S. Goorang1, L.U. Thorpe2, A. Baillod3, S.J. Whiting4
1. Quality of life in Long Term Care Study (Saskatoon site), College of Pharmacy and Nutrition, University of Saskatchewan; 2. Department of Community Health and Epidemiology, College of Medicine, University of Saskatchewan; 3. Department of Psychiatry, College of Medicine, University of Saskatchewan; 4. College of Pharmacy and Nutrition, University of Saskatchewan. Corresponding author: Lilian Thorpe, MD, PhD. Department of Community Health and Epidemiology, College of Medicine, 104 Clinic Place, Saskatoon, SK, S7N 2Z4, Canada; Phone: (306)966-7977 (alternate 306-655-7997), Fax: (306)966-7920, Email: lilian.thorpe@usask.ca
Abstract
Seniors residing in long-term care (LTC) facilities may suffer from nutrient deficiencies, yet supplementation may increase burden with little benefit, especially in advanced dementia with reduced life expectancy. A multidisciplinary team examined the clinical context and prescription of medications and dietary supplements to 29 LTC residents in the latest stages of dementia. All except one had problems with oral intake, and almost half had problems taking medications/supplements. The mean likelihood of death at 6 months was estimated to be 30%. Vitamin D and calcium were prescribed in 19 and 12 residents respectively. The mean (range) oral medication and supplement burden was 8.2 (0-20.5) and 1.4 (0-5) units per day, respectively, with clinical data frequently suggestive of potentially adverse outcomes. We recommend increased acquisition of knowledge and clinical expertise in the practical use of dietary supplementation in frail seniors, especially those in the latest stages of dementia.
Key words: Dietary supplements, nursing homes, older adults, dementia.
Introduction
Long-term care (LTC) residents with cognitive impairment commonly have malnutrition because of impaired absorption of nutrients, poor appetite, swallowing difficulties and poor compliance with nursing care. Unfortunately, supplementation may itself increase burden through polypharmacy and may increase mortality (1, 2). Excessive dosing and duplication of nutrients in several different dietary supplements may result in toxicity and drug interactions (3-5). Medications and supplements may have other specific adverse effects on frail individuals, such as constipation with calcium (6). Increased pill burden also increases stressful nursing interventions in residents with advanced cognitive impairment who may also have swallowing difficulties. This may contribute to increased agitation and aggression, use of psychotropic medications, and further decrease in quality of life. Finally, residents in the latest stages of dementia have limited life-expectancy (7, 8), so the lengthy times required for preventive benefit may reduce usefulness of supplementation.
Little information is available on the use of dietary supplements among LTC residents (9), especially those with cognitive impairment. We previously determined the prevalence of supplement use in LTC (10), but did not examine concomitant use of other medications or clinical context of individual participants. The aim of the current study was to assess the use of dietary supplements and medications in LTC residents in the latest stage of dementia, exploring clinical context and behavioural challenges, and assessing benefits and adverse effects.
Methods
Subjects and data collection
Appropriate ethics approval to access data was obtained from the University of Saskatchewan, Saskatoon Health Region and individual LTC facilities. Nurses on the four urban dementia units with secure dementia units in 2012 then identified residents with advanced dementia, FAST stage 7 (11). Chart data was abstracted by a senior psychiatry resident under the supervision of a geriatric psychiatrist and participants were left in the study if they still met entry criteria after this review. De-identified information was recorded, and included age, sex, medical history, diagnosis, level of functional impairment, functional health concerns, and use of prescribed agents (medications and dietary supplements). The term «agent» was used to designate a specific medication or dietary supplement type, and «unit» to indicate a discrete unit of administration, such as one tablet. This was done to facilitate separation of analysis into overall risks of polypharmacy compared to total burden of oral administration (which might have individual and nursing staff impact). For the purpose of this analysis we considered sodium and potassium ordered for the treatment of electrolyte disorders as medications rather than dietary supplements. Polypharmacy was defined as the regular concurrent prescription of five or more different types of agents. Estimated life expectancy was calculated from clinical information using methods published by Mitchell et al (12). Information was reviewed by a team with geriatric expertise including a primary care physician, pharmacist, geriatric psychiatrist, and two faculty members from the College of Pharmacy and Nutrition. Consensus decisions were made when possible about the likely benefits, adverse effects and appropriateness of each agent prescribed to individual residents.
Analysis
The analysis examined the total number and type of agents prescribed regularly as well as the total oral discrete unit intake counts (units included tablets, liquids or powders) resulting from these prescriptions. Agents not administered orally (such as intramuscular vitamin B12) were included in the types of agents prescribed but did not contribute to the oral intake unit count. Agents administered less than daily were prorated (i.e. a weekly administration schedule resulted in a daily agent fraction of 1/7 units). Sex differences and differences between supplement and non-supplement users were explored. The data were tabulated with means (± SD) and ranges. One-tailed t-tests were performed to examine sex differences in the total number of discrete units of oral agents prescribed as well as the oral medication burden. Statistical significance was set at P ≤ 0.05. We also examined the rate and profile of prescription of different types of vitamin and mineral supplements. Frequencies were explored by sex, supplement type and supplement users’ status.
We investigated the potentially inappropriate prescription of calcium supplements by exploring use in the absence of osteoporosis or previous fractures. Concurrent prescription of calcium and iron supplements (which both have constipating effects) with laxatives/stool softeners were correlated with individual reports of constipation. We also assessed the concomitant prescription of calcium supplements with thyroid hormone replacement and with diuretics.
Results
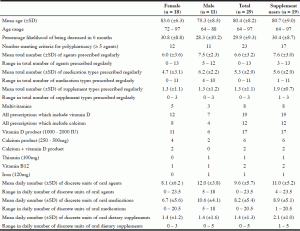
Twenty-nine participants were included in the study, 62% female and 38% male with a mean age of 80.4 years ranging from 64 to 97 (Table 1). Male participants were younger than females (75.3 ± 8.5 compared to 83.6 ± 6.3 years). Because of our selection of participants in the latest stages of dementia, overall functional impairment was marked. Oral intake or swallowing problems in all except one of the participants necessitated pureed/minced diets and crushing of orally administered agents (generally mixed into food). Seventeen participants had problems with agitation and ten were aggressive. Fourteen participants had resistance and/or aggression specifically related to medication or supplement administration.
The mean total daily number of regularly prescribed agents was 6.6 (±3.2) with a range of 0-13. Twenty-three participants met our definition of polypharmacy. Supplements included multivitamins, vitamin D, calcium, thiamin, vitamin B12, and iron. Nineteen participants were taking supplements and 13 were taking more than 1 supplement. Some agents were included in more than one formulation. Almost a third of supplement users (n = 6) were taking ≥ 3 supplements per day. All supplement users took vitamin D (n = 19) while 12 took calcium. Two participants received vitamin B12 separately, one intramuscularly and one orally.
The mean daily number of orally administered units of medication was 8.2 (±5.4) with a range of 0-20.5, and the corresponding rate for supplements was 1.4 (±1.3) with a range of 0 to 5. The combined oral burden (discrete units of oral medications and supplements) was 9.6 (±5.7) mean daily units ranging from 0 to 23.5. Males were prescribed significantly more daily oral units of medications than females (10.6 vs 6.7 units, P = 0.02), and had a higher total daily oral combined burden (12.0 vs 8.1, P = 0.03).
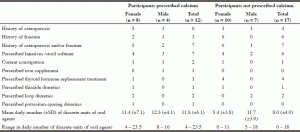
Calcium prescription and risk of adverse effects and interactions
Seven of 12 participants prescribed calcium and 7 of 17 not prescribed calcium had a history of osteoporosis and/or fractures (Table 2). More participants prescribed calcium used laxatives or stool softeners in comparison to those not prescribed calcium (7 of 12 compared to 6 of 17). Two participants prescribed calcium and 1 participant not prescribed calcium had difficulty with constipation despite being prescribed laxatives/stool softeners. Only one person had concurrent prescription of iron and calcium supplements. Three of twelve participants prescribed calcium (all female) were also prescribed diuretics and of these, one was prescribed two different types of diuretics. One participant prescribed calcium was also on thyroid hormone replacement.
Discussion
Our results from this small study were consistent with those of Vetrano et al (1) who found polypharmacy in more than 60% of nursing home residents with advanced cognitive impairment. Result were also consistent with results of our previous study (10) in which we demonstrated concurrent prescription of supplements and medications in all older adults in LTC.
There were a sizable number of participants receiving 3-5 supplements in addition to other medications. We worry particularly about the prescription of calcium in the absence of osteoporosis or fractures because of potential adverse effects. We also suspect that the high oral agent intake burden in our population was partially responsible for agitation, aggression and increased use of psychotropic medications, as nursing staff frequently identifies resistiveness during pill administration as a major concern. In spite of recent recommendations about the use of vitamin D in LTC as an important treatment for falls and fracture prevention (13, 14), only 17 of 29 (58%) participants were prescribed vitamin D as a separate supplement and 19 of 29 (65%) were prescribed vitamin D when all supplement sources were included.
Although this study was enriched by including detailed individual clinical information, the small sample size limited the use of statistical analysis and our ability to correlate oral agent burden with other outcomes. We also only assessed regularly prescribed medications, which would have missed some agents of importance. Lastly, if we overestimated the life expectancy of the residents, many medications with long time to benefit may have been even less useful.
Because of the increasing frailty of seniors in LTC, it is important to better understand the benefits and adverse effects of supplement use. Although general criteria exist to aid clinicians in making appropriate prescribing choices, clinical decision-making regarding supplementation is often complex and dependent on individual clinical context. We therefore believe that skilled professionals should be more available to LTC staff to help in this process. More knowledge also needs to be developed, particularly regarding the use of medications and supplements in the latest stages of dementia. Many interventions require a long time to benefit recipients (see Lee et al (15)) so more immediate adverse outcomes might not be warranted in those with short anticipated life expectancies.
Acknowledgments: We would like to acknowledge the help of Drs. Jane Richardson, Marla Davidson and Alina Cribb for their generous help and clinical expertise in the clinical review of our long-term care participants. We also thank the gracious help of many long-term care staff members (and their administrators) in helping us augment chart information with their clinical understanding when necessary. Lastly we thank our participants and their family members for allowing us to access their information for our research project.
Conflict of interest: Dr. Whiting reports a potential conflict of interest as she is on the Pfizer Consumer Healthcare Advisory Board.
Funding: Primary data was collected by a senior resident in psychiatry as part of her residency research project. Data analysis and the production of this publication was funded, in part, by the Saskatchewan Health Research Foundation.
Ethical Standards: Researchers complied with research standards mandated by the University of Saskatchewan Responsible Conduct of Research policy.
References
1. Vetrano DL, Tosato M, Colloca G, et al. Polypharmacy in nursing home residents with severe cognitive impairment: results from the SHELTER Study. Alzheimers Dement 2013;9:587-93. doi: 10.1016/j.jalz.2012.09.009
2. Onder G, Liperoti R, Foebel A, et al. Polypharmacy and mortality among nursing home residents with advanced cognitive impairment: results from the SHELTER study. J Am Med Dir Assoc 2013;14:450.e7-12. doi: 10.1016/j.jamda.2013.03.014
3. National Center for Complementary and Alternative Medicine (NCCAM). Using dietary supplements wisely. 2009. http://nccam.nih.gov/health/supplements/wiseuse.htm. Accessed 10 March 2014
4. Zamfirescu I, Carlson HE. Absorption of levothyroxine when coadministered with various calcium formulations. Thyroid 2011;21:483-6. doi: 10.1089/thy.2010.0296
5. Lim LS, Fink HA, Kuskowski MA, Cauley JA, Ensrud KE. Diuretic use and bone mineral density in older USA men: the osteoporotic fractures in men (MrOS) study. Age Ageing 2005;34:504-7. doi: 10.1093/ageing/afi133
6. Lewis JR, Zhu K, Prince RL. Adverse events from calcium supplementation: relationship to errors in myocardial infarction self-reporting in randomized controlled trials of calcium supplementation. Bone Miner Res 2012;27:719-22
7. Aminoff BZ, Adunsky A. Their last 6 months: suffering and survival of end-stage dementia patients. Age and Ageing 2006;35: 597–601
8. Mitchell SL, Teno JM, Kiely DK et al. The clinical course of advanced dementia. N Engl J Med 2009;361:1529-38. doi: 10.1056/NEJMoa0902234
9. Goorang S, Ausman L, Houser R, Whiting SJ. Profile of use of vitamin and mineral supplements among elderly institutionalized adults: A systematic review. J Nursing Home Res 2014; in press
10. Viveky N, Toffelmire L, Thorpe L, et al. Use of vitamin and mineral supplements in long-term care home residents. Appl Physiol Nutr Metab 2012;37:100-5. doi: 10.1139/h11-141
11. Reisberg B. Global measures: utility in defining and measuring treatment response in dementia. Int Psychogeriatr. 2007;19:421-56
12. Mitchell SL, Kiely DK, Hamel MB, Park PS, Morris JN, Fries BE. Estimating prognosis for nursing home residents with advanced dementia. JAMA 2004;291:2734-40
13. Wallis SJ, Campbell GA. Preventing falls and fractures in long-term care. Rev Clin Gerontol 2011;21:346-60. doi:10.1017/S0959259811000104
14. Rolland Y, de Souto Barreto P, Abellan Van Kan G, et al. Vitamin D supplementation in older adults: searching for specific guidelines in nursing homes. J Nutr Health Aging 2013;17:402-12. doi: 10.1007/s12603-013-0007-x
15. Lee SJ, Leipzig RM, Walter LC. Incorporating lag time to benefit into prevention decisions for older adults. JAMA 2013;310:2609-10. doi: 10.1001/jama.2013.282612