R. Backhaus1, E. van Rossum1,2, H. Verbeek1, R.J.G. Halfens1, F.E.S. Tan3, E. Capezuti4, J.P.H. Hamers1
1. CAPHRI School for Public Health and Primary Care, Department of Health Services Research, Maastricht University, Maastricht, The Netherlands; 2. Zuyd University of Applied Sciences, Research Centre on Autonomy and Participation, Heerlen, The Netherlands; 3. CAPHRI School for Public Health and Primary Care, Department of Methodology and Statistics, Maastricht University, Maastricht, The Netherlands; 4. Hunter College, City University of New York, New York, NY. Corresponding author: Ramona Backhaus, Maastricht University, Faculty of Health, Medicine and Life Sciences, CAPHRI School for Public Health and Primary Care, Department of Health Services Research, P.O. Box 616, 6200 MD Maastricht, The Netherlands, Telephone: 0031-43 3882456, Email: r.backhaus@maastrichtuniversity.nl
Jour Nursing Home Res 2016;2:90-93
Published online August 17, 2016, http://dx.doi.org/10.14283/jnhrs.2016.13
Abstract
The general belief is that the number of total staff hours per resident day (HPRD) and the staff mix (% registered nurses/total staff) are associated with quality of care (QoC) in nursing homes. However, findings from studies examining these relationships are inconsistent. In this brief report, we present findings from a cross-sectional, observational study on the relationship between HPRD and clinical as well as staff-reported QoC indicators. Data were collected in 55 nursing home wards that participated in the Dutch Prevalence Measurement of Care Problems in April 2014. We conducted adjusted (multilevel) logistic regression analyses for clinical outcomes and multilevel linear regression analyses for staff perception of QoC. Overall, we were unable to demonstrate a relationship between HPRD and QoC. Our findings underscore that focusing on quantity of nursing care might not improve QoC in nursing homes. The quality of the team should be taken into consideration as well.
Key words: Staffing, quality of care, nursing homes.
Introduction
In many European countries, concerns about nursing home quality have led to political discussions on increasing funding, as it is widely assumed that more resources are needed to improve quality of care (QoC) in nursing homes (1). A general, persistent belief is that the number of total staff hours per resident day and the staff mix (% registered nurses/total staff) are associated with QoC in nursing homes. Studies examining this relationship have mostly been conducted in the US and findings are inconsistent (2-5). Findings based on US data cannot be generalized to European countries, as educational backgrounds of nursing staff differ. For example, in the US, a minimum of 75 hours of initial training are required to become a certified nurse assistant (6), while in the Netherlands, the length of the educational program to become a nurse assistant is two years. First European studies show that evidence for a relationship between the number of total staff hours per resident day or the staff mix and QoC in nursing homes is lacking (7-10). Studies that find a positive relationship mostly analyzed facility-level data from large US databases (e.g., OSCAR (Online Survey, Certification and Reporting)) that are not primarily intended for research purposes (2,4). The accuracy of staffing data in such databases might be doubted, as they not necessarily reflect reality (5). Moreover, data on staffing and QoC in these databases do not necessarily cover the same time periods, meaning that researchers are analyzing non-contemporaneous data (4).
In addition, in many studies, QoC is operationalized only as clinical resident outcomes, such as the prevalence of falls or nosocomial pressure ulcers. A limitation of these outcomes is that they only give an indication of QoC at one time point. As staffs’ perception of QoC develops over time and is not based on isolated care components (7), it is an important addition to clinical outcomes. Staffs’ perception of QoC has been used in evaluating care in other settings and is considered a valid proxy measure of QoC (7,11).
Evidence on the relationship between quantity of staff or the staff mix and staffs’ perception of QoC in nursing homes is lacking. In this brief report, we present data on the relationship between the number of staff hours per resident as well as the staff mix and QoC in Dutch nursing homes. We included clinical outcomes as well as staff perception of QoC to assess these relationships.
Methods
A cross-sectional, observational study was conducted among 55 wards within 21 nursing homes that participated in the Dutch Prevalence Measurement of Care Problems (LPZ) in April 2014. The LPZ is a cross-sectional point prevalence measurement of several care problems (such as pressure ulcers and fall incidents), taking place annually on the same day in different health care settings (12). Unlike in some other countries, a national database on staffing and QoC is lacking in the Netherlands (13) and participation in the LPZ is voluntary. Data collection takes place on one day at facility, ward, and resident level, using standardized questionnaires that are based on psychometrically tested instruments or existing guidelines and literature reviews. The questionnaires are developed and regularly updated in collaboration with expert groups. In this study, we only used data measured on resident level (resident characteristics and prevalence of clinical QoC outcomes). Data are collected according a standardized protocol. Within each ward, two health care professionals collected data on resident level. One professional was working on the residents’ ward and one was from another ward. Inter-rater reliability between observers was tested to be good (Cohen’s kappa 0.87) (12, 14, 15). The Medical Ethics Review Committee of the University Hospital Maastricht and Maastricht University approved the study protocol (METC14-4-057).
Resident characteristics (age, gender, length of stay, comorbidities, care dependency status) as well as clinical QoC outcomes (dichotomized (yes/no)) – nosocomial pressure ulcers, falls, antipsychotic drug use, medication incidents, urinary indwelling catheters – were extracted from the LPZ database. To obtain insight into staff perception of QoC, at least five staff members from every ward were invited to assess the QoC on their ward. They graded the overall QoC on their ward (grade 1-10, higher score indicating better QoC) and were asked to which extent they agreed with the statement “In case a family member had to be admitted to a nursing home now, I would recommend this ward” (completely not agree (1) – completely agree (5)).
Based on their ward roster, ward managers provided average total direct care staff hours for an average day within the last seven days. Based on the actual ward roster, they described the number of direct care staff members that worked on that day (morning (7:00 am – 12:00 noon), day (12:00 noon – 5:00 pm), evening (5:00 pm – 11:00 pm), and night (11:00 pm – 7:00 am) shifts), each staff members’ educational background and the exact start and finish time of their shift. Direct care staff consisted of (certified) nurse assistants, nurse aids, specially trained feeding assistants, trainees, untrained staff, and vocationally or baccalaureate-educated registered nurses (RNs). For each ward the total direct care staff hours per resident per day were calculated, further referred to as hours per resident per day (HPRD). In addition, the staff mix was calculated for each ward.
Separate analyses were performed for somatic and psychogeriatric wards due to differences in prevalence of clinical outcomes. We estimated the relationship between HPRD and QoC (dependent variable), adjusting for ward size and resident characteristics (i.e., age, gender, length of stay, number of comorbidities, and care dependency status). We conducted (multilevel) logistic regression analyses for clinical outcomes and multilevel linear regression analyses (random intercept) for staff perception of QoC.
Results
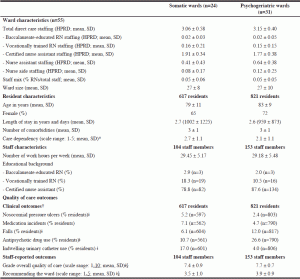
Descriptive statistics are described in Table 1.
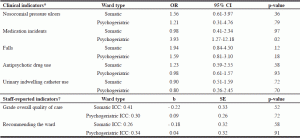
Overall, a relationship between HPRD and clinical resident outcomes was not found. For each outcome, the multilevel and the fixed-effects logistic regression analyses were almost identical, and the ICC was low (ICC ≤ 0.04). Therefore, only the results of the fixed-effects logistic regression are reported (Table 2). For residents from both ward types, the probability of experiencing nosocomial pressure ulcers, falls, antipsychotic drug use, or urinary indwelling catheters was not significantly associated with HPRD (with odds ratios between 0.80 and 1.94; Table 2). For residents living in psychogeriatric wards, however, higher HPRD were associated with a higher probability of experiencing a medication incident (odds ratio 3.93; 95% CI 1.27-12.18). This was not demonstrated for residents living in somatic wards (odds ratio 0.98). In addition, a relationship between HPRD and staff-reported QoC for both ward types was not found, as HPRD were not significantly associated with staff-reported QoC (with parameter estimates ranging from -.22 to .09; Table 2). Due to the low % of RNs in the participating wards, we were unable to estimate the relationship between staff mix and QoC.
Note: SD = standard deviation; * degree to which the resident is dependent upon care provided by others is indicated on a 5-point scale (completely dependent (1) – completely independent (5)); † Nosocomial pressure ulcers: Resident suffers from at least one nosocomial pressure ulcer category 2-4 (12); Medication incidents: Resident had at least one medication incident during the last 30 days (Omitted dose, wrong dose, wrong time taken, wrong drug, wrong drug administration); Falls: Resident has fallen at least once during the last 30 days; Antipsychotic drug use: Antipsychotic drug use during last 7 days; Indwelling urinary catheter use: Resident has an indwelling urinary catheter in place at the time; ǂ significantly different among somatic and psychogeriatric wards (p<.01; independent samples t-test or chi-square); § underlined score is the most favorable score
Note: OR = odds ratio; 95% CI = 95% confidence interval around OR; SE = standard error; ICC= intraclass correlation coefficient; * General logistic regression analyses: Fully adjusted models estimating the relationship between quantity of staff and clinical quality of care controlling for background characteristics, i.e. ward size, and residents’ age, gender, length of stay, number of comorbidities, and care dependency status. † Multilevel linear regression analyses (random intercept): Fully adjusted models estimating the relationship between quantity of staff and staff-reported quality of care controlling for background characteristics, i.e. ward size and residents’ mean age, gender (% female), length of stay, number of comorbidities, and care dependency status
Discussion
Our data analyses showed that the quantity of nursing staff was not related to clinical indicators as well as staff-perceived QoC in nursing homes. This is in line with the conclusions drawn in prior European studies (7-10).
Some methodological limitations should be considered. Due to the cross-sectional design, our findings should be interpreted carefully. Considering staff-reported QoC can be seen as a strength, as staffs’ perception of QoC is an important addition to clinical outcomes. However, staff-reported QoC is based on the subjective views of individual staff members who may interpret the concept of QoC differently. Moreover, we were unable to test the relationship between staff mix and QoC. A strength of the study was that data were of good quality as we made use of an existing data infrastructure (LPZ), collected actual staffing data directly from ward rosters and all data were collected at the same point in time.
Our findings underscore that adding extra manpower will not per se lead to better QoC in European nursing homes. Nevertheless, probably there is a minimum HPRD threshold below which the probability of poor QoC outcomes is higher. However, focusing on quantity of nursing care alone might be too simple to improve QoC. The relationship between staffing and QoC seems to be more complex. Instead of focusing on the quantity of staff, one should therefore consider the quality (i.e., skills and competencies) of the team. In future studies, the quality of the team should be considered as well. Besides educational backgrounds of nursing staff, the ward environment and work processes might contribute to QoC in nursing homes. Tentative evidence suggests that better educated staff, a positive organizational culture and good teamwork, communication and coordination may lead to better QoC in nursing home wards (7).
More information on the effects of ward environment (e.g., team climate) and work processes (e.g., communication or coordination), as well as the optimal allocation of nursing staff from different educational backgrounds is needed.
Funding: The research project was funded by ZonMW (project number: 520001003), the Netherlands Organization for Health Research and Development. The sponsor had no role in the design and conduct of the study; in the collection, analysis, and interpretation of data; in the preparation of the manuscript; or in the review or approval of the manuscript.
Conflicts of interest: All authors (RB, EvR, HV, RJGH, FEST, EC, JPHH) declare no conflicts of interest.
Ethical standards: The Medical Ethics Review Committee of the University Hospital Maastricht and Maastricht University approved the study protocol (METC14-4-057).
References
1. Giorgio LD, Filippini M, Masiero G. Is higher nursing home quality more costly? Eur J Health Econ 2015;[epub ahead of print].
2. Backhaus R, Verbeek H, van Rossum E, Capezuti E, Hamers JPH. Nurse Staffing Impact on Quality of Care in Nursing Homes: A Systematic Review of Longitudinal Studies. J Am Med Dir Assoc 2014;15:383-393.
3. Corazzini KN, Anderson RA, Mueller C, Thorpe JM, McConnell ES. Licensed practical nurse scope of practice and quality of nursing home care. Nurs Res 2013;62:315-324.
4. Spilsbury K, Hewitt C, Stirk L, Bowman C. The relationship between nurse staffing and quality of care in nursing homes: A systematic review. Int J Nurs Stud 2011;48:732-750.
5. Castle N. Nursing home caregiver staffing levels and quality of care. J Appl Gerontol 2008;27:375 – 405.
6. Han K, Trinkoff AM, Storr CL, Lerner N, Johantgen M, Gartrell K. Associations between state regulations, training length, perceived quality and job satisfaction among certified nursing assistants: cross-sectional secondary data analysis. Int J Nurs Stud 2014;51:1135-1141.
7. Zúñiga F, Ausserhofer D, Hamers JPH, Engberg S, Simon M, Schwendimann R. Are staffing, work environment, work stressors, and rationing of care related to care workers’ perception of quality of care? A cross-sectional study. J Am Med Dir Assoc 2015;16:860-866.
8. Huizing AR, Hamers JPH, de Jonge J, Candel M, Berger MP. Organisational determinants of the use of physical restraints: A multilevel approach. Soc Sci Med 2007;65:924-933.
9. Havig AK, Skogstad A, Kjekshus LE, Romøren TI. Leadership, staffing and quality of care in nursing homes. BMC Health Serv Res 2011;11:327.
10. Heeren P, Van de Water G, De Paepe L, Boonen S, Vleugels A, Milisen K. Staffing Levels and the Use of Physical Restraints in Nursing Homes: A Multicenter Study. J Gerontol Nurs 2014;40:48-54.
11. Aiken LH, Sermeus W, Van den Heede K, et al. Patient safety, satisfaction, and quality of hospital care: cross sectional surveys of nurses and patients in 12 countries in Europe and the United States. BMJ 2012;344:e1717.
12. van Nie-Visser NC, Schols JMGA, Meesterberends E, Lohrmann C, Meijers JM, Halfens RJ. An international prevalence measurement of care problems: study protocol. J Adv Nurs 2013;69:e18-e29.
13. Onder G, Carpenter I, Finne-Soveri H, et al. Assessment of nursing home residents in Europe: the Services and Health for Elderly in Long TERm care (SHELTER) study. BMC Health Serv Res 2012;12:5.
14. Meijers JM, Candel MJ, Schols JM, van Bokhorst-de van der Schueren MA, Halfens RJ. Decreasing trends in malnutrition prevalence rates explained by regular audits and feedback. J Nutr 2009;139:1381-1386.
15. Meijers JM, Schols JM, van Bokhorst-de van der Schueren MA, Dassen T, Janssen MA, Halfens RJ. Malnutrition prevalence in The Netherlands: results of the annual Dutch national prevalence measurement of care problems. Br J Nutr 2009;101:417-423.