I.T.Y. Lam1, H.H. Keller1,4, L.M. Duizer2, K.D. Stark1, A.M. Duncan3
1. Department of Kinesiology, University of Waterloo, Waterloo, ON, Canada; 2. Department of Food Science, University of Guelph, Guelph, ON, Canada, 3. Department of Human Health and Nutritional Sciences, University of Guelph, Guelph, ON, Canada; 4. Schelgel Research Chair, Schlegel-UW Research Institute for Aging. Corresponding author: H. Keller, Department of Kinesiology, University of Waterloo, 200 University Avenue West Waterloo, ON, Canada, N2L 3G1, Tel 519 888 4567 ext. 31761, Fax +1 519 746 6776, e-mail: hkeller@uwaterloo.ca
Abstract
Background:Purpose: Malnutrition is common in long-term care (LTC) residents, yet limited research exists on micronutrient deficiencies. Objective: This study used qualitative methods to explore the acceptability of a food-first micronutrient fortification strategy for LTC and further develop this strategy. Design & participants: Qualitative cross-sectional data collection based on eleven staff focus groups (n=45), ten expert key informant interviews, and five family/resident focus groups (n=71) were conducted. Data were triangulated during content analysis, completed by two coders. Results: Stakeholders provided insight into benefits, concerns and potential solutions to minimize barriers and promote adherence to the strategy. Suggested solutions included development of outsourced/pre-made fortified products, mandatory training and clear protocols. Stakeholders can envision food fortification as a strategy to improve micronutrient status if products are easy to access and incorporate into current production systems. Yet, residents and families wish to be informed and have the potential to ‘opt out’. Safety and efficacy also needs to be demonstrated before it is incorporated into standard practice. Conclusion: This work provides a strong foundation for developing a proof-of-concept micronutrient food fortification study for the prevention of deficiencies in LTC.
Key words: Malnutrition, micronutrient fortification, nursing home, acceptability testing.
Introduction
Micronutrient (vitamin/mineral) deficiency is a prevalent yet preventable form of malnutrition among older adults living in long-term care (LTC) (1–4). Plate waste estimation suggests that approximately 1600 kilocalories is consumed (5), with even lower consumption by cognitively impaired residents (~1,100 to 1,200 kcal per day) (1). As menus are typically planned to meet 100% of residents’ micronutrient needs, some residents may not meet their requirement due to low food intake (1). Little intervention research has been conducted on the prevention of micronutrient malnutrition in LTC (6).
Micronutrient deficiencies are often treated with strategies such as oral nutrition supplements (ONS) which attempt to ameliorate overall intake (1, 7). However, waiting for signs of sufficiently low intake to stimulate this strategy means that subclinical deficiency is overlooked. Moreover, there are possible compensatory reductions in food intake at subsequent meals after ONS consumption, making the supplement a ‘replacement’ to regular food intake (8,9). Low adherence to ONS further reduces their long-term use (10–12). Micronutrient pills, although potentially preventative, are also used reactively (13). The risk of drug-nutrient interactions when administering vitamin/mineral pills (14), lack of coverage by drug benefit plans (14) and out-of-pocket costs for residents (15, 16) are reasons for limited use in LTC.
Research suggests that families (17, 18) and providers (13, 19) prefer a ‘food-first’ approach to address nutrition problems (1, 4). Enriched/fortified foods have been proposed as such an approach (19, 20). Most fortification practices focus on protein, which can be increased with naturally high foods (e.g. milk, eggs, or cheese) (20) or supplements (19) added to selected foods. While these strategies appear to improve energy and protein intake (21), these enhanced foods typically do not focus on improving micronutrient intake (20).
At present, there is no consensus on best methods for prevention of micronutrient malnutrition in LTC residents (6). In view of residents’ average low food intake (1, 22) and the recommended micronutrient levels to achieve nutritional adequacy (1, 23), micronutrient fortification of key foods is a potential solution (24), yet has been rarely conducted and research to date does not identify best practices. This strategy is especially relevant for residents with insufficient nutrient intake but a stable body weight due to low levels of activity and energy requirement (6, 25).
Assessment of the acceptability and feasibility of a new intervention should be done with end users prior to implementation, especially when the strategy requires changes in care processes (26). Determining the acceptability of micronutrient fortification with stakeholders who are closely aligned with planning, purchasing, preparing and serving food (dietitians, nutrition managers, cooks), will enhance understanding of barriers to implementation of this strategy and help to develop a strategy that is potentially effective. To date, there is minimal documentation on staff’s perspective on food fortification in LTC. Further, few studies have examined residents’ and family members’ views of nutrition provision in LTC (17, 18). Multiple perspectives of knowledge users will enhance our understanding of the acceptability of this strategy and will allow for triangulation of perspectives (27).
The purpose of this study was to determine the acceptability of a fortification strategy in LTC and to further develop the concept of this strategy based on diverse stakeholder input (e.g. instructions and protocols, the most appropriate foods for fortification, etc.). Specifically, knowledge users were asked to reflect on the potential of micronutrient food fortification, and identify their concerns and potential solutions when considering food production, delivery and consumption.
Methods
Three stakeholder groups verified the acceptability of fortification of food in LTC: staff, expert key informants (KI), and LTC residents and families. Convenience samples were used for all stakeholder groups. Webinar focus groups were conducted with frontline nutrition staff, providing insight into both clinical and production issues with micronutrient fortification. The webinar format traversed geographical barriers and allowed participants to join regardless of time zone or location. From the webinars, a number of participants who were knowledgeable on topics of interest (i.e. had conducted fortification) were identified and invited for individual in-depth KI interviews, along with additional KIs who were experts in strategic areas (e.g. government, food industry). Recognizing that webinar and KI informants were generally in favour of a fortification strategy, resident and families’ views were ascertained via in-person focus groups. This study underwent ethical review and clearance by the Office of Research Ethics at the University of Waterloo (Ethics review #: 18558).
Webinar Focus Groups
Focus groups gather individual and interactive opinion and attitudes through a carefully planned framework of questions and discussions (28). The group format allows for interactions among participants and can contribute to further development of ideas and concepts (28). On-line webinar technology offers the opportunity for on-screen presentations, group discussion, and immediate polling questions to engage all participants. Webinar focus groups allow for the real-time, immediate response of traditional focus groups, similar to teleconference systems, without the physical presence and the need to travel (28), and have been previously used for training of staff (29) and students (30,31) and were thus considered a viable option for conduct of these focus groups. Lower numbers of participants are recommended for online synchronous (real-time sharing) focus groups (29). Thus, several small groups (3-7 participants) were scheduled and conducted. The target participants were dietitians, nutrition managers and chefs working in LTC. Convenience and snowball sampling were used to identify the sample. Participants were initially recruited through the Dietitians of Canada Gerontology Network and the Canadian Society of Nutrition Management (CSNM), with a global email message or newsletter sent to all members of these organizations. Interested participants contacted the investigators via email and were sent an invitation e-mail containing: a detailed information letter outlining the purpose of the study and process, instructions to register, and a link to a pre-session online registration survey to collect pertinent demographics. Participants of the initial webinars were asked to suggest potential further participants, and especially other eligible staff in their home.
An advisory committee consisting of experts from the Universities of Waterloo and Guelph helped develop and review focus group discussion and polling questions. Open-ended questions with additional probes were used as a guideline to solicit information and discussion (30). Polling questions examined nutrients of concern for residents, current strategies used to address micronutrient needs, and participants’ ratings on the appropriateness, feasibility and potential effectiveness of a micronutrient fortification strategy.
One-hour focus groups were conducted with webinar technology (WebEx™, Santa Clara, CA); initial sessions were conducted by the first two authors. Sessions were recorded to allow for transcription of the discussion. A telephone connection was used for audio in addition to the webinar technology for presentation of slides and polling questions. After the webinar, participants were emailed a link to a feedback form, which allowed them to provide further comments on the topic as well as to rate their experience with the webinar format and technology.
Key Informant Interviews
KI interviews provided more in-depth information addressing questions with respect to the feasibility of the developing strategy that arose from the webinar focus groups. The advisory committee provided recommendations on various stakeholder groups whose insight and opinion on the potential strategy was desirable; for example, it was anticipated that a government representative familiar with menu planning and food production in LTC would provide unique insights. Individuals within key sectors were identified through the investigator network. Other participants were identified from the staff webinars; these individuals had experience with attempting fortification or additional unique perspectives identified during webinars. Ten KIs were recruited by the primary author via email and those interested in participating were sent an information letter outlining the expectations for an interview and the study process. Individual KI interviews were conducted by the second author and the primary author took notes. A question outline was used to guide the interview. Sessions were conducted by telephone and digitally recorded for subsequent transcription. Verbal consent was obtained at the start of each session; interviews lasted approximately 45 minutes to 1 hour.
In-person Resident/Family Focus Groups
In-person focus groups were conducted at five LTC homes to obtain the opinions of family members and residents. In-person focus groups were chosen due to the vulnerability of this participant group. Due to geographic constraints, only sites within an hour of the University of Waterloo were recruited; sites included for profit, corporate and non-profit homes. Investigators used their contacts and research network to identify homes that might be interested in participating. The dietitian, nutrition manager or other management who were part of the investigators networks were initially contacted by phone or email to determine their interest. All but one home contacted, participated in focus groups. Recruitment posters/letters were provided to the site contact to notify potential participants of upcoming sessions. Group discussions were scheduled at the routine resident/family council/food committee meetings and a 20-30 minute time slot was allotted to the discussion. As a result, staff members were also present, although their opinions were not elicited; they acted as supports to the researchers for completing consent forms and helping with hearing impaired individuals.
Participants signed consent forms prior to the session and completed an anonymous feedback questionnaire on benefits and concerns about the strategy at the end of the session. This provided the opportunity to capture afterthoughts, as not all participants spoke during the discussion. These sessions were not audio recorded to keep the discussion informal and allay any concerns about confidentiality of the information, as well as challenges with soft-spoken participants on the digital recording. Extensive notes were taken by one of the two researchers present.
Data Analysis and Interpretation
Debriefing occurred after each focus group and KI interview between the first and second author to discuss overall impressions, key points, main areas of agreement or disagreement, and new data that resulted from each session (31). All webinar focus groups and KI interviews were transcribed verbatim prior to analysis, with identifiable information removed. Inductive content analysis was used to identify common points or concepts, patterns, and variations (32). This was the chosen analysis method, as this study aimed to explore the broad scope of the issue of fortification as a strategy. The first author and a student researcher each reviewed and coded half of the transcripts to complete an initial overview of the data using open coding (33). A code book was subsequently developed by the first two authors and the student researcher to assist with organization and categorization of the data (31,34). All transcripts were recoded after the development of the code book using selective coding. Exemplary quotes were identified. Memos were written throughout the analysis process to adjust and finalize the analysis.
Data from pre-session registration surveys, online polling questions, and post-session questionnaires were summarized and interpreted with descriptive quantitative analysis, and where appropriate, supplemented with qualitative data. Other results not amenable to being counted were descriptively summarized with minimal interpretation (e.g. long-answer questions from feedback questionnaires) (28, 31) and are presented as key concepts that address the purpose of the study; specifically i) concerns with micronutrient intake, ii) reflections on current strategies, iii) appropriateness of fortification, iv) promoting feasibility, v) determining effectiveness, and vi) overall acceptability of the strategy. Data from the three groups of diverse stakeholders is integrated under each key concept demonstrating triangulation and thus validity and credibility of results (31, 34).
Results
Eleven webinar focus groups were conducted between March and April 2013, 10 KI interviews from July to August 2013, and five in-person resident/family focus groups between July 2013 and January 2014 (Table 1). All webinar and all but one key informant participants were female (Table 1), as there is a gender inequality in the LTC sector and nutrition-related professions (35). The majority of KI and webinar participants were dietitians. There was an even mix of gender and roles (i.e. family members, residents) for in-person family/resident focus groups. Shared key concepts across these stakeholder groups are described below. Longer exemplar quotes are seen in Table 2.
? Note: All webinar respondents were female; 3 dietitians-only groups, 8 mixed staff groups
Concern about the intake of micronutrients in LTC residents
Polling results during webinars indicated that there was concern about nutrient intake in LTC residents, and specifically vitamin D, calcium, vitamin B12, and zinc (Figure 1). Webinar and KI participants associated certain micronutrients to specific food groups (e.g. vitamin D and calcium with dairy, thiamin with grains, magnesium with vegetables); low overall intake of these food groups was the primary reason for concern. Dietitians noted micronutrients that were commonly prescribed for residents, in particular, vitamins B12 and D.
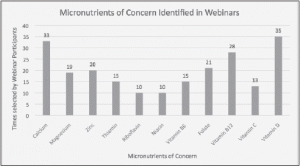
Figure 1 Frequency of micronutrients identified in webinars as being of potential concern in LTC residents (n=45)
In addition to low intake, staff recognized inadequate provision by menus for certain micronutrients; Vitamin D was “a gap” (Registered Dietitian [RD] 20) and “menus [were] not adequate” (RD22). A dietitian from a home that performed nutrient analysis found that the Dietary Refernce Intake (DRI) for potassium was particularly difficult to meet, “due to the amount of food” and “the way [residents] eat” (RD33). Recent publicized research findings on vitamins B12 (RD17) and D (RD16) were also reasons for the awareness of potential problems with these nutrients. Physiological changes with age, low intake, and low biochemical values were among the other reasons noted by participants for why micronutrient fortification might be appropriate for LTC residents
Conversely, certain micronutrients were identified to be potentially problematic for a home-wide fortification strategy due to contraindications for health conditions or fear of toxicity. This included potassium and phosphorus for renal conditions (Nutrition Manager [NM]5), long-term zinc supplementation affecting absorption of other nutrients (RD20), and potential toxic accumulation of fat-soluble vitamins (RD6). Of particular interest was calcium, where staff hesitated to supplement due to recent changes to remove calcium supplements from residents’ medication lists (FC3) as a result of potential increased cardiovascular risk. Accordingly, staff was wary of supplementing calcium outside of food sources and preferred to treat calcium on an “individual basis, depending on dietary intake” (RD20).
Reflections on current strategies
Current practices were mentioned as a barrier to provision of adequate micronutrients from food for older adults. For instance, menu planning currently focuses on macronutrients, with the assumption that micronutrients would be met in the process. Moreover, certain homes may not be equipped to do micronutrient analysis of menus and homes with pre-analyzed menus “don’t know how accurate it is” (RD17). Miscommunication between guidelines and practice may also be a barrier. For instance, LTC homes may plan menus to the Food Guide, focusing on quantity of food to meet food guide servings, when the original intent of this guidance from the government was to provide a variety of food. This demonstrates a need for good knowledge translation when implementing strategies into practice.
Pills were the most common strategy described to address potential micronutrient deficiencies, yet this was unsatisfactory to many participants. Provision of nutrients in pill-form “appears medicinal in nature” (RD28) rather than food. Additionally, the shift to “reduce polypharmacy” (RD26, NM36) in LTC meant physicians were “quite reluctant to supplement with a multivitamin” (RD15). Potential costs incurred to residents for pills not covered by drug benefit programs and the difficulty in finding a single supplement providing complete micronutrients for older adults were also mentioned. Staff noted that use of oral nutritional supplements (ONS) could reduce food intake at subsequent meals and may not provide other nutrients that food does. The process of ONS administration was also noted as redundant and reactive.
Interestingly, some participants preferred provision of ONS as a combined “top up” (RD22) approach that provided calories, protein, and fluids plus micronutrients. Some family members preferred administration of vitamins in pill form for its accuracy and simplicity for tracking. Overall, LTC homes have strategies to address nutrient needs and low food intake, yet these may not be micronutrient-specific, and are more medical than food focused.
* {Braces} provide additional context for quotes
Appropriateness of a fortification strategy
When considering if fortification of common foods was appropriate in the current LTC system, cost was “one of the biggest barriers…” (KI1). The given food budget and cost of food meant that any new strategy had to be cost-effective for acceptance within the industry. As well, it was noted that precision was needed for micronutrient dosage. Participants were concerned with staff’s ability to be precise and accurate when adding fortificant to selected foods in-house; they noted current compliance issues with the addition of supplemental protein and thickeners by staff, due to misinterpreted instructions and lack of time.
Further concerns for appropriateness of the strategy included the classification of fortified products as food or as medications, which had implications on the personnel providing the product. Since most dietary staff and health care aides providing assistance at meals have minimal training, the potential for errors with in-house fortification of food products was a noted limitation. Hence, some participants identified that an outsourced product would be the best approach to promote consistency and safety. Family members were also concerned with the risk of toxicity for residents with good appetites who may consume extra portions.
Taste of fortified products was a top priority. Family and residents noted taste changes with age and were concerned fortification could change tastes of favourite foods, further limiting intake for persons who already had limited intake. Family/resident councils thought fortification was a good strategy but if implementation meant that other activities (e.g. staff providing eating assistance) would be jeopardized, than they stated that, “fortifying foods would go on the back burner” (FRC5). Other family members noted that fortification would not be enough to meet the needs of some highly vulnerable residents who consume very low volumes of food. The desire for choice was voiced by residents and family who wanted the decision to voluntarily opt out of consuming fortified foods.
Overall, staff webinar participants appeared to find the strategy acceptable. Over half provided a high rating (4 or 5/5) on the appropriateness of in-house (57.5%) or out sourced (61%) fortified food products to improve micronutrient intake.
Promoting feasibility of a fortification strategy
Several webinar participants had trialed fortification in LTC. These food-first approaches included the addition of flax (RD26), skim milk (RD30), chickpea flour (KI2), chocolate milk (RD15), or Carnation Instant Breakfast® (RD15). However, such strategies focused on dietary fibre, protein and energy, and although enhancement of other foods with these ingredients may overlap to provide micronutrients (e.g. vitamin D and calcium with milk), the majority of these were not micronutrient-focused efforts. One KI reported on a long-term micronutrient food fortification program (calcium in a whipped topping) in several homes in Nova Scotia, where the purpose of the fortification strategy was “to get away from the medication cart …[and to] put it in our food” (KI3, dietitian). This strategy required buy-in and collaboration with stakeholders at multiple levels: experts (endocrinologists, geriatricians, physicians, pharmacists), home administrators, knowledge users (dietitian, cook, baker, dietary manager) and end-users (family/residents). Taste-testing began at a staff level, then to family councils, and approval at the Ministry of Health level, with funding obtained for the strategy. This example provided evidence that a food-first approach to micronutrient fortification for the general LTC population was not only appropriate, but also feasible. It also provided a process for exploring this concept with other participants.
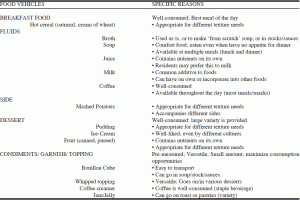
Identifying food carriers (vehicles) for fortification based on common foods most residents enjoy and can consume was required to make the strategy feasible. Participants offered various recommendations for food vehicles (Table 3). Breakfast was the “best meal of the day,” and several staff suggested food vehicles in this category. Fluids, including broth, coffee, juice, and milk were recommended. Soup was frequently mentioned as “a comfort food [that] …is consumed… [even by] people with no appetite” (RD15). Dessert was the most common suggestion among participants. Icecream was suggested as “number one on [residents’ preference] list,” and is preferred across various cultural groups and diets (KI4). Condiments and toppings were also suggested for their small, pre-measured packages and versatility for use with different foods. Participants suggested the aforementioned foods vehicles over entrees (e.g. meats or vegetables) for ease of incorporation (KI4). Overall, staff preferred foods addressing different texture needs (e.g. puddings, oatmeal, mashed potatoes). “Variation” (KI5) of food vehicles or a “multipurpose item” (KI2) are also needed” “to prevent resident boredom” (KI3) and “maximize the opportunity to consume” [foods] (KI7).
Other suggestions to consider for in-house fortification included provision of clear protocols and incorporating fortification into part of the recipe. A systematic framework of the food fortification process, from assessment to monitoring, along with clear direction and assignment of roles would be needed. Involvement of staff and stakeholders at multiple levels to increase resident and family’s awareness of the need for micronutrients and to help them make informed decisions was noted across participant groups as a means to increase adherence.
Determining the potential effectiveness of a fortification strategy
Staff webinar participants rated the overall potential effectiveness of the micronutrient fortification strategy in meeting residents’ needs on a 5-point Likert scale (5=very much). Participants agreed that the concept of the strategy could be effective (rating of 4 (43.5% n=17/39) or were neutral about the strategy (rating of 3 (28%; n=11/39)). However, participants expressed difficulty in determining the effectiveness of the strategy without full knowledge of the content and format of the final product and research to support its use.
Cost was a barrier that could affect the appropriateness of the strategy for LTC and participants suggested that it was necessary to show that benefits outweighed the cost. Family members also requested evidence of effectiveness of the strategy through research, and testing of residents’ serum micronutrient levels to demonstrate need and improvements with this strategy. Likewise, they mentioned that funding could be “prohibitive [for the strategy] due to budget constraints” (FRC2).
Residents valued that the strategy may “improve [residents’] quality of life” (RC3), yet additional factors, including ethical issues with palliative residents, still needed to be addressed before effectiveness could be fully determined.
Overall acceptance of a fortification strategy
Participants generally supported the concept of micronutrient food fortification as a potentially effective, food-first strategy to address micronutrient deficiencies, stating that “trying to use real foods [is their] preference to a supplement” (NM36). Feedback questionnaires from 24 residents and family members rated the overall acceptability of the strategy on a 5-point Likert scale (5 = very much); 75% rated the strategy as 4 (n=10) or 5(n=8). Family members verbally noted that they welcomed any strategies that enhanced the nutrient profile of LTC meals and that fortification was a good alternative. Staff stated that “to add [micronutrients] to foods that residents enjoy eating” (RD26) would be a better accepted than current strategies. The strongest benefit of micronutrient food fortification was its long-term, cumulative effect rather than immediate impact:
I can’t predict they’re going to get 100% of it. But I can… predict if I give it consistently daily, it adds to their nutrient intake. So it works! …We’ve had falls, and…a significant reduction in broken bones! So something’s workin’. (KI3, RD with food fortification experience)
Much work needs to be done to solidify this fortification strategy, yet findings from this study confirm that a food-first strategy addressing micronutrient needs is a “move in the right direction” (Chef7).
Discussion
Fortification has been noted as a potential cost-effective, long-term strategy to address micronutrient deficiencies in vulnerable groups with known low intake (36). Ongoing concerns about population-wide food fortification has been documented, ranging from differences in individual absorptive ability and needs (37), to public health issues of appropriateness and availability of fortified foods (38), to changes in food properties due to reactions with more effective but reactive forms of these micronutrients (39). Food fortification using micronutrients specific to LTC residents’ needs is a novel approach, where the objective is to provide a low-level dosage to prevent or delay long-term complications (similar to a multivitamin), rather than provide short-term or immediate reversal of a micronutrient deficiency. This study aimed to determine acceptance of a potential food fortification strategy from the perspectives of various stakeholders, and to gather feedback to inform this strategy. Due to the novelty of this approach, little prior research is available for comparison and participants were required to assess the concept in an abstract stage of its development.
Previous work has examined pre-made (40,41) and home-produced fortified products (15) in LTC. These studies considered some issues such as sensory changes (15), appropriateness of texture (15) and food habits and preferences of residents (42), areas of consideration consistent with this research. Potential food vehicles mentioned by our participants were also similar to those used in previous studies, which included condiments (e.g. butter) (42), beverages (e.g. juice, milk) (43,44), snacks (e.g. cheese) (41), sides (e.g. bun) (40) and entrées (15). Yet the complexity of food fortification identified in this study, especially the process and procedural considerations required, have not been discussed in prior research. Efficacy of selected micronutrient fortification has been demonstrated (15,40–44) and examined using vitamin-only preparations (15) or targeted to specific health conditions (40), but effectiveness of a population-wide fortification strategy using many micronutrients is still required. Given the known low food intake in LTC (4,25), and potential inadequate micronutrient contents of LTC menus (1), this strategy is logical. Compliance with ONS and pill supplementation remains an issue in LTC, leaving room for alternative food-first micronutrient strategies.
The results of this study provide a foundation for development of a food fortification strategy for LTC. Although generally considered acceptable and appropriate, all stakeholders desired information on the efficacy of this strategy and residents/family specifically noted that they would want to be informed of the micronutrients chosen in the fortification formula and have the option to opt out if desired. The LTC setting is unique in that the same food is offered to all residents. Thus, it is essential that the selected food vehicle be well-liked and consumed by all residents for this strategy to work. Findings suggest that a flexible approach to fortification, with variety in food products and ensuring that sensory qualities are maintained are necessary for stakeholders to consider the strategy as appropriate for LTC. Provision of micronutrient-fortified food options at each meal may increase the likelihood of residents accepting the fortified foods. To be appropriate, the fortification strategy would need to be easy to implement with an accurate, foolproof procedure for staff to follow. As a result, outsourced products were preferred as they overcome feasibility issues associated with consistency in preparation and thus safety, yet any product has to be cost-effective as food budgets are limited in LTC. Finally, once the strategy is developed, creation of effective protocols to train staff, along with tracking and monitoring residents’ intake of the food vehicle are needed.
This study used multiple methods to gather input from diverse participants and is the first published report focused on acceptability testing of a food-related intervention for LTC; yet it had some challenges and limitations. Online focus groups in the literature are largely done as chat-forums (45) and lack the immediate feedback component that in-person focus groups provide (46). Webinar focus groups are an innovative technique for research, allowing for real-time conference and voice discussions, while facilitating ease of participation for those in geographically separate locations. One suggestion for future studies using webinar focus groups is to limit group size to 3-5 participants to promote participation in the discussion and reduce crosstalk. Focus groups with similar participant composition (e.g. all dietitians) may also minimize power imbalance and allow participants to speak more openly (28). Voice-only webinars may be beneficial as webinars may be seen as less threatening than face-to-face, providing a sense of detachment/remoteness that allows participant to freely divulge information (29,47). Participants (84%) provided feedback on the webinar technology, process and content through an anonymous feedback questionnaire. Participants’ main concerns were regarding voice delay/overlaps. Suggestions for improvement include: using phones over computers (better clarity), including type-in chatting (to capture all comments), having test/practice sessions, and additional cueing/direction from facilitators.
A further limitation of the staff webinars was the low number of chef/cooks who participated. Although dietitian and nutrition manager participants were encouraged to recruit these staff members, their views on this strategy were under-represented. Thus, it was vital to recruit administrative dietitians for KI interviews, who had closer experience with chefs or were chefs themselves, to provide greater understanding of this perspective. Webinar polling also had some limitations. Sites where more than one participant came to the same session, typically shared a computer and phone line. Thus, polling results were based on their collective answer rather than on individual participants. There is also the potential that the dietitians and nutrition managers were also not representative of these staff groups as they volunteered for the study and were recruited from membership lists of professional organizations that are not mandatory. Yet saturation was evident near the end of data collection, as few new ideas and issues were raised about the strategy in later webinar groups. A limitation specific to these KI interviews was our inability to recruit a representative from the federal government Food Directorate who could speak to their perspective on food fortification.
Focus groups with LTC residents had some challenges, as many residents had functional and cognitive deficits, and at least one staff member was present to help facilitate the consent process and to help residents communicate. The inclusion of staff in the room may have affected participants’ responses as they may have felt less comfortable reporting issues or concerns. The inclusion of an anonymous feedback questionnaire offered an extra venue for residents and family to share their thoughts in a more private manner. Yet, only 24 of 71 (33.8%) participants completed the feedback form at the end of the session, which provided a rating on their acceptability of the strategy. It is not known if those who did not complete this form did not have the capacity to do so, did not think their opinion mattered, or did not like the strategy proposed. Finally, focus groups with family and residents were limited to the geographic area close to the location of investigators. This group is likely not representative of all residents’ and family members’ view points, but few new comments or concerns arose by the point of the fifth session, suggesting saturation of findings.
Given the low food consumption in LTC (1,4), it is likely that most residents could benefit from a low-level dosage of micronutrients to meet dietary recommendations. Future work is needed to make food fortification of micronutrients in LTC a reality. Specifically, sensory testing to ensure that taste, texture, smell and colour of food vehicles are not influenced is required. Identification of nutrients and dose to be included in the fortificant is also needed; rigorous reviews of the current literature on intake of micronutrients and biochemical status would be a first step. Protocols for implementing the strategy are also needed. For example should triggers based on food intake be used to initiate the strategy (e.g. if resident eats <50% of meals consistently, s/he should receive the food vehicle), or should the entire population be targeted? Finally, efficacy testing that demonstrates improved biochemical markers with fortification are needed to make the case that low dose food fortification has a benefit with respect to nutrient status.
Conclusion
This study provides a comprehensive examination of diverse perspectives on the possibility of micronutrient food fortification for LTC and demonstrates the importance of determining stakeholder acceptability before interventions are implemented. Micronutrient food fortification appears to be acceptable if some considerations are addressed, including development of protocols, proper education and informing of staff, residents, and family, and exploring alternative implementation solutions (e.g. outsourcing the product). Trialing the fortification in actual LTC production systems, and a clinical trial to provide evidence of benefits of the fortification strategy is crucial. It is uncertain if this strategy will surpass, equal, or fall short of current strategies, but participants confirm that it is a needed area of future research and could be an acceptable strategy. As stated by a resident when asked about the acceptability of this strategy: “Nothing ventured, nothing gained.”
Acknowledgements: We thank all dietitians, LTC staff, residents, and family members who willingly provided their expertise and recommendations (especially to the Dietitians of Canada – Gerontology Network). We would like to acknowledge Kaylen Pfisterer and Tony T. Li (University of Waterloo) for investing their time into this research. We are also grateful for the input of experts, fellow researchers, mentors, and friends who provided incredible support from the development to write-up stages of this work. This research is funded by OMAFRA-University of Guelph partnership program and the RIA (Research Institute of Aging). Ivy Lam was also supported by the Ontario Graduate Scholarship and a University of Waterloo President’s Graduate Scholarship.
Conflict of Interest: None of the authors have any conflicts of interest to declare.
Ethical standard: Participants provided written informed for in-person focus groups and verbal informed consent for key informant interviews and webinar focus groups, as these were conducted over the telephone. Participants who provided verbal consents received e-mailed information packages with consent forms notifying participants of the study’s ethics approval, that the session was to be audio recorded, and that their participation was voluntary; participation indicated their consent to participate. These consent procedures were approved by the Research Ethics Board at the University of Waterloo.
References
1. Wendland BE, Greenwood CE, Weinberg I, Young KWH. Malnutrition in institutionalized seniors: The iatrogenic component. J. Am. Geriatr. Soc. 2003;51(1):85–90.
2. Lengyel CO, Smith JT, Whiting SJ, Zello GA. A questionnaire to examine food service satisfaction of elderly residents in long-term care facilities. J. Nutr. Elder. 2004;24(2):5–18.
3. Sturtzel B, Dietrich A, Wagner KH, Gisinger C, Elmadfa I. The status of vitamins B6, B12, folate, and of homocysteine in geriatric home residents receiving laxatives or dietary fiber. J. Nutr. Health Aging. 2010;14(3):219–223.
4. Aghdassi E, McArthur M, Liu B, McGeer A, Simor A, Allard JP. Dietary intake of elderly living in Toronto long-term care facilities: comparison to the dietary reference intake. Rejuvenation Res. 2007;10(3):301–309.
5. Grieger JA, Nowson CA. Nutrient intake and plate waste from an Australian residential care facility. Eur. J. Clin. Nutr. 2007;61(5):655–663.
6. Dunne JL, Dahl WJ. A novel solution is needed to correct low nutrient intakes in elderly long-term care residents. Nutr. Rev. 2007;65(3):135–138.
7. Crogan NL, Alvine C, Pasvogel A. Improving nutrition care for nursing home residents using the INRx process. J. Nutr. Elder. 2006;25(3-4):89–103.
8. Cameron ID, Kurrle SE, Uy C, Lockwood K a, Au L, Schaafsma FG. Effectiveness of oral nutritional supplementation for older women after a fracture: rationale, design and study of the feasibility of a randomized controlled study. BMC Geriatr. 2011;11(1):32.
9. Milne A, Potter J, Vivanti A, Avenell A. Protein and energy supplementation in elderly people at risk from malnutrition ( Review ). 2009;(2).
10. Fiatarone Singh MA, Bernstein MA, Ryan ND, O’Neill EF, Clements KM, Evans WJ. The effect of oral nutritional supplements on habitual dietary quality and quantity in frail elders. J. Nutr. Heal. Aging. 2000;4(1):5–12.
11. Young KWH, Greenwood CE, Van Reekum R, Binns MA. Providing nutrition supplements to institutionalized seniors with probable Alzheimer’s disease is least beneficial to those with low body weight status. J. Am. Geriatr. Soc. 2004;52(8):1305–1312.
12. Miller MD, Daniels LA, Bannerman E, Crotty M. Adherence to nutrition supplements among patients with a fall-related lower limb fracture. Nutr. Clin. Pract. 2005;20(5):569–78.
13. Wilson M-MG, Purushothaman R, Morley JE. Effect of liquid dietary supplements on energy intake in the elderly. Am. J. Clin. Nutr. 2002;75(5):944–7.
14. Romanow RJ. Building on Values: The Future of Health Care in Canada – Final Report. Saskatoon; 2002.
15. Adolphe JL, Whiting SJ, Dahl WJ. Vitamin fortification of puréed foods for long-term care residents. Can. J. Diet. Pract. Res. 2009;70(3):143–50.
16. Oakley GP. Oral synthetic folic acid and vitamin B12 supplements work–if one consumes them. Nutr. Rev. 2004;62(6 Pt 2):S22–6; discussion S27–8.
17. Simmons SF, Lam HY, Rao G, Schnelle JF. Family members’ preferences for nutrition interventions to improve nursing home residents’ oral food and fluid intake. J. Am. Geriatr. Soc. 2003;51(1):69–74.
18. Consultant Dietitians in Health Care Facilities Dietetic Practice Group. Involuntary weight loss. In: Niedert KC, Dorner B, eds. Nutrition Care of the Older Adult. Chicago: American Dietetic Association; 2004:202–209.
19. Castellanos VH, Litchford MD, Campbell WW. Modular protein supplements and their application to long-term care. Nutr. Clin. Pract. 2006;21(5):485–504.
20. Bourdel-Marchasson I. How to improve nutritional support in geriatric institutions. J. Am. Med. Dir. Assoc. 2010;11(1):13–20.
21. Beck AM, Ovesen L, Schroll M. Home-made oral supplement as nutritional support of old nursing home residents, who are undernourished or at risk of undernutrition based on the MNA. A pilot trial. Aging – Clin. Exp. Res. 2002;14(3):212–215.
22. Nowson CA, Sherwin AJ, McPhee JG, Wark JD, Flicker L. Energy, protein, calcium, vitamin D and fibre intakes from meals in residential care establishments in Australia. Asia Pac. J. Clin. Nutr. 2003;12(2):172–177.
23. Health Canada. Dietary Reference Intakes Tables. Gov. Canada. 2010. Available at: http://www.hc-sc.gc.ca/fn-an/nutrition/reference/table/index-eng.php [Accessed February 6, 2014].
24. De Jong N, Chin A Paw MJ, de Graaf C, Hiddink GJ, de Groot L, van Staveren WA. Appraisal of 4 months’ consumption of nutrient-dense foods within the daily feeding pattern of frail elderly. J. Aging Health. 2001;13(2):200–16.
25. Lengyel CO, Whiting SJ, Zello GA. Nutrient inadequacies among elderly residents of long-term care facilities. Can. J. Diet. Pract. Res. 2008;69(2):82–88.
26. Sidani S, Epstein DR, Bootzin RR, Moritz P, Miranda J. Assessment of preferences for treatment: validation of a measure. Res. Nurs. Health. 2009;32(4):419–31.
27. Padgett D. Qualitative methods in social work research: Challenges and rewards. 1st ed. California: SAGE PUBLICATIONS INC; 1998.
28. Krueger RA, Casey MA. Focus Groups : A Practical Guide for Applied Research. Thousand Oaks: Sage Publications; 2000.
29. Galloway KL. Focus groups in the virtual world: Implications for the future of evaluation. New Dir. Eval. 2011;2011(131):47–51.
30. Braun V, Clarke V. Using thematic analysis in psychology. Qual. Res. Psychol. 2006;3(2):77–101.
31. Myers A. Program Evaluation for Exercise Leaders. 1st ed. IL: Human Kinetics; 1999.
32. Corbin JM, Strauss A. Grounded theory research: Procedures, canons, and evaluative criteria. Qual. Sociol. 1990;13(1):3–21.
33. Dahlke R, Wilson SL. Focus Groups as Predictors of Dietitians’ Roles on Interdisciplinary Teams.pdf. 2000.
34. Hsieh H-F, Shannon SE. Three approaches to qualitative content analysis. Qual. Health Res. 2005;15(9):1277–88.
35. Service Canada. Dietitians and Nutritionists. Gov. Canada. 2013. Available at: http://www.servicecanada.gc.ca/eng/qc/job_futures/statistics/3132.shtml [Accessed March 21, 2014].
36. Sazawal S, Habib a KMA, Dhingra U, Dutta A, Dhingra P, Sarkar A, Deb S, Alam J, Husna A, Black RE. Impact of micronutrient fortification of yoghurt on micronutrient status markers and growth – a randomized double blind controlled trial among school children in Bangladesh. BMC Public Health. 2013;13(1):514.
37. Kupferschmidt K. Uncertain verdict as vitamin D goes on trial. Science. 2012;337(6101):1476–8.
38. Begley A, Coveney J. Wonder vitamin or mass medication? Media and academic representation of folate fortification as a policy problem in Australia and New Zealand. Aust. N. Z. J. Public Health. 2010;34(5):466–71.
39. Berry D. Trends in Fortification. Dairy Foods. 2004;105(4):36–41.
40. Mocanu V, Stitt PA, Costan AR, Voroniuc O, Zbranca E, Luca V, Vieth R. Long-term effects of giving nursing home residents bread fortified with 125 microg (5000 IU) vitamin D(3) per daily serving. Am. J. Clin. Nutr. 2009;89(4):1132–1137.
41. Bonjour JP, Benoit V, Pourchaire O, Ferry M, Rousseau B, Souberbielle JC. Inhibition of markers of bone resorption by consumption of vitamin D and calcium-fortified soft plain cheese by institutionalised elderly women. Br. J. Nutr. 2009;102(7):962–966.
42. Bermejo LM, Aparicio A, Rodriguez-Rodriguez E, Lopez-Sobaler M, Andres P, Ortega RM. Dietary strategies for improving folate status in institutionalized elderly persons. Br. J. Nutr. 2009;101(11):1611–1615.
43. Van der Wielen R, van Heereveld H, de Groot C, van Staveren W. Nutritional status of elderly Female nursing home residents; the effect of supplementation with a physiological dose of water-soluble vitamins. Eur J Clin Nutr. 1995;49(9):665–74.
44. Keane EM, O’Broin S, Kelleher B, Coakley D, Walsh JB. Use of folic acid-fortified milk in the elderly population. Gerontology. 1998;44(6):336–339.
45. Turney L, Pocknee C. Virtual Focus Groups : New Frontiers in Research. 2005:32–43.
46. Wang S. Use of the Webinar Tool ( Elluminate ) to Support Training : The Effects of Webinar-Learning Implementation from Student-Trainers ’ Perspective. 2008;7(3):175–194.
47. Kramish Campbell M, Meier A, Carr C, Enga Z, James AS, Reedy J, Zheng B. Health behavior changes after colon cancer: a comparison of findings from face-to-face and on-line focus groups. Fam. Community Health. 2001;24(3):88–103.