J. Williams1, C. Stolp1, G. Roberts1,2, M. Fearn3, C. Doyle1,2,3
1. Villa Maria Catholic Homes, Melbourne, Victoria, Australia; 2. Australian Catholic University, Melbourne, Australia; 3. National Ageing Research Institute, Melbourne, Australia.Corresponding author: Colleen Doyle, Villa Maria Catholic Homes, Melbourne, Victoria, Australia, Colleen.Doyle@acu.edu.au, Telephone +61 409 739 136).
Abstract
Background: A range of staff with different skills undertake care for older people in residential care. When older people in care become unwell, a transfer to hospital may be avoided if their illness is recognised early by staff, and assessed, monitored and treated. Objectives: To improve residential aged care workforce capacity and professionalism, by implementing a new pilot workforce model, and to evaluate the model’s impact on staff and residents, including provision of complex palliative care, confidence and hospital transfer rates. Design: Mixed methods, including staff semi-structured interviews, staff quality improvement surveys, and assessment of monitoring, interventions and resident transfers. Settings: Three aged care residences in Victoria, Australia. Participants: Staff (n=278) in all three aged care residences. Intervention: Implementation of a comprehensive care model, developed to decrease unnecessary transfers of older people to acute care from residential care, and to improve skills in staff. Measurements: Number of ‘Stop and Watch’ reports made, percentage of ‘Stop and Watch’ reports resulting in an intervention, average monthly hospital transfers of residents to acute care (baseline, implementation and post -implementation), percentage of End of life Care Pathways completed based on number of deaths, and staff confidence. Results: Staff reported more confidence in identifying and caring for unwell residents, their capability to provide palliative care was perceived to increase, teamwork with external services improved, and new interventions and a decrease in hospital transfers occurred. Conclusions: This project showed improvement in early detection of deterioration in residents’ health condition, reduction in hospital transfers and improvements in staff satisfaction and confidence. Limitations of the study were the lack of control group and the small sample.
Key words: Hospital transfers, residential aged care, workforce development, clinical skill.
Introduction
Older people who live in residential aged care or nursing homes in Australia are cared for by a range of staff consisting of a minority of registered nurses (RNs) with advanced clinical practice skills and experience, some nurses with one year of training (ENs) and a majority of personal care assistants (PCAs) with less training and varying levels of care experience (1). People living in residential aged care require assistance from a mix of staff skills. Living in residential aged care is a necessity rather than a choice for older Australians who are no longer able to manage at home alone or with help from family carers (2). When residents become acutely unwell, transfer to the local acute hospital may be because staff lack the nursing skills to manage acute incidents, or acute conditions may not be brought to the attention of senior staff until the resident’s condition has deteriorated to the point where transfer to hospital is unavoidable, or the resident or their family may prefer treatment in an acute setting. Clearly, people living in residential aged care have the same rights as others to access acute care when they need it. In Australia, there were over 6.5 million presentations to public hospital emergency departments (ED) in 2011-12, and 221,000 ED presentations from residential aged care in 2008-2009 (3, 4). One systematic review found that the incidence of transfer from aged care residences to ED is more than 30 transfers per 100 RACF beds per year although rates varied considerably (5). Internationally, studies have indicated 7-67% of presentations to ED may be avoidable through improved primary care (6-12). Most transfers from residential aged care to ED are of high acuity patients, and a retrospective audit of records from one Australian hospital found 31% of transfers to acute care were avoidable (7). In that study, avoidable and unavoidable transfers were assessed according to a list of 10 exclusion criteria based on the clinical presentation or other factors such as family request to transfer. Another related study found that providing residential care staff with increased access to clinical expertise can reduce hospital transfers of residents by 17% (13).
Improving Clinical practice
The present model arose from a quality improvement project. A gap analysis of reasons for transfer to acute hospital and staff capability was conducted in our residential care residences. Common reasons for transfer were identified as sepsis, dehydration, pain, falls (often as a consequence of underlying acute medical condition such as sepsis), and end of life. In response to concerns about workforce capability and avoidable transfers of residents from residential aged care to acute care, we developed and evaluated a workforce model (‘Raise the Bar’) that was shaped according to the needs of staff of our aged care residences. Our quality improvement activities indicated that staff were lacking in confidence in their clinical practices about early identification of the unwell resident. Our goal was to improve support, guidance and education for the clinical staff as to the optimal clinical approach for an unwell resident. It was also evident that advanced clinical practice skills for staff were not being used to the fullest extent, and staff capability to provide complex palliative care at the end of life was limited by their lack of knowledge about end of life care pathways. Furthermore, there was limited interdisciplinary teamwork with external health services. Staff indicated that relationships with key external support services, including emergency departments, In Reach services (services provided by the local acute hospital, whereby hospital staff visit the resident before transfer), ambulance services, locum general practitioner (physician) services and pharmacy providers were not ideal. These cumulative factors influencing our residential care settings led to the development of a new workforce model.
The overall goal of developing a new model of practice was to reflect the mission of the service which was to optimise resident health and quality of life and minimise functional decline, while at the same time respecting resident and family choices about transfer to acute care. The aim of this study was to implement a new workforce model and evaluate its impact on staff and residents. We hypothesised that transfers to acute care would be the result of a complex mix of factors (including staff skills), and that the factors listed below under ‘the workforce model’ would need to be changed together in order to effect a change in outcomes. This project aimed to “Raise the Bar” in Relationships, Advanced practice, Innovation, Skill sets and Expectations, to facilitate improvements in residential care workforce capacity, capability, employee satisfaction and professionalism, and standards of resident care delivery. A specific aim for the project was that 20% of all deaths had an end of life care plan (EOLCP) completed for the resident.
The workforce model
The model was developed in response to a needs analysis conducted at the aged care residences, and influenced by a social ecological theoretical framework (14-16). It had four key aspects:
- Teaching staff how to ‘Stop and Watch’ (S&W) – this is an early warning tool for any residential care staff, including personal care workers, kitchen staff, cleaning staff and others to flag and document when residents appear to be becoming unwell. All residents placed on S&W receive a clinical assessment by a nurse who has received extra training through the program (17-19).
- New ‘Emergency Decision Guidelines’ put into place that provide support and guidance for clinical care staff completing a clinical assessment of the resident or to assist when calling a general practitioner, locum service, hospital service or ambulance, to ensure the best clinical communication and approach for an unwell resident. These guidelines were part of the residences’ new policy.
- Introduction of an ‘End of Life Care Pathway’ (EOLCP) tool that is used to provide health care to people nearing the end of life to ensure that high quality, person-centred care is provided, while being responsive to the individual’s needs and previously expressed wishes (e.g. physical, spiritual and emotional care) (20-24).
- Training in advanced clinical practice skills where care staff undertake training to increase the type and level of clinical care that can be provided to a resident at the Residence, thereby providing residents with greater continuity of care and a more productive and coordinated primary care team approach (13,17, 25). An important aspect of the model is an audit of the reasons for transfer of residents during the 12 months prior to introduction of the staff training. The audit pointed to the main areas where nursing staff lacked the clinical skills and confidence to manage clinical situations with the support of external agencies.
Staff at Villa Maria Catholic Homes (formerly Catholic Homes), led by author JW, developed the model in consultation with external stakeholders. The model was implemented by the learning and development team at Villa Maria Catholic Homes (formerly Catholic Homes). The authors JW and CS were employed to support learning and development at the sites, and to provide clinical governance. The evaluation was conducted by researchers external to the organisation (CD, GR and MF) and employed by a local university with an industry partnership agreement with the residential care organisation. The model was piloted in three aged care residences. Three contrasting sites in terms of rural/metropolitan site and large/small size were chosen to explore the impact of these factors on the results. The sites volunteered to be involved in the quality improvement project. Residence A had 131 staff with 90 ‘ageing in place’ beds and 30 ‘extra services’ beds. Residence B had 92 staff with 30 high care beds and 49 low care beds, 1 respite care bed and 15 dementia specific beds. Residence C had 55 staff with 57 ageing in place beds and 1 respite care bed. All staff were trained (n=278). This paper reports on preliminary evidence for the effectiveness of the model.
Methods
Design
The formative evaluation used a mixed methods pre-post design to address the following questions, identified by the team as those most useful to further development of the model:
• What were staff perceptions of transfers to acute hospital?
• How did staff view the implementation of new tools such as the End of Life Care Pathway and the Stop and Watch tool?
• What was the effect of training on staff satisfaction and confidence?
• Did ‘Stop and Watch’ directions lead to implementation of new actions for residents?
• Were End of Life Care Pathways implemented after staff received training?
• Did transfers to acute hospital change during and after implementation of the model?
Qualitative and quantitative methods were used to address the key evaluation questions.
The setting was three residences of Villa Maria Catholic Homes (formerly Catholic Homes), a residential aged care provider in Melbourne, Australia. The Chief Executive Officer approved the project and provided organisational consent for the three residential sites that expressed an interest in participating. Staff who agreed to participate in qualitative interviews were provided with participant information sheets about the project and signed informed consent forms. Participant information sheets explained confidentiality, privacy and the voluntary nature of their participation. Ethics approval (no. 2012262V) was obtained from Australian Catholic University Human Research Ethics Committee.
Qualitative data
Semi-structured, face to face staff interviews were conducted in November 2012 and November 2013, pre and post-project implementation, at each residence. Interviews explored staff perceptions of unexpected transfers to hospital, and the usefulness of advance care plans for residents. Post-implementation interviews explored staff opinions on all aspects of the project. Interviews were recorded and transcribed when permission was received from the participant, otherwise detailed notes were taken during and post interviews. Collected data were then thematically analysed.
In total 51 qualitative interviews were conducted with 41 staff (15% of staff). Pre-implementation, 27 residential care staff were interviewed (16 personal care attendants (PCAs), 8 enrolled nurses (ENs) and 3 registered nurses (RNs) across the three aged care residences involved in the project. Post implementation, 24 residential care staff (11 PCAs, 5 ENs, 5 RNs, 2 Lifestyle staff and 1 Domestic staff) across the three aged care residences involved in the project. Ten staff were interviewed twice, both pre and post implementation. Participation in staff interviews was voluntary. Time pressure on staff was cited as the main reason more staff were not available to be interviewed. Nevertheless using qualitative methodology we were able to reach saturation of themes arising from the interviews.
Quantitative data
For quantitative data, ‘Staff satisfaction and confidence in the model’ surveys were conducted during implementation and after training. All staff (n=278) were invited to complete the questionnaires, and provision of completed questionnaires was considered consent to participate in the evaluation. In total 90 staff completed questionnaires (32% response rate). Because of ethics requirements associated with privacy of participation in questionnaire completion, it was not revealed whether staff who completed questionnaires had also been interviewed in qualitative data collection exercises. Respecting privacy and non-coercion was considered a strategy to maximise the chances of participation in the data collection. A five-point scale to indicate confidence in completing various components of the project, changes in their ability and changes in job satisfaction was used. Respondents were also asked open-ended questions about positive aspects of the project and challenges with the project. The Stop and Watch (S&W) audit tool was completed monthly. Descriptive statistics were used to analyse and describe this data.
The number of resident transfers to hospital was recorded for the eight months prior to the implementation (baseline), during the implementation stage (four months) and then again post-implementation (four months). The length of stay of the resident in hospital was also recorded for the prior to the implementation (baseline), during the implementation stage, and again post-implementation.
The End of Life Care Pathway (EOLCP) audit tool was completed monthly and data collected on the number of EOLCPs that had been introduced again during and post (four months) implementation.
Results
Pre-implementation interviews indicated that existing systems and processes to support staff decision-making about care were vulnerable due to inexperienced duty staff, or lack of a ‘sounding board’ for some staff who required extra support. It was found that even lack of equipment, for example, an ECG machine or x-ray machine, can impact on staff decision making about transfers.
Post-implementation, most staff reported better identifying and caring for unwell residents since the project; that now “many eyes” were assessing residents, as described by one EN:
“… (we are) monitoring very closely now…previously, monitored in handover but didn’t ‘go in deep’ [just] obs…now, all workers in the residence [are watching the resident]”.
Another EN reported on the typically improved clinical practice of the staff, especially the PCAs:
“[Now] when resident is unwell, the PCAs will say, ‘Oh, let’s do a urine test’ – they’re, well, proactive…and bring me the results, instead of going ‘Oh, this person isn’t well’, and walking away. They’re actually taking on some responsibility as well.”
All staff interviewed in the post-implementation stage recognised that unplanned transfers had reduced at their residence.
Most PCAs, ENs and RNs interviewed spoke positively of the clinical assessment skills training they received, and none spoke negatively of them. For example, an RN stated that:
“It’s wonderful, its very effective, I find that, er, for our residents, as well, it is less of a trauma (than) being pushed off to hospital…at times we have to do that, but if we can treat them here, that is wonderful, it is beneficial for our residents. It also makes us feel ‘ok, we are doing something’…not just pushing them off as somebody else’s responsibility – and it is effective, because we have the support and everything around; infrastructure, everything’s available”.
RNs welcomed their training and the project, but indicated that all staff would require ongoing support, training and education to maintain their skills and knowledge.
Pre-implementation, staff interviewed indicated they had no exposure to advance care planning (ACP) education: few had heard the term. If they had, they equated (ACP) with the standard advance care directive (ACD) form used at the residences. Division one RNs (three years’ training) most frequently used the ACD forms. Several RNs described the forms as confusing and unclear: the terminology used (‘aggressive’, or ‘conservative’, or ‘palliative’ treatment) was unhelpful to them in determining what care the residents would prefer. Instead, it was reported that interpretation was left to individual staff, visiting health professionals (e.g. GP), and family members. All staff indicated that they welcomed more education about ACP, and commented that GP’s and family members might benefit from this, too.
Post-implementation, staff indicated their capability to provide complex palliative care at the end of life had improved, a PCA stating that:
“Staff (now) know what to do if someone is sick. (The End of Life pathway is) reassuring staff they have done everything to help resident because it is all written down”.
Some staff stated that their residence had always ‘done palliative care well’, but they now had a clearer structure and process, enhancing their confidence and professional care; they also welcomed the training to enhance their skills, as indicated by an RN:
“We have got all the support from our management and we have had loads and loadd of training to update us all with everything, its great. Without the support of the management and everything, I don’t think we would have been able to have done it (Raise the Bar)…Almost all of RNs have done the training, and it is just a matter of putting in the syringe driver and just doing it…Our clinical manager is very great. She gives us all the support”.
Staff also observed benefits for families in transparently recording care of residents – families indicated to staff that they now felt part of the care process. Staff indicated that joint staff and family involvement in the EOLCP fostered a ‘community’ feel, as described by a Lifestyle staff member:
“ I like the end of life pathway…we don’t send them off, they don’t go to hospital to die, they can stay here, where they are comfortable, where they are happiest…if they have got friends here, their friends (other residents) can go and sit with them…say their goodbyes. You hear the families saying that (they want sick residents to be sent to hospital, possibly to die), but then you’ve got the ones (other relatives) that say ‘I am so grateful that Mum was here. You’ve looked after her beautifully…”.
Staff reported a significant change in the perception of a team approach among all residential care staff in monitoring patients. An RN stated that:
(Stop and watch) “It’s been brilliant, absolutely wonderful because it helps us to pick up early signs of infection, treat it ASAP, prevent complications… in the past, if they were caring for someone and they would find a change, they would not let you know because they are busy, going along with their work, now, with the Stop and Watch, they have been encouraged to monitor and to bring to notice of RNs and in charges, what is happening – even if it is a little thing that is out of place”.
Teamwork was also reported as improved between residential care staff and external services. Staff described being more enabled to work with and get advice from the In Reach teams, and consequently their local hospital services. The In Reach teams were also used for staff training in advanced clinical practice skills and assessment skills, which enhanced relationship building and provided consistency of policy and processes.
In May 2013, 90 staff from across the three residences completed the staff satisfaction and confidence questionnaire, 45 from Residence A, 31 from Residence B and 14 from Residence C (72 were present for end of life training).
The majority of staff (58.9%) felt more confident in their ability to report early triggers of the unwell resident (see Table 1). Similarly the majority (60%) of staff were confident in using the Stop and Watch tool and the majority of staff were also confident in using the End of Life Pathway tool with (64.3%). The majority of staff (62.9%) indicated that the end of life pathway tool had improved their ability to care for the resident. When asked about their confidence in using the Emergency Decision Guidelines, administering IV antibiotics, administering subcutaneous fluids and administering medication via a syringe driver, all the nursing staff that completed this were now more confident. All nursing staff also indicated that the emergency decision making guidelines had improved their ability to care for the resident. Finally the majority of staff (56.3%) had increased their job satisfaction through being involved in the project.
When analysing qualitative comments that were written at the end of the staff satisfaction and confidence questionnaire, emerging positive project themes that included:
• being able to detect resident health changes early
• being able to monitor resident behaviour and changes more effectively
• increased staff education and knowledge about how to care for an unwell resident
• improved quality of care for residents
• time saving by completing documentation on the spot and providing treatment immediately
• reduces unnecessary resident transfers to hospital
• improved documentation and record keeping
• greater staff empowerment and being more alert and aware of the resident’s needs
• improved communication between staff about residents
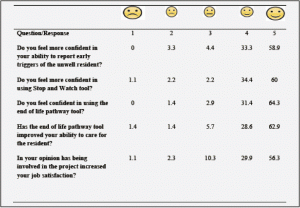
Table 1 Percentage of staff responding to questions about staff confidence (Likert scale responses; N=90)
The challenges that were identified on the staff confidence and satisfaction questionnaire were:
• Sometimes it is difficult to identify changes in residents behaviour early
• Increased documentation and paperwork
• Time management due to increased care and documentation
• Some staff not being provided with education about the model or how it works
• Reluctance or hesitation of staff to implement the skills and knowledge they have learnt through the project
• General problems associated with implementing a new model or program
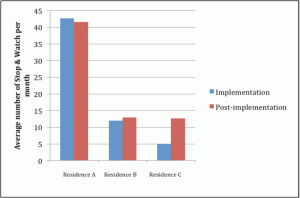
Figure 1 shows the average number of monthly Stop and Watch per month that were initiated during the implementation stage and the post-implementation stage at each Residence (no Stop and Watch notices were implemented prior to the model commencing). As can be seen in Figure 1, the average number of Stop and Watch notices was maintained post-implementation in all three residences and increased substantially in Residence C.
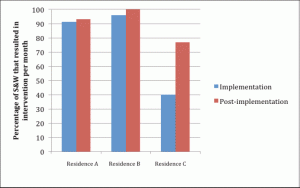
Figure 2 shows the percentage of Stop and Watch that resulted in an intervention being put into place at each Residence during the implementation stage and the post-implementation stage. Figure 2 illustrates that Stop and Watch notices commonly lead to clinical interventions for the residents. As the model became established, clinical interventions increased, suggesting that staff became more adept at using the model to increase interventions.
The types of interventions that clinical staff put into place as a result of the implementation of the model included (but were not limited to):
• External health service providers contacted (In Reach team, GP, locum, transfer to hospital)
• Change in medications (initiating antibiotics, use of PRN medications, change in regular medications, syringe driver)
• End of Life Care Pathway initiation
• Allied health or other medical specialist referral (speech pathologist, dietician, physiotherapist, nephrologist)
• Radiology / Pathology
• Oxygen therapy
• Dietary interventions (increase fluid intake, fluid balance chart, food chart, food supplements)
• Increased monitoring and observations (monitoring vital signs, neurological observations, blood glucose monitoring, pain chart)
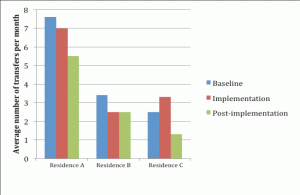
Figure 3 Average number of monthly hospital transfers per residence during baseline, implementation and post-implementation stages
As shown in Figure 3, hospital transfers appeared to change during and post implementation of the model. As indicated in Figure 3, the average number of monthly hospital transfers decreased during implementation and post-implementation stages for Residence A and Residence B, however there was a slight increase in Residence C during the implementation stage. Transfers reduced from 76.2 transfers/100 beds per year before implementation to 50 transfers/100 beds per year in Residence A, from 62.3 transfers/100 beds per year before implementation to 46 in Residence B and from 63.4 to 40.6 in Residence C.
Figure 4 displays the percentage of End of Life Care Pathways that were completed in each Residence during the implementation and post-implementation stages based on the number of deaths that occurred at the Residence. The aim for the project was that 20% of all deaths had an EOLCP completed for it, and as Figure 4 shows, more than that was completed at each Residence in both the implementation and post-implementation stages.
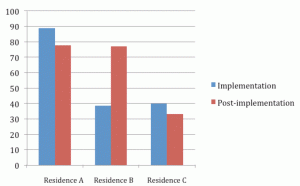
Figure 4 Percentage of End of Life Care Pathways completed based on number of deaths at each residence
Discussion and conclusions
This paper has described a new model of care, ‘Raise the bar’ and its evaluation in three aged care residences. While the components of the clinical practice model implemented appeared to be successful in changing practice, this study indicated that the individual components of the ‘Raise the Bar’ were highly complementary, and possibly mutually reliant for the overall effect observed. The implications for policy and practice are as follows.
Implementation of the ‘Stop and Watch’ component of the ‘Raise the Bar’ project engaged and enabled staff to identify the unwell resident at an early stage. A large proportion of the S&W that were initiated had interventions put into place. Furthermore, in two of the residences, the average number of monthly hospital transfers from baseline to the implementation stage reduced. Studies in the literature have suggested that on average the transfer rate from residential aged care to emergency department was more than 30 transfers per 100 beds per year, although results varied considerably from 20 transfers to over 150 transfers (5). Transfer rates in our study started at the high end and reduced to the low end of published rates. All residences reduced the average number of monthly hospital transfers at post-implementation, suggesting that unwell residents were being identified at an early stage and were able to be treated within the Residence.
The education and training provided as part of ‘Raise the Bar’ appeared to be fundamental to the success of the project. A large number of staff reported how the education and training had contributed to the way they now deliver care to the residents, and also how they feel about delivering care to residents. However, they noted that it is important that this education and training continued on a regular basis and be put on the training calendar.
Including external services as part of the interdisciplinary team also appeared to improve the professional relationship between all parties and increased the relationship building and confidence of staff to obtain advice. Factors that were reported to be integral to the success of the model, and that would help others implement the model, were:
• strong leadership – it is important that there are strong leaders and champions to drive the model, along with strong management support,
• education for all levels of staff, with staff being paid to attend training
• including all levels of staff, not just the nursing or care staff, in the implementation
However, obstacles that may need to be considered when implementing practice change and a new model such as ‘Raise the Bar’, that may impact on the longer-term sustainability, include:
• Having staff with the relevant skills that are motivated and have the time to dedicate to project activities.
• It is necessary to ensure that adequate funding is available to support staff to undertake the role of champion in addition to their existing workloads once the dedicated project funding has ceased.
• Be prepared for staff turnover, in particular if the Residence manager or champion changes and the impact this may have on the project (staff turnover in the residences studied here was low, less than two percent per month).
Limitations and further research
The limitations of this study were that we were unable to compare results to a control group of homes where the model was not implemented, and the small sample size limits the generalizability and power of the results found. Because this was a pilot and numbers were small, statistical analysis of the results was not possible. Instead visual inspection of the data indicated a trend towards reduction. Only three volunteer residences were chosen, diverse in terms of rural/metropolitan setting and size, which was both a limitation and a strength as we were able to demonstrate that the program was effective to some extent in all three settings. While qualitative interviews may have been subject to bias in that we relied on volunteers to participate in interviews, the interviews were conducted and analysed using rigorous qualitative methodology and principles of analysis. Some staff were no longer working within the organisation in the post implementation interviews. However saturation of themes was achieved with the small number of in-depth interviews undertaken. The alignment between qualitative data (a small sample of staff) and quantitative data (larger sample) lends strength to the validity of conclusions made from the qualitative data. Overall the picture provided by data collection was a positive one. Staff who did not complete questionnaires may have been less positive about the program, and this limitation is acknowledged. Further research is needed to increase the power of the results and further understand the generalizability of the results, which show promise in improving the nursing and residential aged care workforce.
Funding: Villa Maria Catholic Homes (formerly, Catholic Homes) funded the quality improvement project that facilitated the Raise the Bar Model. External funding was provided by Health WorkForce Australia.
Acknowledgements: The authors wish to acknowledge the support of Villa Maria Catholic Homes (formerly Catholic Homes) in the development, implementation and evaluation of the quality improvement project that facilitated the Raise the Bar Model.
Conflict of interest: None of the authors have any conflicts of interest to declare.
Ethical Standard: The Australian Catholic University Human Research Ethics Committee approved the study protocol.
References
1. King D, Mavromaras K, Wei Z, et al. The Aged Care Workforce, 2012. Australian Government Department of Health and Ageing. Canberra; 2012
2. Productivity Commission Inquiry Report. Caring for older Australians. Overview, Report no. 53, Final Inquiry Report. 2011. Australian Government, Canberra.
3. Australian Institute of Health and Welfare (2012). Australian hospital statistics 2011–12: emergency department care. Health services series no. 45. Cat. no. HSE 126. 2012. AIHW, Canberra.
4. Australian Institute of Health and Welfare. Movement Between Hospital And Residential Aged Care 2008-09. Data linkage series no. 16. Cat. no. CSI 16. 2013. AIHW, Canberra.
5. Arendts G, Howard K. The interface between residential aged care and the emergency department: a systematic review. Age Ageing. 2010;39:306-312.
6 Bowman CE, Elford J, Dovey J et al. (2001). Acute hospital admissions from nursing homes: some may be avoidable. Postgrad. Med. J. 2001;77:40-42.
7. Codde J, Frankel J, Arendts G, Babich P. (2010). Quantification of the proportion of transfers from aged care residences to the emergency department that could be avoided through improved primary care services. Australasian. J. Ageing. 2010;29:169-171.
8. Finn JC, Flicker, L, Mackenzie E et al. Interface between aged care residences and a teaching hospital emergency department in Western Australia. Med. J. Aust. 2006;184:432-435
9. Kirsebom M, Hedstrom M, Wadensten B, Poder U. (2014). The frequency of and reasons for acute hospital transfers of older nursing home residents. Arch. Gerontol. Geriatr. 2014;58:115-120.
10. Jones JS, Dwyer PR, White LJ et al. Patient transfer from nursing home to emergency department: Outcomes and policy implications. Acad. Emerg. Med. 1997;4:908-915.
11. Ouslander JG, Lamb G, Perloe M et al . Potentially avoidable hospitalizations of nursing home residents: Frequency, causes and costs. J. Am. Geriatr. Soc. 2010;58: 627-635.
12. Saliba D, Kington R, Buchanan J et al. (2000). Appropriateness of the decision to transfer nursing facility residents to the hospital. J. Am. Geriatr. Soc. 2000; 48:154-163.
13. Codde J, Arendts G, Frankel, J et al. Transfers from aged care residences to the emergency department are reduced through improved primary care services: An intervention study. Australasian J. Ageing. 2010;29:150-154
14. Galik E. (2010). Function-focused care for LTC residents with moderate-to-severe dementia: A social ecological approach. Ann. Long Term Care. 2010; 18:27-32.
15. Resnick B, Pretzer-Aboff I, Galik E et al. Barriers and benefits to implementing a restorative care intervention in nursing homes. J. Am. Dir. Assoc. 2008; 9:102-108.
16. Sallis J, Cervero RB, Ascher W et al. An ecological approach to creating active living communities. Ann. Rev. Pub. Health 2006; 27: 297-322.
17. Bourbonniere M, Strumpf NE. Enhancing geriatric nursing competencies for RNs in nursing homes. Res. Gerontol. Nurs. 2008;1:171-175.
18. Braun KL, Cheang M, Shigeta D. Increasing knowledge, skills, and empathy among direct care workers in elder care: a preliminary study of an active-learning model. Gerontol. 2005;45:118-124.
19. Burgio LD, Allen-Burge R, Roth DL et al. Come talk with me: improving communication between nursing assistants and nursing assistants and nursing home residents during care routines. Gerontol. 2001;41:449-460.
20. Caplan GA, Meller A, Squires B, Chan S, Willett W. Advance care planning and hospital in the home. Age Ageing. 2006;35:581-585.
21. Gold Standards Framework Centre. Gold standards framework in end of life care. 2008. National Health Service, United Kingdom. www.goldstandardsframework.org.uk Accessed 1 December 2015.
22. Neuberger J et al. More care, less pathway. A review of the Liverpool Care Pathway. Independent Review of the Liverpool Care Pathway. 2013. Department of Health, United Kingdom. https://www.gov.uk/government/uploads/system/uploads/attachment_data/file/212450/Liverpool_Care_Pathway.pdf Accessed 1 December 2015.
23. Department of Health, National Health Services (NHS) (2008). Commissioning person centred end of life care. A toolkit for health and social care professionals. National End of Life Care Programme. 2008. National Health Service, United Kingdom. www.endoflifecareforadults.nhs.uk Accessed 1 December 2015.
24. Palliative Care Australia. Standards for providing quality palliative care for all Australians. 4th Edition. 2005. Palliative Care Australia.
25. Aylward S, Stolee P, Keet N, Johncox V. Effectiveness of continuing education in long-term care: A literature review. Gerontol. 2003;43:259-271.