K.J. Pfisterer1,2, M.T. Sharratt1,2, G.G. Heckman1,2, H.H. Keller1,2
1. University of Waterloo, Waterloo, ON, Canada; 2. Schlegel-University of Waterloo Research Institute for Aging, Waterloo, ON, Canada. Corresponding author: Heather H. Keller, 200 University Avenue West, Burt Matthews Hall 1106, Waterloo, ON, Canada, N2L 3G1, Email: hkeller@uwaterloo.ca, Telephone: (519) 888-4567 ext. 31783, Fax: (519) 746-6776
Jour Nursing Home Res 2016;2:64-70
Published online July 1, 2016, http://dx.doi.org/10.14283/jnhrs.2016.9
Abstract
Background: Vitamin B12 deficiency is avoidable through screening and treatment. Deficiency in long-term care impacts ~35% of residents, yet it remains unclear as to what long-term care homes are doing to address this issue. Objective: For the first time, to describe the state of B12 screening and treatment protocols in Ontario long-term care homes, influence of geography and corporate structure on protocols, and the proportion of residents who are currently under treatment. Design: This cross-sectional study used stratified random sampling. Setting: Ontario long-term care homes. Participants: Forty-five standardized phone interviews were completed with the directors of nursing care. Measurements: The following measurements were collected: home demographics (geography, for-profit status etc.), protocols pertaining to vitamin B12 testing, treatment, the cut-point each home uses to define B12 deficiency, proportion of residents receiving B12 and the treatment method (intramuscular injection vs. oral). Results: Cut-off values for determination of B12 deficiency varied (31%
Key words: Vitamin B12 deficiency, long-term care, nursing home, screening.
Introduction
Vitamin B12 has been identified as a micronutrient of interest for older adults (1-3), with deficiency primarily caused by either inadequate intake (3) or lack of absorption due to atrophic gastritis, which is highly prevalent in this segment of the population (3). Nonspecific symptoms associated with B12 deficiency make diagnosis challenging and include: depression (4-8), other psychiatric symptoms (4), impaired neurotransmitter and monoamine synthesis (4), cognitive decline or dementia (5-7), memory problems (8), balance and mobility issues due to peripheral neuropathy (5, 7).These are in addition to classic symptoms of vitamin B12 deficiency including macrocytic megaloblastic anemia, and degeneration of the spine (4-6). One particularly vulnerable group for B12 deficiency is older adults (65 years or older) living in long-term care (LTC), where malnutrition affects up to 65% (9). While decreased absorption is the main cause of B12 deficiency, low intake is still a concern especially as absorptive changes with age likely increase B12 requirements. Low micronutrient intake commonly coincides with protein-energy malnutrition and there is a significant potential for deficiency. Generally, older adults in LTC are more vulnerable to micronutrient malnutrition due to any combination of: inadequate micronutrient content of the meal resulting from menu planning challenges; low food intake resulting from functional impairment, slow eating, taste changes, poor appetite (10, 11); and the high use of medications (12).
Prevalence of B12 deficiency (or marginal status) in community-living older adults (age 65+) is estimated at up to 40% depending on the diagnostic criteria used (1, 13, 14). While there is no consistency in cut-points used to define status, typically, B12 deficiency is defined as a B12 blood serum concentration below a very low value (e.g., 250pmol/L (14)). Relatively few studies have reported on B12 deficiency prevalence in LTC and it is anticipated to relatively high due to challenges, due to challenges in eating and deficits in menu planning (15), especially as there are relatively few foods in which B12 naturally exists (i.e., only in animal products) (16); LTC estimates outside of Canada range from 7% (17) to 34% (18). Only two studies from Canada are published, one study in a LTC hospital finding 7% and 35% with low and low normal B12 concentrations (17) while another study found 14% and 39% had low and low normal concentrations at admission to LTC (19). As symptoms of vitamin B12 deficiency are subtle, nonspecific and are frequently unrecognized or misdiagnosed (13, 14) and classic symptoms as such are unreliable for diagnosis (13), deficiency may only be identified with regular testing. Prior estimates of prevalence were primarily based on samples of residents that had been admitted for a period of time. Currently it is unknown if and when LTC does routine testing to screen for B12 deficiency.
This potentially avoidable deficiency may provide an opportunity for improving health outcomes of LTC residents. However, a gap exists in our understanding of LTC practices and specifically the detection, treatment and monitoring patterns of vitamin B12 status. The purpose of this study was to describe the practices of Ontario LTC homes for the detection, treatment and monitoring of vitamin B12 status and whether these practices vary based on characteristics of the LTC home (e.g., location, profit status and corporate structure). Specifically: 1) does vitamin B12 screening occur at admission to LTC; 2) as there is no standardized cut-point used to define and diagnose B12 deficiency, what cut-points are used by LTC homes; 3) what types of vitamin B12 treatment are used in LTC; and 4) how often/does monitoring of B12 status occur in LTC?
Methods
Study Design and Participants
This was a cross-sectional study with data collected through phone interviews with the directors of nursing or an alternative knowledgeable informant from the randomly selected long-term care home. Data were collected between August and December, 2013.
Sampling and Recruitment
The Ontario Long Term Care Association (OLTCA) and the Ontario Association of Non-profit Homes and Services for Seniors (OANHSS) member listings were chosen to provide the widest and largest coverage of Ontario LTC homes. These listings have representation across private, municipal, charitable and non-profit long term care homes. OLTCA and OANHSS were selected instead of the Ontario Ministry of Health and Long-Term Care (MOH-LTC) public reporting site as they provided the necessary detailed information for stratification purposes, as well as up-to-date contact information for the home administrator. These combined associations’ members provide care to approximately 106,000 residents living in LTC in Ontario (70,000 and 36,000 from OLTCA and OANHSS respectively) [20, 21]. A list of all Ontario LTC homes in the OLTCA and OANHSS was compiled (N=651). After removal of long-term care hospitals, recently closed homes, or LTC homes with 0 reported beds (n=31), the remaining 620 homes were then stratified by covariates based on corporate structure and geography.
A home was classified as either for-profit (n=359) or not-for-profit (n=261) as defined by the OLTCA reporting website and/or OANHSS membership. It was hypothesized that for-profit homes may have different protocols than not-for-profit, with respect to preventative practices such as screening for B12 deficiency. A home was classified as either an umbrella (n=445) home or a non-umbrella (n=175) home. Umbrella status was defined as any group of two or more homes owned or operated by the same company. It was hypothesized that umbrella homes may have a different structure that supported policy and practice implementation. A home was classified geographically based on the Local Health Integration Network (LHIN) in which it resides. Geographical region was then categorized as South-Western (n=327), Eastern (n=94), Northern (n=56) or Central Ontario (n=143); it was hypothesized that geographical region and density of LTC homes within a geographical region may impact how policy and practice are implemented particularly with respect to ordering of blood tests. As this was a descriptive study, a random stratified sample consisting of approximately 10% of these homes was desired as potential participating sites. With a goal of recruiting 45-60 sites, 194 homes were invited, assuming a participation rate of approximately 30%.
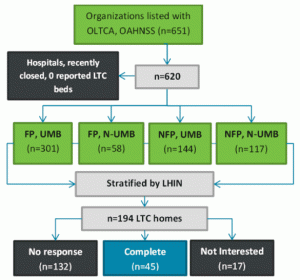
Three methods of contact were used for recruitment: 1) initial hard copy letter to the LTC home explaining the purpose and importance of the project, 2) email to the administrator, and 3) phone call issued to director of care. Figure 1 provides the flowchart depicting sample recruitment and inclusion. Only one hard copy letter was sent to each LTC home. If, in speaking with the informant, they failed to receive the letter, an electronic copy was sent. If there was no response after approximately 2 weeks, one initial email was sent to the administrator. If after three days there was no response, a follow-up email was sent to the same contact. A total of 83 emails and follow-up emails were issued. At least two phone contact attempts were made and up to two voicemails were left for the director of nursing care. If the LTC home advised on calling back later, this added to the number of phone-call attempts made. A total of 61 follow-up phone calls were issued in efforts to determine interest or schedule interviews. Once initial interest in participation was established, at least two more contact attempts were made to schedule and conduct the interview. Recruitment stopped when the 60 homes (plus an anticipated 10% loss) agreed to participate. Of the 68 LTC homes initially recruited, 45 followed through with data collection; participation rate was 23%.
Data Collection
Interviews were completed over the phone by the first author. Questions were provided to informants in advance to support completion of the interview. For missing data identified during the interview, at least one follow-up email or phone call was issued (n=14). Questions were developed by the authors based on the aims of the study. Some questions were modified for clarity after trialing with the first few homes.
Statistical Analyses
Due to proportionately fewer homes from Eastern, Northern, and Central Ontario, both across the LTC population and within our sample, these three geographical regions were collapsed for comparison against South-Western Ontario. This allowed for grouping of geographically higher density versus lower density LTC homes and increased the subsamples sufficiently to allow for statistical analyses.
Data were analysed using IBM SPSS Statistics version 21. Descriptive statistics were completed. A two proportion z test was conducted to establish whether the characteristics (e.g., geography, for-profit status) of participating homes differed significantly from those in the sampling frames. Chi-square or Fisher’s exact tests were conducted to determine whether site characteristics were associated with practices. Since LTC homes varied in size, the proportion of residents receiving vitamin B12 and which form of treatment were reported. A weighted average was calculated by summing these proportions and dividing by the total number of homes reporting residents receiving treatment.
Results
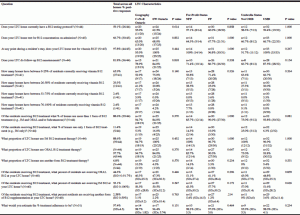
Forty-five participants/homes representing 5243 residents are included in this descriptive analysis. The sample was not found to be statistically different from the sampling frame/population by geography, umbrella status or profit/not profit designation (p>0.1, see Table 1). Table 2 provides a summary of descriptive variables by LTC characteristic; Table 3 provides a summary of additional phone interview responses by question.
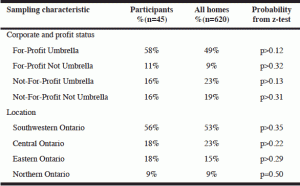
Table 1 Comparing proportions of study participants to all Ontario long-term care homes by corporate status, profit status and geography
*Whenever expected values in cells were greater than five, the χ2 test statistic was calculated with asymptotic 2-sided significance p-value. Whenever expected values in cells were less than five, the exact 2-sided significance p-value from the Fisher’s Exact Test was calculated. SD is the Standard Deviation of the mean. † RG is the range.
Detection
There was diversity in cut-off values used to determine B12 deficiency among the participating homes. The range of values used was 100-300 pmol/L. The most common cut-points to determine B12 deficiency wereAlmost all (44/45) of LTC homes reported that they requested a vitamin B12 test at some point during selected residents’ stay with the remaining home (a for-profit, non-umbrella, medium sized home, between 75-100 beds in Eastern Ontario) reporting that they never did B12 testing, although 21% of their residents were reported to be receiving B12 (85% on oral, 15% on IM). Despite this high reported testing for B12, only 59% (26/44) of homes noted that their home currently had a formalized B12 testing protocol. Further, only 67% (30/45) of the participating sites routinely tested for B12 concentration at admission of the resident to their LTC home. No significant differences were found on screening practices between LTC home characteristics for geography, for-profit status and umbrella status (p>0.20).
Treatment
Current treatment was used as a proxy for identified deficiency. One of the 41 homes reported that 100% of residents, regardless of admission blood work, were treated. This was a not-for-profit, not-umbrella, large home (between 150-175 beds) located in southwestern Ontario; all residents received monthly IM injections. Of the remaining 40 homes, a range of prevalence of residents currently receiving treatment was identified (Figure 2). Two-thirds of homes reported up to 25% of current residents were receiving treatment(s), while 29% report one-quarter to half of residents were currently receiving vitamin B12 treatment(s). A weighted average to compensate for differences in home size was calculated based on the number (or approximate number) of residents reported to be receiving B12; approximately 25% of residents were being treated across homes. No significant differences were found between proportion of residents receiving vitamin B12 treatment and LTC characteristics for geography, for-profit status and umbrella status (p>0.20).
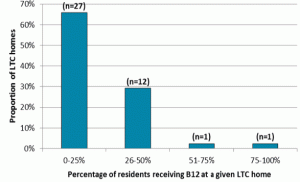
Figure 2 Distribution of the proportion of current residents reported receiving B12 at a given LTC home
Homes were asked to comment on treatment modality. Most homes offered more than one modality (38/43; 88.4%); 87.8% (36/41) of homes used oral, 97.6% (40/41) of homes use IM and 7.3% (3/41) of homes used another form of B12 treatment (subcutaneous injections). Only 5 homes (11.4%) exclusively offered vitamin B12 treatment via IM injections; 36 (81.8%) offered oral and IM; one home (2.3%) offered oral and subcutaneous; and two homes (4.5%) offered either oral, IM or subcutaneous B12 treatment. No significant differences were found between which forms of B12 treatment therapy was offered by an LTC home and characteristics for geography, for-profit status and umbrella status (p>0.10).
Homes were also asked to comment on the proportion of residents receiving each type of treatment modality. Of the residents receiving B12 treatment at a given LTC home on average, 53.1% (range (RG) 0-100%) received treatment in the form of IM B12, followed by 44.3% (RG 0-91.7%) through oral B12 and, 2.58% (RG 0-50%) through another form (e.g., subcutaneous B12). In terms of dosage, IM ranged from 500 to 1000 mcg administered either monthly, bimonthly or biweekly and oral doses ranged from 50 to 1200 mcg administered daily. The remaining 4.5% (2/44) received vitamin B12 through regular subcutaneous injections of 1000 mcg administered either monthly or quarterly. No significant differences were found between the proportion of residents receiving a form of B12 therapy at a given LTC home and LTC characteristics for geography, for-profit status and umbrella status (p>0.10). Reported estimates (n=31) of adherence to B12 treatment were high at 97.4% with no significant difference across LTC characteristics (p>0.10). Several interviewees commented that adherence was high because administration of medications is the responsibility of medical staff, not the residents themselves.
Monitoring
There was no consistent procedure for frequency of follow-up tests. Overall, 36/44 (81.8%) homes reported some form of follow-up. One out of 44 homes (2.3%) was not sure if their home did follow-up testing in light of providing treatment to everyone, and 7/44 (15.9%) homes did not complete follow-up B12 testing. The remaining 36/44 (81.8%) of homes conducted the following form of follow-up testing: annually 22/44 (50%), semi-annually 2/44 (4.5%), quarterly 8/44 (18.2%), monthly 1/44 (2.3%), or only at the discretion of the attending physician 3/44 (6.8%). Among the homes that reported some form of follow-up, no significant differences were found between frequency of follow-up testing and LTC characteristics for geography, for-profit status and umbrella status (p>0.10).
Discussion
This work demonstrates a variety of practices with respect to detection, treatment and monitoring of vitamin B12 status in Ontario LTC. Specifically, different cut-points to define deficiency are used and ranged from 100-300 pmol/L in this sample; 67% (30/45) of the participating sites routinely tested for B12 concentrations at admission. Approximately 25% of residents were receiving B12 treatment across homes. Generally more than one treatment modality was offered by homes; 97.6% and 87.8% of homes offered IM and oral B12 respectively. Of residents receiving B12, 53.1% received treatment in the form of IM B12, followed by 44.3% in the form oral B12. While there was no consistency for how B12 status was monitored, the 81.8% of homes conducted some form of follow-up B12 testing.
Screening at admission and yearly thereafter is a potentially logical and effective practice. Residents who are highly vulnerable and potentially malnourished may move into LTC with an undiagnosed deficiency that can progressively impact their quality of life and health. The classic symptoms associated with vitamin B12 deficiency may be overlooked due to the general high degree of comorbidity in LTC; a blood test is the only way to confirm B12 status. As well, the non-specific symptoms associated with an untreated B12 deficiency may result in other investigations or treatments that lead to further comorbidity. As noted in this sample, approximately 25% were being treated, which suggests a prevalence consistent with screening to case find. With the relatively low cost of a serum B12 measure and, the simplicity and effectiveness of treatment, screening could be efficacious. However, it would be remiss to ignore the inherent challenges in defining screening protocols and the financial investment required for screening. With approximately 71,000 Ontario LTC residents 65+ years of age (22), assuming 30% are new admissions each year, and that a serum B12 test costs on average $12.50 CDN (23), the cost for B12 screening using would be approximately $1.2 million CDN annually (not accounting for treatment and monitoring costs). With this in mind, there is a need both for further studies targeted at addressing the effect of treatment on improved clinical outcomes as well as a formal cost-benefit analysis for screening and subsequent treatment.
While residents on treatment were commonly monitored in some way, there were no consistent practices noted by respondents, such as timing. Two contrasting examples suggest specific gaps in monitoring. In the first case, the home (NFP, not-umbrella, 150-175 beds, in SW Ontario) provided treatment for all residents without admission or follow-up bloodwork concentrations. In the other case, the home (FP, not-umbrella, 75-100 beds, in Eastern Ontario) never conducted B12 testing, yet reported that 21% of residents received B12, 85% of whom received IM. It is unclear from where or how deficiency was identified and there is the potential that these individuals were fully treated and no longer needed supplementation. In the first case, treating all may be deemed efficient, low risk and avoids potential for incident cases of deficiency, but is a potential unnecessary cost to the system, especially if treated by IM. In the latter case, it may be that this home relied exclusively on home care or hospital transfer paperwork, bloodwork and thus B12 prescription. Furthermore, poor care transitions to LTC could also lead to care gaps. For example, a resident may have been receiving B12 treatment in the community but after a poor care transition to LTC, the resident may have been identified as having a normal B12 concentration at admission to LTC and thus did not receive continued required treatment. Without a follow up test to indicate whether the resident’s B12 concentration remained constant or decreased (or increased), a change in B12 concentration could go unnoticed, and thus deficiency could develop.
The proportion of residents receiving B12 treatment could be used to roughly estimate prevalence of identified deficiency. Based on this work, prevalence of deficiency can be approximated at 25%. This estimate is consistent with prior LTC work both outside of Canada and in a recent Canadian study with estimates of B12 deficiency ranging from 7-14% (14, 17, 19, 24) and low-normal B12 estimates ranging from 34-36% (14, 17-19). Prior work demonstrates that B12 deficiency in older adults does respond readily to treatment (24-26), potentially improving the quality of life, cognition and function of older adults living in long-term care. Future work on efficacy of screening should also consider these outcomes as well as determine the cost-benefit of screening, treatment and monitoring protocols.
Strengths and Limitations
It is anticipated that there is selection bias in these data as homes that decided to participate are likely different in some way from those that did not. However, strengths of this study were that the sample was randomly selected and found to not significantly differ from the population of the sampling frame on key characteristics. As well, the sample and their responses were diverse. For example in one home, all residents were treated with B12 contrasted by another home in which no B12 testing was completed. In addition, the minimum desired sample size of 45 homes was met. That said, sample size representing less than 10% of the population and representation of only one region in Canada, limits generalizability of results. Despite several steps to recruit the sample a lower than desired participation rate (23%) occurred. However, this rate is consistent or better than prior research using similar methods with LTC providers. For example the following participation rates were reported in surveys completed by directors of nursing care (8% (27), 11% (28), 26% (29)), with nursing homes (18%) or nurse practitioners working in LTC (19% (30)). The sampling frame is also a limitation of this work. Two organizations in Ontario, which provide lists of members, were available and used to stratify this sample; yet coverage of the entire population of Ontario LTC homes was not 100%.
Interviews were conducted by only one interviewer which ensured consistency of how questions were presented and thus internal validity. While interviews relied on self-reporting, since this study is the first of its kind, there are currently no audits available so self-report is acceptable given the maturity of this field of research. These results are based on the report of a knowledgeable informant in the LTC home. To facilitate accurate responses, the questions were provided to the respondents before the interview, and the majority of respondents (30/45) systematically researched their answers, as evidenced by exact number of residents reported to be currently on B12 therapy. In addition, great lengths were taken to minimize missing data as 3 to 8 points of contact were issued. Despite this approach there was some missing data (range of proportion of missing data per question: 0 to 21%) and interpretation is cautioned for items with a higher level of non-response. As other parameters used to assess B12 status (e.g., MMA, Hcy) are not covered by the provincial medical plan, it was anticipated that B12 status would be solely determined by serum B12. Thus, interviewees were not asked how B12 status was determined, but rather if serum B12 was assessed which may have been a potential limitation. Objective measurement that can be confirmed by audit needs to be used in future research to understand prevalence and care practices. In spite of these limitations, this is the first comprehensive study to examine vitamin B12 testing protocols and even with a relatively small sample, has captured great diversity of practices. These data provide insight into the field of B12 testing in LTC where previously, none has been reported and act as a baseline for future studies on the vitamin B12 status of older adults living in LTC homes.
Conclusion
Although two-thirds of a stratified random sample of LTC homes in Ontario reported conducting admission bloodwork for screening B12 deficiency, there is no consistency in the detection, treatment and monitoring of this potential deficiency. Lack of standardization in cut-points to diagnose deficiency is a significant challenge for understanding prevalence and success with treatment. Once these concepts are better understood, evidence may further inform policy and practices that support adequate vitamin B12 status in LTC residents.
Acknowledgements: The authors would like to acknowledge participants for generously giving their time to complete interviews and Robert Amelard who assisted with recruitment for this study.
Funding: This study was funded in part by the Schlegel-University of Waterloo Research Institute for Aging.
Conflict of interest: All authors declared no conflict of interest with the contents of this work.
Ethical Standard: As approved by the University of Waterloo Ethics Board, verbal consent from participants was attained at the time of the telephone interview. The participants were provided a written information letter providing details of the study and at the beginning of the interview they were explicitly reminded of the purposes of the telephone interview for research and affirmed their consent to proceed.
References
1. Baik HW, Russell RM. Vitamin B12 deficiency in the elderly. Annu Rev Nutr 1999;19:357-77.
2. Lam I, Keller H, Duizer L, Stark K, Duncan AM. Nothing ventured, nothing gained: Acceptability testing of micronutrient fortification in long-term care. J Nurs Home Res 2015;1:9.
3. Allen LH. Causes of vitamin B12 and folate deficiency. Food Nutr Bull 2008;29(2 Suppl):S20-34; discussion S35-7.
4. Rosenberg IH, Miller JW. Nutritional factors in physical and cognitive functions of elderly people. Am J Clin Nutr 1992;55(6 Suppl):1237S-1243S.
5. Vogiatzoglou A, Smith AD, Nurk E, et al. Cognitive function in an elderly population: interaction between vitamin B12 status, depression, and apolipoprotein E epsilon4: the Hordaland Homocysteine Study. Psychosom Med 2013;75(1):20-9.
6. Wolters M, Strohle A, Hahn A. Cobalamin: a critical vitamin in the elderly. Prev Med 2004;39(6):1256-66.
7. Bottiglieri T, Hyland K, Reynolds EH. The clinical potential of ademetionine (S-adenosylmethionine) in neurological disorders. Drugs 1994;48(2):137-52.
8. Hector M, Burton JR. What are the psychiatric manifestations of vitamin B12 deficiency? J Am Geriat Soc 1988;36(12):1105-12.
9. Isenring EA, Banks M, Ferguson M, Bauer JD. Beyond malnutrition screening: appropriate methods to guide nutrition care for aged care residents. J Acad Nutr Diet 2012;112(3):376-381.
10. Ducak K, Keller HH. Menu planning in long-term care: toward resident-centred menus. Can J Diet Pract Res 2011;72(2):83.
11. Lam IT, Keller HH, Duizer L, Stark K. Micronutrients on the Menu: Enhancing the Quality of Food in Long-term Care for Regular, Nontherapeutic Menus. Can J Diet Pract Res 2015;76(2):86-92.
12. Bronskill SE, Gill SS, Paterson JM, et al. Exploring variation in rates of polypharmacy across long term care homes. J Am Med Dir Assoc 2012;13(3):309.e15-21.
13. Andrès E, Loukili NH, Noel E, et al. Vitamin B12 (cobalamin) deficiency in elderly patients. Can Med Assoc J 2004;171(3):251-259.
14. Mirkazemi C, Peterson GM, Tenni PC, Jackson SL. Vitamin B12 deficiency in Australian residential aged care facilities. J Nutr Health Aging 2012;16(3):277-80.
15. Sloane PD, Ivey J, Helton M, Barrick AL, Cerna A. Nutritional issues in long-term care. J Am Med Dir Assoc 2008;9(7):476-85.
16. Dietitians of Canada. Food Sources of Vitamin B12. 2014. 4.
17. Paulionis L, Kane SL, Meckling KA. Vitamin status and cognitive function in a long-term care population. BMC Geriatr 2005;5.
18. Gharaibeh MY, Gahtan RA, Khabour OF, Alomari MA. Science. Hyperhomocysteinemia, low folate, and vitamin B12 deficiency in elderly living at home and care residences: a comparative study. Lab Med 2010;41(7):410-414.
19. Pfisterer KJ, Sharratt MT, Heckman GG, Keller HH. Vitamin B12 status in older adults living in Ontario long-term care homes: Prevalence and incidence of deficiency with supplementation as a protective factor. Appl Physiol Nutr Metab 2016;41(2):219-22.
20. Ontario Long Term Care Association (OLTCA). Welcome! Ontario Long Term Care Association. 2015. http://oltca.com/. Accessed 22 April 2015
21. Ontario Association of Non-Profit Homes and Services for Seniors (OANHSS). OANHSS Quick Facts. Ontario Association of Non-Profit Homes & Services for Seniors. 2015. https://www.oanhss.org/OANHSS/About_OANHSS/Quick_Facts_About_OANHSS/OANHSS/Navigation/AboutOANHSS/QuickFactsAboutOANHSS/Quick_Facts_About_OA.aspx?hkey=35b62b50-fa72-4931-b097-ef97f661194e. Accessed 22 April 2015
22. Canadian Institute for Health Information. Residential Long-Term Care Financial Data Tables 2012. 2012.
23. Health Quality Ontario. Serum vitamin B12 testing: a rapid review. 2012, Health Quality Ontario: Toronto. 16.
24. Baker H, Frank O, Jaslow SP. Oral versus intramuscular vitamin supplementation for hypovitaminosis in the elderly. J Am Geriat Soc 1980;28(1):42-45.
25. Favrat B, Vaucher P, Herzig L, et al. Oral vitamin B12 for patients suspected of subtle cobalamin deficiency: a multicentre pragmatic randomised controlled trial. BMC Fam Pract 2011;12:2.
26. Wouters-Wesseling W, Wouters AE, Kleijer CN, et al. Study of the effect of a liquid nutrition supplement on the nutritional status of psycho-geriatric nursing home patients. Eur J Clin Nutr 2002;56(3):245-51.
27. Buchanan RJ, Seibert AL, Crudden A, Minden S. Assessments of nursing home guidelines for quality of care provided to residents with multiple sclerosis. J Soc Work Disabil Rehabil 2013;12(4):237-55.
28. Lester PE, Stefanacci RG, Feuerman M. Prevalence and Description of Palliative Care in US Nursing Homes: A Descriptive Study. Am J Hosp Palliat Care 2016;33(2):171-7.
29. Aroian JF, Patsdaughter CA, Wyszynski ME. DONs in long-term care facilities: contemporary roles, current credentials, and educational needs. Nurs Econ 2000;18(3):149-56.
30. Rosenfeld P, Kobayashi M, Barber P, Mezey M. Utilization of nurse practitioners in long-term care: findings and implications of a national survey. J Am Med Dir Assoc 2004;5(1):9-15.