L. Duco1,2, C. Legendre1, N. Cohen3, C. Blochet4, P. Demornandie3, J.-F. Huon5, B. Sabatier1, O. Saint-Jean1,6
1. Geriatric Unit, Hôpital Européen Georges Pompidou, Paris, France; 2. Université Paris Descartes, Paris, France; Paris Sorbonne Cité, Paris, France; 3. Institut Bien Vieillir Korian, Paris France; 4. Medissimo, Paris, France; 5. Pharmacie clinique et Santé Publique, Faculté des sciences pharmaceutiques, Nantes, France; 6. Université Paris Descartes, Paris, France; Paris Sorbonne Cité, Paris, France. Corresponding author: Laurence Duco, 20 rue Leblanc, 75015, Paris, France, Phone/Fax : +33156093313/+330156093821
Jour Nursing Home Res 2016;2:71-75
Published online August 9, 2016, http://dx.doi.org/10.14283/jnhrs.2016.10
Abstract
Objective: Describe recent use of medication in France in the advanced in age who live at home or in nursing homes. Design: Observational study, data collected the fourth quarter 2011. Setting: Community dwelling older (≥70 years old) and elderly living in nursing homes (>70 years old). Participants: 72 556 patients living at home, covered by at least one of the three health insurance schemes in France (Echantillon Généraliste des Beneficiares) and 5867 patients in nursing homes. Measurement: The subjects aged 70 or over in the two databases are divided into 10-year ranges. For each of which, we determined the percentage use of medication, the number of drugs per person, and the percentage of users of each drug in the 74 categories according to the Anatomical Therapeutic and Chemical. Results: The patients living at home used 8.7 drugs on average, and 7.7 by patients from nursing homes. 87.4% of elderly patients living at home and 99.3% of elderly in institution were using medication during the study period. The drug classes most used were analgesics, psychotropic medications, cardiovascular and gastrointestinal drugs. Antidepressants such as serotonin reuptake inhibitors, anxiolytics, and antipsychotic medication were prescribed in respectively 27.9%, 38.8%, and 22.3% of patients in nursing homes versus 9.6%, 23.6%, and 4.4% of patients living at home. Renin-angiotensin system inhibitors and beta-blockers were prescribed more among patients living at home. Statin use was greater among elderly living at home than in nursing homes (35% versus 19%). Conclusion: Our data confirm that the elderly in France consume large amounts of medication, whether they live at home or in nursing homes. Extensive use of medication among the elderly and doubts regarding its misuse highlight the importance of reviewing prescriptions during a comprehensive geriatric assessment.
Key words: Elderly, drug use, polymedication.
Introduction
Elderly subjects have multiple comorbidities comprising acute diseases and chronic illnesses with potential acutisation. For these conditions they take multiple medications in long- and short-term treatments and so are heavy users of medication. Use of medication by the elderly varies between countries and changes with advances in geriatric medicine. Literature shows misuse of medication in elderly populations, such as under-prescription, over-prescription, and irrelevant prescriptions (1–9). This misuse appears to be responsible for serious iatrogenic disease or loss of opportunity for patients (10–18), explaining why policies have been implemented to promote correct use of medication in the elderly in France (19–26).
However, actual use of medication by elderly French people is poorly understood. The data are incomplete and relate to samples that are not representative of the general population (27–31). There is not, to our knowledge, large data on drug consumption in nursing homes and therefore no study describing the comparison between drug use in elderly living at home and in institution. The purpose of this study was to describe recent use of medication in French elderly subjects living at home or in nursing homes.
Methods
Elderly people living at home were studied in a sample of 1/97th of all people covered by at least one of the three health insurance schemes in France (ie, 86% of the French population). This sample (Echantillon Généraliste des Bénéficiaires, EGB) (32–34) is representative in terms of age and morbidity, but excludes people living in nursing homes. For each subject, the data include all medical services reimbursed, notably all drugs prescribed by a physician and reimbursed after purchase at a pharmacy. So we determine the percentage of subjects who are reimbursed for drugs, as well as the number and names of the drugs taken.
People living in nursing homes were studied from a group of 63 establishments accommodating 5673 residents, whose records include identification of drugs prescribed. These nursing homes are owned by the Korian group, which residents belong mainly to the upper social class.
Each drug is identified according to the Anatomical Therapeutic and Chemical (ATC) classification (35), which comprises 14 main groups each subdivided into four additional levels. For reasons of convenience, we have chosen to classify all the drugs in 74 categories that we deemed relevant in describing treatments in a population of elderly subjects (Appendix 1). This methodological choice was made by a working group consisting of a clinician, two pharmacists, and statistician.
We analyzed use of medication during the last quarter of 2011. We selected subjects aged 70 or over in the two databases and divided them into 10-year ranges, for each of which we determined the percentage use of medication, the number of drugs per person, and the percentage of users of each drug in the 74 categories. As many marketed products include more than one active ingredient, we considered that the user was taking as many drugs as there were active ingredients. In the analysis we only considered drug categories taken by at least 10% of the population in a given age range.
The results are presented by separating the patients living at home from those in nursing homes. The prevalence of use of drugs in the chosen categories was compared between the two patients populations, using relative risk and the 95% confidence interval, taking patients living at home as the reference.
Results
Of the patients aged 70 or over, 72 556 were living at home and 5867 in a nursing home. Of those living at home, 87.4% (63 421) had been reimbursed for drug prescribed; in nursing homes the percentage was 99.3%. Among the patients living at home, 56.2% were aged between 70 and 79, 36.5% between 80 and 89, 6.5% between 90 and 99 years, and 0.2% were aged 100 or more. Among patients in nursing homes, 10.3% were aged between 70 and 79, 50.7% between 80 and 89, 34.3% between 90 and 99, and 4.7% were aged 100 years or more.
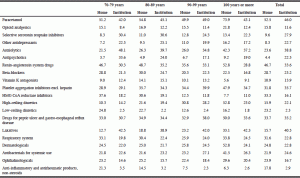
Table 1 Percentage use of medication by age for categories of drugs taken by at least 10% of patients, at home or in institution
During the study period, the patients living at home used 8.7 drugs on average: 8 for those aged 70 to 79, 9.5 for 80 to 89, 9.5 for 90 to 99, and 7.7 for those aged 100 or more. The mean number of drugs used by nursing home patients was 7.7 among the 70- to 89-year-olds, 7.4 for those aged 90 to 99, and 6.7 for those who were 100 years or over.
The drug classes most used were analgesics, psychotropic medications, and cardiovascular and gastrointestinal drugs. Table 1 shows the percentage use of each drug category according to age range among the two patient populations. The prevalence of use of drugs in the chosen categories was compared between the two patients populations, using relative risk and the 95% confidence interval, taking patients living at home as the reference (table 2).
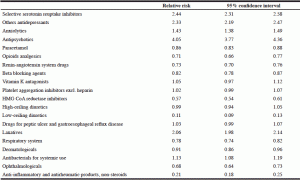
Table 2 Use of categories of drugs (relative risk, 95% confidence interval) by patients aged 80 or more (patients living at home taken as the reference)
Among analgesics, paracetamol, the main drug of step 1 on the World Health Organization (WHO) Pain Ladder (36), was taken by approximately 50% of patients, regardless of age and whether they were living at home (52.5%) or in nursing homes (46%). Opioid analgesics were taken by 15.8% of patients living at home (versus 11.6% of those in elderly care homes) and their use did not change with age (relative risk [RR]=0.71, 95% CI [0.66-0.77] in those aged 80 or more, patients living at home as reference).
Among psychotropic drugs, antidepressants such as serotonin reuptake inhibitors, anxiolytics, and antipsychotic medication were prescribed in respectively 27.9%, 38.8%, and 22.3% of patients in nursing homes versus 9.6%, 23.6%, and 4.4% of patients living at home (RR respectively 2.44, 1.43, 4.05 for those aged 80 or over, living at home as reference). Use of psychotropic drugs decreased very little with age. On average, use of antiepileptics was twice as common among patients in nursing homes (13.8% versus 6.3%), and declined slightly from after 80. Symptomatic treatments of dementia were also more common in nursing homes (28.9% versus 1.9% in those aged 80 or over, RR 14.84), but use decreased with age (34.9% for 80- to 89-year-olds versus 16.4% in those aged 100 or more).
Among cardiovascular treatments, renin-angiotensin system inhibitors were prescribed more among patients living at home (46.8% versus 34% in those aged 80 or over, RR=0.73, 95% CI [0.70-0.75], with living at home as reference), and their use did not change with age. Beta-blockers were also prescribed more for patients living at home (28.5% versus 23.4%, RR=0.82 95% CI [0.78-0.87], with living at home as reference), with a clear decrease in those aged 100 or more. The use of vitamin K antagonists and antiplatelet drugs by patients aged between 70 and 100 was roughly comparable in the two populations: about one patient in 3 was taking antiplatelet drugs and one in 10 vitamin K antagonists. For those aged 100 or over, almost one in 2 patients living at home was taking antiplatelet drugs (47.9% versus 34.7%), whereas vitamin K antagonists were prescribed more in nursing homes (9.1% versus 5.6%). Statin use was greater among 70- to 90-year-olds living at home than in nursing homes (35% versus 19%), whereas above 90 years of age it was roughly equivalent. Use of loop diuretics was more or less equal in the home-based and institutionalized populations at ages 70 to 100, but increased with age. Thiazide diuretics were little used in elderly care homes, but were taken by 23% of patients living at home.
Use of gastroprotective agents (almost exclusively proton pump inhibitors) was similar in patients living at home (33.7%) and in nursing homes (35.2%), and peaked in those aged 100 or over. Laxatives were used by over 40% of patients in nursing homes (versus 15.7% of those living at home). Percentage use did not change with age in nursing homes, but increased among patients living at home.
Respiratory, dermatological, and ophthalmological treatments, as well as antibiotics, were among the most frequently prescribed treatments: on average for patients living at home versus those in nursing homes, respectively, 31.6% versus 22.8%, 24.8%, versus 22.8%, 21.9% versus 24.6%, and 23.9% versus 16.7%.
Nonsteroidal anti-inflammatories and drugs for rheumatological diseases were little used in nursing homes (2.9% versus 17.8% in patients living at home). Use of medication among patients living at home decreased notably with age.
Discussion
Our data confirm that the elderly in France consume large amounts of medication, whether they live at home or in nursing homes. Almost 90% of elderly patients living at home were using medication during the study period. This use increased steadily with age and only decreased in patients aged 100 or more living at home. Use of medication was also very high in nursing homes and was less affected by age. The mean number of drugs taken by elderly patients reached almost 10 different active ingredients. The most frequently used medications were analgesics, cardiovascular drugs, psychotropic drugs, and gastrointestinal drugs. Among the different drug classes there were clear differences between patients living at home and those in nursing homes. This reflects different morbidity profiles and states of health, the clearest example of which was seen for mental health disorders.
Although the methodologies are different, it is instructive to compare our findings with data in the French literature. At the end of the 1990s, a summary of several partial studies indicated that 70% of 75- to 84-year-olds and 69% of those aged 85 or more used medication (29). One can therefore assume that more elderly subjects use medication today. In the 1990s, mean daily intake of medicinal products was 3.3 at 65 years and 4.6 among those aged 85 or more. Although the methodologies are different, our data suggest that the use of medication has practically doubled over the last 15 years. This increase in the number of drugs taken every day is also apparent when comparing our data with those of population cohorts in France. Nearly 10 years ago, in the ‘Personnes âgées QUID’ (PAQUID) (37) and Three-City Study (3C) (38) cohorts, the mean number of drugs taken by patients living at home was 4.5 and 4.4, respectively (27,28). Comparison of the types of drugs used in the late 1990s and today shows that several have disappeared, withdrawn from sale because of inefficacy. Before, elderly subjects took on average 4 drugs, a good proportion of which were ineffective. In contrast, all the drugs recorded in our study show genuine efficacy. Comparative data on elderly patients in nursing homes are scarce. Data from the PAQUID cohort showed that they were taking 5.2 drugs on average. A more recent french study (31), performed on about 43 000 subjects aged 75 and over, being part of the EGB, shows a prescription of about 8.4 drugs per individual living at home. The most drug classes are comparable to the results of our study.
A Swedish study (39) compared use of prescription drugs in patients aged 80 or over, living at home or in nursing homes, over the last quarter of 2008. In Sweden, 391 632 patients living at home were taking half as many drugs (median) in each age range as their counterparts in France. On the other hand, the median number of drugs taken by the 70 475 patients in Swedish nursing homes was slightly higher than among their counterparts in France. The same result is apparent for anxiolytics and antidepressants, use of which was more common in nursing homes (for antidepressants among 80- to 89-year-olds, 46.7% vs 12.1% for those living at home). Percentage use nonetheless remained lower in Sweden, notably for anxiolytics. Use of mild analgesics in nursing homes was equivalent in Sweden and France. In contrast, patients living at home clearly used less medication in Sweden than in France. Among cardiovascular treatments, renin-angiotensin system inhibitors were much less used in Sweden, whether patients were living at home or in nursing homes; beta-blockers, on the other hand, were used more in Sweden. In both cases, use of medication decreased with age. Gastroprotective agents and laxatives were less prescribed in Sweden than in France, both in patients living at home and in those in nursing homes. We have no data enabling analysis of the relevance of the prescriptions recorded. If we assume that morbidity among the advanced in age is similar in Sweden and France, a comparison of the levels of prescription between the two countries is suggestive of different medical practices.
Lastly, our findings regarding use of medication by elderly subjects living at home in France are close to those reported in a North American study (40), which reports that the average use per person and per day doubled between 1990 and 2010, from 2 to 4, and that the proportion of elderly subjects taking more than 5 drugs a day had tripled in 20 years (39%).
The weakness of the data concerning the morbidity of elderly subjects in France, especially those living at home, hampers a more qualitative analysis. A 2008 survey among 8972 subjects (41) representative of the elderly population in nursing homes showed that morbidity could be overestimated using data extracted from a questionnaire completed by the attending physician, using a cost-appraisal tool. A neurological or psychiatric disorder was observed in 82% of patients, and Alzheimer disease affected 36% of the nursing home residents, which seems to be an underestimate. Depression was observed in 34% of cases and anxiety in 27%. Three-quarters of the residents had cardiovascular disease, such as hypertension (52%), heart failure (23%), and heart rhythm disorders (22%). Whatever the limits of these data comparisons, the use of medication observed in our sample does not seem to be in contradiction with these epidemiological data. On the other hand, lack of epidemiological data on patients living at home jeopardizes qualitative interpretation of their use of medication. The data are incomplete and relate to causes of death or hospitalization, cohorts unrepresentative of the general population, or health policy objectives.
Conclusion
Extensive use of medication among the elderly and doubts regarding its misuse highlight the importance of reviewing prescriptions during a comprehensive geriatric assessment. Various ways of reviewing treatments in elderly patients have been proposed and in France are covered by good practice guidelines issued by the National Authority for Health (20,23–26).
References
1. Jackson SHD, Mangoni AA, Batty GM. Optimization of drug prescribing. Br J Clin Pharmacol. 2004 Mar;57(3):231–6.
2. Fick DM, Cooper JW, Wade WE, Waller JL, Maclean JR, Beers MH. Updating the Beers criteria for potentially inappropriate medication use in older adults: results of a US consensus panel of experts. Arch Intern Med. 2003 Dec 8;163(22):2716–24.
3. Curtis LH, Østbye T, Sendersky V, Hutchison S, Dans PE, Wright A, et al. Inappropriate prescribing for elderly Americans in a large outpatient population. Arch Intern Med. 2004 Aug 9;164(15):1621–5.
4. Hanlon JT, Schmader KE, Ruby CM, Weinberger M. Suboptimal prescribing in older inpatients and outpatients. J Am Geriatr Soc. 2001 Feb;49(2):200–9.
5. Fu AZ, Jiang JZ, Reeves JH, Fincham JE, Liu GG, Perri M. Potentially inappropriate medication use and healthcare expenditures in the US community-dwelling elderly. Med Care. 2007 May;45(5):472–6.
6. Lechevallier-Michel N, Gautier-Bertrand M, Alpérovitch A, Berr C, Belmin J, Legrain S, et al. Frequency and risk factors of potentially inappropriate medication use in a community-dwelling elderly population: results from the 3C Study. Eur J Clin Pharmacol. 2005 Jan;60(11):813–9.
7. Davidoff AJ, Miller GE, Sarpong EM, Yang E, Brandt N, Fick DM. Prevalence of potentially inappropriate medication use in older adults using the 2012 Beers criteria. J Am Geriatr Soc. 2015 Mar;63(3):486–500.
8. Zhang Y-J, Liu W-W, Wang J-B, Guo JJ. Potentially inappropriate medication use among older adults in the USA in 2007. Age Ageing. 2011 May;40(3):398–401.
9. Bao Y, Shao H, Bishop TF, Schackman BR, Bruce ML. Inappropriate medication in a national sample of US elderly patients receiving home health care. J Gen Intern Med. 2012 Mar;27(3):304–10.
10. Fauchais A-L, Ploquin I, Ly K, Rhaïem K, Bezanahary H, Tarnaud T, et al. [Adverse drug related events in a postemergency unit: prospective cohort study with 6 months follow up]. Rev Médecine Interne Fondée Par Société Natl Francaise Médecine Interne. 2006 May;27(5):375–81.
11. Pirmohamed M, James S, Meakin S, Green C, Scott AK, Walley TJ, et al. Adverse drug reactions as cause of admission to hospital: prospective analysis of 18 820 patients. BMJ. 2004 Jul 3;329(7456):15–9.
12. Tamblyn R, Laprise R, Hanley JA, Abrahamowicz M, Scott S, Mayo N, et al. Adverse events associated with prescription drug cost-sharing among poor and elderly persons. JAMA. 2001 Jan 24;285(4):421–9.
13. Lau DT, Kasper JD, Potter DEB, Lyles A, Bennett RG. Hospitalization and death associated with potentially inappropriate medication prescriptions among elderly nursing home residents. Arch Intern Med. 2005 Jan 10;165(1):68–74.
14. Beijer HJM, de Blaey CJ. Hospitalisations caused by adverse drug reactions (ADR): a meta-analysis of observational studies. Pharm World Sci PWS. 2002 Apr;24(2):46–54.
15. Dedhiya SD, Hancock E, Craig BA, Doebbeling CC, Thomas J. Incident use and outcomes associated with potentially inappropriate medication use in older adults. Am J Geriatr Pharmacother. 2010 Dec;8(6):562–70.
16. Kanaan AO, Donovan JL, Duchin NP, Field TS, Tjia J, Cutrona SL, et al. Adverse drug events after hospital discharge in older adults: types, severity, and involvement of Beers Criteria Medications. J Am Geriatr Soc. 2013 Nov;61(11):1894–9.
17. Koyama A, Steinman M, Ensrud K, Hillier TA, Yaffe K. Long-term cognitive and functional effects of potentially inappropriate medications in older women. J Gerontol A Biol Sci Med Sci. 2014 Apr;69(4):423–9.
18. Hines LE, Murphy JE. Potentially harmful drug-drug interactions in the elderly: a review. Am J Geriatr Pharmacother. 2011 Dec;9(6):364–77.
19. DE LA PRESCRIPTION PD. PLATE-FORME D’ECHANGES HAS PMSA. 2012 [cited 2016 Apr 27]; Available from: http://www.has-sante.fr/portail/jcms/c_1637200/fr/pleniere-has-pmsa-29-12-2012-projets-amelioration
20. Blain H, Rambourg P, Le Quellec A, Ayach L, Biboulet P, Bismuth M, et al. Bon usage des médicaments chez le sujet âgé. Rev Médecine Interne. 2015 Oct;36(10):677–89.
21. Laroche M-L, Bouthier F, Merle L, Charmes J-P. Médicaments potentiellement inappropriés aux personnes âgées : intérêt d’une liste adaptée à la pratique médicale française. Rev Médecine Interne. 2009 Jul;30(7):592–601.
22. Lang P-O, Hasso Y, Belmin J, Payot I, Baeyens J-P, Vogt-Ferrier N, et al. [STOPP-START: adaptation of a French language screening tool for detecting inappropriate prescriptions in older people]. Can J Public Health Rev Can Santé Publique. 2009 Dec;100(6):426–31.
23. Améliorer la prescription des psychotropes chez le sujet âgé. Propositions d’actions concertées. [Internet]. [cited 2016 Apr 27]. Available from: http://www.has-sante.fr/portail/upload/docs/application/pdf/rapport_psychotropes_version_longue_190208.pdf
24. Modalités d’arrêt des benzodiazépines et médicaments apparentés chez le patient âgé. [Internet]. [cited 2016 Apr 27]. Available from: http://www.has-sante.fr/portail/upload/docs/application/pdf/synthese_bzd_-_version_finale_2008.pdf
25. Pasquier F. [Professional guidelines for the diagnosis and management of Alzheimer’s disease and related diseases, HAS (Haute Autorité de Santé) 2008]. Rev Neurol (Paris). 2008 Sep;164(8–9):753–4.
26. Haute Autorité de Santée (HAS). [Diagnosis and management of Alzheimer’s disease and related diseases]. Rev Neurol (Paris). 2008 Sep;164(8–9):754–74.
27. Emeriau JP, Fourrier A, Dartigues JF, Begaud B. [Drug prescriptions for the elderly]. Bull Académie Natl Médecine. 1998;182(7):1419-1428-1429.
28. Fourrier A, Letenneur L, Dartigues J, Decamps A, Begaud B. Consommation médicamenteuse chez le sujet âgé vivant à domicile et en institution à partir de la cohorte Paquid : importance de la polymédication et utilisation des psychotropes. In: La Revue de gériatrie [Internet]. Gériamed; 1996 [cited 2015 Jul 17]. p. 473–82. Available from: http://cat.inist.fr/?aModele=afficheN&cpsidt=3232624
29. Auvray L, Sermet C. Consommations et prescriptions pharmaceutiques chez les personnes âgées: Un état des lieux. Gérontologie Société. 2002;103(4):13.
30. Huon J-F, Lenain E, LeGuen J, Chatellier G, Sabatier B, Saint-Jean O. How Drug Use by French Elderly Patients Has Changed During the Last Decade. Drugs – Real World Outcomes. 2015;2(4):327–33.
31. Le Cossec C. La polymédication au regard de différents indicateurs de sa mesure: impact sur la prévalence, les classes thérapeutiques concernées et les facteurs associés. Paris: IRDES; 2015.
32. Moulis G, Lapeyre-Mestre M, Palmaro A, Pugnet G, Montastruc J-L, Sailler L. French health insurance databases: What interest for medical research? Rev Médecine Interne Fondée Par Société Natl Francaise Médecine Interne. 2015 Jun;36(6):411–7.
33. Tuppin P, de Roquefeuil L, Weill A, Ricordeau P, Merlière Y. French national health insurance information system and the permanent beneficiaries sample. Rev Dépidémiologie Santé Publique. 2010 Aug;58(4):286–90.
34. Roquefeuil LD, Studer A, Neumann A, Merlière Y. L’échantillon généraliste de bénéficiaires : représentativité, portée et limites. Prat Organ Soins. 2009 Sep 1;40(3):213–23.
35. Skrbo A, Begović B, Skrbo S. [Classification of drugs using the ATC system (Anatomic, Therapeutic, Chemical Classification) and the latest changes]. Med Arh. 2004;58(1 Suppl 2):138–41.
36. Vargas-Schaffer G. Is the WHO analgesic ladder still valid? Twenty-four years of experience. Can Fam Physician Médecin Fam Can. 2010 Jun;56(6):514–7, e202-205.
37. Dartigues J-F, Helmer C, Letenneur L, Péres K, Amieva H, Auriacombe S, et al. Paquid 2012 : illustration et bilan. Gériatrie Psychol Neuropsychiatr Vieil. 2012 Sep 1;10(3):325–31.
38. 3C Study Group. Vascular factors and risk of dementia: design of the Three-City Study and baseline characteristics of the study population. Neuroepidemiology. 2003 Dec;22(6):316–25.
39. Wastesson JW, Parker MG, Fastbom J, Thorslund M, Johnell K. Drug use in centenarians compared with nonagenarians and octogenarians in Sweden: a nationwide register-based study. Age Ageing. 2012 Mar;41(2):218–24.
40. Charlesworth CJ, Smit E, Lee DSH, Alramadhan F, Odden MC. Polypharmacy Among Adults Aged 65 Years and Older in the United States: 1988-2010. J Gerontol A Biol Sci Med Sci. 2015 Aug;70(8):989–95.
41. CALVET L, MONTAUT A. Dossiers solidarité et santé. Dépenses de soins de ville ds personnes âgées dépendantes. Des dépenses comparables en institution et à domicile. 2013 [cited 2016 Apr 27]; Available from: http://drees.social-sante.gouv.fr/IMG/pdf/article42.pdf
