R.B. Veenhuizen1,2,3, T. Hogeveen4, L.W. van Buul1,2,3, E.M. Wattel1,2,3, C.M.P.M. Hertogh1,2,3
1. University Network of Organizations for Care for the elderly of VU University Medical Center, UNO-VUmc, Amsterdam, PO Box 7057, 1007 MB Amsterdam, the Netherlands; 2. Department of General Practice and Elderly Care Medicine, VU University Medical Center, Amsterdam, the Netherlands; 3. EMGO Institute for Health and Care Research, Amsterdam, the Netherlands; 4. Beweging 3.0, Amersfoort, the Netherlands. Corresponding author: R. B. Veenhuizen, r.veenhuizen@vumc.nl, Tel +3120 444 9366, Fax nr.+3120 444 8234
Jour Nursing Home Res 2016;2:94-96
Published online August 19, 2016, http://dx.doi.org/10.14283/jnhrs.2016.14
Abstract
In this study exercise is investigated as preventive action for falling. Frequently falling nursing home residents exercised for 2 months on a daily basis under the guidance of a physiotherapist, who measured endurance with the 6 minute walking test, and kept a track record of falling incidents and attendance to the exercise group. 15 Nursing homes participated in this study. A total of 63 residents with falls in the previous 2 months enrolled in the study. The number of falls decreased from 67 per month to 25 in the second month of the intervention and to 43 in the first month after cessation of the intervention. The majority of the patients had a significant increase in endurance. This study suggests that a moderately intensive exercise program may lead to a significant reduction of falls. Further research, involving a control group, is warranted to support these findings.
Key words: Falls, exercise, nursing home, LTCF, fall prevention.
Introduction
Since 2015 the Dutch government demands nursing homes (NHs) to implement exercise programs for better health and wellbeing of their residents. This program should include 30 minutes of moderately intensive exercise for at least 5 days a week, and is called “mobility standard”. One of the NHs from our University Network of Organizations for Care for the elderly performed a pilot study evaluating this intervention. The researcher, a physiotherapist, hypothesized an increase of falls in frequently falling residents as a consequence of more mobility. However, a serious decrease of fall incidents (from 28 to 3 falls in 2 months’ time for 7 frequently falling residents) and an improvement of endurance was found instead. This triggered the set-up of a larger study, described in this article, in which we aimed to evaluate whether a daily exercise program could diminish the number of falls and improve endurance in NH residents. In addition, we aimed to investigate the feasibility of the program.
Methods
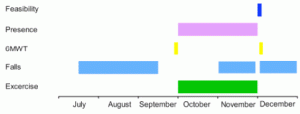
NHs from the University Network of Organizations for Care for the Elderly of the VU University Medical Center (UNO-VUMC, Amsterdam) were asked to participate in this small study with a before-after design. This network includes 20 elderly care organizations and the Department of General Practice & Elderly Care Medicine of VU University Medical Center Amsterdam. During a total of 2 months the intervention comprised a group therapy of about 6 residents per NH, who performed 5 minutes warming up, 30 minutes moderately intensive exercise (muscle strength, sit/stand exercises, balance in standing position, endurance) which implied tiresome exertion and 5 minutes cooling down. It was to the judgement of the attending physiotherapist whether the program was adapted to individual needs. The exercise groups were performed on the 5 weekdays in the end of the morning or midafternoon. Predictability in time of day, place and program was strived for. It varied between the NH’s whether the group was held in a special room or in the living room. Music familiar to the residents accompanied the exercise program. The exercise groups were organized and coordinated by physiotherapists employed by the NHs, who all followed the same exercise manual, which allowed room for professional expertise of the individual physiotherapist. Physiotherapists used balloons, cones, tinted rings for balance exercises, but this was not required. Patients were included if they were long term residents and had suffered 1 or more falling incidents in the 2 months prior to the initiation of the program, and if they were capable of understanding and executing instructions (including the 6 minute walking test) and participating in the group for 30 minutes. No other exclusion criteria were used. No precepts were ordered and no limitations or extra interventions to usual care and/or treatment. Before onset of the program (T0) fall incidents over the previous 2 months (July 15th – September 15th) were counted from the incident reporting system, which is obligatory for Dutch NHs, and the 6 minute walking test (6MWT) was assessed as a measure for endurance (Fig. 1). This test measures the distance a person can walk in 6 minutes (1). During the program, attendance was kept record of in a diary. Time and extra financial investments were investigated in a questionnaire at T2. After 2 months of intervention (T1) falls were counted over the month November and the 6MWT was reassessed. In December (T2, 1 month after the intervention stopped) the number of fall incidents was counted for the third time.
Data were collected in an Excel-database and SPSS 20 (Wilcoxon signed Rank test (α 0.05)) was used to calculate the difference between the 2 time points T1-T0.
No ethical approval was required, as the exercise program is considered usual care, the documentation of falls is common practice, and the 6MWTis an instrument commonly used in practice.
Results
Fall incidents
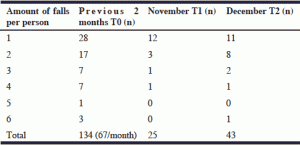
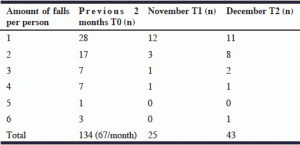
15 NHs agreed to participate and a total of 63 patients (59 psychogeriatric and 4 somatic) attended the exercise groups. 28 Patients had fallen once and 35 patients (the frequent fallers) 2 or more times in the 2 months prior to the intervention, see Table I. In total, these patients had fallen 134 times in 2 months (67/month).
In the second month (November) of the intervention fall incidents decreased to 25, which implies a 63% reduction. The month after the intervention stopped (December), fall incidents increased again to 43, which still is a 36% reduction compared to fall incidents measured before the intervention.
Endurance
At T1 data on 6 MWT were incomplete for 8 residents. At T0 the scores of the 55 remaining patients did not differ significantly from these 8 patients (p = 0.828). Of 55 patients 39 improved in their endurance, the overall scores on the 6 MWT improved significantly in comparison to T0 (see Table II).
* Wilcoxon signed rank test
Organization and Attendance
The exercise groups were organized by physiotherapists who were supported by activities supervisors, volunteers, others (trainees) and care personnel in decreasing frequency. The total time investment for the project ranged from 58 to 211 hours per organization. In 4 organizations, extra financial investments were made for personnel or purchase of small equipment.
The majority of the participants attended the exercise groups for 9 weeks with a mean of 7.4 weeks (std. 2.4). A minority of attendants could fulfil 5 days exercise per week, the mean frequency of attendance was 3.5 days a week (std. 0.9). Most common reasons for absence were shortage of supervisors, viral infection in the institution, participant situation (e.g. lack of motivation or not feeling fit for exercise). No relation was found between attendance to the exercise group and change in falling incidence or performance on the 6MWT.
Discussion
Falling is a serious problem amongst NH residents suffering from dementia. It may lead to injury and death in these frail elderly (2). A reduction of falls and related injuries was shown in this review on the efficacy of exercise programs. However, these studies were conducted in community dwelling frail elderly and not in NH residents (3). When psychogeriatric patients are admitted to a NH their risk of falling increases due to diminishing capacities to keep balance and to recognize and avoid hazards (4). Until now no unequivocal evidence is available on the reduction of falls in NH residents through exercise programs (5).
In this study a 2 months participation in an exercise group with mean frequency of 3.5 days a week was associated with a significant reduction in fall incidents among frequently falling NH residents. Moderately intensive exercise leading to such a decrease was not reported for this patient group before (5,6). Evidence on fall prevention programs in NHs is scarce. A few multifactorial intervention programs focusing on prevention did show significant reductions in falls for NH residents (4,8-10). One study conducted in another patient group, i.e. residents with intellectual disabilities, showed that obstacle training resulted in a substantial decrease in number of falls after the intervention (7).
Of course our study has limitations by its design. First, our design was uncontrolled and not randomized. So a firm conclusion that exercise diminishes fall incidents cannot be drawn. Second, the intervention was executed by 15 different supervisors, which could result in a diversity within the intervention. Nevertheless, the physiotherapists who were in charge of these groups all received identical training encompassing the same instruction meeting and written manuals of the exercise program. Third, until now, the natural course of falls in patients after the first fall is unclear, therefore one may hypothesize that a reduction in number of falls seems more obvious than an increase due to a possible ceiling effect. A controlled trial is needed to further elucidate the relation we observed in this pilot study. Of course there are other possible explanations for a reduction of fall frequency, e.g. attention to patients keeps them busy and prevents walking on their own and exhausting activities may lead to fatigue and sedentary pursuits during the rest of the day. In addition, the absence of a relation between attendance frequency, endurance and fall incidents is puzzling and needs further investigation.
Interestingly, the execution of this study, which was time consuming, appeared relatively simple; within 6 months the study grew from idea to implementation. The fact that the NHs are used to work together in an academic network (11) and moreover the enthusiasm of the physiotherapists who guided the groups might be explanations for this easy way of performing research.
Conclusion
Our before-after study suggests that a moderately intensive exercise program may be associated with a significant reduction of falls and an increase of endurance in frequently falling NH residents. A randomized controlled trial is needed to further support and elucidate these findings.
Conflict of interest: None of the authors has conflicts of interest.
Acknowledgement: We gratefully acknowledge all physiotherapists and coworkers in the NHs who helped executing the intervention and the measurements.
Ethical standards: Intervention and meausrements are usual care. Measurements were collected anonymously. Therewith no extra ethical deliberation is necessary.
References
1. Bossers WJ, van der Woude LH, Boersma F, et al. Recommended measures for the assessment of cognitive and physical performance in older patients with dementia: a systematic review. Dement Geriatr Cogn Dis. Extra 2012 Jan;2(1):589-609.
2. Vance J. The clinical practice guideline for falls and fall risk. Translat Behav Med. 2012;2:241–243.
3. El-Khoury F, Cassou B, Charles MA, et al. The effect of fall prevention exercise programmes on fall induced injuries in community dwelling older adults: systematic review and meta-analysis of randomised controlled trials. Brit Med J. 2013;29:347:f6234.
4. Neyens JC, Dijcks BP, Twisk J, et al. A multifactorial intervention for the prevention of falls in psychogeriatric nursing home patients, a randomised controlled trial (RCT). Age Ageing 2009;38(2):194-9.
5. Cameron ID, Gillespie LD, Robertson MC, et al. Interventions in preventing falls in older people in care facilities and hospitals (Review) Cochrane Database Syst Rev. 2012 Dec 12;12:CD005465.
6. Bunn F, Dickinson A, Simpson C, et al. Preventing falls among older people with mental health problems: a systematic review. BMC Nurs. 2014;13:4.
7. Van Hanegem E, Enkelaar L, Smulders E, et al. Obstacle course training can improve mobility and prevent falls in people with intellectual disabilities. J Intellect Disabil Res. 2014 May;58(5):485-92.
8. Becker C, Kron M, Lindemann U, et al. Effectiveness of a multifaceted intervention on falls in nursing home residents. J Am Geriatr Soc. 2003;51:306–13.
9. Jensen J, Lundin-Olsson L, Nyberg L, et al. Fall and injury prevention in older people living in residential care facilities. Ann Intern Med. 2002;136:733–41.
10. Ray WA, Taylor JA, Meador KG, et al. A randomised trial of a consultation service to reduce falls in nursing homes. JAMA. 1997;278:557–62.
11. Koopmans RT, Lavrijsen JC, Hoek F. Concrete Steps Toward Academic Medicine in Long Term Care. J Am Med Dir Assoc. 14 (2013) 781e783