P. Quail1, S.a. Ahmed1, M. Shaw1, S. Parry2, M. Hofmeister1, N. Drummond3
1. Department of Family Medicine, University of Calgary, Faculty of Medicine, Health Sciences Centre Foothills Campus, Calgary, Alberta, Canada; 2. Intercare Corporate Group, , Calgary, Alberta,Canada; 3. Department of Family Medicine, University of Alberta, Edmonton, Alberta, Canada.
Corresponding author: Marta Shaw, Department of Family Medicine, University of Calgary, Faculty of Medicine, Health Sciences Centre Foothills Campus, 3330 Hospital Drive NW | Calgary, Alberta, T2N 4N1. Canada, marta.shaw@ucalgary.ca
Abstract
Objectives: To implement and evaluate a targeted training initiative for care aides with the aim of improving recognition and reporting of early symptoms of Nursing Home Acquired Pneumonia (NHAP) and Urinary Tract Infection (UTI). Design: Pre-post, non-randomized, intervention trial design with care aides and residents. Setting: Three long-term care facilities: one site implemented the intervention and two maintained normal practices and procedures. Intervention: A nurse-led educational intervention and tool kit were delivered to health care aides to improve recognition and reporting of subtle behavioral or physiological changes in residents, which may be indicative of NHAP and UTI. Measurements: Paired t-tests were used to compare scores on questionnaires completed by care aides at baseline, immediately post-intervention and 3 months later, to identify their knowledge of UTI and NHAP symptoms, their perceptions of the professional relationships between care aides and members of other professions, and on workload. Resident charts were also reviewed. Results: Significant changes in NHAP symptom recognition were found for the intervention group between baseline (M = 2.45, SD = 1.18) and the three month follow-up (M = 2.94, SD = 1.34); t(31) = -2.05, p = .049. There was a significant increase in UTI symptom recognition scores for the intervention group between baseline (M = 2.20, SD = 1.18), immediately post-intervention (M = 2.80, SD = 1.05); t(35) = -3.34, p = .002 and after three months (M = 3.88, SD = 1.83); t(25) = -3.73, p = .001. Conclusion: A simple and inexpensive educational intervention among care aides may improve their recognition of UTI symptoms in residents in LTC.
Key words: Ageing, seniors’ health, gerontology, geriatrics, training.
Introduction
Nursing home acquired pneumonia (NHAP)
Long-term care (LTC) residents with cognitive impairment coPneumonia is the leading cause of death among nursing home residents (1) and the second most common infection (2) with reported incidences of between 0.3 and 2.5 episodes per 1000 resident care days (3). In patients over 75 years old, the case mortality is as high as 57% (4). What primarily distinguishes NHAP from community-acquired pneumonia is this higher mortality (5) The diagnosis of NHAP is often delayed due to possible absence of fever and cough, as well as changes in mental status (delirium), which further contributes to the high morbidity and mortality (6). Timely detection and treatment of NHAP is essential for improving outcomes, but can be challenging among LTC residents, who may suffer from cognitive deficits, impairing their ability to communicate.
Urinary tract infections (UTIs)
UTIs are the most common infection in long term care and source of acute hospital transfers (LTC) (7), with prevalence estimated to be between 5% and 10% and incidence of 2.6 to 9.5 per 1000 resident days (8). UTIs can be difficult to identify among higher need patients as clinical presentation in the LTC population is varied and often non-specific, resulting in common misdiagnosis (9, 10). Management of UTI in LTC has been identified as a key priority in quality assurance and performance improvement processes (11).
Health Care Aides (HCA), who contribute 80-90% of all care to residents in nursing homes, can relieve professional nurses of job stress and work overload, as well as improving patient health outcomes (12). Improvements in protocol implementation related to earlier case identification, may result from engaging HCAs in the process, alongside Licensed Practical Nurses (LPN). Previous studies have reported the effectiveness of low-intensity educational initiatives for HCA in improving outcomes of pressure ulcers (13), oral health (14), functional care for the elderly (15), urinary incontinence (16), and activities of daily living (17).
In order to enhance HCA knowledge of NHAP and UTIs and improve LTC resident outcomes through earlier recognition of change in condition, we implemented and evaluated a targeted training initiative in which an LPN provided informal, face-to-face education for HCAs with the aim of improving recognition and reporting of early symptoms of NHAP and UTI.
This study aimed to answer the following questions: How does the educational intervention impact HCA knowledge of NHAP and UTIs? What is the impact of the intervention on professional relationships between HCAs and LPNs?
Methods
We utilized a pre-post, non-randomized, intervention trial design with HCAs and residents at three, comparable, long-term care facilities in Calgary, of which one site implemented the intervention and two maintained normal practices and procedures. The sites were not randomized as 85% of HCAs work exclusively at one site. Consequently, the likelihood of cross-contamination was considered to be low. Resident recruitment was based on strategies used by Slaughter (18). Residents were recruited by LTC staff. The researchers obtained informed consent to review medical charts from residents, or surrogate decision-makers. HCAs were employed by the LTC organization for the full duration of the study and were invited to consent to participate in the study by the research associate. The University of Calgary Conjoint Health Research Board (CHREB) approved this research.
Educational Intervention
HCAs in the intervention site were educated in informal, small group sessions by the designated RN educator. HCA were also provided with an NHAP/UTI ‘toolkit’ to use in everyday practice (Appendix 1). Twenty-eight education sessions were offered on UTI, attended by one to eight HCAs. Twenty-five sessions offered on NHAP were also attended by one to eight HCAs ( average attendance by HCA was 3.5). Study participants attended only one session each for NHAP and UTI. Sessions varied from 10-30 minutes, depending on HCA interest in the topic and time considerations. Each session varied depending on topic of interest but could include information on 1) What is NHAP/UTI, 2) What is the significance of these illnesses in LTC, 3) The significance of these illnesses to caregivers in LTC, 4) Review of importance of prompt reporting of changes in patient condition. A review of symptoms from the toolkit was reviewed in each session. Material was presented through mini-lecture, discussion and/or a game. Sessions were timed during work shifts to maximize convenience and attract the greatest number of HCAs. The intervention period lasted 6 months.
Data Collection
Questionnaires were completed by HCAs at baseline, immediately post-intervention and 3 months later, to identify knowledge of UTI and NHAP symptoms, a 4-point Likert scale to measure their perceptions of the professional relationships between themselves and LPNs, and on workload. Residents’ charts were assessed for 1) incidence of NHAP/UTI, 2) transfers to hospital and length of stay in acute care, 3) death, 4) time to assessment by clinicians after onset of symptoms, 5) time to initiation of treatment.
Data Analysis
Number of identified symptoms, and scores for each item on the relationship and workload questionnaires were compared across the three time-points using paired t-tests.
Results
Rates of hospital transfer, length of stay and mortality were to low to include in the analysis. Response rate for the intervention group decreased between baseline (n=60) and immediately post-intervention (n=35) to 58.30%. Response rate at 3 months post-intervention (n=31) was at 51.70%. For the control group, response rate dropped between baseline (n=46) and immediately post intervention (n=37) to 80.40%. Response rate fell further at 3 months (n=30) to 65.20%. Of all HCA working in the intervention site, 44% volunteered to participate in the intervention.
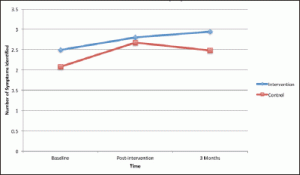
NHAP
Scores for NHAP symptom recognition in the intervention group were approaching significance between baseline (M = 2.49, SD = 1.10) and immediately post-intervention (M = 2.80, SD = 1.02); t(35)= -1.63. p = 0.11. There was a significant increase in NHAP symptom recognition scores for the control group between baseline (M = 2.08, SD = 1.25) and immediately post-intervention (M = 2.67, SD = .86); t(36)= -2.74. p = .009. Significant changes in NHAP symptom recognition were found for the intervention group between baseline (M = 2.45, SD = 1.18) and the three month follow-up (M = 2.94, SD = 1.34); t(31) = -2.05, p = .049 (Figure 1).
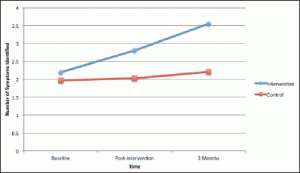
UTI
There was a significant increase in UTI symptom recognition scores for the intervention group between baseline (M = 2.20, SD = 1.18) and immediately post-intervention (M = 2.80, SD = 1.05); t(35) = -3.34, p = .002. There was also a significant increase in UTI symptom recognition scores for the intervention group between immediate post-intervention (M = 2.68, SD = 1.03) and after three months (M = 3.88, SD = 1.83); t(25) = -3.73, p = .001. There was no significant difference in scores for the control group (Figure 2).
Health Care Aide perceptions of relationship with LPN
There was a significant increase in HCA scores rating their relationship with the LPN with which they work between baseline (M = 3.12, SD =.48) and post-intervention (M = 3.35, SD =.49); t(34) = -2.26, p = 0.03, for ‘The LPN I work with respects my work’. There was a significant decrease in scores between post-intervention (M = 3.12, SD = .44) and three months later (M = 2.92, SD = .40); t(25) = 2.45, p = .02, for ‘The LPNs I work with trust me’. There was a significant decrease in scores between post-intervention (M = 3.04, SD = .61) to three months later (M = 2.88, SD = .60); t(25) = 2.14, p = .04, for ‘I trust the LPNs I work with’. There were no significant changes in scores for the control group.
Discussion
Findings from the study suggest HCA symptom recognition of UTI in LTC patients can be improved by a low-key, personal educational intervention delivered to complement HCA work schedules. A similar effect was not observed for NHAP, where both intervention and control groups recorded improvements in symptom recognition.
This was a small study of limited scope. Our response rate decreased at each time-point, possibly creating a self-selected population who participated in test two and three. We were not able to assess whether improvements in knowledge were associated with behavioural change among HCAs in relation to residents in whom symptoms were observed or other key outcomes such as hospital transfers and mortality. Our observational window was short and our sample sizes were small.
HCAs in the intervention group identified an increase in LPNs’ respect for them immediately after the intervention but this effect degraded by three months. This may be the result of LPNs temporarily recognizing HCA’ improved symptom knowledge, an appreciation which is subsequently normalized and discounted. Without objective validation (such as complementary data from LPNs themselves) it is unclear whether this perception was attributable to actual change in LPNs or was merely a halo effect in the perception of the care aides associated with participating in the intervention. HCAs reported that their trust in, and sense that they were trusted by, LPNs decreased between the intervention and three month follow-up. This may be attributed to HCA knowledge of UTI and NHAP concerns having been improved but little tangible recognition of the fact being observed among LPNs.
Our study indicates that a simple and inexpensive educational intervention among HCAs may improve their recognition of UTI symptoms in residents in LTC. This joins the growing body of evidence in support of the potential that these staff offer to improving the quality of care in long-term residential settings. Replication of this study in a larger number of sites over a longer observation period, with more rigorous assessment of care aides actual behaviours, with larger samples of residents and aides, is important to quantify the potential health gain associated with the intervention.
Conflict of interest: None of the authors has a conflict of interest.
Funding: This study was funded by the Intercare Foundation. The sponsors had no role in the design and conduct of the study; in the collection, analysis, and interpretation of data; in the preparation of the manuscript; or in the review or approval of the manuscript.
References
1. Muder RR. Management of nursing home-acquired pneumonia: unresolved issues and priorities for future investigation. Journal of the American Geriatrics Society 2000;48(1).
2. Mylotte JM. Nursing home-acquired pneumonia. Aging and Infectious Diseases 20002;35:1205-11.
3. Mylotte JM. Nursing home-associated pneumonia. Clin Geriatr Med 2007;23:553-565.
4. El-sohl AA, Sikka P, Ramadan F, Davies J. Etiology of severe pneumonia in the elderly. Am J Resp Crit Care Med 2001;163: 645-651.
5. Mylotte J. Nursing Home Acquired Pneumonia:Update on Treatment Options Drugs Ageing 2006;23(5); 377-390.
6. Janssens, JP. & Krause KH. Pneumonia in the very old. The Lancet infectious diseases 2004; 4(2); 112-124.
7. Nicolle LE. Urinary tract infections in long term-care facilities. Infect Control Hosp Epidemiol 2001;22:167-175.
8. O’Donnell JA, Hofmann MT. Urinary tract infections: how to manage nursing home patients with or without chronic catheterization. Infectious Disease 2002; 57(5).
9. Loeb M, Brazil K, Lohfeld L, McGeer A, et al. Optimizing antibiotics in residents of nursing homes: protocol of a randomized trial. BMC Health Services 2002;2:17.
10. Nace D, Drinka P, Crnich C. Clinical uncertainties in the approach to long term care residents with possible urinary tract infection. Journal of the American Medical Directors Association 2014; 15(2): 133-139.
11. Pennington K, Scott J, Magilvy K. The role of certified nursing assistants in the nursing home. JONA 2003; 33(11): 578-584
12. D’Agata E, Loeb MB, & Mitchell SL. Challenges Assessing Nursing Home Residents with Advanced Dementia for Suspected Urinary Tract Infections. Journal of the American Geriatrics Society 2013; 61(1): 62–66.
13. Howe L. Education and empowerment of the nursing assistant: validating their important role in skincare and pressure ulcer prevention and demonstrating productivity enhancement and cost savings. Adv Skin Wound Care 2008;21:275-81.
14. Boczko F, McKeon S, Sturkie D. Long-term care and oral health knowledge. JAMDA 2009;10:204-206.
15. Weitzel T, Robinson SB. A model of nursing assistant care to promote functional status in hospitalized elders. Journal for nurses in staff development 2004;20(4):181-186.
16. Beck C, Ortigara A, Mercer S, Shue V. Enabling and empowering certified nursing assistants for quality dementia care. International Journal of Geriatric Psychiatry 1999;14: 197-212.
17. Engelman KK, Altus DE, Mosier MC, Mathews RM. Brief training to promote the use of less intrusive prompts by nursing assistants in a dementia care unit. Journal of Applied Behavior Analysis 2003;36(1):129-132.
18. Slaughter, S.E. Incidence and predictors of excess disability among nursing home residents with middle-stage dementia: a prospective cohort study of functional transitions. Unpublished doctoral dissertation, University of Calgary, Alberta. 2008.