognized clinical issue for older adults requiring LTC and rehospitalization. Increasing awareness of this condition might assist in improving the patient’s fluid status prior to discharge from the hospital thereby potentially preventing avoidable readmissions.
Acknowledgements: The authors would like to acknowledge Rinki Sundhani-Newkirk and Jill Cotroneo for administrative support.
Funding: This research did not receive outside funding.
Conflict of Interest: The authors declare that there is no conflict of interest regarding to the publication of this paper.
Ethical standard: This research has been approved by the NSLIJ Health System IRB (#12-351B).
References
1. Jencks SF, Williams MV, Coleman EA. Rehospitalizations among patients in the Medicare fee-for-service program. N Engl J Med 2009;360(14):1418–1428.
2. Dharmarajan K, Hsieh AF, Lin Z, et al. Diagnoses and timing of 30-day readmissions after hospitalization for heart failure, acute myocardial infarction, or pneumonia. JAMA 2013;309(4):355-363.
3. Kociol RD, Lopes RD, Clare R, et al. International variation in and factors associated with hospital readmission after myocardial infarction. JAMA 2012;307(1):66-74. 4. CMS Readmissions Reduction Program. http://www.cms.gov/Medicare/Medicare-Fee-for-Service-Payment/AcuteInpatientPPS/Readmissions-Reduction-Program.html. Accessed 7 March, 2014.
5. Fiegel C. 2,200 hospitals face Medicare pay penalty for readmissions. American Medical News. 2012. http://www.amednews.com/article/20120827/ government/308279952/6/. Accessed 7 March, 2014.
6. Mor V, Intrator O, Feng Z, Grabowski DC. The revolving door of rehospitalization from skilled nursing facilities. Health Aff 2010;29(1):57-64.
7. Ouslander JG, Berenson RA. Reducing unnecessary hospitalizations of nursing home residents. N Engl J Med 2011;365(13):1165-1167.
8. van Walraven C, Bennett C, Jennings A, Austin PC, Forster AJ. Proportion of hospital readmissions deemed avoidable: a systematic review. CMAJ 2011;183(7):E391-E402.
9. El-Sharkawy AM, Sahota O, Maughan RJ, Lobo DN. The pathophysiology of fluid and electrolyte balance in the older adult surgical patient. Clin Nutr 2014;33(1):6-13.
10. Wysocki A, Kane RL, Golberstein E, Dowd B, Lum T, Shippee T. The association between long-term care setting and potentially preventable hospitalizations among older dual eligibles. Health Serv Res. 2014; Mar 13. [epub ahead of print]
11. Kehayias JJ, Ribeiro SML, Skahan A, et al. Water homeostasis, frailty and cognitive function in the nursing home. J Nutr Health Aging 2012;16(1):35-39.
12. Presse N, Ferland G. Risk factors contributing to insufficient water intake in elderly living in nursing homes and long-term care units: a review of the literature. Can J Diet Pract Res 2010;71(4):e94-e99.
13. Guidelines Summary – Agency for Healthcare Research and Quality. Dehydration and fluid maintenance in the long-term care setting. Published by the US Department of Health and Human Services. http://www.guideline.gov/content.aspx?id=15590. Accessed 7 March, 2014.
14. Lindner G, Exadaktylos AK. Disorders of serum sodium in emergency patients: Salt in the soup of emergency medicine. Anaesthesist 2013;62(4):296-303.
15. Lindner G, Funk GC, Lassnigg A, et al. Intensive care-acquired hypernatremia after major cardiothoracic surgery is associated with increased mortality. Intensive Care Med 2010;36(10):1718-1723.
16. Maughan RJ. Hydration, morbidity, and mortality in vulnerable populations. Nutr Rev 2012;70(s2):S152–S155.
17. PubMed.Gov. Accessed 21 May, 2013.
18. Holyday M, Daniells S, Bare M, Caplan GA, Petocz P, Bolin T. Malnutrition screening and early nutrition intervention in hospitalised patients in acute aged care: A randomised controlled trial. J Nutr Health Aging 2012;16(6):562-568.
19. Allison SP, Lobo DN. Fluid and electrolytes in the elderly. Curr Opin Clin Nutr Metab Care 2004;7(1):27-33.
20. Molaschi M, Ponzetto M, Massaia M, Villa L, Scarafiotti C, Ferrario E. Hypernatremic dehydration in the elderly on admission to hospital. J Nutr Health Aging 1997;1(3):156-160.
21. Begum MN, Johnson CS. A review of the literature on dehydration in the institutionalized elderly. E J ClinNutrMetab 2010;5(1):e47–e53.
22. Feinsod FM, Levenson SA, Rapp K, Rapp MP, Beechinor E, Liebmann L. Dehydration in frail, older residents in long-term care facilities. J Am Med Dir Assoc 2004;5(2 Suppl):S35-S41.
23. Lieberman HR. Methods for assessing the effects of dehydration on cognitive function. Nutr Rev 2012;70(2):S143-S146.
24. Ferry, M. Strategies for ensuring good hydration in the elderly. Nutr Rev 2005;63(6):S22–S29.
25. Inouye SK, Bogardus ST Jr, Baker DI, Leo-Summers L, Cooney LM Jr. The Hospital Elder Life Program: a model of care to prevent cognitive and functional decline in older hospitalized patients. Hospital Elder Life Program. J Am Geriatr Soc 2000;48(12):1697-1706.
26. Faes MC, Spigt MG, Olde Rikkert MGM. Dehydration in geriatrics. Geriatr Aging 2007;10(9):590-596.
27. Riccardi A, Chiarbonello B, Minuto P, Guiddo G, Corti L, Lerza R. Identification of the hydration state in emergency patients: correlation between caval index and BUN/creatinine ratio. Eur Rev Med Pharmacol Sci 2013;17(13):1800-1803.
28. Dehydration and Fluid Maintenance. AMDA CPGNews.Org Guidelines. http://www.cpgnews.org/DF/index.cfm. Accessed 7 March 2014.
29. Thomas DR, Cote TR, Lawhorne L, et al. Understanding clinical dehydration and its treatment. J Am Med Dir Assoc 2008;9(5):292-301.
30. Aono T, Matsubayashi K, Kawamoto A, Kimura S, Doi Y Ozawa T. Normal ranges of blood urea nitrogen and serum creatinine levels in the community-dwelling elderly subjects aged 70 years or over–correlation between age and renal function. Nihon Ronen Igakkai Zasshi 1994;31(3):232-236.
31. Warren JL, Bacon WE, Harris T, McBean AM, Foley DJ, Phillips C. The burden and outcomes associated with dehydration among US elderly, 1991. Am J Public Health 1994;84(8):1265-1269.
32. Bennett JA, Thomas V, Riegel B. Unrecognized chronic dehydration in older adults: examining prevalence rate and risk factors. J Gerontol Nurs 2004;30(11):22-28.
33. Stookey JD, Pieper CF, Cohen HJ. Is the prevalence of dehydration among community-dwelling older adults really low? Informing current debate over the fluid recommendation for adults aged 70+years. Public Health Nutr 2005;8(8):1275-1285.
34. Beattie E, O’Reilly M, Strange E, Franklin S, Isenring E. How much do residential aged care staff members know about the nutritional needs of residents? Int J Older People Nurs 2014;9(1):54-64.
35. Panel on Dietary Reference Intakes for Electrolytes and Water. Dietary Reference Intakes for Water, Potassium, Sodium, Chloride, and Sulfate. Washington DC: National Academy Press; 2005 http://www.nal.usda.gov/fnic/DRI/DRI_Water /water_full_report.pdf. Accessed 13 March 2014.
36. Wu SJ, Wang HH, Yeh SH Yang YM. Hydration status of nursing home residents in Taiwan: a cross-sectional study. J Adv Nurs 2011;67(3) 583-590.
37. Culp K, Mentes J, Wakefield B. Hydration and acute confusion in long-term care residents. West J Nurs Res 2003;25(3):251-266; discussion 267-273.
38. Mentes J. Oral hydration in older adults: greater awareness is needed in preventing, recognizing, and treating dehydration. Am J Nurs. 2006;106(6):40-49.
39. Akner G, Flöistrup H. Individual assessment of intake of energy, nutrients and water in 54 elderly multidiseased nursing-home residents. J Nutr Health Aging 2003;7:2-12.
40. Androgue HJ, Madias NE. Hypernatremia. N Engl J Med 2000;342:1493-1499.
41. Thomas DR, Tariq SH, Makhdomm S, Haddad R, Moinuddin A. Physician misdiagnosis of dehydration in older adults. J Am Med Dir Assoc 2004;4(5):251-254.
42. Charlton K, Nichols C, Bowden S, et al. Poor nutritional status of older subacute patients predicts clinical outcomes and mortality at 18 months of follow-up. Eur J Clin Nutr 2012;66(11):1224-1228.
43. Baldelli MV, Boiardi R, Ferrari P, Basile E, Campari C. Evaluation of the nutritional status during stay in the subacute care nursing home. Arch Gerontol Geriatr Suppl 2004;(9):39-43.
44. Shyu YI, Liang J, Tseng MY, et al. Comprehensive and subacute care interventions improve health-related quality of life for older patients after surgery for hip fracture: A randomised controlled trial. Int J Nurs Stud 2013;50(8):1013-1024.