S. Jung1, V.R. Cimarolli2
1. Fordham University, Bronx, NY; 2. Jewish Home Lifecare, Research Institute on Aging, New York, NY. Corresponding author: Seojung Jung, MA, Fordham University, Department of Psychology, Dealy 226, 441 East Fordham Road, Bronx, NY 10458-9993, USA. E-mail address: sjung13@fordham.edu (S.Jung), Telephone: (917) 728-0971, Fax: (718) 817-3785
Abstract
Background: Recreational activities have the potential to improve nursing home residents’ quality of life, but little is known about the factors that are associated with the preferences that residents may voice regarding specific types of activities. Objectives: To identify personal, and health-related factors associated with recreational activity preferences in nursing home residents. Design: Cross-sectional study. Setting: An urban nursing home facility in the United States. Participants: Newly admitted, long-stay nursing home residents (N = 123). Measurements: Data obtained from residents’ admission Minimum Data Set (MDS) 3.0, including age, gender, race/ethnicity, marital status, subjective vision and hearing impairment ratings, cognitive functioning, depressive symptoms, and pain presence were examined as predictors of eight activity preferences items (i.e., having books, listening to music, participating in religious services) using multivariate logistic analyses. Results: In general, nursing home residents reported high preferences for most recreational activities. Vision and hearing impairments were significantly associated with vision-specific (reading) and hearing-specific activities (listening to music), respectively. Racial/ethnic minority residents were more likely to prefer group activities, keeping up with news, and religious practices, when compared to non-minority residents. Conclusions: Understanding activity preferences is a necessary first step in establishing and designing recreational programs that meet the needs of diverse populations in nursing homes.
Key words: Recreational activity, activity preferences, nursing home, Minimum Data Set, MDS 3.0.
Introduction
Recreational activities are ways of exposing nursing home residents to meaningful and pleasurable leisure experiences as well as engaging them in social interactions. Historically, as part of an effort to provide improved quality of care to nursing home residents, the Omnibus Budget Reconciliation Act of 1987 mandated that all nursing home facilities provide an “ongoing program of activities designed to meet, in accordance with the comprehensive assessment, the interests, and the mental, and psychosocial well-being of each resident” (1). Recreational activities provided by nursing home facilities typically include music, art, reading, writing, fitness, pet visits, and religious programs. Studies have shown that recreational activities have the potential to improve nursing home residents’ quality of life including benefits such as reduced anxiety, agitation (2, 3), depression (4, 5), and increased positive affect (6).
In order to plan for recreational activities that are meaningful and important to nursing home resident, it is imperative to assess residents’ preferences for activities. For that reason, the Minimum Data Set (MDS) – a federally mandated standardized assessment tool that is used with all nursing home residents in the US to ensure highest quality of care – includes a recreational activity preferences questionnaire. The most recent revision of the MDS (version 3.0) was implemented in October 2010. The main goal of the new version was to improve its clinical usefulness, with a focus on promoting resident-centered care (7, 8). One of the noteworthy changes in MDS 3.0 was that the Customary Routine and Activity items in MDS 2.0 were replaced by the Preference Assessment Tool (PAT), which specifically asks residents their preferences for daily support and care as well as for various recreational activities they consider important while they are in the facility (9). This concept of person-centered care reflected in the MDS 3.0 represents an opportunity to hear nursing home residents’ voices regarding their needs and preferences.
There is empirical evidence supporting that nursing home residents’ preferences for activities promote their engagement. Cohen-Mansfield and colleagues (10), for example, found that nursing home residents’ past and current preferences for an activity (e.g., music, art, pets) predicted their levels of engagement in the activity. This finding underscores the importance of understanding individual preferences for activities in care planning. However, given the vast differences in nursing home residents’ background, functional and cognitive limitations, and personal preferences, it is possible that activities provided by nursing home facilities may not meet the needs and interests of individual residents. For instance, one study found that nursing home residents with dementia received little or inappropriate activities (11). Hence, understanding the needs and preferences is the first step in planning for appropriate, meaningful, and effective activities (that is both individual and group activities).
Numerous studies have documented various factors influencing nursing home residents’ actual social and recreational participation, such as depression, cognitive impairment, vision and hearing impairment, and functional disability (12-16). However, little is known about personal and health-related factors (e.g., vision and hearing impairments) that are associated with the preferences that residents may voice regarding specific types of activities. Therefore, the aim of the current study was to explore the associations of person and health-related variables with eight distinct activity preferences assessed with the MDS 3.0 Preference Assessment Tool (PAT). We used the World Health Organization’s model of functioning, disability and health as a conceptual framework for including the most important factors (17). We, therefore, examined the unique contributions of personal (i.e., age, sex, race/ethnicity, marital status) and health-related factors (i.e., quality of vision and hearing, cognitive functioning, depressive symptoms, and pain) to preference reports of eight different recreational activities assessed via the MDS 3.0.
Methods
Participants
The study protocol was approved by two Institutional Review Boards and conducted at a geriatric healthcare organization based in New York City. All study data were retrospectively extracted from the MDS 3.0 admission assessment of the nursing home residents’ electronic medical record (EMR). Inclusion criteria for the current study were (1) newly admitted to the long-stay nursing care, and (2) having a completed Interview for Activity Preferences in the MDS 3.0. EMR of all residents who were newly admitted to an urban nursing home over a previous 18-month period were reviewed for the study. Of the 150 residents who were newly admitted during this period, we had to eliminate 27 residents who did not have a completed the Interview for Activity Preferences in the MDS. If the Interview for Activity Preferences is not completed, this means that based on staff’s judgment the resident was too cognitively impaired to answer the questions and a family member or significant other was not available to serve as a proxy respondent. The final sample consisted of 123 long-stay nursing home residents.
Measures
Personal Factors
Sociodemographic variables extracted included age, gender, ethnicity/race, and marital status. Gender was coded as 0 = male and 1 = female. Ethnicity/race was dichotomized as minority (1 = Black/African American, Hispanic/Latino, Asian) or non-minority (0 = White/Caucasians). Marital status was also dichotomized as 1 representing currently married and 0 representing not currently married.
Health-Related Factors
Level of hearing and vision impairment was rated by staff designated to complete the MDS assessment. Hearing is rated using a 4-point Likert scale (0 = adequate, 1 = minimal difficulty, 2 = moderate difficulty, 3 = highly impaired) and vision on a 5-point Likert scale (0 = adequate, 1 = impaired, 2 = moderately impaired, 3 = highly impaired, 4 = severely impaired).
Cognitive functioning was assessed by staff with the Brief Interview for Mental Status [18] (BIMS). The BIMS is a performance based cognitive screen that can be administered by nursing home staff. This screen consists of three sections; (a) repetition of three words, (b) temporal orientation, and (c) recall. The repetition of three words is assessed by asking residents to repeat the words after the evaluator said the three words. The number of words repeated after the first attempt is recorded. The temporal orientation section asks residents to report what year, month, and day of the week it is right now. The answer is coded as correct or incorrect, and the degree of the incorrect answer. The recall section asks residents to recall each of the three words that were used in the previous section on repetition of words. Residents’ answers were coded as 0 = no, 1 = yes, after cueing, or 2 = yes, no cue required. The summary score was used in the analysis and ranged from 0 to 15. Research has suggested that individuals with cognitive impairment are capable of expressing preferences and reliably answering questions about their preferences [19]. Cronbach’s alpha for the current sample was .87.
One-item from the Resident Mood Interview (PHQ-9) was used as an indicator of depressive symptoms. The item asks either residents or staff to report the extent to which the resident has been bothered by feeling down, depressed, or hopeless over the past 2 weeks, using a 4-point Likert type scale (0 = never or 1 day, 1 = 2-6 days, 2 = 7-11 days, 3 = 12-14 days). The item is identical for the resident and the staff version. We used a dichotomized variable with 1 representing «depressed» (2 or more days) and 0 representing «not depressed» (never or 1 day). One hundred and seven residents had a self-assessment and 16 a staff assessment (proxy assessment).
A single item of the Pain Assessment Interview was used as an indicator of the presence of pain. The items asks residents to rate the extent to which they had pain or hurting at any time in the last 5 days with yes (= 1) or no (= 0) answers.
Activity Preferences Outcomes
The MDS activity preferences section asks residents or a family or significant other to rate the importance of eight distinct recreational activities (i.e., “having books, newspapers, and magazines to read”; “listening to music you like”; “being around animals such as pets”; “keeping up with news”; “doing things with groups of people”; “doing your favorite activities”; “going outside to get fresh air when the weather is good”; “participating in religious services or practices”). Items are rated on a 4-point scale (1 = very important, 4 = not important at all) and an additional option is “important, but can’t do or no choice (= 5)”. One hundred eight residents answered the activity preference section by themselves (87.8%), and the remaining 15 residents’ answers were provided by their family or significant other (12.2%).
Statistical Analyses
First, we conducted descriptive analyses for all study variables followed by correlational analyses (not shown) to ensure that multicollinearity among study variables was not an issue. For descriptive statistics, including means and standard deviation, items were reverse coded; therefore high scores indicate high preference. Then, for subsequent multiple logistic regression analyses, preferences for activities were dichotomized into two groups, one comprised of residents who considered the activity as “very important/somewhat important/important but can’t do or no choice” (coded as 1), and the other comprised of those who considered the activity as “not very important/not important at all” (coded as 0). Logistic regression models (Odds Ratios (OR), 95% confidence intervals) were conducted to determine whether independent variables (personal and health-related factors) predicted nursing home residents’ preference for each activity item. In the final models, we left out a non-significant personal variable, marital status, in order to reduce the number of indicator variables. Because two items of activity preferences, “Do your favorite activities”, and “Go outside to get fresh when the weather is good”, had too few participants who considered them as not important (less than n = 10), further logistic analyses yielded no meaningful interpretation. Therefore, excluding these two outcomes, a total of six separate multiple logistic regression analyses were conducted with each activity preference item as a dependent variable. All data were analyzed using SPSS version 21.0.
Results
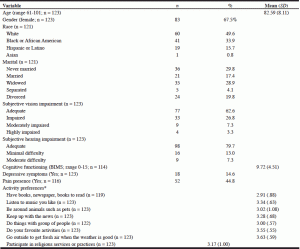
Descriptive statistics including means, standard deviation, and range scores for demographic and study variables are presented in Table 1. The participants were on average 83 years old with ages ranging from 61 to 101 years old and were primarily women (67.5%). About 50% of residents were members of minority groups, for example of Black/African American (33.9%) or Hispanic/Latino descent (15.7%). And about 30% of the participants were never married. Based on their BIMS score, 32% of residents’ cognitive functioning could be classified as intact/borderline, 32% had moderate cognitive impairments, and 36% were severely cognitively impaired. Ninety of 107 residents who self-rated symptoms of depression, and 15 out of 16 residents who had a proxy/staff rating of depressive symptoms had no symptoms of depression.
*Activity preferences average scores were computed after items were reverse coded (4 = very important, 3 = somewhat important, 2 = not very important, 1=not important at all) and exclude “important, but can’t do or no choic“. High scores indicate higher preference
The most preferred activity was “going outside to get fresh air when the weather is good“ (M = 3.63, SD = 0.59), followed by “doing favorite activities“(M = 3.55, SD = 0.55). Responses for “important, but can’t do or no choice“ were minimal. Only one resident chose this option for “do favorite activities” and four residents for “have books, newspapers, and magazines to read.”
Table 2 presents multiple logistic regression analyses of the relationship of independent variables and activity preferences, in which the activity preferences were dichotomized (important vs not important). For having books, magazine, and newspaper to read, vision impairment emerged as a significant predictor, indicating that a higher degree of vision impairment was associated with a decrease in preference for this activity (OR = .52, p < .05). Age and hearing impairment were significantly associated with listening to music residents like (OR = 1.11, p < .05; OR = .26, p < .05, respectively), indicating that older residents were more likely to prefer listening to music they like, while residents with more hearing impairment were less likely to prefer this activity. For being around animals such as pets, none of the predictor variables were significant. Being a racial/ethnic minority was associated with increased levels of preferences for keeping up with the news (OR = 6.17,
p < .05), doing things with a group of people (OR = 3.63,
p < .05), and participating in religious services or practices (OR = 20.09, p < .001). Cognitive functioning, depression, and pain presence were not significantly related to any of the six activity preference outcomes.
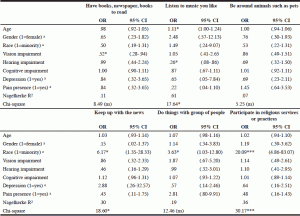
Table 2 Multiple Logistic Regression (Enter Method) Predicting Activity Preferences (1 = important, 0 = not important) (N = 123)
OR, Odds Ratios; CI, confidence interval; aReference groups were male (= 0), non-minority (= 0), not currently married (never married, separated, widowed, divorced = 0), no depression (= 0), no pain presence (= 0); *p < .05. **p < .01. ***p < .001; Note: Three models using the enter method presented in the table were not significant; however, the forward selection (likelihood-ratio) method, which enters independent variables one at a time using the likelihood-ratio for variable selection, yielded 5 out of 6 models statistically reliable to distinguishing the dependent variable, with the exception of the model predicting ‘being around animals such as pets’. This method, however, did not change the overall pattern of significance of the predictors; therefore, we only presented the full logistic model using the enter method.
Discussion
This study examined personal and health-related factors associated with long-stay nursing home residents’ preferences for various recreational activities using MDS 3.0 data. First, our findings provided an overview of patterns of residents’ preferred activities suggesting that in general nursing home residents place a high value on various recreational activities. The majority of residents considered most of the listed activities as important, particularly with regard to doing favorite activities and going outside to get fresh air when the weather is good. High preference levels for these two activity items were obtained from almost all nursing home residents regardless of personal and health-related factors. This finding demonstrates the importance of understanding the needs for activities in general and providing these options to all nursing home residents. In practice, scheduling for outdoor activities or providing areas for residents to get fresh air is not as routinely done as it should be (20). However, providing these types of activities is imperative given its benefits for improving residents’ quality of life as well as promoting person-centered care in nursing homes.
Also, our findings suggest that sensory impairments are related to importance of activity preferences. Vision impairment was associated with placing less importance on vision-specific activities (reading), and hearing impairment was related to placing less importance on hearing-specific activities (listening to music). Hence, therapeutic recreation specialists working with nursing home residents need to be aware of sensory impairments that may influence residents’ reports of preferences for certain activities. Upon discussion with a resident with sensory impairments, alternate formats for reading (e.g., talking books) can be offered to residents who may still be interested in re-engaging in an activity that they may have been important to them in the past and that they gave up because of the sensory impairment.
Previous studies have shown that visually impaired residents engage in less social and recreational activities, and exhibit more depressive symptoms (14). Lamoureux and colleagues (21), for example, found that vision impairment affects reading, hobbies, and social interaction. Our findings, however, suggested that nursing home residents’ vision impairment does not affect their preferences for most recreational activities, with the exception of reading. Similarly, although our study showed that those with higher hearing impairment were less likely to prefer hearing-specific activity (listening to music they like), hearing impairment was not a significant predictor for preferences of other activities, including having books, newspaper, books to read, being around animals, keeping up with news, doing things with group of people, and participating in religious services. Given that previous studies support that vision and hearing impairments become a barrier for residents’ participation in a wide range of activities, which in turn contribute to poor mood and loneliness (14, 22, 23), future studies should investigate whether poor mental health (i.e., depression, loneliness, poor mood) in residents with sensory impairments is influenced by the discrepancy between their preferences and actual participation in recreational activities.
Although previous studies reported that cognitive functioning predicts nursing home residents’ limited participation and engagement in activities (12, 15, 16), our findings indicated that despite cognitive difficulties, residents can still report their preferences for activities.
We also found that racial/ethnic minority residents were more likely than non-minority to prefer keeping up with the news, doing things with groups of people, and participating in religious services or practices. Minority residents’ values and interests in group activities may be shaped by their cultural orientation which tends to emphasize collectivistic values, such as relationships and group goals, unlike Western society which emphasizes independence and autonomy (24). Minority residents’ preference for religious services is also consistent with the previous literature showing that religious activities and spirituality play a prominent role in many African American and Mexican American older adults (25-28). It is not surprising that minority residents exhibited a higher desire to keep up with the news, given that these older minority residents may have experienced racism and inequalities throughout their lives. Staying informed about the current news may be a way of exercising their power and agency (29). Given that the proportion of minority older adults is increasing in the US, understanding the meaning of religious activities and preparing culturally and ethnically appropriate activities options for these populations is prominent. To further advance our understanding of minority residents’ preferences for recreational activities, development and use of more in-depth assessment of activity preferences in addition to the MDS is required (30).
Several limitations of the present study should be noted. First, our study was cross-sectional in nature, which limits causal inferences regarding our study variables. Secondly, the participants were drawn from a nursing home facility located in New York City, a highly dense urban area. Hence, our sample may not be representative of the nation and may differ from nursing home residents in rural or suburban areas; therefore, generalization of our results to other nursing home residents should be made with caution. Third, some assessments of preferred activities and of health-related variables relied on proxy ratings (e.g., ratings of staff). Moreover, we did not include educational level as a predictor variable as this information is not available in the MDS. Education is a factor likely influencing activity preferences. In addition, our sample size was relatively small. Thus, lack of significant associations may have been due to inadequate power to detect all significant associations. Lastly, the recreational activities listed in MDS is limited to eight items, and the use of a more comprehensive activity list including art, writing, movies, and fitness may provide more insightful information.
Despite its limitations, this study is one of the first studies that examined various factors related to long-stay nursing home residents’ recreational activity preferences using the section F of MDS. One of the important implications is that our findings demonstrate the utility of MDS data for nursing home staff to incorporate individual residents’ voices when designing and planning activities.
Conclusions
Providing meaningful and preferred activities to nursing home residents is well reflected in the recent trend of person-centered care. Identifying what they prefer is the first step to designing and providing appropriate and meaningful activities and services for residents. The findings from the current study are important in understanding the factors that are associated with nursing home residents’ preferences for recreational activities. Residents place high importance on preferences for activities. Our findings suggest that sensory impairments are related to nursing home residents’ preferences for certain activities. Furthermore, being of minority status played an important role with regard to preferring doing activities with group, keeping up with news, and religious practices. Addressing the unique needs and interests of this population is eminent. The study also supports the potential usefulness of the section F of the MDS 3.0 for individualized care planning, specifically in designing and planning recreational activities for newly admitted nursing home residents. Further research examining the changes of activity preferences over time and effects of discrepancy between activity preferences and actual participation should be warranted.
Funding: None.
Acknowledgements: The authors wish to thank Miriam Levi, Director of Community Life Activities, and the staff of the Therapeutic Recreation Department at Jewish Home Lifecare for their valuable discussions and support in carrying out this research. We also thank Dr. Joann P. Reinhardt for her comments on previous versions of this manuscript.
Ethical Standards: The study reported in this manuscript has been performed in accordance with the guidelines for the protection of the rights, welfare, and wellbeing of subjects involved in research as set forth by the Office for Human Research Protections of the U.S. Department of Health and Human Services.
References
1. Wiener JM, Freiman MP, Brown D, Henry J. Kaiser Family Foundation. Nursing Home Care Quality. 2007:1–53. Available at: http://scholar.google.com/scholar?q=related:ZYvIiw7dWdEJ:scholar.google.com/&hl=en&num=20&as_sdt=0,5.
2. Putman L, Wang JT. The Closing Group: Therapeutic Recreation for Nursing Home Residents with Dementia and Accompanying Agitation and/or Anxiety. Am J Alzheimers Dis Other Demen. 2007;22(3):167–175. doi:10.1177/1533317507300514.
3. Sung H-C, Chang AM, Lee W-L. A preferred music listening intervention to reduce anxiety in older adults with dementia in nursing homes. J Clin Nurs. 2010;19(7-8):1056–1064. doi:10.1111/j.1365-2702.2009.03016.x.
4. Buettner LL. AD-venture program: Therapeutic biking for the treatment of depression in long-term care residents with dementia. Am J Alzheimers Dis Other Demen. 2002;17(2):121–127. doi:10.1177/153331750201700205.
5. Meeks S, Looney SW, Van Haitsma K, Teri L. BE-ACTIV: a staff-assisted behavioral intervention for depression in nursing homes. Gerontologist. 2008;48(1):105–114.
6. Schreiner AS, Yamamoto E, Shiotani H. Positive affect among nursing home residents with Alzheimer’s dementia: The effect of recreational activity. Aging Ment Health. 2005;9(2):129–134. doi:10.1080/13607860412331336841.
7. Saliba D. Making the Investment Count: Revision of the Minimum Data Set for Nursing Homes, MDS 3.0. J Am Med Dir Assoc. 2012;13(7):602–610. doi:10.1016/j.jamda.2012.06.002.
8. Saliba D, Jones M, Streim J, Ouslander J, Berlowitz D, Buchanan J. Overview of significant changes in the Minimum Data Set for nursing homes version 3.0. J Am Med Dir Assoc. 2012;13(7):595–601. doi:10.1016/j.jamda.2012.06.001.
9. Simons K, Connolly RP, Bonifas R, et al. Psychosocial assessment of nursing home residents via MDS 3.0: Recommendations for social service training, staffing, and roles in interdisciplinary care. J Am Med Dir Assoc. 2012;13(2):190. e9–190. e15.
10. Cohen-Mansfield J, Thein K, Dakheel-Ali M, Marx MS. Engaging nursing home residents with dementia in activities: The effects of modeling, presentation order, time of day, and setting characteristics. Aging Ment Health. 2010;14(4):471–480. doi:10.1080/13607860903586102.
11. Buettner LL. Activity calendars for older adults with dementia: What you see is not what you get. Am J Alzheimers Dis Other Demen. 2003;18(4):215–226. doi:10.1177/153331750301800405.
12. Kolanowski A. Factors that relate to activity engagement in nursing home residents. Am J Alzheimers Dis Other Demen. 2006;21(1):15–22. doi:10.1177/153331750602100109.
13. Perlmutter MS, Bhorade A, Gordon M, Hollingsworth HH, Baum MC. Cognitive, Visual, Auditory, and Emotional Factors That Affect Participation in Older Adults. Am J Occup Ther. 2010;64(4):570–579. doi:10.5014/ajot.2010.09089.
14. Resnick HE, Fries BE, Verbrugge LM. Windows to their world: The effect of sensory impairments on social engagement and activity time in nursing home residents. J Gerontol B Psychol Sci Soc Sci. 1997;52(3):S135–S144.
15. Schroll M, Jónsson PV, Berg K, Sherwood S. An International Study of Social Engagement Among Nursing Home Residents. Age Ageing. 1997;26(suppl 2):55–59. doi:10.1093/ageing/26.suppl_2.55.
16. Voelkl JE, Fries BE, Galecki AT. Predictors of nursing home residents’ participation in activity programs. Gerontologist. 1995;35(1):44–51.
17. World Health Organization. International classification of functioning, disability and health: ICF. Geneva: World Health Organization; 2001.
18. Chodosh J, Edelen MO, Buchanan JL. Nursing home assessment of cognitive impairment: Development and testing of a brief instrument of mental status. J Am Geriatr Soc. 2008; 56:2069–2075.
19. Feinberg LF, Whitlatch CJ. Are persons with cognitive impairment able to state consistent choices? Gerontologist. 2001;41(3):374–382.
20. Cutler LJ, Kane RA. As great as all outdoors: A study of outdoor spaces as a neglected resource for nursing home residents. J Hous Elderly. 2006;19(3-4), 29-48.
21. Lamoureux EL, Fenwick E, Moore K, Klaic M, Borschmann K, Hill K. Impact of the Severity of Distance and Near-Vision Impairment on Depression and Vision-Specific Quality of Life in Older People Living in Residential Care. Invest Ophthalmol Vis Sci. 2009;50(9):4103–4109. doi:10.1167/iovs.08-3294.
22. Bookwala J, Lawson B. Poor Vision, Functioning, and Depressive Symptoms: A Test of the Activity Restriction Model. Gerontologist. 2011;51(6):798–808. doi:10.1093/geront/gnr051.
23. Brink P, Stones M. Examination of the relationship among hearing impairment, linguistic communication, mood, and social engagement of residents in complex continuing-care facilities. Gerontologist. 2007;47(5):633–641.
24. Singelis TM, Triandis HC, Bhawuk D. Horizontal and vertical dimensions of individualism and collectivism: A theoretical and measurement refinement. Cross Cult Res. 1995;29(3): 240-275.
25. Chatters LM, Taylor RJ, Bullard KM, Jackson JS. Race and ethnic differences in religious involvement: African Americans, Caribbean blacks and non-Hispanic whites. Ethn Racial Stud. 2009;32(7):1143–1163. doi:10.1080/01419870802334531.
26. Taylor RJ, Chatters LM, Jackson JS. Religious and spiritual involvement among older African Americans, Caribbean blacks, and non-Hispanic whites: Findings from the national survey of American life. J Gerontol B Psychol Sci Soc Sci. 2007;62(4):238-250.
27. Branco KJ. Religious Activities, Strength from Faith, and Social Functioning Among African American and White Nursing Home Residents. J Relig Spiritual Aging. 2007;19(4):3–20. doi:10.1300/J496v19n04_02.
28. Krause N, Bastida E. Church-Based Social Relationships, Belonging, and Health Among Older Mexican Americans. J Sci Study Relig. 2011;50(2):397–409.
29. Wray S. Women Growing Older: Agency, Ethnicity and Culture. Sociology. 2003;37(3):511–527. doi:10.1177/00380385030373007.
30. Van Haitsma K, Curyto K, Spector A, Towsley G, Kleban M, Carpenter B, … & Koren MJ. The preferences for everyday living inventory: Scale development and description of psychosocial preferences responses in community-dwelling elders. Gerontologist. 2013;53(4). 582-595.