P. de Souto Barreto
Gérontopôle de Toulouse, Institut du Vieillissement, Centre Hospitalo-Universitaire de Toulouse (CHU Toulouse), Toulouse.Corresponding author: Dr. Philipe de Souto Barreto. Gérontopôle de Toulouse, Institut du Vieillissement. 37, Allées Jules Guesde. 31000 Toulouse, France, Telephone number: (+33) 561 145 668, Fax: (+33) 561 145 640, e-mail: philipebarreto81@yahoo.com.br
Experts in the field of nursing home (NH) research and clinical practice agree that non-pharmacological interventions must be a priority in institutional settings. As recommended by a panel of experts, and validated by the International Association of Gerontology and Geriatrics and the World Health Organization, it is important that “‘meaningful activities’ be offered to residents to provide physical and mental exercise and opportunities to participate within the nursing home and in community life, enhancing personal autonomy, social relationships (including intergenerational relationships), and social support” (1). Effective non-pharmacological interventions have the advantages of being low cost and low risk for older adults. This is a growing research field, with most studies examining the benefits of non-pharmacological interventions for residents with dementia (2-4), especially due to concerns raised by the use of potentially harmful drugs often used to treat/manage neuropsychiatric symptoms (5-8), or studying the effects of interventions on specific and widespread conditions, such as chronic pain (9), overall functional ability and mobility disability (10). One of the most widespread conditions among NH residents is related to a reduced functional ability (11-14), with more than 80% of residents having some degree of disability in executing activities of daily living (ADL) (12, 13). Mobility disability, as measured by the ability to walk a few meters, is a major issue in NHs: according with data from IQUARE (study performed in 175 French NHs, for a total of 6275 residents) (12), mobility disability reaches almost 70% of residents, with almost 40% needing human help to walk (12).
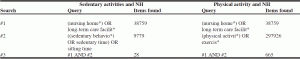
Table Results of PubMed search performed on April 22nd, 2014, about studies potentially developed in the nursing home setting on both sedentary and physical activities
Regarding non-pharmacological interventions to improve functional ability and reduce mobility disability in older adults, physical exercise is a well-established approach (15), including in people with dementia (16) and institutionalized older adults (10). Nevertheless, less attention has been paid to the adverse effects of sedentary time, a component of a physically active behavior, on function and mobility in the institutionalized elderly. Sedentary activities are defined as activities performed during waking hours that do not increase energy expenditure above 1.5 metabolic equivalents (17), which according with the recently updated Compendium of physical activities (18, 19) can be illustrated by activities such as sitting and/or lying down for watching television, listening to music, reading or talking on the phone. However, to the best of our knowledge no study has examined the effects of sedentary behaviors in predicting future physical function and mobility, even though sedentary behaviors have been found to be associated with the risk of type 2 diabetes (20), cardiovascular disease (20) and mortality (20, 21) in the general population. This research gap could explain why the time spent in sedentary activities has almost never been investigated in the NH setting. The Table below shows the results of a quick search in PubMed that retrieved studies investigating both sedentary and physical activities that have potentially been developed in NHs: whereas more than six hundred titles have been retrieved for physical activity, only less than thirty have been for sedentary activities.
Moreover, from the 28 articles retrieved for the sedentary activities search, only two (22, 23) were performed in NHs and really assessed and reported a measure of sedentary activity. In these studies, Chin A Paw et al. (22) found that residents spent more than 8 hours per day sitting (which represented around 77% of the total time evaluated by those researchers), and Ikezoe et al. (23) showed that residents spent 74.3% of their time in sitting or lying activities. Therefore, there is preliminary evidence showing that NH residents who are still able to stand up and ambulate independently (with or without walking-aids) spent around three-quarters of their waking time in sedentary activities.
Is sedentary behavior a useful outcome to be targeted in the NH setting?
Although there is no definitive, evidence-based, response to this question (since no study has examined the effects of reducing the time spent in sedentary activities on health outcomes (particularly functional ability and mobility disability) in the NH population), there is limited evidence indicating that breaking sedentary time could improve function in NH residents (24). Indeed, Slaughter and Estabrooks (24) recently found, in a preliminary study developed in two NHs (n=26), that residents’ performance in sit-to-stand activity improved functional fitness as measured by the 30-seconds chair rise test. The intervention introduced by these authors consisted in asking NH staff to encourage residents to stand up and sit down as many times as possible on two occasions each day and evening shift; therefore, this intervention is better defined as an intervention to break sedentary time more than a structured exercise program. Although one could argue about the safety of this activity, since standing slowly and sitting (alongside walking forward) are the main causes of falls in long-term care facilities (25), Slaughter and Estabrooks (24) found that no falls occurred during the execution of the sit-to-stand activity.
Perspectives
Breaking the time NH residents who are still able to stand up and ambulate a few meters may potentially slow down the progression of mobility disability. Breaking sedentary time could be used as an intervention to potentiate the positive effects of an exercise program; this intervention could also be focused in residents who do not wish to participate in structured exercise classes. This is a promising research field, since breaking sedentary time is less physically demanding than participating in exercise classes; therefore, although it is probably less effective than exercise to maintain physical function and mobility, it has the advantage to be easier to adopt and maybe adhere in a long-term basis to the vulnerable population of NH residents. Further research is, therefore, needed to establish the effectiveness and safety of interventions aiming to break sedentary time; integrating such an intervention in the routine care in NHs would facilitate its implementation in a long-term basis.
References
1. Tolson D, Rolland Y, Andrieu S, Aquino J-P, Beard J, Benetos A, et al. International Association of Gerontology and Geriatrics: a global agenda for clinical research and quality of care in nursing homes. J Am Med Dir Assoc. 2011;12(3):184-189.
2. Konno R, Kang HS, Makimoto K. A best-evidence review of intervention studies for minimizing resistance-to-care behaviours for older adults with dementia in nursing homes. J Adv Nurs. 2014. In Press. doi: 10.1111/jan.12432
3. Kales HC, Gitlin LN, Lyketsos CG, Detroit Expert Panel on the Assessment and Management of the Neuropsychiatric Symptoms of Dementia. Management of neuropsychiatric symptoms of dementia in clinical settings: recommendations from a multidisciplinary expert panel. J Am Geriatr Soc. 2014;62(4):762-769.
4. Kolanowski A, Resnick B, Beck C, Grady P. Commentary on the State of the Science in Gerontological Nursing: Advances in Non-Pharmacological Interventions during 2011-2012. Res Gerontol Nurs. 2013;6(1):5-8.
5. Seitz DP, Gill SS, Herrmann N, Brisbin S, Rapoport MJ, Rines J, et al. Pharmacological treatments for neuropsychiatric symptoms of dementia in long-term care: a systematic review. Int Psychogeriatr 2013; 25: 185–203.
6. Schneider LS, Dagerman KS, Insel P. Risk of death with atypical antipsychotic drug treatment for dementia: meta-analysis of randomized placebo-controlled trials. JAMA 2005; 294: 1934–43.
7. Ballard C, Hanney ML, Theodoulou M, Douglas S, McShane R, Kossakowski K, et al. The dementia antipsychotic withdrawal trial (DART-AD): long-term follow-up of a randomised placebo-controlled trial. Lancet Neurol 2009; 8: 151–7.
8. Richter T, Meyer G, Möhler R, Köpke S. Psychosocial interventions for reducing antipsychotic medication in care home residents. Cochrane Database Syst Rev. 2012;12:CD008634.
9. Tse MMY, Tang SK, Wan VTC, Vong SKS. The Effectiveness of Physical Exercise Training in Pain, Mobility, and Psychological Well-being of Older Persons Living in Nursing Homes. Pain Manag Nurs Off J Am Soc Pain Manag Nurses. 2013. In Press. doi: 10.1016/j.pmn.2013.08.003
10. Crocker T, Forster A, Young J, Brown L, Ozer S, Smith J, et al. Physical rehabilitation for older people in long-term care. Cochrane Database Syst Rev. 2013;2:CD004294.
11. Rolland Y, Abellan van Kan G, Hermabessiere S, Gerard S, Guyonnet Gillette S, Vellas B. Descriptive study of nursing home residents from the REHPA network. J Nutr Health Aging. 2009;13(8):679-683.
12. De Souto Barreto P, Lapeyre-Mestre M, Mathieu C, Piau C, Bouget C, Cayla F, et al. A multicentric individually-tailored controlled trial of education and professional support to nursing home staff: research protocol and baseline data of the IQUARE study. J Nutr Health Aging. 2013;17(2):173-178.
13. Onder G, Carpenter I, Finne-Soveri H, Gindin J, Frijters D, Henrard JC, et al. Assessment of nursing home residents in Europe: the Services and Health for Elderly in Long TERm care (SHELTER) study. BMC Health Serv Res. 2012;12:5.
14. Rolland Y, Andrieu S, Crochard A, Goni S, Hein C, Vellas B. Psychotropic drug consumption at admission and discharge of nursing home residents. J Am Med Dir Assoc. 2012;13(4):407.e7-12.
15. Chou C-H, Hwang C-L, Wu Y-T. Effect of exercise on physical function, daily living activities, and quality of life in the frail older adults: a meta-analysis. Arch Phys Med Rehabil. 2012;93(2):237-244.
16. Forbes D, Thiessen EJ, Blake CM, Forbes SC, Forbes S. Exercise programs for people with dementia. Cochrane Database Syst Rev. 2013;12:CD006489
17. Shuval K, Dipietro L, Skinner CS, Barlow CE, Morrow J, Goldsteen R, et al. « Sedentary behaviour counselling »: the next step in lifestyle counselling in primary care; pilot findings from the Rapid Assessment Disuse Index (RADI) study. Br J Sports Med. 2012. In Press. doi:10.1136/bjsports-2012-091357
18. Ainsworth BE, Haskell WL, Herrmann SD, Meckes N, Bassett DR Jr, Tudor-Locke C, et al. 2011 Compendium of Physical Activities: a second update of codes and MET values. Med Sci Sports Exerc. 2011;43(8):1575-1581.
19. Ainsworth BE, Haskell WL, Herrmann SD, Meckes N, Bassett Jr DR, Tudor-Locke C, Greer JL, Vezina J, Whitt-Glover MC, Leon AS. The Compendium of Physical Activities Tracking Guide. Healthy Lifestyles Research Center, College of Nursing & Health Innovation, Arizona State University. Retrieved [date] from the World Wide Web. https://sites.google.com/site/compendiumofphysicalactivities/
20. Grøntved A, Hu FB. Television viewing and risk of type 2 diabetes, cardiovascular disease, and all-cause mortality: a meta-analysis. JAMA J Am Med Assoc. 15 juin 2011;305(23):2448-2455.
21. Van der Ploeg HP, Chey T, Korda RJ, Banks E, Bauman A. Sitting time and all-cause mortality risk in 222 497 Australian adults. Arch Intern Med. 26 mars 2012;172(6):494-500.
22. Chin A Paw MJM, van Poppel MNM, van Mechelen W. Effects of resistance and functional-skills training on habitual activity and constipation among older adults living in long-term care facilities: a randomized controlled trial. BMC Geriatr. 2006;6:9.
23. Ikezoe T, Asakawa Y, Shima H, Kishibuchi K, Ichihashi N. Daytime physical activity patterns and physical fitness in institutionalized elderly women: an exploratory study. Arch Gerontol Geriatr. oct 2013;57(2):221-225.
24. Slaughter SE, Estabrooks CA. Optimizing the mobility of residents with dementia: a pilot study promoting healthcare aide uptake of a simple mobility innovation in diverse nursing home settings. BMC Geriatr. 2013;13:110.
25. Robinovitch SN, Feldman F, Yang Y, Schonnop R, Leung PM, Sarraf T, et al. Video capture of the circumstances of falls in elderly people residing in long-term care: an observational study. Lancet. 2013;381(9860):47-54
