P. Saidlitz1, T. Voisin1,2
1. Alzheimer’s disease center, Gerontopole, Purpan University Hospital, Toulouse, France; 2. Inserm, UMR1027, Epidemiology and public health analyzes: Risks, chronic diseases and disabilities, Faculty of Medicine, Toulouse, F-31062, France. Corresponding author: Saidlitz Pascal, Alzheimer’s disease center, 170 avenue de Casselardit, TSA 40031, Purpan University Hospital, 31059 Toulouse Cedex 09, saidlitz.p@chu-toulouse.fr
Estimated number of patients with dementia is 24 million worldwide, a majority with Alzheimer disease (1). Near half of prevalent cases of Alzheimer disease need a high level of care, equivalent to that of a nursing home (2), and one fifth of all nursing home residents receive antipsychotics (3). This rate varies according to the psychiatric consultant, ranging from 12.2% to 26.4% (3). Although the response rate is variable according to studies, a small but significant effect was found in a recent meta-analysis (4). In view of recommendations of American (Food and Drug Administration, FDA) and European (European Medicines Agency, EMA) agencies on the decline in use of antipsychotics for supported behavioural symptoms in dementia, we propose an analysis of interest and risks of antipsychotic for treatment of agitation, and propose alternatives to these treatments in nursing home on the basis of recent publications.
Antipsychotics are they safe?
Antipsychotics are frequently used for treatment of behavioral disorders in dementia including agitation, but also obsessive compulsive disorders or aggression. Adverse effects in elderly subjects most frequently found are the extrapyramidal symptoms, stroke, urinary symptoms and increased risk of death (4). However, results regarding the increased risk of death with antipsychotics vary according to the analysis. The first reason is that presence of behavioural symptoms (including psychosis and agitation) in patients with dementia increases the risk of adverse events, including rate of institutionalization and death (5, 6). Several studies in demented subjects were able to show an increased risk of death associated with the prescription of antipsychotics for the treatment of behavioural symptoms (4, 7, 8). The increase risk of mortality, regardless of the cause, does not seem the same as molecules used, and it seems that conventional antipsychotics (like Haloperidone) are associated with a higher risk than atypical (9), particularly those of the last generation as Quetiapine. This molecule seems to be the only one having no dose-response relation. In the same time, increased risk of stroke has been clearly established, particularly with Risperidone (7). Yet there are some confounding factors, among others severity of dementia and polypharmacy. This probably explains in part the conflicting results found elsewhere in the literature, for example in a prospective study of 2 years that found significant association of mortality with high number of medications and physical restraint while the requirements of antipsychotics (atypical or conventional) were not found (10).
It seems that use of antipsychotics in behaviorals symptoms in dementia need careful assessment and regular reassessment. Even if the risk of serious adverse events (death, institutionalization or hospital events) is difficult to identify and that several studies contradict this association (6, 9, 11), frequent side effects are found in elderly patients (urinary tract, extrapyramidal symptoms, somnolence) (7).
Antipsychotics are they effective?
The effectiveness of antipsychotics in agitation is also discussed in literature. It seems that antipsychotics, whether conventional and atypical, are associated with improvement of certain behavioral symptoms in dementia. The most significant results were found with atypical antipsychotics (Risperidone and Aripiprazole) on global scales, although they are small (6) in a wide meta-analysis. Despite the lack of positive results found with Quetiapine and Olanzapine, many limitations (size of staff, response rate) may bias the results. Some difference in efficacy were found depending on the molecules among the atypical antipsychotic: Risperidone appears statistically more effective for obsessive compulsive disorders (4), antipsychotics analyzed (Aripiprazole, Risperidone and Olanzapine) were able to show efficacy on symptoms overall behavior and agitation in dementia. As the search for the association of antipsychotics and risk of death, many confounding factors may explain the conflicting results in the literature, as the association of psychiatric disorders or severity of dementia (7).
Antipsychotics in nursing home to treat agitation: How to use? What alternatives?
Antipsychotics are therefore sometimes necessary for the management of behavioral disorders in dementia, among other agitation. Yet we have shown that they require many precautions, with regular reassessment of their indication and long-term tolerance. Indeed data from the literature seem to favor an increased risk of adverse events (institutionalization rate, risk of death, hospital events), in addition to recognized adverse effects (stroke, extra-pyramidal symptoms, somnolence, urinary tract affection). Moreover, their effectiveness appears to be present but modest, with a limited evidence of longer term benefits (12). Choice of antipsychotic should take into account differences between molecules, and should favor an atypical whose effectiveness seems better. The lack of proven efficacy of low doses of conventional antipsychotics (like Haloperidone) vs placebo grows to favour the use of atypical antipsychotics because of the risk of poor motor tolerance to high doses (2-3mg/jour) of Haloperidol (13).
Other therapeutic strategies exist for the treatment of behavioral disorders in dementia, in particular for agitation. Citalopram, a serotoninergic antidepressant, has showed an efficacy vs placebo on agitation in dementia due to Alzheimer on global scales (NPI, Cohen mansfield, NBRS) in an interventional study of 9 weeks (14). The increase in cognitive impairment and the risk of cardiac arrhythmia (QT interval prolongation) require regular monitoring, among other ECG at 3rd week according to the authors. An alternative strategy to antipsychotics can be the use of antiepileptic drugs for behavioral interventions. A study with Carbamazepine (300 mg/day) over 6 weeks vs placebo in patients with dementia living in nursing home showed effectiveness on agitation and aggression on the BPRS scale, without significant aggravation of cognitive impairment (15). On the other side, several studies with Valproate for agitation in dementia due to Alzheimer did not find any superiority vs placebo. For exemple, the placebo-control trial of Herrmann & al. (16) in demented Alzheimer subjects living in long term care has not proved any superiority on agitation NPI subscale and Cohen-Mansfield Inventory. According to current data of literature, antiepileptic choice seems to be carbamazepine.
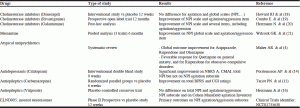
Agitation in dementia, including Alzheimer’s disease, is a common behavioral symptom in nursing home. Antipsychotics remain the most frequently prescribed treatments, despite the many warnings from FDA and EMA on the over-use. Antipsychotics seem to have a small but significant efficacy on behavioral disorders, even if the results are not comparable under the molecules. Choice must be reasoned and reassessed regularly, especially because of adverse long-term effects (increased risk of stroke, institutionalization, extra-pyramidal symptoms). The increased risk of death is uncertain, mainly because of confounders (psychiatric disorders, severity of dementia, other treatment). If the practitioner prescribes antipsychotics, preference should go to an atypical, and take into account the differences between molecules. Regular reassessment of this treatment should help find different strategies, with classes of psychotropic better tolerated in a long term use, such as serotonergic antidepressants (Citalopram) and antiepileptic drugs (Carbamazepine), after individual reflection. Table 1 summarises characteristics of principal drugs used in agitation in demented patients with Alzheimer disease.
Place of drugs in the treatment of agitation remains a use of 2nd line, according to the recommendations of all drugs agencies, after the establishment of non pharmacological interventions. Authors agree that it remains difficult to prove effectiveness of non-drug interventions for behavioral symptoms in dementia, because double-blind studies are illusory. Yet those interventions delivered by family caregivers showed in a meta-analysis their efficacy on behavioural symptoms (severity and frequency), as well as to reduce caregiver’s adverse reactions. Although this study was not conducted in nursing home, it brings two size data for non pharmacological strategies: as effective as drug strategies, and especially no adverse effects (17).
Conclusion
Because safety and efficacy of antipsychotics are unclear and uncertain for long term use, it is necessary for physicians in nursing home to emphasize non-pharmacological measures first, and use psychotropic medications with caution to treat behavioral disorders like agitation. In addition to caregiver’s and family member’s education about the potential risks and
benefits of certain drugs, physicians should carefully document their treatment to minimize the risk of adverse effects. In all cases it is also necessary to take into account major’s comorbidities, in particular cardiac and cerebro-vascular disease, to choose the least harmful treatment.
References
1. Ballard C, Corbett A, Jones EL. Dementia: challenges and promising developments. Lancet Neurol. 2011 Jan;10(1):7-9. doi: 10.1016/S1474-4422(10)70304-5.
2. Brookmeyer R1, Johnson E, Ziegler-Graham K, Arrighi HM. Forecasting the global burden of Alzheimer’s disease. Alzheimers Dement. 2007 Jul;3(3):186-91.
3. Tjia J, Field T, Lemay C, Mazor K, Pandolfi M, Spenard A, Ho SY, Kanaan A, Donovan J, Gurwitz JH, Briesacher B. Antipsychotic use in nursing homes varies by psychiatric consultant. Med Care. 2014 Mar;52(3):267-71.
4. Maher AR, Maglione M, Bagley S, Suttorp M, Hu JH, Ewing B, Wang Z, Timmer M, Sultzer D, Shekelle PG. Efficacy and comparative effectiveness of atypical antipsychotic medications for off-label uses in adults: a systematic review and meta-analysis. JAMA. 2011 Sep 28;306(12):1359-69.
5. Scarmeas N, Brandt J, Blacker D, Albert M, Hadjigeorgiou G, Dubois B, Devanand D, Honig L, Stern Y. Disruptive behavior as a predictor in Alzheimer disease. Arch Neurol. 2007 Dec;64(12):1755-61.
6. Lopez OL, Becker JT, Chang YF, Sweet RA, Aizenstein H, Snitz B, Saxton J, McDade E, Kamboh MI, DeKosky ST, Reynolds CF 3rd, Klunk WE. The long-term effects of conventional and atypical antipsychotics in patients with probable Alzheimer’s disease. Am J Psychiatry. 2013 Sep 1;170(9):1051-8. doi: 10.1176/appi.ajp.2013.12081046.
7. Lon S. Schneider, M.D., M.S., Karen Dagerman, M.S., Philip S. Insel, M.S. Efficacy and Adverse Effects of Atypical Antipsychotics for Dementia: Meta-analysis of Randomized, Placebo-Controlled Trials. Am J Geriatr Psychiatry 14:3, March 2006
8. Schneider LS, Dagerman KS, Insel P. Risk of death with atypical antipsychotic drug treatment for dementia: meta-analysis of randomized placebo-controlled trials. JAMA. 2005 Oct 19;294(15):1934-43.
9. Huybrechts KF, Gerhard T, Crystal S, Olfson M, Avorn J, Levin R, Lucas JA, Schneeweiss S. Differential risk of death in older residents in nursing homes prescribed specific antipsychotic drugs: population based cohort study. BMJ. 2012 Feb 23;344:e977.
10. Raivio MM, Laurila JV, Strandberg TE, Tilvis RS, Pitkälä KH. Neither atypical nor conventional antipsychotics increase mortality or hospital admissions among elderly patients with dementia: a two-year prospective study. Am J Geriatr Psychiatry. 2007 May;15(5):416-24.
11. Simoni-Wastila L, Ryder PT, Qian J, Zuckerman IH, Shaffer T, Zhao L. Association of antipsychotic use with hospital events and mortality among medicare beneficiaries residing in long-term care facilities. Am J Geriatr Psychiatry. 2009 May;17(5):417-27.
12. Ballard C, Howard R. Neuroleptic drugs in dementia: benefits and harm. Nat Rev Neurosci. 2006 Jun;7(6):492-500.
13. Devanand DP, Marder K, Michaels KS, Sackeim HA, Bell K, Sullivan MA, Cooper TB, Pelton GH, Mayeux R. A randomized, placebo-controlled dose-comparison trial of haloperidol for psychosis and disruptive behaviors in Alzheimer’s disease. Am J Psychiatry. 1998 Nov;155(11):1512-20.
14. Porsteinsson AP, Drye LT, Pollock BG, Devanand DP, Frangakis C, Ismail Z, Marano C, Meinert CL, Mintzer JE, Munro CA, Pelton G, Rabins PV,Rosenberg PB, Schneider LS, Shade DM, Weintraub D, Yesavage J, Lyketsos CG; CitAD Research Group. Effect of citalopram on agitation in Alzheimer disease: the CitAD randomized clinical trial. JAMA. 2014 Feb 19;311(7):682-91.
15. Tariot PN, Erb R, Podgorski CA, Cox C, Patel S, Jakimovich L, Irvine C. Efficacy and tolerability of carbamazepine for agitation and aggression in dementia. Am J Psychiatry. 1998 Jan;155(1):54-61.
16. Herrmann N, Lanctot KL, Rothenberg LS, Eryavec G. A placebo-controlled trial of valproate for agitation and aggression in Alzheimer’s disease. Dement Geriatr Cogn. 2007;23:116–119.
17. Brodaty H, Arasaratnam C. Meta-analysis of nonpharmacological interventions for neuropsychiatric symptoms of dementia. Am J Psychiatry. 2012 Sep;169(9):946-53.
18. Howard RJ, Juszczak E, Ballard CG, Bentham P, Brown RG, Bullock R, Burns AS, Holmes C, Jacoby R, Johnson T, Knapp M, Lindesay J, O’Brien JT, Wilcock G, Katona C, Jones RW, DeCesare J, Rodger M; CALM-AD Trial Group. Donepezil for the treatment of agitation in Alzheimer’s disease. N Engl J Med. 2007 Oct 4;357(14):1382-92.
19. Cumbo E, Ligori LD. Differential effects of current specific treatments on behavioral and psychological symptoms in patients with Alzheimer’s disease: a 12-month, randomized, open-label trial. J Alzheimers Dis. 2014;39(3):477-85.
20. Herrmann N, Rabheru K, Wang J, Binder C. Galantamine treatment of problematic behavior in Alzheimer disease: post-hoc analysis of pooled data from three large trials. Am J Geriatr Psychiatry. 2005 Jun;13(6):527-34.
21. Wilcock GK, Ballard CG, Cooper JA, Loft H. Memantine for agitation/aggression and psychosis in moderately severe to severe Alzheimer’s disease: a pooled analysis of 3 studies. J Clin Psychiatry. 2008 Mar;69(3):341-8.