H.J. Shim
Corresponding author: H.J. Shim, George Warren Brown School of Social Work, Washington University in St. Louis, USA, simhyunju@hotmail.com
Abstract
The increasing number of older adults in the US suggests accordingly increasing older populations with Alzheimer’s Disease (AD). As some studies found a higher prevalence of AD among ethnic minority older adults, understanding different needs of ethnic minority caregivers is an important task. Using the REACH II data, the current study analyzed what caregivers’ and care recipients’ characteristics contribute to predicting caregivers’ consideration about institutionalization, and whether such difference was associated with caregivers’ ethnicity/race. A binary logistic regression was done to evaluate how these characteristics were associated with caregivers’ having consideration/no consideration about institutionalization. The final model was significant (χ2 (12) = 741.37, p <.001), with caregivers’ ethnicity and perceived burden about caregiving as strong predictors.
Key words: Alzheimer’s disease, caregivers, stress, Institutionalization, ethnicity.
Introduction
Studies show that ethnic minority caregivers are less likely to institutionalize their loved ones than White caregivers (1, 2). The ethnic composition of the older adult population in the US is expected to become dramatically diverse by 2050. Whereas non-Hispanic White older adults aged 65 years and over accounted for 80.2% of older populations in the US in 2010, by 2050, this number is projected to drop to 58.5% (3). With this dramatic rise in the diversity of the older populations comes an increase in the number of ethnic minorities diagnosed with Alzheimer’s Disease (AD). Non-Hispanic White older adults aged 65 and older have a prevalence of 7.8% in developing AD while this prevalence goes up to 18.8% for African Americans and 20.8% for Hispanics (4). Considering these estimates, understanding the different needs of African American and Hispanic older adults is a crucial task for both researchers and practitioners.
Unfortunately, despite a growing interest in the ethnic differences that shape the context of caregiving experiences, previous studies have so far been mostly exploratory and atheoretical and focused on White caregivers (2, 5). Culturally relevant and reliable practices are needed for caregivers of individuals with AD across different ethnic groups (6).The findings of previous studies have also largely reinforced the popular beliefs about ethnic minority caregivers: compared to White caregivers, (a) they are less likely to feel stressed out about caregiving and more likely to endorse positive aspects of caregiving experiences (7, 8); (b) they use less formal support and more informal support (6); (c) they are more likely to have poor physical health (9); (d) they are less likely to institutionalize care recipients (10). However, several limitations of the previous literature warrant caution in directly translating these results across different ethnic groups of caregivers.
First, previous studies use inconsistent measures without reliable theoretical models; therefore, the results are not comparable. Also, most studies involving a sample of different ethnic caregivers primarily relied on a convenience sample; thus, generalizing the results to larger and diverse populations of caregivers solely based on their ethnicity is not appropriate (5).
In addition, studies show that ethnic minority caregivers are less likely to institutionalize their care recipients than White caregivers (1, 2). Despite these findings, the reasons have not been fully explored. Previous literature analyzing the caregivers’ reasons for institutionalization has used predominantly White, female samples.
Thus far, no studies have examined different levels of consideration about institutionalization among ethnic minority caregivers of older adults with AD. To promote deeper understanding of diverse ethnic caregivers’ consideration for institutionalization, the aim of the current study is to examine variations in consideration about institutionalization among different ethnic groups of caregivers using the secondary analysis of the Resources for Enhancing Alzheimer’s Caregiver Health II (REACH) data. The REACH II study is the first cross-sectional study to simultaneously test a comprehensive caregiver intervention in three distinct racial/ethnic groups: Hispanic, African American, and White. The hypothesis assumes that ethnic minority caregivers will be less likely to have consideration about institutionalization of their care recipients. The primary objective of the study is to explore whether such variation is attributable to ethnicity or other caregivers’ or care recipients’ characteristics that have been identified through previous literature, which include caregivers’ use of formal services, amount of caregiving hours, burden, and other socioeconomic backgrounds, and care recipients’ physical and cognitive health. The study will use 2002-2004 REACH II baseline data to answer the following question:
Is there a difference in having consideration about institutionalization according to caregivers’ different ethnicity (i.e., Non-Hispanic White, African Americans, and Hispanic) controlling for caregivers’ other characteristics (i.e., hours of caregiving, use of formal services, burden) and care recipients’ characteristics (i.e., cognitive and physical functioning)?
The findings of the proposed study will be important for policy-makers and practitioners who work with older adults of ethnic minority by deepening the understanding about the heterogeneity of their caregiving experiences and different concerns regarding placement.
Ha: The caregivers’ having consideration/no consideration about institutionalization will significantly differ by races (i.e., Non-Hispanic White, African-Americans, and Hispanic).
Ho: The caregivers’ having consideration/no consideration about institutionalization will not significantly differ by races (i.e., Non-Hispanic White, African-Americans, and Hispanic).
Literature review
Previous studies have been largely exploratory and atheoretical
As the number of minority elders is projected to rise significantly, the effort to understand their different needs and also the distinct needs of caregivers has been demonstrated through many studies on caregiving among diverse ethnic groups (5, 6). Caregivers are “hidden patients” of AD (11). Therefore, the higher prevalence of AD among older adults of ethnic minority does not solely indicate the needs of those individuals with AD, but also the needs of their caregivers. Although African Americans are more than twice as likely to develop AD and Hispanics at least more than one and a half times more likely compared to White counterparts, their rates of Medicare-claimed diagnosis of AD falls significantly below this difference (4). Possible reasons for this have been proposed as lack of insurance coverage, mistrust of health professionals, and a lack of knowledge of AD among caregivers; hence, more research is needed to validate these explanations.
Several authors raised concerns that existing literature largely replicates findings that reinforce popular myths about ethnic minority caregivers. Pinquart and Sorensen (2005) challenged previous literature in analyzing popular beliefs about ethnic minority caregivers (e.g., they were younger, less likely to be a spouse, and less likely to be married than White caregivers, more likely to provide higher care hours per week and more likely to report a larger number of caregiving tasks). With a meta-analysis of the results of 116 empirical studies, these authors examined how differences of caregivers’ race influenced their objective stressors, filial obligations, beliefs, and psychological and physical health. Some findings raised important issues for further research. For example, although it was found that African American caregivers were significantly less likely to feel burden related to caregiving compared to non-Hispanic White caregivers, Hispanic and Asian caregivers were more likely to feel depressed than Whites. Also, only Asian American caregivers were less likely to use formal support than non-Hispanic White caregivers, and no significant differences were found among African Americans and Hispanics.
In summary, the review of previous studies on ethnic minority caregivers of elderly with AD suggests a need to develop a culturally sensitive and reliable theoretical model that can be consistently applied to studies of different ethnic minorities and to examine at a deeper level what factors influence the different caregiving experiences of different ethnic groups, rather than replicating results that reinforce popular myths about ethnic minority caregivers.
There is a need to examine socioeconomic contexts across different ethnicities.
When examining institutionalization of care recipients with Alzheimer’s, most studies consistently found that ethnic minority caregivers were significantly less likely to institutionalize their care recipients with AD(7, 10).
Several authors came up with possible reasons, such as language barrier, discrimination, and positive aspects of caregiving (8), but these results have not been validated through further studies with a qualitative approach that seeks responses from those caregivers. Most of them have been conducted as quantitative studies and rely heavily on the investigators’ assumption that might have been influenced by popular beliefs about ethnic minority caregivers. However, some studies raise critical question around this issue. For example, in a study that compared non-Hispanic White female caregivers to Hispanic female caregivers, Mausbach and other colleagues (2004) concluded that Hispanics were significantly less likely to institutionalize their care recipients with AD, but only the positive aspects of caregiving were found to contribute to this ethnic difference. They found, to their surprise, that the Hispanic caregivers with less positive views of caregiving were not only more likely to institutionalize compared to other Hispanics with more positive views of caregiving, but also more likely to institutionalize than non-Hispanic White caregivers with both more and less positive views of caregiving. Thus, it is misleading to state that ethnic minority caregivers are less likely to institutionalize simply because they feel less burden due to their ethnic and there is a strong need to examine socioeconomic contexts.
In conclusion, while many studies report that ethnic minority caregivers are significantly less likely to institutionalize care recipients with AD, the effort to examine why should be exerted to explain reasons behind such phenomena and deepen the understanding about ethnic minority caregivers.
Most research on institutionalization has focused on identifying predictors of institutionalization, rather than examining the concerns behind caregivers’ decisions
Not enough research has examined communication behind the decision to institutionalize patients with AD among ethnically diverse caregivers. Previous literature analyzing the caregivers’ reasons for institutionalization used a sample of caregivers primarily composed of White women (1, 2). McLennon, Habermann and Davis (2010) reported that the main reasons for institutionalization stemmed from health problems, either of caregivers or care recipients or both, and the caregivers who eventually institutionalized their care recipients discussed the need for more help approximately 3 to 4 months prior to actual placement. Likewise, Buhr, Kuchibhatla and Clipp (2006) found that caregivers’ reasons for placement included the need for more skilled care, caregivers’ poor health, and care recipients’ dementia-related behavior problems, and White caregivers were 1.7 times more likely to institutionalize compared to non-White counterparts. Finally, Spitznagel, Tremont, Davis and Foster (12) found that the caregivers who institutionalized their care recipients were significantly more likely to have higher levels of burden and greater caregiver knowledge about dementia compared to those who did not institutionalize. However, as previously mentioned, the limitation of the sample is noted across those studies, and thus there is a strong need to examine the reasons for institutionalization by ethnic minority caregivers.
Theoretical Framework
Theoretical Basis: A Model of Ethnic Differences in Caregiving Variables
Previous studies have been largely limited in the use of theoretical models and primarily relied on empirical generalization. Several authors proposed a need to develop conceptual frameworks and theoretical perspectives that are culturally relevant to ethnic minority caregivers. To meet this need, Pinquart and Sorensen (2005) proposed a model of ethnic differences in associations between caregiving variables based on their review of 116 empirical studies related to ethnic minority caregivers (Figure 1 in Appendix A).
In this model, Pinquart and Sorensen (2005) propose that ethnic variation exists depending on four different constructs: (a) resources and cultural norms (e.g., positive appraisal, faith, use of formal services, etc.), (b) care receiver health and functioning (e.g., objective care needs, physical functioning, cognitive status, etc.), (c) amount of care provided (e.g., hours per day, etc.); (d) other caregiver background (e.g., age, gender, family position, employment, education, income) (p. 91). These constructs lead to different outcomes in psychological and physical health of caregivers, which can then be shown to influence ethnic differences in caregiving outcomes. Based on the model developed by Pinquart and Sorensen (2005), this study proposes to examine how ethnic differences lead to variations in consideration about institutionalization using five predictors (i.e., caregivers’ use of formal services, caregiving burden, hours of caregiving, care recipients’ physical functioning & cognitive functioning) as illustrated in Figure 2 (Appendix A).
Methodology
Data Set
The current study uses the Resources for Enhancing Alzheimer’s Caregivers Health (REACH) II study collected from 2002 to 2004 available from the ICPSR website. The REACH II study aimed to offer a multicomponent intervention for caregivers taking care of people with AD at home to reduce their caregiving burden and stress and improve their well-being. The study was conducted in five different cities (Birmingham, Alabama; Memphis, Tennessee; Miami, Florida; Palo Alto, California; and Philadelphia, Pennsylvania) and was the first research to include a similar proportion of Hispanic, African-American, and White caregivers. The data that were collected at the baseline from 2002-2003 had a total sample of 670 caregivers. However, for the purpose of this study, the following participants were excluded from the sample. Caregivers who did not specify their race were excluded (n=28) and those who did not have responses to the outcome questions were excluded (n=27). As a result, a total of 615 cases including 204 Hispanics, 200 African Americans, and 211 non-Hispanic Whites were analyzed for the final model.
Instruments and Measures
The validity and reliability of the overall assessment questionnaire used in the REACH II study have been found to be significant with the Cronbach’s alpha= .65 (13). Out of all 59 items on the questionnaire, the following items were chosen for the present study.
Dependent Variable
Consideration about institutionalization: The REACH II study used the Desire to Institutionalize (DIS) scale with six items that were used to record information regarding the caregiver’s plans for institutionalization of a care recipient (see Appendix B). The items indicated a self-reported level of consideration about institutionalization ranging from considering placement of a care recipient, whether a caregiver thought doing so would be better off for the care recipient, discussing such consideration with other family members, friends, or the care recipient, to actually planning to move the care recipient to an institution. For the purpose of the present study, all responses to the six questions were summed up as an index variable to predict caregivers’ having consideration/ no consideration about institutionalization as the binary outcome variable.
Independent Variable
Race/Ethnicity: Two questions asked the race of caregivers. The first question asked, “Would you describe yourself as Hispanic or Latino/a?” and the participants answered either “Yes” or “No.” The second question asked, “How would you describe your primary racial group?” and the participants could choose “White,” “African American,” “Asian,” “American Indian,” “Native Hawaiian,” and “other.” The response variables of both questions were combined into one single variable and the respondents of other races besides White, Hispanic, and African Americans were excluded (n = 28). Finally, the race of caregivers was recoded into three dummy variables- White (White = 1, other races = 0), Black (African American = 1, other races = 0), Hispanic (Hispanic = 1, other races = 0)- for each ethnic group.
Control Variables
Resources and Cultural Norms: There were 23 items used in the original REACH II study to record information regarding the variety and frequency of usage of community-based medical and other care services. Unfortunately, no single question comprehensively assessed different formal services available to caregivers. Therefore, for the purpose of this study, key questions were selected based on the highest frequency and questions with high missing values were screened out. Based on these procedures, five close-ended questions that asked about the use of homemakers, transportation services, visiting nurses, and the use of a day care center and the visits to a doctor were selected for the analysis (see Appendix C). These variables were binary coded as “0=No” or “1=Yes,” since the participants could answer “yes” to more than one question. Most caregivers using the formal services said that they were using them for care recipients, as 82.9% of caregivers using the transportation service said they were using it for their loved ones, and 92.2% of caregivers using the visiting nurse and 88.8% of those using the adult day care center responded the same way. However, only 31.0% of caregivers who used the homemaker said they were using it for care recipients, and also 50.8% of those who had visits to their doctors said they did so for their loved ones.
Caregivers’ Amount of Care Provided: The amount of care provided to care recipients a day was measured with an open question that asked, “About how many hours a day do you estimate that you are actually doing things for a care recipient (CR)?” The amount of care provided to care recipients is a continuous variable measured in number of hours of care provided.
Caregiver Burden: The REACH II study used 12 items of the Zarit Burden Interview to record information regarding the caregivers’ burden in caring for the care recipients in the original data. As the Cronbach’s alpha = .86, it is reasonable to conclude that caregiver burden was reliably measured. For the purpose of the study, a continuous variable that adds together caregivers’ answers to six questions was created as a summated index and entered in the final model.
Care Recipients’ Physical and Cognitive Functioning: To measure physical health of care recipients, one question measuring Activities of Daily Living (ADL; e.g., dressing, eating, bathing, etc.) and one question measuring Instrumental Activities of Daily Living (IADL; shopping, medication, finances, etc.) were entered as the overall measure of physical health of the care recipient. Each question asked in the same format, “During the past six months, have you seen any improvement overall, in the areas we just discussed? Was there no change, minimal decline or substantial decline in these areas?” The answers for both ADL and IADL questions were recoded as “0=No change” and “1=Decline.” The Mini–mental state examination (MMSE) scores of each care recipient were used as a continuous variable to measure the cognitive functioning of care recipients in the model.
Statistical Analyses
First of all, descriptive statistics were conducted on the independent and dependent variables. Next, bivariate analyses were used to compare the relationship of each control variable in the model; chi-square tests were used for categorical variables, and independent samples t tests were used for continuous variables. Finally, the multivariate analysis was conducted using binary logistic regression to predict caregivers’ having consideration/no consideration about institutionalization. SAS version 9.0 was used for both bivariate and multivariate analyses.
Results
Table 1 presents the characteristics of caregivers and care recipients in the study. Overall, 52.7% (n = 324) of caregivers had no consideration about institutionalization, compared to 47.3% (n = 291) who had consideration. As previously described, the racial proportion of participants was evenly distributed, as 34.3% (n = 211) were Non-Hispanic White, 32.5% (n = 200) were African Americans, and 33.2% (n = 204) were Hispanic. On average, caregivers were taking care of their care recipients 8.49 (SD=5.00) hours a day. Also, the average score of caregivers’ burden scale was 18.49 (SD=9.80) and no extreme values were observed. As for care recipients’ characteristics, 52.8% (n=325) were reported to have a decline in their ADL and 62% (n=381) had a decline in their IADL. The care recipients’ cognitive functioning was measured with the scores of the MMSE, and the average score was 12.5 (SD=7.40).
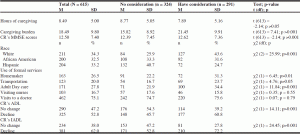
Table 1 Characteristics of caregivers and care recipients sample from the REACH II study (2002-2004) (N=615)
Table 2 illustrates that there was a statistically significant association between the race of caregivers and the caregivers’ consideration about institutionalization, χ2 (2, N=615) = 25.99; p <.001. Compared to only 39.8% of White caregivers who had no consideration about institutionalization, more than half of African American (54.0%) and Hispanic (64.7%) caregivers denied having any consideration about placing their loved ones in institutions. In addition, whereas almost two thirds of White caregivers (60.2%) had consideration about institutionalization, fewer than half of African American (46.0%) and even fewer Hispanic (35.3%) caregivers said they had such consideration.
To test assumptions of binary logistic regression, the diagnostic tests were done prior to running binary logistic regression, to determine if the model was a good fit for the data. Multicollinearity and the tolerance level were tested, and no tolerance value was < .25 and no VIF value was >2. The average VIF was slightly greater than 1, indicating no concerns for multicollinearity. Also, running the model with the continuous IV yielded a non-significant result of Hosmer and Lemeshow Goodness-of-Fit Test (χ2= 5.23, p = 0.73). As for the influence analysis, Cook’s D and Standardized residuals were examined and no outliers were identified. In summary, diagnostic tests of the model showed that the model was a good fit for the data and can be generalized to larger populations.
Table 3 describes the results from the binary logistic regression model predicting caregivers’ having consideration/no consideration about institutionalization. The table illustrates odds ratios with the reference group of having consideration about institutionalization which are significant at the 5% level. The model controlled for both caregivers’ characteristics (use of formal services, caregiver burden, caregiving hours) and care recipients’ characteristics (IADL, ADL, MMSE scores) except for ethnicity/race, which was an independent variable.
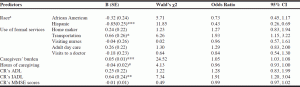
Table 3 Binary Logistic Regression Results for Characteristics predicting Caregivers’ Level of Consideration about Institutionalization
As presented in Table 3, the model was significant, at χ2 (12) = 741.37; p <.0001, with Nagelkerke R2 = .20. Overall, the model correctly classified 63.1% using the standard threshold for predicting event (p<.05). The results indicate that caregivers’ race and stress were significant indicators of predicting caregivers’ having consideration/no consideration about institutionalization (p < .001), controlling for other variables in the model. Interestingly, caregivers’ race was significantly associated with caregivers’ consideration about institutionalization among only Hispanic caregivers, but the result was not statistically significant for African American caregivers. For instance, the odds of having consideration about institutionalization was 57% lower for Hispanic caregivers compared to Non-Hispanic White caregivers (OR = 0.85; 95% CI = 0.26 – 0.69, p < .001), controlling for other variables in the model. Another strong predictor was the caregivers’ burden. As caregiver’s burden increased by one unit, the odds of having consideration about institutionalization increased by 5% (OR = 0.05; 95% CI = 1.03 – 1.08, p < .001) when controlling for other variables in the model. Other significant predictors include caregivers’ use of transportation service for care recipients and caregiving hours (p < .05). Other caregiving characteristics associated with consideration about institutionalization were hours of caregiving, the use of transportation services, although these results were not as strongly significant as caregivers’ race and burden. When controlling for other variables in the model, one additional caregiving hour reduced the odds of having consideration by 4% (OR = – 0.04; 95% CI = 0.93 – 1.00, p < .05). On the other hand, caregivers who used the transportation service for care recipients were 93% more likely to consider institutionalization (OR = 0.66; 95% CI = 1.15 – 3.22, p < .05).
Finally, among care recipients’ characteristics, only the IADL was significantly associated with caregivers’ consideration about institutionalization. Controlling for other variables in the model, the odds ratios of thinking about institutionalization for care recipients who have more declines in their IADL were 91% higher compared to the odds of care recipients who have mild/no decline in their IADL (OR = 0.64; 95% CI =1.20 – 3.04, p < .001).
Discussion
The current study is one of the few to examine factors associated with caregivers’ consideration about institutionalization of their care recipients with AD and how this consideration differs across three different ethnic groups controlling for other caregivers’ and care recipients’ characteristics. The hypothesis was partially supported in that ethnicity was significantly associated with caregivers’ consideration about institutionalization. However, the result was only significant for Hispanic caregivers but not significant for African American caregivers, compared to Non-Hispanic White caregivers. This result raises an important need to examine reason behind Hispanic caregivers’ reluctance to think of institutionalization. Some previous studies indicate that linguistic barrier and cultural incompetence of service providers act as a great hindrance for ethnic minority caregivers to utilize health care services, especially when their first language is not English (9). Hence, further research should examine whether language barrier is the main reason that deters Hispanic caregivers from considering the placement of their loved ones.
Secondly, one of the key findings of this study is that caregivers’ burden was found to be another strong predictor of institutional consideration besides ethnicity. Therefore, further analysis of how ethnic minority caregivers differ in their perceived burden about caregiving will be an important task for both researchers and professionals in practice. Although the majority of previous studies suggest that ethnic minority caregivers tend to express less burden about caregiving compared to Non-Hispanic White counterparts (5), some studies reported that African American caregivers showed significantly lower burden about caregiving compared to Non-Hispanic White caregivers, while Asian American and Hispanic caregivers expressed higher burden compared to African Americans (6). Considering the fact that older populations in the US are increasingly becoming more diverse and the number of patients diagnosed with AD and their caregivers is on the rise, the effort to understand differences in perceived burden and the needs of ethnic minority caregivers is urgently needed. At the same time, social workers and policy makers should not be misinformed that being an ethnic minority makes caregivers immune from feeling stressed. Practitioners and clinicians should work toward meeting the diverse needs of caregivers related to transitioning their loved ones to an institution.
However, some limitations of the current study should be taken into consideration when interpreting the results. First, it is limited in that the data is cross-sectional and rely heavily on the self-reported questionnaires of caregivers of persons with AD. Also, it should be noted that the REACH II study uses a convenience sample, which indicates a concern for generalizing the results to larger groups of caregivers solely based on their ethnicity. Therefore, a future study should be developed to employ a probability sampling and use a prospective, longitudinal design in order to examine in detail what factors influence consideration of institutionalization for different ethnic groups of caregivers.
Finally, this research commits the “homogeneity fallacy” (14) by treating caregivers of different ethnicities as a homogeneous group with the same cultural values. For instance, the term Hispanic can be broken down into several subcategories of ethnic groups (i.e., Mexican, Cuban, Chileans, etc.) and they may not necessarily share the same beliefs around caregiving experiences. However, for the present research, the term Hispanic was used as an umbrella term that includes all of different subgroups of people who speak Spanish and are from Latin America. Future studies may focus on a particular ethnic group (e.g. Asians) and examine how different subgroups (e.g., Chinese, Koreans, Japanese) perceive caregiving experiences and consider institutionalization differently.
In conclusion, the present study examined how caregivers’ consideration about institutionalization differed by ethnicity controlling for other caregivers’ characteristics and care recipients’ characteristics. The results show that, while caregivers’ ethnicity may have some effect on caregivers’ consideration, understanding caregivers’ burden and other caregivers’ characteristics and also knowing about care recipients’ IADL functioning level is important. Despite its several limitations, the findings raise an important need to understand perceived burden related to caregiving among caregivers who are of different ethnic groups. Health and social service professionals should bear these results in mind when working with families impacted by AD and assessing caregiving situations among ethnic minority caregivers and care recipients.
Acknowledgements: The author would like to thank Dr. Nancy Morrow-Howell and Dr. Shanta Pandey for their assistance with article preparation and research guidance.
Conflict of Interest: The author certify that no funding has been received for the conduct of this study. There is no conflict of interest with any financial organization regarding the material discussed in the manuscript.
Ethical standard: I certify that this study involving caregivers and their care recipients diagnosed with Alzheimer’s disease followed the institutional and national guidelines for conducting the research.
References
1. Buhr, G. T., Kuchibhatla, M. M., & Clipp, E. C. Caregivers’ reasons for nursing home placement: Clues for improving discussions with families prior to the transitions. The Gerontologist, 2006;46(1), 52-61.
2. McLennon, S., Habermann, B., & Davis, L. Deciding to institutionalize: Why do family members cease caregiving at home? Journal of Neuroscience Nursing, 2010;42(2), 95-103.
3. U.S. Bureau of the Census. The next four decades. The older population in the United States: 2010 to 2050. Retrieved from http://www.census.gov/prod/2010pubs/p25-1138.pdf
4. Alzheimer’s Association. Alzheimer’s disease facts and figures 2010: Includes a special report on race, ethnicity and Alzheimer’s disease. Retrieved from http://www.alz.org/documents_custom/report_alzfactsfigures2010.pdf
5. Dilworth-Anderson, P., Williams, I., & Gibson, B. Issues of race, ethnicity, and culture in caregiving research: A 20-year review (1980-2000). The Gerontologist, 2002;42(2), 237-272.
6. Pinquart, M. M., & Sorensen, S. S. Ethnic differences in stressors, resources, and psychological outcomes of family caregiving: a meta-analysis. The Gerontologist, 2005;45(1), 90-106.
7. Mausbach, B., Coon, D., Depp, C., Rabinowitz, Y., Wilson-Arias, E., Kraemer, H., & … Gallagher-Thompson, D. Ethnicity and time to institutionalization of dementia patients: A comparison of Latina and Caucasian female family caregivers. Journal of the American Geriatrics Society, 2004;52(7), 1077-1084. Retrieved from http://web.ebscohost.com.libproxy.wustl.edu
8. Vickrey, B. G., Strickland, T. L., Fitten, L. J., Adams, G. R., Ortiz, F. F., & Hays, R. D. Ethnic variations in dementia caregiving experiences: Insights from focus groups. Journal of Human Behavior in the Social Environment, 2007;15(2/3), 233-249. Retrieved from http://web.ebscohost.com.libproxy.wustl.edu
9. Ho, C., Weitzman, P., Cui, X., & Levkoff, S. Stress and service use among minority caregivers to elders with dementia. Journal of Gerontological Social Work, 2000;33(1), 67-88. Retrieved from http://web.ebscohost.com.libproxy.wustl.edu
10. Yaffe, K., Fox, P., Newcomer, R., Sands, L., Lindquist, K., Dane, K., & Covinsky, K. E. Patient and caregiver characteristics and nursing home placement in patients with dementia. Journal of the American Medical Association, 2002;287(16), 2090-2097. doi:10.1001/jama.287.16.2090
11. Griffith, P. Supporting caregivers in ethnically diverse communities: Focus on Alzheimer’s disease. Clinical Geriatrics, 2010;18(2), 36-40. Retrieved from http://69.167.171.53/articles/Supporting-Caregivers-Ethnically-Diverse-Communities-Focus-Alzheimer%E2%80%99s-Disease?page=0,5
12. Spitznagel, M., Tremont, G., Davis, J., & Foster, S. M. Psychosocial predictors of dementia caregiver desire to institutionalize: Caregiver, care recipient, and family relationship factors. Journal of Geriatric Psychiatry & Neurology, 2006;19(1), 16-20. doi:10.1177/0891988705284713
13. Czaja, S. J., Gitlin, L. N., Schulz, R., Song, Z., Burgio, L. D., Stevens, A. B., & … Gallagher-Thompson, D. Development of the Risk Appraisal Measure: A brief screen to identify risk areas and guide interventions for dementia caregivers. Journal of the American Geriatrics Society, 2009;57(6), 1064-1072. doi:10.1111/j.1532-5415.2009.02260
14. Ishii-Kuntz, M. Intergenerational Relationships Among Chinese, Japanese, and Korean Americans. Family Relations, 1997;46(1), 23-32. Retrieved from http://web.ebscohost.com.libproxy.wustl.edu
Appendix A
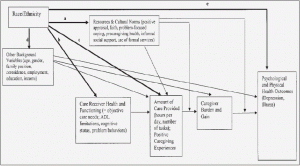
Figure 1. A model of ethnic differences in the mean levels of and associations between caregiving variables (ADL = activity of daily living) by Pinquart & Sorensen (2005)
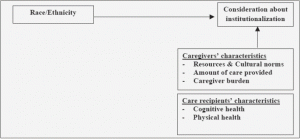
Figure 2. Revised model of ethnic differences in caregivers’ level of consideration about institutionalization
Appendix B
Caregivers’ Desire to Institutionalize Scale (DIS)
(1) In the past six months, have you considered a nursing home, boarding home or assisted living for a care recipient?
No = 1, Yes = 2
(2) In the past six months, have you felt that a care recipient would be better off in a nursing home, boarding home or assisted living?
No = 1, Yes = 2
(3) In the past six months, have you discussed the possibility of a nursing, boarding home or assisted living with family members or others?
No = 1, Yes = 2
(4) In the past six months, have you discussed that possibility with a care recipient?
No = 1, Yes = 2
(5) In the past six months, have you taken any steps towards placement?
No = 1, Yes = 2
(6) In the next six months, are you likely to move a care recipient to another living arrangement? No = 1, Yes = 2
Index Variable
– 1= No consideration = scores of 6
– 0= Have consideration = scores of 7 and above
Appendix C
Caregivers’ Use of Formal Services
(1) In the past month, did you or CR have a homemaker who helped with shopping, cleaning, laundry, preparing meals, etc?
No = 1, Yes = 2
(2) In the past month, did you or CR use a formal service that provided transportation to places outside the home (i.e doctors, clinics, shopping)?
No = 1, Yes = 2
(3) In the past month, did you or CR have a visiting nurse come to check medications, blood pressure or other medical needs?
No = 1, Yes = 2
(4) In the past month, did you or CR attend a senior day care or senior day health program?
No = 1, Yes = 2
(5) In the past month, did you or CR have any visits to a physician and/or psychiatrist?
No = 1, Yes = 2

