V. Armstrong, M. Renaud
Corresponding author: Dr. Vickie Armstrong, DNP, RN, GNP-BC, 1000 Old Denbigh Blvd. Newport News VA 23601, vickie.armstrong@rivhs.com
Abstract
Objectives: The objective of this study was to evaluate the effect of Physician Order for Scope of Treatment (POST) orders on interdisciplinary staff caregiver satisfaction, hospital admissions and hospice enrollment. POST is a program that provides a vehicle for clear communication of an individual’s desires for EOLC care in a physician order to be honored across the continuum of care. The effect of POST orders on staff caregiver satisfaction, hospital admissions and hospice enrollment has not been published. Design: This study used a quasi-experimental pre-test/post-test design for a single group of participants to measure staff caregiver satisfaction change. Retrospective chart reviews for data collection for comparison to historical data for change of hospice enrollment and hospital admission. Setting: The study was conducted in nine nursing homes in Southeastern Virginia from August 1, 2013 to December 31, 2013. Participants: Participants were the interdisciplinary staff caregivers who cared for residents with POST orders. Intervention: Implementation of POST orders. Measurements: Pre and post POST order surveys that were completed by staff and retrospective chart reviews for evidence of hospice enrollment and hospital admission. Results: There was no demonstrated change in staff caregiver satisfaction (p=0.05). 86 charts with POST orders were reviewed. Hospice enrollment for residents with POST orders was 16.2% compared to 2.10% in 2013 and 1.68% in 2012 of nursing home residents without POST orders. Hospital admissions were 0% as compared to 2012 and 2013 hospital admission rates of 4.8% and 6.2% respectively. Conclusion: POST orders did not change staff caregiver satisfaction with EOLC, however there were significant changes in the rate of hospital admissions and utilization of hospice services. These results may provide basis for further examination and possibly dedication of resources for further development of Advance Care Planning Facilitator training. The ability to identify and communicate individual wishes for EOLC beneficially impacts the patient, family, caregivers and society; continued efforts in this arena are imperative.
Key words: POLST, end of life care, hospice, hospital admissions, staff satisfaction, advance care planning.
Introduction
End of Life Care (EOLC) frequently takes place in the nursing home setting, and it is known that there is need for improvement in this care (1). Many people have desires about their care in the setting of a life limiting illness or event, but too many times these desires are unknown or not communicated to family members or their healthcare providers. This can result in unwanted aggressive care that causes prolonged suffering and limits access to beneficial services such as hospice. Physician Orders for Life Sustaining Treatment (POLST) is a widely recognized program that helps to define and communicate an individual’s desires for EOLC in a recognized medical order that can transition across the continuum of care (2).
The Patient Self Determination Act (PSDA) started the awareness of choices as Advance Directives (AD), but since there was not a systematic method for recognition and translation of those wishes to medical orders that were portable across care settings, quality and cost of EOLC was unaffected. According to the Centers for Medicare and Medicaid Services (CMS) health care expenditures in 2010 for the elderly and disabled was $73 billion and estimated to continue rising; the costs associated with the last year of life total about 25% of total CMS costs (3), with no evidence that quality was improved. Costs of EOLC has been substantial since there currently are “…complex financial incentives for expensive services that are acute care oriented…..but does not pay for skin care or spoon feeding for stroke patients at home” (4).
Oregon Health and Sciences University recognized that the scope of the PSDA and AD was limited since there were no systematic processes to enact choices across the continuum of care. They developed the Physician Orders for Life Sustaining Treatment (POLST) program in 1991 to help patient’s desires follow them across different health care settings in the form of physician orders (5).
EOLC is experienced by all, since we all die. Self-determination of EOLC is a fundamental patient right. It is generally accepted that high quality EOLC is care that is patient centered, desired, and controls symptoms and pain. The IOM’s report Approaching Death: Improving Care at the End of Life states in part: “…proposed that people should be able to expect and achieve a decent or good death—one that is free from avoidable distress and suffering for patients, families, and caregivers; in general accord with patients’ and families’ wishes; and reasonably consistent with clinical, cultural, and ethical standards. A bad death is characterized by needless suffering, disregard for patient or family wishes or values, and a sense among participants or observers that norms of decency have been offended” (6).
Quality EOLC is also care that is cost effective; the presence of POST orders to communicate choices is significant since it implies recognition of nearing end of life and may result in earlier palliative care or hospice referral and enrollment which have been shown to reduce acute care hospitalizations and reduce overall cost while improving care (7).
The significance of cost effective care is becoming increasingly important since the Patient Protection and Affordable Care Act of 2010 and Accountable Care Organizations. Penalties for higher than expected hospital readmissions were effective October 1, 2012. Almost one in five Medicare beneficiaries returns to the hospital setting within thirty days of discharge (8) and with increased scrutiny and incentives to avoid readmissions health systems are monitoring this with increased interest. POLST has the potential to positively impact hospice enrollment and hospital readmission rates as well as improve the quality of EOLC.
Nursing home residents are of particular interest since historically nursing homes have “….a notable site of death….” (9) and this is expected to increase. Currently, 17% of all deaths in the U.S. occur in the nursing home setting (10) and when our country’s demographics are considered there is little to suggest that this will be reduced in the near future; in fact it is predicted that this will double by 2020. It is expected to increase to two out of five Americans will die in a nursing home (11).
Nursing homes are a unique setting in healthcare. Historically highly regulated, order processing in the nursing home has multiple steps and opportunities for delay and error. The process starts with approval of orders by the medical director, attending physician or advance practice provider. Many times orders from outside sources may not be recognized as valid since the attending physician frequently has changed during transitions of care and so then requires another approval. AD may have accompanied a resident that is newly admitted to the nursing home, but most facilities require physician orders to convert AD into an actionable plan of care and medical orders. Many times there is a lack of provider presence to execute this order on admission, creating an inconsistency of care that can result in repeated questioning of resident or family member to clarify choices.
The use of POLST orders is beginning to be utilized in Virginia; the acronym has been altered to POST-Physician Orders for Scope of Treatment (appendix A and B). This effort was started in 2006 by The Palliative Care Partnership in Roanoke, Virginia. Regional coalitions began pilot programs in cooperation with some of the major health care organizations in the state: The Medical Society of Virginia, the Virginia Department of Health, the Virginia Hospital and Healthcare Organization and the Virginia State Bar as well as healthcare systems. Trained Advance Care Planners (ACPs) facilitate the discussions with residents and families about their expectations and desires for an individual’s choices and assist with completion of POST orders (12).
The purpose of this study was threefold: to determine what effect POST orders had on the clinical staff that care for people at end of life in the nursing home setting when their wishes are clearly identified and communicated by POST orders, and if POST orders changed the rate of hospital admissions and enrollment in hospice.
Methods
Research Design
This study was a quasi-experimental pre-test/post-test design for a single group of participants to measure staff caregiver satisfaction change. Retrospective chart reviews for data collection was done for comparison of change in hospice enrollment and hospital admissions were compared to the organization’s historical data. Questionnaire was adapted from Friedman et al (19).
Study Sites
The study sites were nursing facilities in the Hampton Roads area of southeast Virginia. This was an ideal setting for this study since residents of the nursing facility matched the target population for Advance Care Planning and POST orders for this study.
Participants
Participants were nursing home residents with POST orders and their interdisciplinary staff caregivers. The study was limited to 100 English speaking participants who completed the electronic pre and post POST survey. This was an anonymous survey with minimal risk involved; anonymity and retrospective chart reviews provided adequate Human Subject Protection. IRB approval was obtained from Old Dominion University in Norfolk, Virginia as well as Riverside Health System Privacy Board Review.
Data Collection
Data was collected by chart review for presence of POST document, evidence of hospice referral and hospital admission.
Procedure
After IRB approval was obtained, information regarding the survey was given to the facility staff caregivers. They were given the opportunity to participate in the pre-POST survey (Appendix C) and the post-POST survey (Appendix D). The data from the first 100 pre and post POST surveys were entered in SPSS password protected database.
Enrollment
Interdisciplinary staff caregivers who met inclusion criteria included nurses, social workers, dietary and therapists were given the opportunity to participate in an anonymous survey. Recruitment was done with flyers providing participants instructions regarding accessing the survey by computer.
Randomization
No randomization was done due to study design.
Control Group
No control group was used due to study design, although historical data that was used for comparison of hospital transfers and hospice referral.
Intervention
The intervention was the implementation of POST orders.
Results
Data Analysis
Data analysis for this study was conducted using sums and percentages for nominal data to describe the frequency of the department and therefore the discipline of the participant. This data was collected during the electronic survey displayed in table 1.
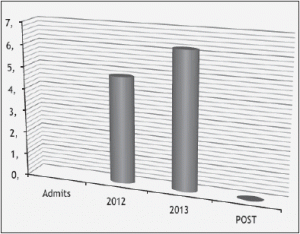
Demographic Data
Most of the participants were experienced staff; 50% reported ten years or more of experience in their discipline (Table 1). The majority of the participants in the survey were nursing staff; 23.3% were Registered Nurses, 20% were Licensed Practical Nurses, and 6.7% were Certified Nursing Assistants totaling fourteen nursing staff for total percentage of 50% of the participants. Other disciplines were 20% therapists, 6.7% social workers and 10% dietary workers as well as 13.3% unidentified nursing home workers participated in the survey.
Research Question One The results for research question one “Did the satisfaction and confidence of the clinical staff change after POST orders were implemented ?» are detailed in Table 2. N=30 which was suitable for parametric testing. The data was pooled into an aggregated data analysis using independent t-testing. There was no missing data. Evaluation by independent t-test did not show any statistically significant change in staff satisfaction or confidence in EOLC after POST orders were implemented.
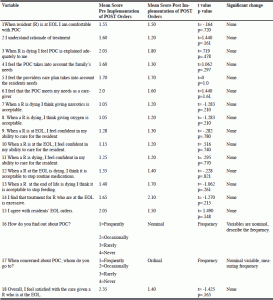
Table 2 Research Question One: Does the satisfaction and confidence of the clinical staff change after POST orders are enacted?
Research Question Two Results for the research question two: What effect did the presence of POST orders have on rate of hospital admission from the nursing home is shown in Table 3. The rate of hospitalization is dramatically reduced in the nursing home population that has POST orders implemented. Demonstrated rate was 0% which is significantly reduced from this organizations historical data that showed hospitalization rates of 4.8% in 2012 and 6.2% in 2013 in comparison to 0% hospital admission for residents with POST orders (Chart 1).

Table 3 Research Question Two: What effect does the presence of POST orders have on rate of hospital admission from the nursing home?

Table 4 Research Question Three: Is there a change in enrollment to hospice after the implementation of POST orders?
Research Question Three The results of the data analysis of research question three: “Was there a change in enrollment in hospice after the implementation of POST orders?” are shown below in Table 4. The current hospice enrollment rate for nursing home residents with POST orders demonstrated by this study was 16.2%. This was compared to the historical data of hospice utilization rate for nursing home residents in 2012 of 1.68% and 2.1% in 2013 (Chart 2).
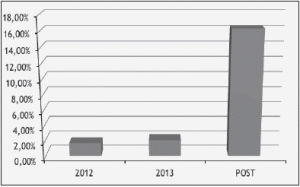
Figure 2 Comparison of Historical Hospice Utilization with Hospice Utilization for Residents with POST Orders
Discussion
The statistics for death in Virginia show that in 1997, 24.9% of people died at home and 21% of people died at a nursing home, but 54% died in a hospital. Other states have much higher incidence in hospital death, as high as 71.9% in the District of Columbia (13). The cost of hospital care at the end of life is burdensome to the patient and family both physically and financially and to society since taxpayers fund Medicare and Medicaid and are ultimately the end payer of healthcare services. Interventions that identify choices about EOLC may be able to positively impact quality and cost of care.
High quality EOLC with hospice services provides better care at lower costs; this was demonstrated in a study that compared Los Angeles and San Diego CA. End of Life inpatient hospital costs were shown to be 65% higher in Los Angeles as opposed to San Diego. Much of the cost differences were attributed to higher utilization of hospice services in San Diego and less time in hospitals and intensive care units during the final two years of life which resulted in lower costs (7).
The ability to know and respect what residents choices are regarding EOLC been discussed in the literature since 1990, but the systematic processes to convert the desires to a portable medical order has taken more time. Oregon Health and Science University developed POLST in 1991. This program has been adopted by many states, but it is neither nationwide, nor legislated and the programs are a various stages of maturity (14).
There are still gaps in EOLC in the nursing home; policy and payment changes that have changed focus to rehabilitation have had the unintended consequence of ignoring those at end of life or subjecting them to aggressive rehabilitation services (4).
Hospice services are growing, but there are systematic barriers to providing nursing home residents with hospice services (15, 16) staff lack of knowledge of the benefits of hospice services, staff and family perceptions that hospice care is redundant, and reimbursement that encourages facilities to encourage skilled nursing care in favor of hospice care that is paid for by Medicare Hospice benefits (11). Physician lack of knowledge of the benefits of hospice services, affordability, and difficulty in predicting the CMS mandated six month life expectancy are also barriers to optimal provision of hospice services that can improve the quality of EOLC (17).
The effect of POST orders on the staff caregiver satisfaction and impact on quality of care has not been well researched although there are known gaps in quality of EOLC. Studies show that a common theme voiced by nursing home staff is for more education to provide good EOLC (9). Other aspects of EOLC that have been studied and published are cultural and socioeconomic factors that influence end of life decision making have also been documented by previous studies (11, 18). Communication about the end of life plan of care has also been studied and found to be problematic due to ambiguity, accuracy and lack of agreement between physician and nurses. This have been cited as a barrier to quality EOLC as well as what types of treatments are to be provided to a resident at the end of life (19).
There is little known about how POST orders affect the interdisciplinary staff that provides day to day care for nursing home residents. This is the case even in states such as Washington and Oregon that were early adopters of POLST. Studies have demonstrated that hospice enrollment reduced costs of EOLC and improved the quality as measured by symptom control and pain management, but it is not demonstrated if POST orders changes staff perception and satisfaction of quality of EOLC or influences costs by increased hospice enrollment or decreased hospital admissions.
Limitations
Limitations of this study were small sample size and limited length of time for this study as well as the presence only of POST orders without further classification of the specifics of the orders. Further definition of the options on POST orders that were chosen was beyond the scope of this study. The POST program was new to the facilities and staff, so survey response may have been increased if the program had been mature.
This group of nursing homes is serviced by a long term care practice that is employed by the health system. There are physicians and nurse practitioners embedded in these facilities daily. This group also provides after hours call coverage and there is a robust EMR system that provides access to medical records. These factors may have an unknown impact on the historical data that was used for comparison for change.
Conclusion
The POST program has great potential to improve EOLC in the nursing home setting as well as impacting the cost of care at the end of life. Clear direction for care as provided by POST orders was shown to improve communication about choices for EOLC. This in turn lessened burden to residents and families and increased value by avoiding unwanted hospitalizations and increasing hospice utilization. The use of ACP facilitators and discussions about wishes for EOLC should be systematized so that every person with a life limiting illness is given the opportunity to express their wishes for EOLC and document those wishes. This should also provide improved access to services that are known to benefit patients at end of life.
Acknowledgements: The author wishes to extend a sincere thanks to the team of Riverside Health System’s division of Lifelong Health. Without them, this study would not have been possible.
Conflict of Interest: The authors declare no conflict of interest.
Ethical standards: This study was anonymous therefore an exempt study approved by Old Dominion University’s IRB and Riverside’s Privacy Board.
References
1. Meyers, J. L., Moore, C., Mc Grory, et al. Physician orders for life sustaining treatment form Honoring end of life directives for nursing home residents. J Gerontol Nurs. 2004; 30(9), 37-46.
2. Respecting Choices. (2013). http://respectingchoices.org/
3. Tilden, V. P., Nelson, C. A., Dunn, P. M., et al. Nursing’s perspective on improving communication about nursing home residents preferences for medical treatments at end of life. Nurs Outlook 2000; 2000 48, 109-115. http://dx.doi.org/doi:10.1067/mno.2000.100434
4. Tilden, V., & Thompson, S. Policy Issues in EOLC. J Prof Nurs 2009 25(6), 363-368.
5. Struglinski, S. (2008, December). POLST programs catching on. Provider 34(12), 21-22.
6. Field, M. J., & Cassel, C. Approaching death Improving care at the end of life. Retrieved from http://iom.edu/Reports/1998/Approaching-Death-Improving-Care-at-the-End-of-Life.aspx
7. Kaplan, R. Variation between end of life health care costs in Los Angeles and San Diego: why are they so different? J Pallat Med 2011; 14, 215-220. http://dx.doi.org/DOI: 10.1089/jpm.2010.0285
8. Rau, J. (2012). Medicare revises hospitals’ readmissions penalties. Retrieved from http://www.kaiserhealthnews.org/Stories/2012/October/03/medicare-revises-hospitals-readmissions-penalties.aspx
9. Zimmerman, S., Sloane, P. D., Hanson, L., et al. Staff perceptions of EOLC in long term care. J Am Med Dir Assoc; 2003, 23-26. http://dx.doi.org/10.1097/01.JAM.0000046935.64053.54
10. Brock, D. B., & Foley, D. J. Demography and epidemiology of dying in the US with emphasis on deaths of older persons. Hosp J; 1998;13(1-2):49-60.
11. Han, B., Tiggle, R. B., & Remsburg, R. E. Characteristics of patients receiving hospice care at home versus in nursing homes: results from the national home and hospice care survey and the national nursing home survey. Am J Hosp Palliat Care 2008; 24, 479-486. http://dx.doi.org/10.1177/1049909107305654
12. http://virginiapost.org/. Accessed on March 21, 2014.
13. Last Acts. (2002). Means to a better end: a report on dying in America today. Retrieved from Indiana University Perdue University: https://scholarworks.iupui.edu/handle/1805/722
14. POST program helps caregivers with end of life decisions. (2012). Retrieved from http://www.tidewaterems.org/index.php?option=com_content&view=article&id=1475:post-program-helps-caregivers-with-end-of-life-decisions&catid=149:news&Itemid=184
15. Jenull, B., & Brunner, E Death and dying in nursing home A burden on staff. J Appl Gerontol 2008; 27, 166-180. http://dx.doi.org/DOI: 10.1177/0733464807313404
16. Watson, J., Hockley, J., & Dewar, B. Barriers to implementing an integrated pathway for last days of life in nursing homes. Int J Palliat Nurs 2006; 5, 234-240.
17. Brickner, L., Scannell, K., Marquet, S., & Ackerson, L. Barriers to hospice care and referrals Survey of physicians knowledge attitudes and perceptions in a health maintenance organization. J Palliat Med 2004; 7, 411-418.
18. Munn, J., Dobbs, D., Meir, A., et al. The end of life experience in long term care Five themes identified from focus groups with residents family members and staff. Gerontologist 2008; 48, 485-494.
19. Friedman, S. L., Choueiri, R., & Gilmore, D. Staff carers’ understanding of EOLC. J Policy Pract Intellect Disabil 2008; 5(1), 56-64.
20. Institute of Medicine. (2011). The future of nursing: leading change, advancing health. Retrieved from http://www.nap.edu/catalog.php?record_id=12956