E. Gremeaux1, M. Grino2,3, C. Molines1, C. Oliver1,3, F. Retornaz1,4,5
1. Division of Geriatric Medicine, State Geriatric Centre, Marseille, France; 2. Inserm, UMR1062, « Nutrition, Obesity and Risk of Thrombosis », Medical School, Aix-Marseille University, Marseille, France; 3. Marseille’s Medical School, Aix-Marseille University, Marseille, France; 4. Department of Public Health, EA3279 Self-perceived Health Assessment Research Unit, Medical School, Aix-Marseille University, Marseille, France; 5. Department of Internal Medicine, European Hospital, Marseille. Corresponding author: Dr Charles Oliver, Division of Geriatric Medicine, State Geriatric Centre, 176 Avenue de Montolivet, 13012 Marseille, Tel: 04 91 12 75 49, Fax: 04 91 12 75 52, e-mail: charles.oliver30@orange.fr
Abstract
Abstract: Objectives: To examine the prevalence of blood lipid monitoring and statin use in secondary prevention of residents in southern French nursing homes for dependent elderly people. Design, Setting and Participants: Observational study in 12 southern French nursing homes for dependent old persons with coronary heart disease, ischemic stroke, peripheral artery disease or diabetes. Measurements: Collection from medical charts of blood lipid monitoring, LDL-C levels, statin use and geriatric assessment among 965 residents. Results: 410/965 residents were eligible for secondary prevention of atherosclerotic complications. Blood lipid was measured in 195 residents and lipid-lowering drugs were given to 106 (statin in 101). The rate of statin use was significantly reduced with increasing age and dependence severity. One third of residents under statin were not monitored for blood lipid. Conclusion: Blood lipid monitoring and statin use were subnormal in nursing home residents under secondary prevention. There is a need for prospective studies in this population and precise recommendations taking into account geriatric assessment criteria.
Key words: Atherosclerotic pathologies, secondary prevention, statin, nursing home.
Introduction
Atherosclerotic cardiovascular diseases are the major (63 %) cause of death in nursing home residents (1). Thus, efforts to reduce their incidence, recurrence and complications are important in such patients. There has been some controversy on the influence of cholesterol on atherosclerotic complications in very old persons, but it is now recognized that the absolute effects of cholesterol on annual ischemic heart mortality rates are much greater in older than in younger although its relative role in atherosclerotic diseases decreases with age (2, 3).
Statins are highly effective for reducing cardiovascular morbi-mortality as well as all-cause mortality in secondary prevention and in primary prevention of high risk adults (4). However, patients older than 75 years have been excluded from large randomized clinical trials (5). Lack of evidence, doubts about their benefits and concerns about their side effects have led to an underutilization of statin in this population. Actually, statin indication in older (6,7) and in nursing home is a matter of debate (8).
Residents in nursing home are a special subset of older people with high incidence of dependency, co-morbidities, poly-medications and limited life expectancy. It has been recommended that in secondary prevention statin prescription in older than 75 should be personalized and should take into account indices of geriatric assessment (9-11). The objectives of our observational study was (1) to evaluate the prevalence of statin treatment and lipid monitoring in secondary prevention (coronary heart disease [CHD]; ischemic stroke; peripheral artery disease [PAD] and diabetes) in southern French nursing home, (2) to study their association with geriatric assessment and physicians attitude.
Patients and methods
Study population
The study was approved by the Ethical Committee of the Departmental Geriatrics Center. The study population consisted of 965 residents living in 04 public and 08 private nursing homes in Marseille and its surroundings.
Data collection
Age, gender, geriatric assessment (GA), atherosclerotic vascular diseases (CHD, ischemic stroke, PAD), congestive heart failure (CHF), atrial fibrillation and diabetes data were collected from computerizedmedical charts. GA includes functional and cognitive status, mobility and polymedication. Functional status was assessed by the 1-6 «Autonomie Gerontologie Groupe Iso Ressources» (AGGIR) composite scale (12). This scale used in French geriatric setting as a proxy for dependency estimates the ability of old persons to perform cognitive and daily-life activities without the help of someone else. The residents were ranked in heavily (scores 1-2) or mildly (scores 3-4) functional dependent and independent (scores 5-6). Mini Mental State Examination (MMSE) was used to identify mild and severe cognitive impairment. Resident’s mobility was separated into normal (walking one block without help), limited (walking with stick or walker aid) and very limited (chair ridden). Polypharmacy (defined as four or more medications per day) was further separated into three classes: 4-6, 7-8 and ≥ 9. Glomerular filtration rate (GFR) was calculated using the Modification of Diet in Renal Disease equation. Moderate or severe renal insufficiency was diagnosed if the GFR was less than 60 or 30 ml/min/1.73 m² respectively. Nutritional status has been evaluated with body mass index (BMI), weight change over the last 1-6 month and serum albumin. Moderate undernutrition was defined by one of these indices: BMI ≤ 21, weight loss ≥ 5 % or 10 % during the last 1 or 6 months respectively or serum albumin ≤ 35 gram/liter. Severe undernutrition was defined by one of these criteria: BMI ≤ 18, weight loss ≥ 10 % or 15 % during the last 1 or 6 months respectively or serum albumin ≤ 30 gram/liter. Specific treatment for cardiovascular diseases including lipid lowering drugs, anti-platelets, anticoagulant and antihypertensive drugs were collected.
Questionnaire-based survey of physicians
Physicians in charge of nursing home residents completed a questionnaire on their attitude about statin prescription in secondary prevention including initiating or not and discontinuing this treatment. They were asked to give the reasons why they do not initiate or discontinue statin treatment: doubts on its benefits, on statin tolerance or other priorities, polypathology, polypharmacy.
Statistical analysis
Results are given as mean ± standard deviation (SD). Between groups comparisons were tested for statistical significance with the χ2 test for categorical variables and with the Mann-Whitney U test for continuous variables as appropriate. Statistical significance was determined at p < 0.05. Statistical analysis was performed with the Graph Pad Prism 5 software (La Jolla, CA).
Results
Characteristics of patients
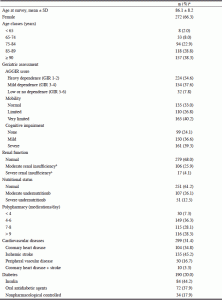
410 residents with atherosclerotic vascular diseases or diabetes were identified among the population of 965 residents (272 men and 693 women) from 04 public and 08 private nursing homes for dependent aged persons. They were separated into 138 men (mean age: 82.8 ± 9.7 years) and 272 women (mean age: 87.7 ± 6.9 years).
Atherosclerotic cardiovascular diseases and diabetes (table 1)
The prevalence of atherosclerotic cardiovascular diseases was 30.98 % (299/965 residents: 103 men and 196 women), separated into CHD (n=104), ischemic stroke (n=135), PAD (n= 50) and associated CHD -ischemic stroke (n=10). Residents with chronic atrial fibrillation (n= 86) and congestive heart failure (n=44) were not included in this group.
The prevalence of diabetes in the population of nursing homes participating in the study was 19.7 % (190/965 residents). The patients with diabetes were either insulin-treated (n=84), treated with oral antidiabetic agents (OAA, n=72) or without any antidiabetic medication (n= 34). Seventy-nine of these residents (39 insulin-treated, 26 OAA-treated and 14 without antidiabetic treatment) had an atherosclerotic pathology.
a. All data are presented as numbers (%) except when indicated otherwise; b. Some data were not available: 13 related to renal function and 2 related to nutrition status.
Geriatric assessment (table 1)
The majority of residents included in the survey showed a high degree of dependency as evidenced by the high percentage of residents with an 1-2 AGGIR score (54.6%), with a very limited mobility (40.2%) and with a severe cognitive impairment (39.3%). Residents displayed moderate renal insufficiency in 25.9 % of cases and severe renal insufficiency in 4.1 %. Moderate undernutrition was observed in 26.1 % and severe undernutrition in 12.5 %. Polymedication with 4 or more medications/day) was noticed in 92.7 % of residents; 28.1 % of them received 7-8 medications/day and 28.3 % received 9 or more medications/day.
Statin treatment
Lipid-lowering drugs including statin in 101 cases, fibrate in 3 cases, ezetimibe in 1 case and cholestyramine in 1 case were used in 106 residents. Atorvastatin and rosuvastatin were the most used statins. In the majority of residents, the intensity of statin was moderate: 5-10 mg for rosuvastatin, 10 mg for atorvastatin, 10-20 mg for simvastatin and 20-40 mg for pravastatin. Clinical and biological tolerance of statin was good in all cases: no increase in liver enzymes and creatine kinase (CK) levels were observed and no muscle complaints were recorded.
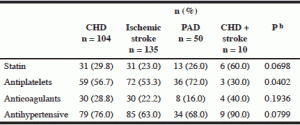
No significant difference was observed in statin prescription between CHD, ischemic stroke, PAD and the association CHD-ischemic stroke. Antiplatelets and antihypertensive drugs were significantly more used than statin (table 2). The majority of statin-treated residents (n= 101) were given antiplatelets (69/101; 68.3 %) or antihypertensive drugs (80/101; 79.2 %). The rate of statin use was similar in residents with diabetes than in residents with atherosclerotic diseases. Statin use was more frequent in insulin-treated (19/81; 23.5 %) than in OAA-treated (9/72; 12.5 %) and in non-treated residents (2/33; 6.1 %).
a. All data are presented as numbers (%). CHD: coronary heart disease; PAD: peripheral artery disease; b. P values for differences between pathologies were calculated using the χ2 test
A significant reduction in statin prescription was observed with increasing age (from 75 % in residents younger than 65 years old to 2Z % at 85-90 years and 16 % in older than 90. Similarly, statin was less used with increasing dependence as shown by the AGGIR score, very limited mobility and undernutrition. Statin prescription increases significantly and proportionally with polymedication rates. A moderate, but no significant reduction in statin use was observed in severe cognitive impairment and renal insufficiency (Table 3).
a. All data are presented as numbers (%); b. P values for differences between statin use or not were calculated using the χ2 test; c. Some data were not available: 13 related to renal function and 2 related to nutrition status.
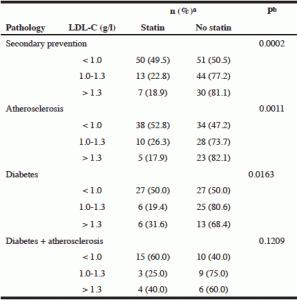
Blood lipid levels (table 4)
Blood lipid was measured in 195/410 residents (72/101 statin users). No lipid assay was available in 29/101 residents treated with statin. LDL-C levels lower than 1g/l were observed in 101 residents (50 statin users); LDL-C ranged between 1 and 1,3 g/l in 57 residents (13 statin users) while it was above 1.3g/l in 37 (7 statin users). LDL-C could not be calculated in 2 residents due to hypertriglyceridemia. LDL-C less than 1 g/l was significantly higher in residents treated with statin compared with those without statin (71.4 % vs 40.8 % in secondary prevention; 71.7 % vs 40 % in atherosclerotic cardiovascular diseases; 69.2 % vs 41.5 % in diabetes; 62.2 % vs 40 % in diabetes + atherosclerosis).
a. All data are presented as numbers (%); b. P values for differences between statin use or not were calculated using the χ2 test.
Factors affecting physician’s’ decision
Thirty-three physicians (in charge of 188/410 residents; 45.9 %) completed the questionnaire. 14/33 physicians did not initiate statin treatment for several reasons: polypathology (100 %), polypharmacy (92.9 %), doubt on its benefits (71.4 %) and tolerance (28.6 %). The underlying factors to the discontinuation of statin were: polypharmacy (78.8 %), polypathology (75.8 %), doubt on statin benefit (51.7 %) or tolerance (37.9 %).
Discussion
Our results show that the prevalence of cardiovascular diseases and diabetes are high as already reported in the literature. In the present study, only one-fourth of the residents in secondary prevention were treated with statin, the rate of statin prescription decreasing with aging and dependence severity. Statin was also less used in residents with fewer daily medications. Blood lipid was measured in 47.6 % residents in secondary prevention and in 71.3 % residents treated with statin. Physicians in charge of these residents described other priorities due to polypathology and polymedication.
Our data confirm the cholesterol paradox previously reported in older people (13). Indeed, statin use is subnormal although cardiovascular diseases are the most frequent cause of death in persons 75 years and more (14, 15). In older people, statin is still underutilized as reported in several studies (13, 16-21). The prevalence of statin utilization in nursing home residents varies from 30 % in Spain (22) to 31,8 % after hospitalization in cardiology (23). Underutilization of lipid-lowering therapy in the elderly could have many explanations (24).
Firstly, physician could be inattentive to cardiovascular prevention because of multiple other diseases. Priority is then given to manage other chronic conditions due to constraints in time, expertise and preferences (25). Indeed, polypathology and polymedication are the main reasons for not initiating or discontinuing statin treatment in nursing home residents. The lack of blood lipid assessment in one-third of patients under statin use supports this explanation.
Secondly, the cholesterol paradox is likely due to misconception in benefit-harm tradeoff since there is a lack of perception of real risk by physicians in this age category (26, 27) although the excessive cardiovascular mortality attributable to elevated serum cholesterol levels increase with age (28).
Thirdly, there is a belief that treatment is less effective in older people despite counter evidence. Indeed, beneficial effects of statin have been reported in several studies on secondary prevention of cardiovascular diseases in very old persons. In an observational prospective study of 1410 older patients, mean age 81 years, with prior myocardial infarction and a serum LDL- C of 1.25 g/l or higher, use of statin for a 3-year period significantly reduced CHD related death or nonfatal myocardial infarction by 50%, stroke by 60% and heart failure by 48%. New coronary events were also significantly reduced in patients older than 90 years. (29). Beneficial effects of statin in secondary prevention have also been reported in elderly people with polypathology (30) and in nursing home residents (31). In older patients with diabetes, statin reduces cardiovascular morbidity (32) and all- cause of mortality (33).
Fourthly, there are also concerns about statin safety due to the higher comorbidities and polypharmacy. However, tolerance and safety of statin do not change in older people, especially with low or moderate doses (24). Intensive statin therapy is associated with a moderate, but significant increase in muscular intolerance in older patients (34).
Physicians and geriatricians should be aware of the real-benefit risk of statin in older people. Interestingly, statin use in patients with coronary heart disease living in an academic nursing home increased from 21 % in 2002 to 70 % and to 87 % in 2003 and 2008, respectively, following an educational program (35).
According to the guidelines recently published, statin should be used in secondary prevention, although after 75, it should be limited to moderate doses (9, 36, 37). Statin treatment should be continued unless concerns about tolerance or safety emerge. The introduction of statin in so far untreated patient may be discussed: in the STOPP-START screening tool, statin use was advised in persons with CHD, ischemic stroke or PAD if the life expectancy is higher than 5 years and if they have a good activity daily life score; in persons with diabetes, statin should be given if one major cardiovascular risk factor present (38). Residents in nursing home are a specific subgroup of older persons with high incidence of comorbidities and limited life expectancy. Therefore, decisions about statin prescription or discontinuation should take into account their life expectancy (39). The minimal exposure to statin that could be beneficial ranges from 3.2 years (40) to 5.3 years (41). Law et al have reported that after lowering blood cholesterol by 10 % in the 55-64 years, CHD incidence is reduced by 7 % during the first two years, 22 % and 25 % after 2.1-5, and more than 5 years, respectively (3). When life expectancy is limited and especially in the palliative care setting, statin should be discontinued since no difference in life duration and even improved quality of life have been reported (42).
The strength of our study is based on the analysis of a large number of medical charts of residents living in several nursing homes under the medicare of numerous physicians. One limitation of our study is the lack of knowledge on blood lipid level and statin utilization on hospital discharge after cardiovascular events. Indeed, statin may have been prescribed to a larger number of residents prior to discontinuing its use for undetermined reasons. Besides, the putative beneficial effect of statin could not be investigated in our study.
In conclusion, secondary prevention of cardiovascular diseases by intervention on blood lipid levels remains underemployed in nursing home in the absence of guidelines for this population. Further extensive cohort studies on statin tolerance, safety and reduction of mortality or new cardiovascular events are needed to delineate the profiles of residents in nursing homes leading to the prescription or discontinuation of this treatment.
Acknowledgment: E.G and C.O collected data, contributed to discussion and wrote the manuscript; M.G performed statistical analysis and contributed to discussion and edition of the manuscript; C.M contributed to analysis of results and discussion. F.R initiated the study, contributed to discussion and edited the manuscript. The authors thank Mr C. Gammelin (IT Department, State Geriatrics Centre for his excellent assistance in statistical analysis, Ms N. Grémeaux for her excellent assistance in English edition and Ms A. Langar for editorial assistance. This work was made possible through the collaboration of Doctors D. Frant, L. Mari and I. Moussa (from the Centre Gérontologique Départemental) and Doctors B. Adevah (Le Baou et Horizon Bleu), P. Clot-Faybesse (Korian Perier), G. Delalande (Villa des Poètes), N. Drancourt (Le Mas des Ainés), B. Labarrière (Résidence Saint Barnabé), F. Masseboeuf (Résidence Notre Dame), O. Reynaud-Lévy (Maison de Retraite de Cassis), A. San José (Korian Mistral) and the Groupement de Coopération Sanitaire PGAM, Marseille.
Conflict of interest: E. G, M.G, C.M, C.O and F.R declare no conflict of interest.
Ethical standards: This work has been approved by the ethical committee of the Departmental Geriatric Center.
References
1. Aronow WS. Clinical causes of death of 2372 older persons in a nursing home during 15-year follow-up. J Am Med Dir Assoc 2000;1:95-96
2. Lewington S, Whitlock G, Clarke R et al. Blood cholesterol and vascular mortality by age, sex, and blood pressure: a meta-analysis of individual data from 61 prospective studies with 55,000 vascular deaths. Lancet 2007;370:1829-1839
3. Law MR, Wald NJ, Thompson SG. By how much and how quickly does reduction in serum cholesterol concentration lower risk of ischaemic heart disease? BMJ 1994;308:367-372
4. Baigent C, Keech A, Kearney PM et al. Cholesterol Treatment Trialists’ (CTT) Collaborators. Efficacy and safety of cholesterol-lowering treatment: prospective meta-analysis of data from 90,056 participants in 14 randomised trials of statins. Lancet 2005;366:1267-1278
5. Lee PY, Alexander KP, Hammill BG et al. Representation of elderly persons and women in published randomized trials of acute coronary syndromes. JAMA 2001;286:708-713
6. Stone NJ, Intwala S, Katz D. Statins in very elderly adults (debate). J Am Geriatr Soc 2014;62:943-945
7. Rich MW. Aggressive lipid management in very elderly adults: less is more. J Am Geriatr Soc 2014;62:945-947
8. Morley JE, Mahon G. Statins and the nursing home. J Am Med Dir Assoc 2014;14:853-854
9. Stone NJ, Robinson JG, Lichtenstein AH et al. American College of Cardiology/American Heart Association Task Force on Practice Guidelines. 2013 ACC/AHA guideline on the treatment of blood cholesterol to reduce atherosclerotic cardiovascular risk in adults: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. J Am Coll Cardiol 2014;63(25 Pt B):2889-2934
10. Schaefer EJ, Lamon-Fava S, Cohn SD et al. ESC/EAS Guidelines for the management of dyslipidaemias: the Task Force for the management of dyslipidaemias of the European Society of Cardiology (ESC) and the European Atherosclerosis Society (EAS). Eur Heart J 2011;32:1769-1818
11. Expert Dyslipidemia Panel, Grundy SM. An International Atherosclerosis Society Position Paper: Global recommendations for the management of dyslipidemia. J Clin Lipidol 2013;7:561-565
12. Vetel J. AGGIR: Guide pratique pour la codification des variables. Principaux profils des groupes iso-ressources. Rev Gériatr 1994;19:249-259
13. Ko DT, Mamdani M, Alter DA. Lipid-lowering therapy with statins in high-risk elderly patients: the treatment-risk paradox. JAMA 2004;291:1864-1870
14. Driver JA, Djoussé L, Logroscino G et al. Incidence of cardiovascular disease and cancer in advanced age: prospective cohort study. BMJ 2008;337:a2467
15. Go AS, Mozaffarian D, Roger VL et al. American Heart Association Statistics Committee and Stroke Statistics Subcommittee. Heart disease and stroke statistics-2014 update: a report from the American Heart Association. Circulation 2014;129:399-410
16. Whincup PH, Emberson JR, Lennon L et al. Low prevalence of lipid lowering drug use in older men with established coronary heart disease. Heart 2002;88: 25-29
17. Lemaitre RN, Furberg CD, Newman AB et al. Time trends in the use of cholesterol-lowering agents in older adults: the Cardiovascular Health Study. Arch Intern Med 1998;158:1761-1768
18. Ford ES, Mokdad AH, Giles WH et al. Serum total cholesterol concentrations and awareness, treatment, and control of hypercholesterolemia among US adults: findings from the National Health and Nutrition Examination Survey, 1999 to 2000.Circulation 2003;107:2185-2189
19. Allen Maycock CA, Muhlestein JB, Horne BD et al. Intermountain Heart Collaborative Study Statin therapy is associated with reduced mortality across all age groups of individuals with significant coronary disease, including very elderly patients. J Am Coll Cardiol 2002;40:1777-1785
20. Chokshi NP, Messerli FH, Sutin D et al. Appropriateness of statins in patients aged ≥80 years and comparison to other age groups. Am J Cardiol 2012;110:1477-1481
21. Cournot M, Cambou JP, Quentzel S et al. Key factors associated with the under-prescription of statins in elderly coronary heart disease patients: Results from the ELIAGE and ELICOEUR surveys. Int J Cardiol 2006;111:12-18
22. García-Gollarte F, Baleriola-Júlvez J, Ferrero-López I et al. Inappropriate drug prescription at nursing home admission. J Am Med Dir Assoc 2012;13:83.e9-15
23. Parikh S, Shrank WH, Mogun H et al. Statin utilization in nursing home patients after cardiac hospitalization. J Gen Intern Med 2010;25:1293-1299
24. Alonzo CB. Myths and facts concerning the use of statins in very old patients. Cardiovasc Hematol Disord Drug Targets 2011;11:17-23
25. Redelmeier DA, Tan SH, Booth GL. The treatment of unrelated disorders in patients with chronic medical diseases. N Engl J Med 1998;338:1516-1520
26. Grundy SM, Cleeman JI, Rifkind BM et al. Cholesterol lowering in the elderly population. Coordinating Committee of the National Cholesterol Education Program. Arch Intern Med 1999;159:1670-1678
27. Wenger NK. Dyslipidemia as a risk factor at elderly age. Am J Geriatr Cardiol 2004;13 (Suppl 1):4-9
28. Rubin SM, Sidney S, Black DM et al. High blood cholesterol in elderly men and the excess risk for coronary heart disease. Ann Intern Med 1990;113:916-920
29. Aronow WS. Treatment of high-risk older persons with lipid-lowering drug therapy. Am J Ther 2008;15:102-107
30. Galindo-Ocaña J, Bernabeu-Wittel M, Formiga F, et al. PROFUND Project researchers. Effects of renin-angiotensin blockers/inhibitors and statins on mortality and functional impairment in polypathological patients. Eur J Intern Med 2012;23:179-184
31. Eaton CB, Lapane KL, Murphy JB et al. Effect of statin (HMG-Co-A-Reductase Inhibitor) use on 1-year mortality and hospitalization rates in older patients with cardiovascular disease living in nursing homes. J Am Geriatr Soc 2002;50:1389-1395
32. Olafsdottir E, Aspelund T, Sigurdsson G et al. Effects of statin medication on mortality risk associated with type 2 diabetes in older persons: the population-based AGES-Reykjavik Study. BMJ Open 2011;1:e00013
33. Pilotto A, Panza F, Copetti M et al. MPI_AGE Project Investigators. Statin treatment and mortality in community-dwelling frail older patients with diabetes mellitus: a retrospective observational study. PLoS One 2015;10: e0130946
34. Yan YL, Qiu B, Hu LJ, Jing XD et al. Efficacy and safety evaluation of intensive statin therapy in older patients with coronary heart disease: a systematic review and meta-analysis. Eur J Clin Pharmacol 2013;69:2001-2009
35. Joseph J, Koka M, Aronow WS. Preval2013;ence of moderate and severe renal insufficiency in older persons with hypertension, diabetes mellitus, coronary artery disease, peripheral arterial disease, ischemic stroke, or congestive heart failure in an academic nursing home. J Am Med Dir Assoc 2008;9:124-127
36. Schaefer EJ, Lamon-Fava S, Cohn SD, et al. Effects European Association for Cardiovascular Prevention & Rehabilitation, Reiner Z, Catapano AL, et al. ESC/EAS Guidelines for the management of dyslipidaemias: the Task Force for the management of dyslipidaemias of the European Society of Cardiology (ESC) and the European Atherosclerosis Society (EAS). Eur Heart J 2011;32:1769-1818
37. Expert Dyslipidemia Panel of the International Atherosclerosis Society Panel members. An International Atherosclerosis Society Position Paper: global recommendations for the management of dyslipidemia–full report. J Clin Lipidol 2014;8:29-60
38. Heart Protection Study Collaborative Group.MRC/BHF Heart Protection. Study of cholesterol lowering with simvastatin in 20,536 high-risk individuals: a randomised placebo-controlled trial. Lancet 2002;360:7-22
39. Sever PS, Dahlöf B, Poulter NR et al. ASCOT investigators. Prevention of coronary and stroke events with atorvastatin in hypertensive patients who have average or lower-than-average cholesterol concentrations, in the Anglo-Scandinavian Cardiac Outcomes Trial–Lipid Lowering Arm (ASCOT-LLA): a multicentre randomised controlled trial. Lancet 2003;361:1149-58
40. Gallagher P, Ryan C, Byrne S Kennedy J et al. STOPP (Screening Tool of Older Person’s Prescriptions) and START (Screening Tool to Alert doctors to Right Treatment) Consensus validation. Int J Clin Pharmacol Ther 2008;46:72-83
41. Lee SJ, Leipzig RM, Walter LC. Incorporating lag time to benefit into prevention decisions for older adults. JAMA 2013;310:2609-2610
42. Kutner JS, Blatchford PJ, Taylor DH Jr. Safety and benefit of discontinuing statin therapy in the setting of advanced, life-limiting illness: a randomized clinical trial. JAMA Intern Med 2015;175:691-700