R. Meehan1, R. Shura2
1. Kent State University, Kent, OH, USA; 2. Hiram College, Hiram, OH, USA. Corresponding author: Rebecca Meehan, Ph.D., Assistant Professor of Health Informatics, Kent State University, 1125 Risman Rd., Kent, OH, USA 44242, RMeehan3@kent.edu
Abstract
Few qualitative studies have explored the day-to-day experiences of people with vision impairment living in assisted living. Long-term care residents with vision impairment are more likely to have problems with ADLs, like dressing and feeding themselves, and increased rates of depression, social isolation, and falls. To better understand how visual health may impact care and quality of life in long-term care, this qualitative study used semi-structured interviews to consider the direct experiences of vision impairment among residents of an assisted living facility within a continuing care retirement community (CCRC) in the United States (N=13). Results indicate that vision impairment may be an ‘unseen’ and often overlooked experience among institutionalized elders that is critical for appropriate care and improving quality of life. Residents’ reported impact of vision impairment on daily life and their reported coping strategies are discussed, yielding implications for adaptations of individuals, caregivers, and long-term care institutions and staff.
Key words: Long-term care, ageing, vision impairment, disability, institutionalized care, care providers.
Background
The experiences of long-term care residents with vision impairment are under studied but relevant to research on illness experience. Vision impairment and late-life changes in visual acuity can be detrimental to the quality of life and the appropriateness of medical care of elders who live in long-term care settings, particularly if the impacts of vision limitations on elders’ daily lives are not well understood. Adults across the world are living longer. The World Health Organization (1) reports that between 2000 and 2050, the proportion of the world’s population over 60 years will double from about 11 per cent to 22 per cent, with an absolute number of people aged 60 years and over expected to increase from 605 million to 2 billion over the same period of time. As more people are living longer, there is a marked increase in the number of older adults who have vision impairment. The International Federation on Ageing issued a report in 2012 calling for more research to be conducted on vision impairment and its connections to elders’ daily experiences, noting the lack of research that specifically examines these topics (2). The report outlines that worldwide, 285 million people are visually impaired, including 39 million who are blind (2). In the United States, vision loss ranks among the top ten causes of disability (3). The prevalence of vision impairment among older adults (over age 65) and subsequently nursing home residents is increasing (4). The number of persons aged 65 and over with severe vision impairments in the U.S. is expected to be 7.7 million people by 2030 (5). Many older adults with vision impairment require formal caregiving, and support in long-term care settings. Research findings suggest that 29 per cent to 62 per cent of long-term care residents experience vision impairments (6). The higher proportions reflect that the prevalence of vision impairment rises among nursing home residents when including those with a diagnosis of at least moderately impaired vision (7).
Limited but important research has considered how vision impairment may be linked explicitly to major resident outcomes in long-term care, including quality of life and appropriateness of care. Nursing home residents with vision impairment had significantly higher limitations in activities of daily living (ADL) compared with other residents who were not visually impaired (8). Older adults with vision impairment are more likely to have problems dressing and feeding themselves, have higher rates of depression, and experience higher incidence of falls (9), all of which can lead to diminished quality of life. Elliot and colleagues noted the risk for older adults with low vision to have maladaptive mood changes, social difficulties, and lack of leisure activity (6).
Personal meaning, appraisal, and experience of vision loss play a major factor in disability, as self-reports of vision loss are affected by adaptations of the individual, their outlook, as well as severity of their impairment (10; 11). For instance, some residents may have a far better visual acuity than others upon examination, but may feel totally incapacitated by the vision loss; whereas another person with a more diminished visual capacity may not report as many difficulties, because they may be coping with their situation more effectively. Living with vision loss can lead to forms of depression if positive coping strategies are not implemented (12). Gellis and McCracken found that assisted-living residents appear to have significant rates of depression and depressive symptoms, yet their conditions are under-detected and under-treated (13). Residents can feel demoralized by their disability, which would increase likelihood of depression, although prevention of such depression may be possible in some cases of vision impairment (14). Many older adults with vision impairment reach a point where they may think there is nothing that can be done to make their lives better in terms of their vision and its related effect on their functional ability (12). Those who remain involved in personally meaningful activities are likely to make more successful adjustments to both ageing and visual impairment. Personal adaptations allow a person with vision impairment to limit or eliminate a disability (15). Long-term care staff and other caregivers are critical in helping institutionalized elders with vision impairment to make appropriate and effective adaptations.
Elders who live in long-term care settings, like assisted living facilities (hereafter ALF), need to manage their vision impairment or vision changes in the context of a shared living environment. This generally includes communal meals and activities with other residents, as well as families who visit and nursing staff who are part of their daily lives. Thus, the ongoing experience and management of vision impairment for older adult ALF residents is impacted by the ALF social environment and patterns of care. Few studies have examined the daily experiences of elders with vision impairment in ALF settings. Vision impairments and related complications can be exacerbated by lack of communication and errors in medical charting among ALF staff (16). Vision problems among long-term care residents can be overlooked or may not be given adequate rehabilitative attention. Several factors may contribute to this situation. Specifically, changes in the resident’s vision may be gradual; hence the impact of such changes may not be fully appreciated by the resident, family or the staff. Moreover, vision loss may be obscured by other serious acute or chronic conditions. As a result, issues with vision impairment may never be documented or addressed, which could hinder the continuity, appropriateness and quality of care (16). Long-term care staff must be cognizant that visual impairment is a significant barrier to the older adult’s ability to fully engage in life in the long-term care setting (17). Fatalism among long-term care workers regarding vision ability in later-life, which has not been studied systematically, may also be a contributing factor to lack of attention to visual health in U.S. long-term care facilities. These factors indicate that visual health can be a key factor that influences institutionalized elders’ health and vitality, as well as the efficacy of caregivers, services, and care plans.
Aligning these trends in visual health and ageing to the complex issues of health care access and affordability in the United States reveals additional complexities and challenges. Policies that provide health care access to elders in the United States – including Medicare, Medicaid, veterans’ benefits, and private-pay health insurance policies — are incredibly complex; uneven in their eligibility requirements, accessibility, and services covered; and fragmented, leaving gaps in availability and affordability of routine vision care for some elders. For example, basic Medicare, the only health care policy that is available to all Americans over the age 65, does not cover routine eye exams, but it does include coverage for some preventive and diagnostic visual examinations (18). Since 2002, older adults using Medicare have been eligible for physician prescribed low vision rehabilitation (hereafter LVR) (Labour/HHS/Education Appropriations Bill, 2002) (18). LVR is available to the patient as long as he or she shows an ability to improve. LVR can be managed and delivered by physicians, ophthalmologists, occupational therapists, and physical therapists. Older adults living in long-term care settings, including ALF, are also eligible for this care. The availability of LVR for older adults is potentially a tremendous resource, providing an impactful opportunity for patients to improve their management of low vision. However, the geographic availability and ease of accessibility of these LVR services for institutionalized elders is uneven and not guaranteed. Access to care by ophthalmologists and other eye care specialists is, thus, not assured to assisted living residents under current health care policy and provision.
In order to understand the most salient ways to enhance quality of life and quality of care of elders who experience vision challenges, it is imperative to hear directly from older adults about their experiences of living with vision impairment. There are very few qualitative studies of older adults’ adjustments to vision loss. Kleinschmidt interviewed 12 community dwelling older adults to discuss how they adapted to vision loss (19). The study results describe that participants used both internal (coping and positive attitude) and external resources (emotional and social support from family and friends) (19). Teitelman and Copolillo extend upon Kleinshmidt’s work by further exploring vision loss of community dwelling older adults (20). Their study used focus groups and interviews and described the psychosocial and emotional implications of vision loss among participants. The current study continues this examination of the lived experience of older adults with vision impairment by seeking first hand description and responses from older adults themselves. Moreover, the current study is unique and fills a gap in the literature, in that it focuses on older adults with vision impairment who live in a long-term care (e.g. ALF) setting. This study gives a voice to the older adult residents of an ALF, and through their interview responses, they provide insights about ways to improve quality of care and quality of life.
The objectives of this study include: a) to describe residents’ experiences of vision impairment; b) to identify strategies for coping and adapting to vision impairment, including the use of assistive devices; and c) to identify educational and training suggestions for long-term care staff and caregivers to improve quality of care for elder long-term care residents with vision impairment.
Methods
This study uses a qualitative descriptive method (21) with semi-structured interviews to consider the direct experiences of vision impairment among older adult residents of an ALF in the Midwest United States. The study was not designed to produce generalizable findings but rather to give voice to members of a vulnerable population to understand their experiences of impairment through their own voices. Semi-structured interview guides allow for participants to elaborate if and when they would like to expand on specific topics. Before research began, approval from the Institutional Review Board (IRB) was obtained from the ALF. All potential participants who showed interest in the study were first screened according to inclusion criteria. Inclusion criteria were: a) being an assisted living resident with vision impairment, b) score of at least 24 on the Mini Mental Status Exam (22), indicating satisfactory cognitive status, and c) English language fluency. In accordance with the study’s approved IRB protocol, all potential participants were given the opportunity to provide verbal and written informed consent prior to beginning the interview. No financial incentives were offered. Voluntary participation was maintained, and participants were reminded that they could end participation at any time, without reason. No full names of participants were gathered in the course of the interview recordings, transcripts, or analysis, nor were names ever attached to study documentation in order to protect the anonymity of participants. All interview records were only accessible by members of the research team, to protect the confidentiality of participants.
Study Site and Participants
The study site was a non-profit, independent ALF in the Midwest United States (U.S.), with 118 apartments. Twenty-four residents were identified by the ALF nursing staff as having vision impairment of varying types and degrees. These residents were then approached by the research team for their consent to participate in this study. Of those residents, nine were not interested in participating and two were either physically or cognitively unable. The remaining group (n=13) agreed to participate in interviews and gave written informed consent. All participants were Caucasian, and only one respondent was male. The length of the interviews ranged from ten minutes to 45 minutes, averaging 21 minutes. At the time of the study, low vision rehabilitation (LVR) services were not available to residents on site in the ALF.
Procedure
One-on-one, semi-structured interviews with residents were conducted. All interviews were audio-recorded and transcribed verbatim. Data were analysed using a coding process followed by thematic analysis. This process involved having two reviewers (the principal researcher and research associate) read the interview transcripts independently to identify emergent themes and concepts mentioned by respondents. Each reviewer looked for patterns emerging among the data, and then met to compare findings. Reviewers discussed results overall, and discussed results as they aligned to study goals: a) to describe residents’ experiences of vision impairment; b) to identify strategies for coping and adapting to vision impairment, including the use of assistive devices; and c) to identify educational and training suggestions for long-term care staff and caregivers to improve quality of care for elder long-term care residents with vision impairment. Differences were resolved by discussion and negotiated consensus (23).
Results
Vision Status
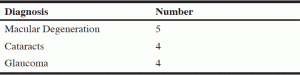
Table 1 lists official diagnoses of vision impairment reported by study participants. Residents were asked to describe when they first experienced vision issues and any vision impairment diagnosis (see Table 1). A few residents could not recall when vision problems first started. Others (n=7) reported that vision problems began several years ago, and for some (n=4) the problem with vision began within the past two years. Many (n=7) of the residents reported experiencing a decline in vision within the past year. Residents were asked if they sought medical intervention for help with vision. Seven respondents said that they used glasses. However, of those who used glasses, only four residents indicated that the glasses were helpful. Three of the residents reported they had cataract surgery in the past to help correct vision, and only one of those three indicated that the surgery was helpful.
Residents were not asked to rank severity of their vision impairments, which is sometimes done to quantify experience of impairment. In line with the purpose of this study, authors were interested in the qualitative, embodied everyday experience of vision impairment and how residents’ accounts of their day to day challenges had implications for quality of life and appropriateness of care in the assisted living setting.
Experience of Vision Impairment
Residents were asked if vision problems affected their daily lives, and if so, in what ways. Almost all of the residents interviewed (n=11) reported that daily life had been affected by vision challenges. Some reported that they can no longer read, drive, go anywhere, or recognize people who are not directly in front of them. Others said that they feel embarrassed or discouraged due to the effects of their loss of vision, with particular emphasis on the negative experience of losing prior abilities. One resident (Resident 13) responded, “Sure. It’s hard, because people call to you, but you don’t know who it is.” Other residents shared their frustration over the inability to enjoy social activities they once did:
«You cannot see what’s on your plate. You can walk a less normal distance than you used to. The normal things [changed].” -Resident 10
“[I can’t watch] the TV and my books I can’t read any more. That is very hard on me because I love to read.” -Resident 2
Residents were then asked if their social lives have been affected because of the vision impairment. Many described that not only the vision loss, but their overall health affects their social lives. These examples illustrate ways that residents claim their vision impairment has affected their social lives:
“You know damn well I would be lying if I said it didn’t. I try and go out to dinner as much as I can. I can’t go see movies. I used to go to plays and now I would have to sit on the stage to see it.” – Resident 11
“It’s hard to go to a movie unless I am in the first or second row. Even then my eyes start to hurt so badly. I miss that [going to movies].” – Resident 4
Overall, there was no distinct correlation between experience of vision impairment and type of vision diagnosis. Limitations of our sample size, however, suggest that more data would be needed to substantiate whether there is a meaningful relationship between type of vision diagnosis and patterns in residents’ reports of impacts on everyday life.
Adaptation and Coping
Respondents were asked what changes they have made in their lives because of vision impairment. Many respondents indicated they had made a change in their daily lives to maintain their independence while managing vision impairment. Some of these changes included being more careful (n=4), taking the bus or not driving (n=3). Others indicated that coming to live at the ALF community was an adaptation they made in their lives because of vision impairment (n=2). One resident (Resident 1) commented, “The ‘change’ was that I would not be able to live alone. I was in my own condo [condominium] for the last thirteen years since my husband passed away, and I knew I had to make a change. I made that decision right then and there that I was going to go into this type of life here. It was a really big change for me.”
When asked how they coped with vision issues, responses included having a routine (n=4), and having patience and acceptance (n=3). One respondent (Resident 3) said, “[You need] to have the patience of a saint.” Many of the residents indicated that they are careful and move slowly to try to minimize the chance of a fall. A few (n=3) sought out additional help at a local non-profit assistive centre for people with vision impairment. Several of those interviewed (n=8) still leave the assisted living facility for day trips. When asked if they had fears related specifically to vision impairment, respondents were divided in their reply with seven indicating they do not have any fears related to their vision loss. Still others (n=6) had fears of falling and of completely losing their vision.
Institutional Challenges
Residents’ interviews revealed challenges in their daily experiences due to vision impairment that were specific to the environment of the assisted living setting in which they lived. For example, there were issues with navigation and signage. When asked about the ease with which respondents could navigate within the assisted living facility and use signage marking entrances to various areas in the building, many said that they have had trouble reading the names on doors. Several (n=8) have trouble reading the bulletin board and the meal menus because of the small lettering. A few respondents mentioned having trouble seeing food on their plates at mealtimes. While some respondents had memorized the path to certain destinations (e.g. dining room), others described difficulty because of not being able to navigate back, and thus were not as engaged in daily activities in the ALF as they could be. Only a few (n=4) who did have trouble asked for help with navigation or other signage. One resident (Resident 8) indicates: “I would go to a lot of things if they came and got me…they need to let me know because I can’t read the calendar.”
Other descriptions of the social impact of vision impairment point to recommendations for ALF staff to follow. For example, one resident (Resident 9) reported a situation that occurred in the dining room of the assisted living facility. When the resident was trying to interact with people at her dinner table and meet new people, she introduced herself at the table, only to have other residents tell her that they knew her already, and had just sat with her the previous evening. This respondent did not have dementia. She remembered people at the table, but simply could not see them. “This was so embarrassing,” she said. “Why couldn’t the nurse just tell me who was there? [so I wouldn’t be embarrassed].” This respondent went on to describe that this kind of scenario made her feel like she could not make friends, and discouraged her from trying. She also points out the potential role that staff could play in preventing or otherwise ameliorating this situation.
Assistive Devices
Most all residents interviewed (n=12) reported they used some assistive device to cope with their vision impairment, including magnifying glasses, large print books or audio books. Most respondents (n=11) were comfortable using these devices in public, and denied being self-conscious about using them. Respondents articulated frustrations around ease of use of the devices. Usability issues ranged from difficulty holding the device (i.e. when reading a book/newspaper), to reading faster than the magnifying glass would allow. One resident (Resident 7) conveyed that “[the device] causes as much trouble as it helps, so I quit using it.” Even when using large print books, some residents report that they could barely read the words or that they could not read for very long.
Respondents shared various experiences of seeking assistance for vision impairment, but many suggested that it was disappointing to them. Three residents reported that they and their families had made an effort to get the various devices offered at the local non-profit centre (e.g. large print calendars, special device to help them thread a needle, etc.). The most popular device was a bright bulb lamp. Many respondents (n=6) purchased the lamp and found it to be beneficial. However, problems occurred when necessary maintenance (e.g. changing batteries or bulbs) was not done. As a result, some residents were only able to derive benefit from the device for a limited time. One resident complained that the assistive device “just stopped working,” so they went on without it. The resident had not mentioned the non-working lamp to the nursing staff or family members. The problem was ultimately a burned out bulb in the lamp, which was later fixed (after the interview).
Discussion
This qualitative study contributes to the understanding of the day-to-day experiences of residents of assisted living with vision impairment. While every long-term care resident is unique, staff caregivers can improve their quality of care by having care recommendations informed by the accounts of residents themselves that describe their experiences of everyday life with vision impairment. Other works (19; 20) have reported the experiences of community dwelling older adults with vision impairment. The current study builds upon these and adds the unique contribution of qualitative feedback from older adults living in an assisted living setting.
The first objective of this study was to describe residents’ experiences of vision impairment. The vast majority of residents described the frustration over losing the ability to participate socially and to enjoy leisure activities as they once did. In some instances, it is clear that caregivers including ALF staff may have little direct knowledge of the ways that vision impairment is affecting specific residents’ daily experiences. Respondents described that most often it is the combination of overall health and vision impairment that impacts their social lives. This relationship between vision impairment and its impact on the social participation of long-term care residents appears to be related to co-morbidities and overall health. Other research has demonstrated an association between vision impairment among long-term care residents and social functioning, and suggested that co-morbidities could be influencing outcomes, although specific co-morbidities were not measured (24). This highlights an area for future research to identify the impact on social functioning of co-morbidities for long-term care residents with vision impairment.
The second objective of the study was to identify strategies for coping and adapting to vision impairment, including the use of assistive devices. Overall, respondents in the study employed an array of coping mechanisms, adaptations, and attempts to marshal support for their vision impairment. This array included some residents who took an active role in seeking help for vision impairment by working with their families to identify low vision assistive devices and rehabilitation at a local vision centre. Some residents found ways to adapt to the ALF physical environment (i.e. memorizing a path to get to a destination) and to the ALF social life in ways that accommodated their vision challenges. Still, some residents, with or without support from family, were not as active in seeking help or assistance for low vision. Some residents struggled with emotions and a negative outlook related to their vision impairment. This struggle is consistent with the literature (25) that describes an increased incidence of depressive symptoms related to vision impairment. Still, other residents showed resiliency through acceptance. While these respondents reported feelings of frustration with vision impairment, they reported coming to terms with the limitation and adapting their lives accordingly. Some reported emotional challenges with coping with these limitations, but were able to rely on other personal capabilities and social support. Residents noted vision-related challenges that they experienced in their living environment, including loss of prior valued activities and institutional barriers to social participation (e.g., inadequate signage which announces upcoming activities in their community, embarrassing social situations). Some residents shared advice on coping and adaptation that included accepting vision limitations, trying assistive devices whenever possible, and having assisted living staff intervene to help minimize the negative social impact of vision impairment.
The third objective of this study called for educational and training suggestions for long-term care staff and caregivers to improve quality of care for elder long-term care residents with vision impairment. As there is an increasing number of older adults who are living with vision impairment in long-term care settings (including ALF settings), it is imperative that caregivers and clinicians have educational and training materials that are informed by direct accounts and feedback of older adults in this population. Results suggest at least four distinct recommendations that emanate from residents’ accounts and that are salient to the education and training of caregivers in ALF and other long-term care settings, with the goal of improvement of quality of life and appropriateness of care of older adults in these settings (see Table 2).
First, residents’ accounts suggest that caregiving staff should evaluate the adequacy of signage, activity calendars, menus, and other written announcements in the long-term care setting, and not assume that all residents with vision impairment are able to benefit from these important aspects of the social environment. Font size, colour, clarity of wordage, and placement of announcements, as well as lighting, must also be considered (e.g., do some residents use wheelchairs? Is signage readable from this view?) as part of an ongoing assessment of the adequacy of the social environment’s signage by ALF staff. Second, staff should proactively and routinely initiate conversations with residents about any assistance they may need, including to give them another opportunity to attend events, as residents may need encouragement and help. This care practice ought to include ongoing and routine inquiries by ALF care staff about residents’ vision, including whether they are experiencing vision changes or otherwise might need evaluation or assistance. Third, residents with vision impairment recommended that staff discreetly let them know who is sitting with them at a meal or social event, in order to avoid a socially awkward or embarrassing interaction of not knowing who is around them due to vision challenges. These suggestions by residents highlight the potential role ALF staff can play in ameliorating the immediate social consequences of vision impairment of residents, if ALF staff are both aware of the vision status of residents and encouraged by their employer to be observant and proactive during social events. Lastly, caregiving staff should actively inquire with the resident and/or family members about the maintenance and upkeep of assistive devices for vision impairment. For example, a lamp may be providing much needed assistance to the resident, so care staff ought to ask about the status of this assistive device, and bulbs and batteries should be stocked and able to be changed when necessary. While this can seem obvious, this is not a routine request or responsibility of staff caregivers. As residents come to rely upon additional assistive and technological devices, routine maintenance — ranging from changing batteries to updating software — will become more important in supporting the care needs of older adults.
Overall, visual health and assistance should become part of the regular and ongoing conversation staff and family have about the well-being of the resident, and deliberate communication about vision experiences and needs on the part of ALF care staff ought to be encouraged as a priority by administrators of ALF. Houde and Huff recommended that gerontological nurses describe assistive devices to their residents and encourage vision rehabilitation to increase the number of older adults who are more aware of and are actively using visual aids (26). Moreover, caregiving staff should assess all residents for new or progressive symptoms of visual impairment, as well as recommend annual physical assessments of residents with low vision (26).
These recommendations for staff are supported by other research in the literature. Simple institutional and environmental changes include evaluations of both adequacy of signage and increased lighting. Larger font sizes, bolder print, colour contrast, and thoughtful placement of signage to include accessibility to residents with vision impairment who use wheelchairs are all suggestions for easy but impactful institutional changes (27). Beyond navigation benefits, increased lighting levels and visual contrast in table settings in long-term care dining areas has been associated with improved oral intake of food as well as improvement in functional abilities (28). Moreover, the National Institute on Aging suggests that there ought to be bright and adequate lighting when interacting with older adult residents who may have vision impairment (29). This recommendation is a strategy to reduce barriers to communication between clinicians and their patients in long-term care.
Worldwide Application of Findings
Findings from this study have direct application to caregivers of older people with vision impairment worldwide. Specifically, the findings are a call for a renewed sensitivity to consider the situational dynamics of older adults with vision impairment who are also living in a long-term care setting or ALF, and a call to solicit the accounts of daily life experiences directly from older adults. Despite the fact that long-term care facilities around the world differ in their cultural approaches and structures, the recommendations in this report are indicative of a need to re-examine care patterns to older adults with vision impairment living in long-term care or within the community. The recommendations can be applied globally, with some degree of variety, including: modifying the environment where necessary (e.g. signage), modifying techniques when trying to encourage residents to be more socially engaged (i.e. letting them know who is sitting next to them); being sensitive to frustration over loss of ability; and proactively discussing and supporting any changes in vision status and positive adaptation a resident may want to make (i.e. using assistive devices). All of these personal and institutional recommendations highlight the prominent role that larger social structures play as they scaffold the daily experiences of elders in ALF. On-site physician services, routine vision screenings, and low vision rehabilitation services ought to be priority health care services within ALF.
One limitation of this study is that it is based on a small, homogenous sample size (n=13) and uses a convenience sample, which makes it inappropriate to generalize these findings to the entire population of assisted living residents who experience vision impairment. Still, valuable first-hand accounts by residents who live with vision impairment in long-term care may help to inform strategies globally for improving quality of care for older adults.
Conclusion
While this small-scale study is limited in its ability to suggest causal relationships, it suggests through vivid and lived experiences of elders themselves several effects vision impairment has on residents’ experiences in assisted living in the US context. Findings point to specific and relatively easy practical changes in care practices and institutional settings that could provide more support for residents with vision impairment, improve their quality of life, and strengthen their care plans. This work also provides a basis for future research. Visual impairments, and the great array of potential environmental modifications and devices to assist those with visual impairments, may be potent and often ‘unseen’ influences that underlie quality of life and quality of care for long-term care residents. Visual health of residents should be taken seriously, measured, and analysed, and additional personal and institutional adaptations should be outlined. The value of this study’s qualitative approach lies in hearing from the residents themselves. Their responses highlight the impact visual health has on residents’ daily experiences in long-term care, and the complex potential connections between vision impairment and co-morbidities. These can often go unrecognized, and may be falsely conflated with depression and dementia. For those who are intent to improve the quality of life and care of long-term care residents — from administrators to clinicians to loved ones to residents themselves – visual health assessment and assistance deserve more systematic attention.
Conflict of interest: None.
Ethical standards: These have been met.
References
1. World Health Organization, 2014. Ten facts on aging and the life course. World Health Organization. Retrieved from http://www.who.int/features/factfiles/ageing/en/
2. International Federation on Ageing, 2012. The high cost of low vision. International Federation on Ageing. Retrieved from http://www.ifa-fiv.org/wp-content/uploads/2013/02/The-High-Cost-of-Low-Vision-The-Evidence-on-Ageing-and-the-Loss-of-Sight.pdf
3. Center for Disease Control and Prevention, 2013. Vision health initiative: Fast facts. Center for Disease Control and Prevention. Retrieved from http://www.cdc.gov/visionhealth/basic_information/fast_facts.htm
4. Deremeik, J., Broman, A.T., Friedman, D., West, S.K., Massof, R., Park, W.… Munoz, B. Low vision rehabilitation in a nursing home population: The seeing study. Journal of Visual Impairment & Blindness, 2007;101 (11), 701-714.
5. Lighthouse International, 2013. Projected estimates of vision impairment. GuideStar. Available at http://li129-107.members.linode.com/research/statistics-on-vision-impairment/projected-estimates/.
6. Elliot, A.F., Dreer, L.E., McGwin Jr, G., Scilley, K. & Owsley, C. The personal burden of decreased vision-targeted health-related quality of life in nursing home residents. Journal of Aging and Health, 2010;22 (4), 504-521.
7. Horowitz, A., Balistreri, E., Stuen, C. & Fangmeier, R. Visual impairment and rehabilitation needs of nursing home residents. Journal of Visual Impairment & Blindness, 1995;89 (1), 7-15.
8. Marx, M., Werner, P., Cohen-Mansfield, J. & Feldman, R. The relationship between low vision and performance of activities of daily living in nursing home residents. Journal of the American Geriatrics Society, 1992;40, 1018-1020.
9. Freeman, E., Munoz, B., Rubin, G. & West, S. Visual field loss increases the risk of falls in older adults: The Salisbury eye evaluation. Investigative Ophthalmology & Visual Science, 2007;49 (10), 4445-4450.
10. Rovner, B., Zisselman, P. & Shuely-Dulitzki, Y. Depression and disability in older people with impaired vision: A follow-up study. Journal of the American Geriatrics Society, 1996;44, 181-184.
11. Girdler, S., Packer, T.L. & Boldly, D. The impact of age-related vision loss. Occupation, Participation, and Health, 2008;8 (3), 110-119.
12. Stone, T., Santo, J. & Wittich, W. Mediating and moderating effects on the association between vision loss and depression among an older population. Insight: Research and Practice in Visual Impairment and Blindness, 2012;5 (1), 30-36.
13. Gellis, Z.D. & McCracken, S.G. 2008. Depressive disorders in older adults. In S. Diwan (Ed.), Mental Health and Older Adults. Retrieved from http://www.cswe.org/File.aspx?id=23509
14. Rovner, B., & Casten, R. Depression and cognitive disorders in patients with AMD. In H.P.N. Scholl, R. Massoff, & S. West (Eds.), Essentials in Ophthalmology (A. Singh, Series Editor): Ophthalmology and the Ageing Society, 2013;pp. 207-215). Berlin, Germany: Springer-Verlag.
15. Kempen, G., Verbrugge, L., Merrill, S. & Ormel, J. The impact of multiple impairments on disability in community-dwelling older people. Age & Ageing, 1998;27 (5), 595-604.
16. Sinoo, M.M., Kort, H.S.M. & Duijnstee, M.S.H. Visual functioning in nursing home residents: information in client records. Journal of Clinical Nursing, 2012;21(13/14), 1913-1921.
17. Cacchione, P. Nursing care of older adults with age-related vision loss. In S. Crocker Houde (Ed.), Vision Loss in Older Adults: Nursing Assessment and Care Management, 2007;pp. 142-143). New York, NY: Springer.
18. Medicare.gov: The Official U.S. Government Site for Medicare, 2015. Your Medicare coverage: Eye exams. U.S. Government. Retrieved from http://www.medicare.gov/coverage/eye-exams.html/
19. Kleinschmidt, J.J. Older adults’ perspectives on their successful adjustment to vision loss. Journal of Visual Impairment & Blindness, 1999;93(2), 69-81.
20. Teitelman, J., & Copolillo, A. Psychosocial issues in older adults’ adjustment to vision loss: Findings from qualitative interviews and focus groups. American Journal of Occupational Therapy, 2005;59, 409-417.
21. Sandelowski, M. Focus on research methods: Whatever happened to qualitative description?. Research in Nursing & Health, 2000;23, 334-40.
22. Folstein, M.F., Folstein, S.E. & McHugh, P.R. Mini-mental state: A practical method for grading the cognitive state of patients for the clinician. Journal of Psychiatric Research, 1975;12 (3), 189-198.
23. Bradley, E., Curry, L. & Devers, K. Qualitative data analysis for health services research: Developing taxonomy, themes, and theory. Health Services Research, 2007;42 (4), 1758-1772.
24. Dev, M.K., Paudel, N., Joshi, N.D., Shah, D.N & Subba, S. Psycho-social impact of visual impairment on health-related quality of life among nursing home residents. BMC Health Services Research, 2014;14, 345.
25. Horowitz, A. & Reinhardt, J.P. Mental health issues in vision impairment: Research in depression, disability, and rehabilitation. In B. Silverstone, M.A. Long, B.P. Rosenthal & E.F. Faye (Eds.), The Lighthouse Handbook of Vision Impairment and Vision Rehabilitation, 2000;pp. 1089-1090). New York, NY: Oxford University Press.
26. Houde, S.C. & Huff, M.A. Age-related vision loss in older adults: A challenge for gerontological nurses. Journal of Gerontological Nursing, 2003;29 (4), 25-33.
27. Shura, R., Siders, R. & Dannefer, D. Culture change in long-term care: Participatory action research and the role of the resident. The Gerontologist, 2011;51 (2), 212-225.
28. Brush, J.A., Meehan, R.A. & Calkins, M.P. Using the environment to improve intake in people with dementia. Alzheimer’s Care Quarterly, 2002;3 (4), 330-338.
29. National Institute on Aging, National Institutes of Health, Department of Health and Human Services, 2008. A Clinician’s Handbook: Talking with Your Older Patient. U.S. Department of Health and Human Services. Retrieved from http://www.nia.nih.gov/sites/default/files/talking_with_your_older_patient.pdf