I. Syed1, T. Daly1, P. Armstrong2, R. Lowndes2, M. Chadoin3, V. Naidoo1
1. York University Department of Health Policy and Health Equity, Toronto, Canada; 2. York University Department of Sociology; 3. Université du Québec à Montréal, Interdisciplinaire en Santé et Société, Toronto, Canada. Corresponding author: Iffath U.B. Syed, MPH, PhD Candidate, York University, 4700 Keele Street, Toronto, Ontario, M3J 1P3, Canada, (416)-835-8418, iusyed@yorku.ca
Abstract
Background: According to the Canadian Health Care Association (1), there are 2,577 long-term care (“LTC”) facilities across Canada, with the largest proportion (33.4%) located in Ontario. Most studies focus on residents’ health, with less attention paid to the health and safety experiences of staff. Given that the work performed in Ontario LTC facilities is very gendered, increasingly racialized, task-oriented, and with strict divisions of labour, this paper explores in what ways some of these factors impact workers’ experiences of health and safety. Objectives: The study objectives included the following research question: How are work hierarchies and task orientation experienced by staff? Design and Setting: This paper draws on data from rapid team-based ethnographies of the shifting division of labour in LTC due to use of informal carers in six non-profit LTC facilities located in Toronto, Ontario. Methods: Our method involved conducting observations and key informant interviews (N=167) with registered nurses, registered practical nurses, personal support workers, dietary aides, recreation therapists, families, privately paid companions, students, and volunteers. Interviews were audio-recorded, transcribed verbatim, and thematically analyzed. For observations, researchers were paired and covered shifts between 7 a.m. and 11 p.m., as well as into the late night over six days, at each of the six sites. Detailed ethnographic field notes were written during and immediately following observational fieldwork. Results: Our results indicate that employee stress is linked to the experiences of care work hierarchies, task orientation, and strict divisions of labour between and among various staff designations. Conclusion: Findings from this project confirm and extend current research that demonstrates there are challenging working conditions in LTC, which can result in occupational health and safety problems, as well as stress for individual workers.
Key words: Qualitative methodologies, long-term care, nursing homes, carers, safety of staff, stress and coping, health.
Introduction
The problems of task orientation and a strict division of labour are increasing concerns for many workplaces, including nursing homes. A strict division of labour refers to the allocation of tasks that are divided between groups in the care work force on the basis of skill, education, or job classification, and it means that the work is boundaried, highly regulated, and formalized (2). In conjunction to this type of work division, task orientation often involves heavy staff workload, high intensity work that occurs in assembly-line fashion, and limitations in how much time that workers have to carry out their duties (2). We define task orientation as work that is highly focused and prioritized on the completion of tasks, without adequately considering the outcomes of the tasks completed. For example, in Canadian LTC environments, dining might be completed at the posted time, baths are given when posted, but these do not necessarily occur in reference to the individual needs of the residents, but rather according to a work schedule that breaks down care into discreet tasks (2).
Task orientation combined with a strict division of labour can modulate the wellbeing of staff by inducing stress (2), and may impact the occupational health and safety of workers, while reducing productivity or efficiency of the work that is to be completed. The effects of stressful working conditions are known to be detrimental to workers’ occupational health and safety (3), and can induce a neurological flight or fight response, release adrenocorticotropic hormones, as well as elevate plasma lipids and blood pressure (4, 5). Task orientation stands in sharp contrast to relational work. Relational work involves co-operative task sharing, more flexible regulations, limited restrictions on work, and increased work autonomy (6). Relational work is beneficial to workers through stress reduction, and beneficial to residents through improvements in their care needs (2).
Previously it was reported that the large size of Canadian LTC facilities, increasing numbers of frail residents with complex needs, and low staffing levels all lead to task orientation and high levels of stress among workers, which is in sharp contrast to relational work found in the Swedish LTC environments (2). Canadian LTC workers reported that their work involved a strict division of labour, was arranged in an assembly line fashion, and that there was frequent downloading of tasks (2). For example, Canadian care workers seldom carried out cleaning, cooking, recreation, and social activities. They usually relied on a specialized workforce such as: housekeepers, dietary aides, and recreation or activation therapists for these duties respectively. On the other hand, in the Swedish LTC facilities, Swedish care workers reported that they carried out a variety of these tasks, including cleaning of the residents’ rooms/apartments, and social activities such as accompanying residents on errands outside of the facility, or chatting and having a cup of coffee with residents (2).
Adding to these notions of strict divisions of labour and task orientation is the presence of work hierarchies. Work hierarchies are defined as unequal social relations that are embedded in and produced (or reproduced) through historical and contemporary organization of particular spaces (7, 8). Work hierarchies can be understood in the context of Canada’s urban work centres, in which there is organization of social relations such that high levels of power, privilege, and class is concentrated at the top with managerial positions and executive roles, and this power diffuses down significantly towards the bottom of the hierarchy and at the front-lines, with the latter positions often being racialized (9).
Strict divisions of labour, task orientation and work hierarchies may have an intensifying effect in reducing workers’ occupational health through psychosocial factors in the organization. Psychosocial factors in the work environment refer to: job demand, job control, social support, time pressure, degree of monotonous work, extent of social reciprocity (or effort-reward balance), autonomy, fairness, job security, as well as social contact between co-workers and supervisors (4, 5). Samra, Gilbert, Shain, and Bilsker (10) have developed 13 factors contributing to psychosocial health: workload management, psychological support, organizational culture, clear leadership and expectations, civility and respect, psychological job fit, growth and development, recognition and reward, involvement and influence, engagement, balance, psychological protection, and protection of physical safety (11).
Job demand and job control are two types of psychosocial factors that are often associated with social attitudes of staff, and can affect their health through the modulation of stress and anxiety among workers (12). Job demand factors refer to workload, time pressures, work surges, work pace, or rest breaks; while job control factors refer to level of influence on work, level of participation in decisions, job satisfaction/dissatisfaction, and level of social support (12, 13, 14). High job demands and low control, which includes low levels of social support, have been associated with a high prevalence of cardiovascular disease (15, 16). Additionally, these factors can induce stress and strain (14, 17, 18), contribute to the development of musculoskeletal disorders (13, 19, 20) and affect mental health (21) by inducing anxiety and depression among workers (22, 23).
Previous research shows that LTC workers experience highly task-oriented work that responds to pre-determined schedules, strict divisions of labour, and psychosocial factors in ways that adversely impact their health and safety (24). Armstrong et al. (24) found that LTC workers have less control over their workday, have high levels of stress, and frequently experience work-related violence. Zaman (8) found that workers involved in care-giving duties often reported high workload that demands long working hours, and other adverse psychosocial factors such as the lack of opportunity for work autonomy; the participants also reported high levels of job dissatisfaction, job stress, and musculoskeletal pain (8).
Both strict divisions of labour and work hierarchies can involve unequal distribution of power and privilege, and unbalanced social relations in everyday encounters. Connecting power relations and racism, Agnew (25, p. 8) reports, “racialization is a process that occurs in the context of power relations, whether it is in discourses, systemic to structures and institutions, or merely a matter of everyday encounters”. Borrowing from Agnew (25), we analysed LTC workplaces as sites of potentially sharply divided work and work hierarchies.
We also note that LTC work is increasingly gendered and racialized, and also a source of employment for migrant and racialized workers, whose other jobs skills are under-recognized in the Canadian job market (26, 27, 28, 29, 30, 31). Therefore, focusing research and data analysis on these and other work spaces, as well as using gender, immigrant status, culture or race lenses, and connecting these to acute and chronic health effects is increasingly important and is a relatively under-researched area (32).
Methods
This umbrella study is part of a larger project funded by the Canadian Institutes of Health Research, headed by the Principal Investigator Dr. Tamara Daly and used rapid team-based ethnography with a feminist political economy framework to understand the organization, policies, procedures, and characteristics of long-term care in Ontario. Six case studies were analyzed. The focus was on the intersection of formal and informal care work and the health consequences of it. Feminist political economy is concerned with the inequity that results from gendered stereotypes, roles, and ideas about women, tensions related to women’s paid and unpaid work, and the importance of how material conditions affect women’s lives (29, 33, 34). Rapid team-based ethnography is an innovative, multi-method ethnography in which interviews and observations are conducted over short periods of time collectively by a team of researchers (35).
In this project, we investigated the relationship between formal and informal paid care provision in long term care, and sought, among other things, to explore work hierarchies and the division of labour. For this part of our study, the objectives included the following research questions: What are the tasks performed by paid employees across the various LTC sites? What (if any) divisions of labour or task sharing (i.e. relational work) are evident? Is there evidence of power and privilege dynamics? Are social relations equal / unequal? Are work hierarchies present? Is task performance connected to social relations (and work hierarchies)? How do the paid staff experience divisions of labour, work hierarchies, and related psychosocial factors? What is the impact on employees’ occupational health and safety?
This study was part of a larger project in which a team of researchers conducted rapid ethnographic case studies in six non-profit LTC facilities located in Toronto, Ontario. Sites were characterised as having 100+ beds, publicly funded, and they were either non-denominational or held religious affiliation. Some of the sites were contracting out services such as food, laundry, management to for-profit operators, and three out of six had retirement homes associated with their organization. We conducted observations on secure (locked) units and in public spaces (e.g. dining spaces, recreations spaces, atriums, and outside grounds).
We conducted key informant, semi-structured interviews (N=167) with managers, health care providers, family members, students, companions and volunteers, as well as week-long participant observations, during which researchers were paired and covered shifts between 7 a.m. and 11 p.m. (and often into the night) over a six-day period at each of the six sites. Detailed ethnographic field notes were written both during and immediately following observations. Individual interviews were conducted face to face, in a mutually agreed upon location at a time that was convenient for the participants in a private location away from the formal work environment, such as in meeting or boardrooms within the organization. Recruitment for sites was conducted by the Principal Investigator. Interviewees were either identified by the facility or recruited directly by researchers using snowball methods, and facilitated through posters of the study or brochures that were handed out by the researchers. Ethical approval was obtained from York University Office of Research Ethics and Université du Québec à Montréal, and informed consent was read and signed by participants prior to their participation in interviews. During field observations, members of the research team also approached staff, volunteers, and families, and conducted informal interviews after informed consent was obtained and ethics paperwork were read and signed by the participants. Interviews were audio-recorded and transcribed verbatim. Interview data and field notes were thematically analyzed using N-Vivo software.
For the purposes of this paper, we collected detailed descriptions of the various types of tasks performed by each of the categories of paid staff. We then examined whether or not the patterns of task performance was indicative of task sharing (relational work) or of task orientation. We also collected information about psychosocial factors such as workloads, work intensity and surges, adequacy of time to complete tasks, staffing adequacy, etc. We did not assess volunteer, family or unpaid staff work or other work hazards within this part of our study, as these groups and aspects of occupational health and safety were carried out as a part of a series of separate parallel studies (36).
Findings
Divisions of Labour and Human Resource Constraints
We summarized our observations for a variety of tasks performed by paid workers. These workers were categorized as follows:
1) Nurses: registered nurses (“RNs”) / registered practical nurses (“RPNs”);
2) Personal support workers (“PSWs”): care aides (“CAs”) / health care aides (“HCAs”);
3) Support staff: dieticians, dietary aides, recreation therapists, restorative care aides, holistic aides, and cleaners, maintenance workers, or housekeepers.
We observed a number of tasks performed by each of the aforementioned workers, as illustrated by this table. For example, documentation and dining were carried out by all three categories of workers. Although we indicate that dining and documentation were carried out by all three staff categories, we note that there were certain variations in the work. For example, specific types of documentation were only completed by certain staff. For instance, PSWs documented the entirety of dining-related work, although nurses and support staff assisted in the dining room. We also observed that this type of work was often carried out at specific and posted times. Therefore, this particular key activity was interpreted as having a strict division of labour and as being task-oriented work.
Four domains of work were found to have particularly strict divisions of labour and were task oriented: 1) dispensing of medications, which was carried out by nurses; 2) socialization activities (such as celebrations of birthday parties, and organization of pub nights), 3) recreational activities (such as music and game activities) which were both carried out by support staff; and 4) direct care (toileting, showering, grooming), which was carried out by PSWs (Table 1).
Our key informant interviews reconfirmed some of our observations at the worksites about the nature of the tasks that are performed by particular workers, and that these workplaces can be highly task-oriented environments with strict divisions of labour. Workers sometimes directly communicated these experiences as exemplified in the following quotes:
A: “For me I have to do the charting, the flow sheets. I have to do the computer […] We don’t lift up the heavy stuff.
I: “You mean so you’d have like the orderly you mean to push around people?”
A: “Yes. Not push around. Empty the linen.”
I: “Oh. You mean like maintenance and housekeeping and all that.”
A: “Yes. We don’t empty the linen, you know, like the dirty linen. They [cleaning / other staff] do that for us.” – PSW1, Site 4.
For nurses, they have key responsibilities such as dispensing of medication. Further, this quote highlights the nurse’s expressed feelings of being overwhelmed by the number of responsibilities, and being expected to do more:
I: “So do you want to tell me anything else? […]”
A: “Because I think here if you’re a nurse on the floor you have lots, it’s your responsibilities beyond the medication […] And sometimes I think that we already have lots of tasks and they, our superiors, are expecting more from us. Like we already have lots.” – RPN 1, Site 3
For the food servers and dietary aides, rigid divisions of labour were also observed, as indicated by Table 1. Interviews with support staff, such as maintenance personnel and housekeepers, also provided evidence of strict divisions of labour, and interestingly it was maintained systematically through power relations and work hierarchies stemming from persons holding authority over their work, such as a supervisor:
I: “So talk to me about what you do on a daily basis.”
A: “I’m a housekeeper so I come in and I clean the second floor[.] I also clean first floor, the main floor[…]The office part. Every morning[…]We have three rooms a day [for] general cleaning. And then after we’re done those three rooms we go along and we clean every bathroom of the residents, floors and bathrooms[…]and then work yourself around doing the activity rooms[…] Plus two kitchenettes. From time to time [my supervisor will] ask me if I’ll do the lunchroom. There’s a lunchroom for staff.”
I: “And what about vacuuming? Do [PSWs] do that?”
A: “No. I do the vacuuming.
I: “You do it?”
A: “Yeah. I do the vacuuming and I bring up the linen.”
I: “Okay, the heavy cart.”
A: “Yes. I take the cart down before I go for break and then bring it up.”
I: “So do you feel as though […] you work more with the other housekeepers or do you work more with the PSWs on this floor?”
A: “I like working as a team but she [the supervisor] doesn’t allow us to.”
I: “Really? Talk to me about that. What do you mean?”
A: “No, she doesn’t. Like if I’m up here and a resident needs my help…”
I: “Yeah.”
A: “[…]if she [the supervisor] comes up and she sees me [helping a resident] ‘Well that doesn’t belong to your job. Just do what’s part of your job.’ It’s always about what’s part of my job. She doesn’t want us to do anything that’s part of their [the PSW’s] job.” – Housekeeper, Site 1
Interviews with recreation therapists also addressed the division of labour, in which one worker expressed disappointment in doing extra work, in this instance assisting with dining:
“They don’t tell us in the job description [about dining]. I would say ‘Oh, you didn’t tell us we would have to do meal partnering.’ Well it’s under ‘All other duties’, right?” – Recreation Therapist, Site 5
One recreation therapist confirmed how she does not do certain tasks such as toileting and dispensing of medication but confirmed that she does undertake recreation-related documentation.
“I don’t have to toilet people, I don’t give medications…I think we’re given 30 minutes to document, 15 to 30 minutes…I will help [PSWs] bring them to the toilet… I’m not trained on the lift so I can’t help you if it’s a lift. To wipe them I’m not qualified technically. I haven’t been trained for that.” – Recreation Therapist, Site 3
Another recreation therapist indicated details of the recreation activities she coordinates with residents, including: music, concerts, performances, theater, drama, dance, poetry, and games.
I: “So what is it that you do here?”
A: “Okay. So I’m a recreation therapist so generally what our profession does is take activities that are interesting to people so leisure and recreation activities and help to use that as a form of therapy […] I’m responsible for central recreation so I coordinate all the programs that don’t happen on any particular floor that are open to clients on all the floors […] A lot of my programs will revolve around music and concerts. Games based. They could be board games, card games, bingo, that sort of thing. They could be arts based. Tonight we have a theatre performance coming in and they could be around any kind of theatre, drama, poetry, dance.” – Rec Therapist, Site 4
Previous studies have pointed out that in Canadian LTC work, task orientation and strict divisions of labour are features of work environments that have both human resource shortages and demonstrated time constraints (2). The results of our key informant interviews with workers suggest that staff shortages and heavy workloads are an endemic feature of the LTC facilities we visited. One RPN stated:
“We’re often short staffed here and this is a heavy floor because a lot of residents are in wheelchairs. A lot of times I’m really in there helping them and helping them with transfers.” – RPN 2, Site 3
At another site, a PSW echoed the same difficulties of staff shortages and connected it as a barrier to focusing on residents’ care:
“They keep saying focus on the residents’ care. But how could you focus on the residents’ care? You tell me. It’s easier said than done. To say that okay, we focus on the residents’ care but how if you don’t have the staff?” – PSW 1, Site 4
Our findings also indicate that strict divisions of labour combined with being over-worked involves prioritizing care duties and trading-off of certain duties over others, which is often accompanied by rushing and assembly line style of work. Workers communicated these complexities in interviews:
I: “Can I ask you a quick question? When I was walking around with you I noticed often that people interrupt you.”
A: “Mmhmm.”
I: “You’re in the middle of doing one thing and people are pulling you in to do other things.”
A: “Yeah.”
I: “Is that frustrating?”
A: “It’s frustrating but you have to try because as I said after working here for years you have to try your priority. But I am not afraid to. I try to make my judgement which is…”
I: “Which is more important.”
A: “[…] We have priorities. We have to always tell them ‘We have 28 residents and every resident has needs. Some more than others, so as a staff I have to make my priorities. Which is more priority? I have to prioritize my priority. Who needs me more than…?’ You know.” – PSW1, Site 4
The same PSW said earlier in the interview:
A: […] But the time is the problem. We don’t have the time anymore. And even with the feeding you see […] you have to put them in the table like, you know.”
I: “Like an assembly line. You’re sort of showing how you…”
A: “Like assembly line. But you have to improvise. As I said, you know, it’s not right. This is what I said to them [management]. It’s inhuman.”
Another PSW stated:
“And then I’m rushing through my residents to help them so we can get to dinner and all this and, you know, time constraints and all that kind of stuff it can be quite frustrating […] You know, this is not a factory. This is not a factory job. It’s not an assembly line.” – PSW 2, Site 4
Our analysis of the tasks performed and the division of labour delineate four important points. First, there are indeed strict divisions of labour and task orientation with workers being highly focused on their specific duties. Despite this, in some instances workers expressed their willingness to do extra duties. Secondly, the divisions of labour were sometimes maintained systematically through power relations and work hierarchies between and among workers. The above interview with the housekeeper at Site 1 provides an eloquent example of how a supervisor maintained hierarchical authority over the housekeeper’s work, and how there is a lack of work autonomy because of pressures from those in charge. Thirdly, the quote from the housekeeper also demonstrates how direct resident care that could be provided by cleaners is discouraged; and how cleaning tasks are prioritized over relational care. It could also be indicative of quality of care that could otherwise be improved if the housekeeper had the autonomy to focus on residential care. Fourthly, time limitations, staff shortages, rushing, and assembly line style of work continue to be a feature of Ontario LTC facilities.
Previous survey research of LTC workers demonstrates average Canadian staff-to-resident workloads of 1 assistant nurse per 33 residents (1:33) and 1 direct care worker per 15 residents (1:15), taking all three shifts into account (2). Our study demonstrates variable workloads and staff-to-resident ratios, depending on the time of day. In the nursing homes we observed, there were between 8 and 12 residents per PSW, and 24 to 32 residents per RPN on the day and evening shifts. These numbers changed dramatically during the late night shifts, when it was more common to have 1 PSW per unit/residential wing of 24 to 32 people and a shared RPN for between 50 and 64 residents. These numbers should be interpreted with caution; however, as the presence of staff and hours worked may not necessarily reflect hours paid, and workers may be engaged in unpaid or overtime work to meet job demands.
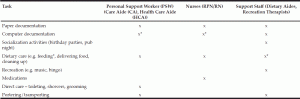
Table 1 This table lists various tasks carried out during a typical workday at six long-term care sites in Toronto. A presence of an x denotes that a particular group of workers carried out a specific task, whereas an absence of an x indicates that workers did not participate in or carry out this work
* indicates that not all staff allowed to carry out this task (e.g. dietary aides would not feed at most sites)
Evidence of Work Hierarchies
Our evidence of work hierarchies between different job categories was conveyed in interviews with several workers who described and identified unequally balanced social relationships within the workplace. These relations also intersect race or visible minority status. For example, one PSW, who is racialized, expressed that the responsibility for transferring residents is a shared one, and that if there is a need, a manager should be willing to assist a PSW with a transfer, and they should not consider their position as a manager to be above the needs of the residents:
“Even if you’re the manager and I need help with a resident because that’s what we’re here for, you shouldn’t be too high to come and transfer me with somebody.” – PSW 1, Site 3 [emphasis added].
At another site, one RN expressed hierarchies between herself and a PSW:
“There’s lots of hierarchy, right? And then you get into okay, well I’m Filipino and I’m an RN, you know. That puts me higher than a Filipino PSW” – RN2/Unit Manager, Site 4
Our key findings about work hierarchies in LTC indicate the existence of social positioning among various occupations. In the first example, the PSW describes the perceived ‘high’ social position of the manager. At the same time, the PSW also expects the manager to help him in his PSW-related duties. In the second example, the RN, who is also a racialized worker, talks about her perceived ‘higher’ social position to someone of the same race, who is a PSW, a designation that she perceives to be below hers. It is plausible that inequalities in social positioning could have the potential to perpetuate strict boundaries around tasks by discouraging task sharing. We further explored potential impacts of strict divisions of labour, work hierarchies and other factors for workers’ health.
Evidence of Adverse Psychosocial Factors and Occupational Health Issues
In order to examine work-related morbidity and job stress, we asked staff about their work experiences, including work intensity, workload, and other psychosocial characteristics of their job. The responses conveyed a broad range of issues such as: feelings of under-appreciation among staff, job stress, surrender, tension, guilt, anger, resentment and resignation, and even incidences of bullying in the workplace.
“You know, they [the PSWs] do feel under-appreciated sometimes. They feel like they’re not being paid enough, that nobody cares what they say or what they think, the management is not listening. You know, I hear them daily complaining about little things like that.” – RPN 2, Site 3
One worker expressed that LTC work is complex, and is not as simple as a matter of money or customer service:
I: “It’s that bad?”
A: “It’s that bad. Yeah. […] We’re getting paid to do a job and we know what we got into. This is not working in customer service at the McDonald’s. This is more than that, right? And personally how I feel, if I can’t do it, I’m gone. Not because of the money. And [with] a lot of people you get that. And it’s sad.” – PSW 1, Site 1
Workers expressed their experiences of stress:
“[…] I can’t be running around like a monkey. It’s just too much for me and I was just running around and getting too stressed.” – PSW 2, Site 4
Workers also expressed their experiences of bullying, and how it was affecting them and many others:
I: “So is it, is she [the supervisor] too strict?”
A: “Yeah, she is very strict. Very strict. And we’re under a lot of stress here. […] they just let her do what she wants, you know, and she bullies everybody. Everybody. I’m not just saying about me. It’s everybody. She’s very hard on everybody. […] There was actually people, they even cried about certain things she did. And it was worse for us.”
I: “After. It didn’t get better.”
A: “It didn’t get any better. She came up with work assignments with a lot more work just to get back at us […] And if she comes up to the floor and she don’t see me she’ll look for me. She’ll go in each room. If you’re in the bathroom she’ll stand outside the bathroom.”
I: “Oh. That’s even more embarrassing.”
A: “Yeah. But she won’t do it just to me. She’ll do it to everybody.”
I: “So you don’t feel like you’re alone in that.”
A: “No.”
I: “You all feel as though this is something that’s a shared experience.”
A: “Yeah. And it’s getting out of hand. She talks to people the way she feels like it. She screams at people.” – Housekeeper, Site 1
Other workers communicated feelings of guilt:
“For me like sometimes I feel so guilty… because I’m very conscious of my job […] I know that I shouldn’t be. But I feel it because, you know, after working with them for so many years they become a part of you. They become your family. Like they’re a part of your family. You know, like if they’re hurting you hurt.” – PSW 1, Site 4
LTC workers experience a wide variety of stressors in relation to their work environment. Workers such as PSWs felt under-appreciated and had feelings of low self worth. Other members of the staff such as RPNs also exhibited these feelings. Further, there were sources of worker stress due to instances of bullying as exemplified above. Next, we sought to determine how some of these circumstances would manifest themselves in behavioral responses and compensatory mechanisms in carrying out LTC work.
Sometimes the adverse psychosocial factors described in the above examples resulted in behavioral responses that might exacerbate adverse working conditions. This might also impact occupational health of workers and put workers at risk of harm. For example, workers communicated that they either willingly or unwillingly trade off their break periods in order to continue care for residents.
“Sometimes I sacrifice myself. I sacrifice my break. I don’t go for my break and I said for so many years [Site 4] must owe me a lot of money for not having a break. But I don’t want to tell the right hand what my left hand is doing, you know […] I’m not exaggerating. I have to sacrifice myself. It’s me. People are not going to do that. They’re going to go for their break and so what happens? The care is even going to be…
I: “Lower.”
A: “…Lower.”- PSW 1, Site 4
Others stated that they are unable to have adequate rest periods and bathroom breaks:
“We can’t be able to pee. We always watch them [the residents], where are they and what they’re doing […] So even our boss she kept on reminding because I work with her and she was an RN here before. She said we have to watch them constantly.
I: “Do you feel you can take your breaks? Do you get your breaks?”
A: “[…] Oh break is always questionable in this area.”
I: “You need your break.”
A: “We need our break. […] I mean you need a gap to relax, unwind yourself.” – PSW 2, Site 1
From this part of the study, it is indicated that workers exhibit stress responses, which can be counterproductive for their own health and wellbeing. As suggested above, they may trade off their rest periods in order to compensate for time constraints in their work.
Discussion
Job demand and job control factors have been increasing due to high workloads for employees in LTC (37). These circumstances can have profound impacts on occupational health and safety of staff. Job demand factors such as workload, time pressures, work pace, rest breaks, or work surges; and job control factors such as level of influence on work, perceived lack of participation in decisions, job satisfaction, and social support can all lead to either increased risk of occupational morbidity, or increased high-risk behaviours that compromise employee health and safety (12, 13, 14). Bullying in the workplace is also known to be harmful to workers and their health, as it is a source of social stress (38, 39) and also induces isolation, psychosomatic illness, depression, helplessness, anger, anxiety, and despair (40), as well as inducing suicides in extreme cases (41, 42). Bullying in the workplace might also manifest itself in the form of work hierarchies, unequal social relations in the workplace, unequal social contact, and class, power, and privilege dynamics.
Ontario LTC facilities are complex work environments where there are tensions between caring for residents and meeting work obligations and duties. These work environments are not isolated microcosms; rather, they are embedded in political, economic and social contexts. LTC staff must work within the boundaries of limited human resources, and the resultant time constraints that impair completion of tasks. While budgetary factors might explain some of these limitations, our study highlights that it is more than this. We emphasize that organizational and supervisory attitudes can also impact and limit the duties that are performed by various staff, even when participation in such duties is desired.
Another complexity is that when certain tasks are prioritized within limited time periods, some tasks are not completed, or are expected to be completed by other staff. This situation can further spiral into more difficulties for workers, leaving some workers burdened with extensive duties that demand trading off rest periods and breaks to meet certain levels of care for the residents of the homes. These workers also have to negotiate their own feelings and psychosocial responses to their work environment, such as intensive job stress, feelings of under-appreciation, guilt, and resentment. On an everyday basis, and over long periods of time, such chronic stress and strain can be detrimental for workers (23, 43). Indeed, one survey suggests that 97% of Ontario LTC workers reported being ill or injured as a result of their work in the last five years (44).
Certain tasks are assigned by government legislation and scope of practice regulations, set up by professional regulatory boards and colleges, or outlined in unions contracts, though it remains feasible to advocate for a less strict division of labour and more relational work. We note that extensive task sharing and relational work has been observed in the Swedish model and has positive benefits through stress reduction and improvements in residential care needs (2). Thus, further investigation into the factors that might explain the successful implementation of relational work and task sharing in certain models and not others is required.
Limitations
This paper described several key tensions and problems in Ontario long-term care work; however, it is also limited in certain ways. Although we examined work hierarchies and divisions of labour, one of the limitations was that not all psychosocial factors were systematically examined in this part of our study. For example, we did not assess workplace policies, in-service education, or leadership culture within organizations. These aspects can be tied to types of management models, such as for-profit versus not-for-profit, unionized versus non-unionization of staff, and hiring practices such as hiring of casual or part-time employees (26). For-profit management models tend to have high dissatisfaction among workers and high turnover of staff (26). Examining the link of management models to task orientation and care work hierarchies was outside of the scope of this paper, and warrants future investigation.
Conclusion
Our study shows how work hierarchies; rigid divisions of labour, and task orientation within LTC are highly complex phenomenon that can intersect with psychosocial factors. Employee job stress, high job demands, and time pressures, which are exhibited in our study, also seem to be linked to the experiences of care work hierarchies and of task oriented work between and among various worker groups. Care work is gendered and racialized, and these workers’ experiences include many types of psychosocial issues and challenges. These challenges should be addressed by stakeholders.
The implications of our findings are threefold. First, it might warrant government financial support to ensure adequate staffing levels in order to reduce workload and worker stress. Secondly, the findings could warrant policy changes that would prioritize social care and allow for relational care models that would in turn allow for increased flexibility and worker autonomy, and which is also imperative for resident quality of life. Finally, the issues presented should also be on the agenda of public health research, as ignoring them will not only lead to the possibility of diminished quality of care for residents, but also leave employees who are labouring under these complex working conditions at risk of harm.
Acknowledgement: This work was supported by the Canadian Institutes of Health Research, under Grant number 123787-1. Thank you to the other members of the Invisible Women Research Team: Karen Messing, PhD, Charlotte Rowell, MSW, Julia Brassolotto, PhD, Alison Jenkins Jayman, PhD, and Magali Rootham.
Conflict of interest: I.S, T.D, P.A, R.L, M.C, and V.N declare no conflict of interest.
Ethical standards: This work has been approved by the research ethics committees of York University and Université du Québec à Montréal.
References
1. Canadian Healthcare Association (CHA). Guide to Canadian Healthcare Facilities, 2007-2008. Vol. 15. Ottawa: CHA Press, 2007.
2. Daly, T. and Szebehely, M. Unheard voices, unmapped terrain: Care work in long-term residential care for older people in Canada and Sweden. International J. of Social Welfare. 2012;21(2):139-148.
3. Messing, K. One-Eyed Science: Occupational Health and Women Workers. Philadelphia: Temple University Press, 1998.
4. Bartley, M. Health Inequality: An Introduction to Theories, Concepts, and Methods. Cambridge, UK: Polity Press, 2004.
5. Bambra, C. Work, Worklessness, and the Political Economy of Health. Oxford: Oxford University Press, 2011.
6. Daly, T., Struthers, J., Muller, B., Taylor, D., Goldmann, M., Doupe, M., and Jacobsen, F.F. Prescriptive or interpretive regulation at the frontlines of care work in the three worlds of Canada, Germany and Norway, Labour / Le Travail. Spring, 2016;77: pp 1-35.
7. Razack, S.H. When place becomes race. In Razack, S.H. (Ed.). Race, Space and the Law: Unmapping a White Settler Society. Toronto: Between the Lines, 2002.
8. Zaman, H. Asian Immigrants in “Two Canadas”: Racialization, Marginalization, and Deregulated Work. Halifax: Fernwood Publishing, 2012.
9. Das Gupta, T. Racism and Paid Work. Toronto: Garamond Press, 1996.
10. Samra, J., Gilbert, M., Shain, M., & Bilsker, D. 2012. Psychosocial risk factors. Centre for Applied Research in Mental Health and Addiction (CARMHA). Retrieved from http://www.guardingmindsatwork.ca/docs/FAQ.pdf 1 Dec 2015.
11. CCOHS. Mental Health – Psychosocial Risk Factors in the Workplace. Retrieved from: http://www.ccohs.ca/oshanswers/psychosocial/mentalhealth_risk.html Accessed 1 Dec 2015.
12. Karasek, R., and Theorell, T. Healthy work: Stress, productivity, and the reconstruction of working life. New York, NY: Basic Book, 1990
13. CCOHS, 2014. Musculoskeletal Disorders – Psychosocial Factors. Retrieved from: http://www.ccohs.ca/oshanswers/psychosocial/musculoskeletal.html Accessed 1 Dec 2015.
14. Moen, P., Kelly, E.L., and Lam, J. Healthy Work Revisited: Do Changes in Time Strain Predict Well-Being? J. Occupational Health Psychology. April; 2013;18(2): 157–172. doi:10.1037/a0031804.
15. Johnson, J.V., and Hall, E.M. Job strain, workplace social support and cardiovascular disease: a cross-sectional study of a random sample of Swedish workers. American J. of Public Health. 1988;78:1336-1342
16. Karasek R., Theorell, T., Schwartz, J.E., Schnall, P.L., Pieper, C.F., and Michela J.L. Job characteristics in relation to the prevalence of myocardial infarction in the US Health Examination Survey (HES) and the Health and Nutrition Examination Survey (HANES). American J. of Public Health. 1988;78(8): 910-918.
17. Karasek, R.A. Job demands, job decision latitude and mental strain: implications for job redesign. Administrative Science Quarterly. 1979;24:285-307.
18. Cahill, J., and Landsbergis, P.A. Job strain among post office mail handlers. International Journal of Health Services. 1996;26/4 (73):1-750
19. Bongers PM, deWinter CR, Kompier MAJ, Hildebrandt VH. Psychosocial factors at work and musculoskeletal disease. Scandinavian Journal of Work Environment and Health. 1993;19(5), 297-3 12.
20. Koehoorn, M. Work Organization Factors and Musculoskeletal Symptoms and Claims Among Health Care Workers. Unpublished doctoral dissertation, University of British Columbia, Vancouver, Canada, 1999.
21. Sverke, M., Hellgren, J., and Naswall, K. No security: a meta-analysis and review of job insecurity and its consequences. Journal of Occupational Health Psychology. 2002;7:242-264.
22. Virtanen, M., Ferrie, J.E., Singh-Manoux. A., Shipley, M.J., Stansfeld, S.A., Marmot, M.G., and Kivimäki, M. Long working hours and symptoms of anxiety and depressions: A 5-year follow-up of the White hall II study. Psychological Medicine. 2011;41(12):2485-2494 doi: 2494.10.1017/S0033291711000171
23. Lewchuk, W., Clarke, M., and De Wolff, A. Working Without Commitments. The Health Effects of Precarious Employment. Montreal: McGill-Queen’s University Press, 2011.
24. Armstrong, P., Banerjee, A., Szebehely, M., Armstrong, H., Daly, T., and LaFrance, S. They Deserve Better: The Long-term Care Experience in Canada and Scandinavia. Ottawa, Canadian Centre for Policy Alternatives, 2009.
25. Agnew, V. Racialized Migrant Women in Canada. Toronto: University of Toronto Press, 2009.
26. Neysmith, S.M., and Aronson, J. Working conditions in home care: Negotiating race and class boundaries in gendered work. International Journal of Health Services. 1997;27(3):479-499.
27. Armstrong, P. and Laxer, K. Precarious work, privatization, and the health care industry: the case of ancillary workers. In Vosko, L.F. (Ed.). Precarious Employment: Understanding Labour Market Insecurity in Canada. p. 115-138, 2005. Montreal: McGill-Queen’s University Press, 2005.
28. Armstrong, P. Relocating Care: Home Care in Ontario. In Morrow, M., Hankivsky, O., and Varcoe, C. (Eds.). Women’s Health in Canada: Critical Perspectives on Theory and Policy. pp. 528-553. Toronto: University of Toronto Press, 2007.
29. Armstrong, P., Armstrong, H., and Scott-Dixon, K. Critical to care: The invisible women in health services. Toronto: University of Toronto Press, 2008.
30. Bourgeault, I.L., Atanackovic, J., Rashid, A., and Parpia, R. Relations between Immigrant care workers and older persons in home and long term care. Canadian Journal on Aging. 2010;29(1):109-118.
31. Syed, I.U. Labour Exploitation and Health Inequities among Market Migrants: A Political Economy Perspective. J. of International Migration and Integration. 2016;17(2):449-465 doi: 10.1007/s12134-015-0427-z
32. Syed, I.U. Chronic Illness among Immigrant Workers in Canada: An Overview of Existing knowledge. In Stone, S.D., Crooks, V.A., and Owen, M. (Eds.) Working Bodies: Chronic Illness in the Canadian Workplace. Montreal: McGill-Queens University Press. p. 161-176, 2014.
33. Doyal, L. What Makes Women Sick: Gender and the Political Economy of Health. Macmillan, Houndmills, 1995.
34. Armstrong, P., and Armstrong, H. The Double Ghetto: Canadian Women and their Segregated Work. 3rd Edition. Oxford: Oxford University Press, 2010. (First Published in 1994).
35. Baines, D., and Cunningham, I. Using comparative perspective rapid ethnography in international case studies: strengths and challenges. Qualitative Social Work. 2011;12(1):73-78.
36. Daly, T., Armstrong, P., and Lowndes, R. Liminality in Ontario’s long-term care facilities: Private companions’ care work in the space ‘betwixt and between’. Competition and Change. 2015;19(3): 246–263. doi: 10.1177/ 1024529415580262].
37. Armstrong, P., and Jansen, I. Assessing the impact of restructuring and work reorganization in long term care. In Van Esterik, P. (Ed.). Head, Heart and Hands: Partnerships for Women’s Health in Canadian Environments. p. 175-217. Toronto: National Network on Environments and Women’s Health, 2003.
38. Vartia, M. Psychological harassment (bullying, mobbing) at work. In Kauppinen-Toropainen, K. (Ed.) OECD Panel Group on Women Work and Health: National Report. Finland: The Ministry of Social Affairs and Health. The Institute of Occupational Health, Publications. 1993;6:149-152
39. Zapf, D., Dormann, C., Frese, M. Longitudinal studies in organizational stress research: A review of the literature with reference to methodological issues. Journal of Occupational Health Psychology. 1:145-169.
40. Leymann, H. Mobbing and psychological terror at workplaces. Violence and Victims 1990;5:119-125.
41. Leymann, H. Vuxenmobbning pa svenska arbeidsplatser: Delrapport 1 om frekvenser. Adult bullying at Swedish workplaces: Report 1 concerning frequencies. Stockholm: Arbetarskydd styrelsen, 1992.
42. Einarsen, S. and Mikkelson, E.G. Individual effects of exposure to bullying at work. In Einarsen, S., Hoel, H., Cooper, C. (Eds.) Bullying and Emotional Abuse in the Workplace: International Perspectives in Research and Practice. London: Taylor and Francis, 2003.
43. Stone, S.D., Crooks, V.A., and Owen, M. (Eds.). Introduction: Chronic Illness in the Canadian Workplace. In Working Bodies: Chronic Illness in the Canadian Workplace. pp. 3-25. Montreal: McGill-Queens University Press, 2014.
44. Armstrong, P., and Daly, T. There are not enough hands: Conditions in Ontario’s long term care facilities. Toronto: Canadian Union of Public Employees (CUPE)], 2004
