R.E. Roller1, A. Morgner2, D. Eglseer3, G.H. Wirnsberger4
1. Department of Internal Medicine – Geriatrics, Medical University of Graz, Austria; 2. Nestlé Österreich GmbH, Am Euro Platz 2, A-1120 Vienna, Austria; 3. Department of Nursing Science, Medical University of Graz, Austria; 4. Division of Nephrology, Department of Internal Medicine, Medical University of Graz, Austria. Corresponding author: Prof. Regina E. Roller MD, MME, Department of Internal Medicine – Geriatrics, Medical University of Graz, Auenbruggerplatz 15, 8036 Graz, Austria, E-mail: regina.roller-wirnsberger@medunigraz.at, Tel.: +43 316 385 12274, Fax: +43 316 385 13062
Abstract
Objectives: To assess the attitudes and knowledge of health care professionals, who work with long term nursing home residents, with respect to key factors that influence malnutrition. Methods: Based on the results of a comprehensive literature research, a qualitative study was carried out by conducting problem-centered and structured interviews with healthcare professionals (N=25) from different professions. Each individual qualitative interview consisted of 10 open and problem-centered questions. Specific areas of interest were problems experienced by nursing home residents, useful measures that could be taken in cases of malnutrition and the prevalence of malnutrition in the nursing homes. 80 items were extrapolated from the interviews, transferred to a 5-point Likert-like scale questionnaire and included in an electronic survey, which was sent out to the 25 experts who had already been interviewed. Raters were first asked to rate the items according to their professional opinion and, second, according to the current state of nursing homes in Austria. Results: 77% of the 80 factors that may influence the treatment of malnutrition were identified as important, having an arithmetic mean (Ø a.m.) = 4.15. The top five determinants were: two factors related to kitchen food (i.e., “age-adapted texture and portion size” and “quality, freshness, taste, appearance and smell”), further education of nursing staff, interdisciplinary cooperation and education of dietitians. The evaluation of the 80 factors in terms of their status quo resulted in an Ø a.m. of 2.94. No factor was rated higher than Ø a.m. 3.74 in terms of its status quo (i.e., according to guidelines). The status quo quality was evaluated critically especially with regard to financial support and education. Conclusion: A gap exists between the attitudes of health care professionals and the status quo (what is being done) in Austrian nursing homes.
Key words: Malnutrition, screening, public health nutrition, nursing home, long term care, quality assurance.
Introduction
The nutritional requirements of individual older people differ and depend upon their living context and lifestyle. In nursing homes, nutritional care as well as social integration and beneficial care are important to ensure a good quality of life and encourage independence in the last years of life (1, 2). Although the efficacy of tailored nutrition therapy has been demonstrated in nursing home resident populations, the effectiveness of individual nutritional interventions may vary significantly. Acceptance and appreciation of the served food by residents is an important issue. Lack of acceptance and appreciation of the food may lead to malnutrition in residents (3-5). Various studies have demonstrated that the prevalence of malnutrition in nursing homes varies from 25% to 60%, depending on the definition applied, types of screening tools used and the characteristics of the patient population (7-10). However, if individual nutritional needs are not optimized, health outcomes are negatively impacted. The results of meta-analyses of trials have suggested that by providing nutritional therapy to malnourished older people, complications such as infections and wound breakdown could be reduced by 70%, and mortality, by 40% (11). Tailored nutritional care, therefore, must be delivered and fair, personalized, safe and effective care standards must be upheld to assure that residents experience the best quality of life (12).
The provision of nutritional care in nursing home settings depends on the existence of effective management structures that connect multidisciplinary care pathways. In Austria, as in many other European member states, the structures of nursing homes are heterogenous in terms of their funding and organizational structure. Furthermore, no centralized data management system or assessment structure has yet been established for nursing homes in Austria. Benchmarking – in terms gathering and processing quantitative data – has, therefore, not been systematically effected in nursing homes in Austria. Few national projects are currently ongoing that try to assess the nutritional situation of nursing home residents locally. A cross-sectional survey conducted in Europe (“Nutrition Day in Nursing Homes 2011“), which was based on the Mini Nutritional Assessment-short form (MNA-sf), reported that 17.9% of the entire population of nursing home residents were malnourished (13). Another Austrian survey suggested that up to 45.5% of nursing home residents are at risk of malnutrition in Austria (14). The Nutrition Day data demonstrated that – despite the fact that many care providers closely monitor the patients’ weights and screen them for nutritional risks– a higher proportion of Austrian residents is at risk than in other European countries.
This is the first study conducted in Austria that aims to identify influential factors that contribute to the development of malnutrition in nursing homes in Austria from the viewpoint of the long-term care staff.
Methods
Before commencement of the study, a waiver was obtained from the local ethics committee of the city of Vienna. The study was conducted following the guidelines appearing in the World Medical Association (WMA) declaration of 1991, and data were stored as recommended in the National Data Protection Guidelines.
Qualitative Study Design
It was the aim of this study to obtain an overview of the most relevant factors that affected the levels of malnutrition in nursing home residents. First, a thorough literature review was performed by searching the PubMed Health search engine via the Internet the key terms “malnutrition”, “nursing home” and “contributing factors”, filtering the results for articles published from 2005 to 2014. Review articles were also included to capture relevant data appearing in literature published before 2005.
Due to the complex nature of the data set gained during this pre-analysis step, a semi-qualitative study design was prepared. Individual, personal interviews were chosen as the primary research strategy. It was important to establish direct rapport with the experts and practitioners working in the field of nursing home care, in order to ask and receive answers to complex questions that had arisen following the detailed analysis of the literature review. Data in the international literature indicated that factors contributing to the development of malnutrition in nursing home residents could be categorized as either endogenous or exogenous determinants. These could then be additionally related to either the patient (micro-level), institution (meso-level) or social welfare or healthcare system at the country level (macro-level). Within this structure, 10 problem-centered questions that were based upon the literature review findings were created by the study team and included in the interviews (see table 1). The first 2 of these 10 questions allowed the interviewer to evaluate nutritional status in terms of the anthropology and eating patterns of the residents. Question 3 was designed to identify which of the existing screening tools were commonly used and question 4, to gather details about the nutritional assessment that was carried out on routine, structured basis. Questions 5 to 7 were designed to help the interviewer identify influential factors operating on public health levels (micro-, meso-, macro-levels) that could affect nutritional care in nursing homes. Question 8 was an open-ended question that explored individual opinions on possible scale-up procedures for the nutritional supply in nursing homes. Questions 9 and 10 allowed the interviewer to gain an estimate of the prevalence of malnutrition in Austrian nursing homes.
Study Participants / Target groups for Interviews
The inclusion criteria to select interview partners were designed on the basis of their long-term experience, either in the daily practice or as researchers in the field of nursing home residents and nutrition. In either case, interview partners were selected on the basis of their strong personal dedication towards systemic approaches. 11 experts were nominated by three Austrian scientific societies, the “Austrian Society for Clinical Nutrition” (AKE), “Austrian Society for Geriatrics and Gerontology” (ÖGGG) and “Austrian Nutrition Society” (ÖGE). 14 practitioners were selected from a public nursing home database due to the fact that they worked at nursing homes that were considered “average” in terms of the number of beds (n=88). Members of the following professions were included in the interviewee group: physicians, nurses, dietitians, nutritionists, cooks and nursing home management personnel (see table 2). Therefore, opinions were recorded from a range of personnel involved in different aspects of delivering nutritional care in nursing homes.
To reduce inter-rater variability, the personal interviews with individuals were conducted by one single interviewer. All interviews were recorded with permission of the participants, thereafter transcribed and qualitatively assessed using the method of Mayring by two independent raters from the study team. Overall, the coherence of interpretation was 90%. The method of Mayring can be used to analyze texts within the context of communication in an empirical, methodologically controlled way and assign text elements to categories in a step-by-step model (15). Key text elements were excerpted, grouped, paraphrased and reduced to the final 80 influential factors identified.
Semi-quantitative Study Approach
To ensure the validity of the data assessed in the interviews and additionally test for the generalizability of the interview results, 80 items that were extrapolated from the interviews and transferred to a 5-point Likert-like scale questionnaire were then included in an electronic survey and sent out to 25 experts who had agreed to participate in the interviews. Raters were asked to rank the items according to their impact on the daily nursing home procedures as well as process management and planning in nursing homes. 18 items on the questionnaire addressed factors operating at the micro-level; namely, these were factors that could potentially influence food acceptance by individual residents and risk factors for malnutrition. 62 items addressed factors operating at the meso- and macro-levels in nursing homes in Austria. The raters were asked a) to rate the importance of the factors addressed on the basis of their personal opinion and b) to rank the current situation in Austrian nursing homes (status quo in Austria) on the basis of their personal experience. The Likert-like scale values provided to all raters for the 80 items were expressed as arithmetic means (Ø a.m.) and analyzed according to their ranking using SPSS 21.
Results
25 participants (18 females and 7 males) were involved in the study. The median age was 45 years (range: 28-62). 4 of the participants interviewed worked in strategic and operational management departments. 12 of the 25 participants had academic backgrounds. The average interview took 44 minutes (range: 20-75) per person. The values recorded during the interview are listed in Tables 4, 5, 6. The experts and practitioners interviewed during the study estimated the prevalence of malnutrition in Austrian nursing homes to be approximately 36% (range: 15-90%). They estimated the nutritional supply level, this means the percentage of malnourished patients that receive nutritional therapy, at 35% (range: 5-80%).
Supply level = percentage of malnourished patients that receive nutritional therapy
The 67 factors in the questionnaire that reflected possible risk factors for the development of malnutrition were all rated very high (Ø a.m. of 4.15, with 77.1% of the respondents providing a rating of 4 or 5 on the 5-point Likert scale). When evaluating the status quo on the Likert-scale, considering the actual importance of these factors in their daily life in Austrian nursing homes, only 39% of the respondents provided ratings of 4 or 5 points on the Likert scale (Ø a.m. of 2.94, with 30.9% of the respondents providing a rating of 4 or 5 on the 5-point Likert scale). These data indicate the general need for improvement in the status quo of numerous determinants in Austrian long-term care. The 10 most important factors that affect nutritional therapy in nursing homes are shown in table 3.
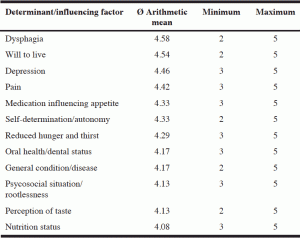
Table 4 Patient-related determinants (micro level) that affect nutritional therapy in nursing homes rated by experts
The three most important influential factors (table 5) that addressed the therapy of malnutrition operated within the nursing home or on the meso-level and included: “Kitchen food: Age adapted texture and portion size” (Ø a.m: 4.79), “Kitchen food“: Quality, freshness, taste, appearance, smell” (Ø a.m: 4.79) and “Further education: Nursing staff” (Ø a.m: 4.75). Other determinants related to the nursing home were “interdisciplinary cooperation” (Ø a.m: 4.74), the “individual causal research on the development of malnutrition” (Ø a.m: 4.71), the consideration of the “individual’s biography of eating habits” (Ø a.m: 4.67), “screening for malnutrition” (Ø a.m: 4.67) and “interpersonal skills of medical staff” (Ø a.m: 4.67), as shown in table 5. The main influential factors operating on the macro-level (local and national health authorities and scientific organizations) were related to areas such as education, transparency and control of the quality of nursing, benchmark systems and financing, as shown in table 6.
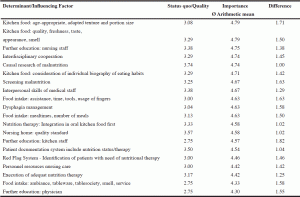
Table 5 The 20 most important nursing-home related determinants (meso level) that affect nutritional therapy in nursing homes rated by experts
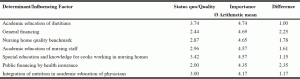
Table 6 The 7 most important determinants related to health authorities (macro level) that affect nutritional therapy in nursing homes rated by experts
Discussion
Experts and practitioners who were interviewed during this study estimated the prevalence of malnutrition in Austrian nursing homes to be approximately 36% (ranging from 15-90%). This means that experts and practitioners seem to be estimating the prevalence of malnutrition in nursing home residents in Austria on the basis of data published in literature since these numbers agree with those found during our thorough literature review (13,14). We specifically wanted to ask the question: which factors contribute to these estimates of malnutrition in nursing home residents?
67 out of 80 factors that we identified as having the potential to affect nutritional therapy in nursing homes in Austria were rated as “very important” by experts with an Ø a.m. score in the Likert-like scales above 4.0. However, when comparing the importance of factors in terms of the best evidence gathered on actual practices to the status quo of delivery in Austria, the greatest differences among the ratings given by experts were found for the determinants related to financing, knowledge management, education and kitchen food.
The most important determinants identified at the patient- or micro-level were “dysphagia“ (Ø a.m. 4.58), “will to live“ (Ø a.m. 4.54), “depression“ (Ø a.m. 4.46), “pain“ (Ø a.m. 4.42) and “medication affecting appetite“ (Ø a.m. 4.33, table 4). While endogenous or patient-related factors such as “will to live” and “depression” are difficult to influence, selected exogenous determinants operating on the meso- and macro-levels, which our study has identified as important, could be improved by different stakeholders and staff of the public health authorities.
Good nutritional status has been identified as an important factor with reference to quality of life and wellbeing, because it promotes better autonomy, mobility, self-reliance, alertness and more active participation in social life. Although nutrition therapy was recommended by 100% of the interviewers in our study, only 2 of 14 practitioners (14%) and 4 of 11 experts (36%) stressed the need for individual causal research for the assessment of malnutrition as an integral part of nutritional therapy. The frequently used body mass index (BMI) is not sufficient as a stand-alone screening tool to assess malnutrition (17). Very often, measuring the BMI does not allow the identification of patients who suffer from unintended weight loss or sarcopenia. Still, weight loss is often the first sign that a resident is at risk of malnutrition. One possible option that would allow all points mentioned by the interviewees to be addressed would be to introduce MNA-sf in the daily routine at long-term care facilities (18). MNA-sf has been validated in several studies and settings and has been recommended by the European Society of Clinical Nutrition and Metabolism (ESPEN) for nutritional screening in older people.
Based on Volkert et al. (5), it is difficult or nearly impossible to reduce the risk of malnutrition below 20-25% by attempting to address endogenous factors (“micro-level“). To verify these numbers and confirm the “unavoidable” prevalence of malnutrition in nursing homes with respect to specific patient characteristics, a longitudinal multicenter analysis among nursing home residents would be required. We agree that patients at risk of malnutrition with unintentional weight loss and malnourished patients should receive nutritional intervention following the guidelines. Volkert et al. (5) emphasized that only 20% of patients with malnutrition receive nutritional therapy.
Once patients with a need for nutritional therapy have been identified, a multidisciplinary team that includes members of the nursing, kitchen, medical, and service staff must define and adjust the requirements of the individual’s nutritional therapy, according to opinions expressed by experts included in our study (Ø a.m. 4.74). Nutritional therapy can only function if the cause of malnutrition is identified, directly addressed and the underlying conditions improve. The effectiveness of nutritional therapy might, therefore, be reduced if the loss of appetite is caused by pain, medication or promoted by feelings of loneliness. Nutritional therapy compensates for the gap that exists between the identification of nutritional needs and the consummation of food prepared in the kitchen. The kitchen food, which consists of five meals per day, offers between 1800 and 2000 kcal daily. However, the average consumption rate varies, and patients with malnutrition may consume less than 70-80% (approx. 1600 kcal) per day (19). Regular controls of the consumed food and supplementation with plate waste records should be performed to measure patients’ acceptance and, hence, the potential effectiveness of the therapy (4). According to the experts interviewed, nutritional therapy can be supported by considering the individual’s biography of eating habits (Ø a.m. 4.67), taking more time and receiving assistance during food intake (Ø a.m. 4.63), optimizing meal times to avoid long periods of fasting at night (Ø a.m. 4.63), creating an appetizing ambiance by optimizing table settings, societal interaction and the presentation and smell of the food (Ø a.m. 4.33) and providing more finger foods, especially for patients with dementia (Ø a.m. 4.04). All the approaches mentioned here have also been discussed in literature (21-25). The age-adapted textures and portion sizes of the meals served (Ø a.m. 4.79) are of particular importance, as up to 40% of nursing home residents suffer from dysphagia (26, 27). This issue has recently been addressed in several publications, and its importance has been underlined through the creation of several European Working Groups such as the Dysphagia Working Group of European Union Geriatric Medicine Society (EUGMS), Dysphagia Europe and others. Intense efforts, driven by members of the European Innovation Partnership on Active and Healthy Aging (EIP-AHA), are also being made to optimize primary food care for older European citizens with special nutritional needs. One of the major impacts of the EIP-AHA program is the continuous professional training of chefs (28).
Improving the education and awareness of and knowledge transfer among all caregiver groups working in nursing homes is vital. This is an important starting point to gain a proper understanding of the need for screening and individual nutritional therapy in older adults. On a macro-level, it is important to support the transfer of knowledge about malnutrition among different educational facilities and between competence levels as well as into institutions in the tertiary sector such as universities. At the meso-level of nursing homes, the ability to regularly update and exchange knowledge and experience plays an important role. Data collected during a recent multicenter study that assessed knowledge and attitudes of nursing staff in Austrian nursing homes showed that, in particular, the topics of multidisciplinary nutritional care and screening and assessment of malnutrition are understudied (14). Educational activities, addressing educational aspects both within and between professions, should be performed while adhering to the quality standards described in the European Framework of Continuous Professional Education (29).
The implementation of a nutritional management system that considers all key factors described in this study requires sponsorship and commitment as well as financial support of nursing home management teams to assure sufficient project management. It also requires that adequate numbers of staff, financial resources, innovative communication channels between different team members and clear set targets be available. Clear targets include the identification of key performance indicators (KPI), which take into account the fact that contextual factors operating on the micro-level may not be influenced in any case even though nutritional care is optimized. These KPIs will gain importance when benchmarked and made available through an openly-accessible international nursing home database, such as that which has already been established as part of the “Nutrition Day” initiative (30).
Limitations of the study
The questions included in the qualitative interviews were created on the basis of the results of a thorough literature review conducted using the PubMed search engine. The 10 questions created did not represent all relevant questions that could be potentially asked in this field. Nine of the 10 interview questions were problem-centered questions, and only one question was an open-end question. Due to the high level of complexity of this topic, the inclusion of additional open-end questions could have allowed more issues to arise than occurred using the selected methodological format. However, the size of the pool of interview partners (n=25) and high level of agreement among the answers provided in the interviews and on the Likert-like questionnaire, provides support as to the extrapolability of the results obtained.
Conclusion
The data gathered during our study showed that malnutrition can be tackled by addressing specific issues related to the care system. It seems necessary to determine the “unavoidable prevalence of malnutrition” that are due the existence of micro-level factors in every nursing home. We identified several important influential factors that appear to affect the extent to which malnutrition can be reduced as part of long-term nursing care. We also detected relevant factors operating on the micro-level, which we would refer to as “resident specific factors” that do not respond to optimization of nutritional care. The results of our study did not allow us to determine which percentage of malnutrition can be considered acceptable or unavoidable in Austrian nursing homes. To provide a general recommendation and attain a key performance level on a broader European scale, well-designed interventional cohort studies are needed.
Acknowledgments: We thank the staff and residents of the nursing homes as well as the interview partners (health care professionals) who took part in this study for their time and patience.
Conflict of interest: The authors have no conflicts of interest to declare.
References
1. Fries JF. Measuring and monitoring success in compressing morbidity. Ann Intern Med 2003;139:455-459
2. Hammar M, Ostgren CJ. Healthy aging and age-adjusted nutrition and physical fitness. Best Pract Res Clin Obstet Gynaecol 2013;27:741-752
3. Ljungqvist O, Man F. Undernutrition: a major health problem in Europe. Nutr Hosp 2009;24:369-370
4. Guest JF, Panca M, Baeyens JP et al. Health economic impact of managing patients following a community-based diagnosis of malnutrition in the UK. Clin Nutr 2011;30:422-429
5. Volkert D. Malnutrition in older adults – urgent need for action: a plea for improving the nutritional situation of older adults. Gerontology 2013;59:328-333
6. Bauer JM, Volkert D, Wirth R et al. Diagnosing malnutrition in the elderly. Deutsch Med Wochenschr 2003;131:223-227
7. Tominz R, Germano CD, Bovenzi M et al. Prevalence of malnutrition among institutionalized elderly subjects in Trieste, Northern Italy. Epidemiol Prev 2012;36:263-272
8. Volkert D, Pauly L, Stehle P et al. Prevalence of malnutrition in orally and tube-fed elderly nursing home residents in Germany and its relation to health complaints and dietary intake. Gastroenterol Res Pract Article ID 247315, Epub, 2011.
9. Bartholomeyczik S, Reuther S, Luft L et al. Prevalence of malnutrition, interventions and quality indicators in German nursing homes – first results of a nationwide pilot study. Gesundheitswesen 2010;72:868-874
10. Meijers JM, Halfens RJ, van Bokhorst-de van der Schueren MA et al. Malnutrition in Dutch health care: prevalence, prevention, treatment, and quality indicators. Nutrition 2009;25:512-519
11. Stratton RJ, Green C, Oxon EM. Disease related malnutrition: an evidence-based approach to treatment. CABI Publishing, Wallingford, 2003
12. Department of Health. Our NHS, our future, 2007. http://www.dh.gov.uk/en/ Publicationsandstatistics/Publications/PublicationsPolicyAndGuidance/dh_079077
13. Feedback NutritionDay, 2012. http://www.nutritionday.org/cms/upload/pdf/6_about_nutritionDay/6.1.example_reports/report_NH_example_english.pdf
14. Bauer S, Halfens RJG, Lohrmann C. Knowledge and attitudes of nursing staff towards malnutrition care in nursing homes: A multicentre cross-sectional study. J Nutr Health Aging 2015;19:734-740
15. Mayring P. Qualitative Inhaltsanalyse, Grundlagen und Techniken. Deutscher Studienverlag, Weinheim, p31, 1990
16. Schönherr S, Halfens RJG, Meijers JMM et al. Structural and process indicators of nutritional care: A comparison between Austrian hospitals and nursing homes. Nutrition 2012;28:868-873
17. Gavriilidou NN, Pihlsgard M, Elmstahl S. High degree of BMI misclassification of malnutrition among Swedish elderly population: Age-adjusted height estimation using knee height and demispan. Eur J Clin Nutr 2015;69:565-571
18. Rubenstein LZ, Harker JO, Salva A et al. Screening for undernutrition in geriatric practice: Developing the short-form mini-nutritional assessment (mna-sf). J Gerontol A Biol Sci Med Sci 2001;56:M366-372
19. Grieger JA, Nowson CA. Nutrient intake and plate waste from an Australian residential care facility. Eur J Clin Nutr 2007;61:655-663
20. Milne AC, Potter J, Vivanti A, Avenell A. Protein and energy supplementation in elderly people at risk from malnutrition. Cochrane Database Syst Rev 2009;15:CD003288.
21. Gariballa S, Forster S, Walters S et al. A randomized, double-blind, placebo controlled trial of nutritional supplementation during acute illness. Am J Med 2006;119:693-699
22. Volkert D, Berner YN, Berry E et al. Espen guidelines on enteral nutrition: Geriatrics. Clin Nutr 2006;25:330-360
23. Splett PL, Roth-Yousey LL, Vogelzang JL. Medical nutrition therapy for the prevention and treatment of unintentional weight loss in residential healthcare facilities. J Am Diet Assoc 2003;103:352-362
24. Lauque S, Arnaud-Battandier F, Mansourian R et al. Protein-energy oral supplementation in malnourished nursing-home residents. A controlled trial. Age Ageing 2000;29:51-56
25. Ljungqvist O, Man F. Undernutrition: a major health problem in Europe. Nutr Hosp 2009;24:369-370
26. Nogueira D, Reis E. Swallowing disorders in nursing home residents: how can the problem be explained? Clin Interv Aging 2013;8:221-227
27. Park YH, Han HR, Oh BM et al. Prevalence and associated factors of dysphagia in nursing home residents. Geriatr Nurs 2013;34:212-217
28. Illario M, Maione AS, Rusciano MR, Goosens E, Rauter A, Braz N, Jager-Wittenaar H, Di Somma C, Crola C, Soprano M, Vuolo L, Campiglia P, Iaccarino G, Griffiths H, Hartmann T, Tramontano D, Colao A, Roller-Wirnsberger RE. NutriLive: An Integrated Nutritional Approach as a Sustainable Tool to Prevent Malnutrition in Older People and Promote Active and Healthy Ageing—The EIP-AHA Nutrition Action Group. Advances Publ Health 2016, in press
29. Hallin K, Henriksson P, Dalén N et al. Effects of interprofessional education on patient perceived quality of care. Med Teach 2011;33:22-26
30. Valentini L, Schindler K, Schlaffer R et al. The first NutritionDay in nursing homes: participation may improve malnutrition awareness. Clin Nutr 2009;28:109-116