C.H. Lee1, V. Gruss1, M. Stuercke2, C.J. Ryan1
1. University of Illinois at Chicago College of Nursing, 845 S. Damen Ave., MC 802, Chicago, IL, USA; 2. Glen Health and Home Management, Chicago, IL, USA. Corresponding author: Curie H. Lee, DNP, AGNP, RN, Department of Biobehavioral Health Science, UIC College of Nursing (MC 802), 845 South Damen Avenue, Chicago IL 60612, (312) 996-9183, FAX: (312) 996-4979, clee217@uic.edu
Jour Nursing Home Res 2016;2:104-109
Published online October 21, 2016, http://dx.doi.org/10.14283/jnhrs.2016.16
Abstract
Background: Hospital readmissions in nursing home populations are rising every year. Little is known of how to prevent such hospital readmissions. The study’s purpose was to explore the relation of communication on 30-day readmission rates via the Stop and Watch (SW) Tool with Certified Nursing Assistants (CNAs) in the Interventions to Reduce Acute Care Transfers (INTERACT) program: a program implemented in skilled nursing facilities (SNFs). Objectives: The objectives were: describe the relation of the INTERACT SW Tool Use among admission/readmission patients and correlate outcomes on 30-day hospital readmission rates. Design: Quality improvement project. Setting: 234-bed skilled nursing facility in a large Chicago urban area in the United States; 3-unit facility with 91% occupancy. Participants: Licensed/registered nurses (N = 11) and CNAs (N = 21) on SNF unit with 80 residents. Intervention: INTERACT protocol, including identification of admission patients; CNAs’ daily monitoring of admission/readmission patients using the SW Tool; and licensed nurses’ review of SW Tool daily reports and follow-ups. Measurements: SW Tool use from each day, evening, and night shift; number of transfers to hospitals for readmission; and communication between CNAs and licensed nurses measured as SW Tool leading to a Situation, Background, Assessment, and Recommendation (SBAR) communication form. Results: For the four-month study period, 30-day readmission rates in the study unit decreased to 34% from over 50% at baseline. Readmission rates were associated with consistent SW Tool use (p = .007, Pearson Correlation = -0.304). Conclusions: 30-day transfer rates are reduced by CNAs’ consistent use of the SW Tool.
Key words: Communication, 30 day-hospital readmissions, Stop and Watch Tool, skilled nursing facility, INTERACT program.
Introduction
Hospital readmissions in nursing home populations are rising every year (1,2). Little is known on how to prevent such hospital readmissions (3). One Medicare patient in five is discharged from hospital to skilled nursing facilities (SNFs), and the number of patients in SNFs continues to rise every year (4). The rates of readmissions in the 30-day period after discharge from a SNF increased slightly in 2014, and SNF care cost was $28.6 billion (5). In 2013, $280 million of 30-day readmission reimbursements to hospitals went unpaid, especially for the readmission diagnoses myocardial infarction, heart failure, and pneumonia. Today, more diagnoses are included under conditions that are not reimbursed since the 2010 Affordable Care Act. Readmission penalties are increasing and reached $400 million in 2015 (6). The Centers for Medicare and Medicaid (CMS) see performance improvement projects in SNFs as a top priority (7). In response, SNFs are looking for more efficient care models that can reduce high costs: in particular, 30-day readmissions due to emergency room visits or hospital transfers (8).
In an attempt to reduce hospital readmission rates, the Interventions to Reduce Acute Care Transfers (INTERACT) program was implemented in SNFs. The INTERACT program provides nursing staff with tools and strategies to reduce hospital readmission rates. INTERACT is a quality improvement program used to identify, assess, and manage acute resident changes, thereby reducing readmission rates (9). In previous studies, the use of INTERACT was associated with a decrease in readmissions ranging from 7%-50% (10-14). INTERACT program tools such as the Stop and Watch Tool (SW; Fig. 1) are designed to alert nurses, unit managers, nurse practitioners, and medical doctors of changes in SNF residents’ status and potential hospital readmission as reported by supportive nursing staff, such as CNAs using the SW Tool (9).

Figure1 Data Analysis and STOP AND WATCH (SW) acronyms (http://www.monarchriskmanagement.com/wp-content/uploads/2014/04/StopandWatch.jpg)
INTERACT Program
Since 2013, the SW Tool has been used by Certified Nursing Assistants (CNAs; frontline direct-care workers) at the study unit to identify acute changes and communicate those changes to licensed nurses, who then assess the patient and report changes to medical providers. However, SNF in this study did not fully understand the impact of this tool on 30-day transfer rates because the facility did not review data or follow up on the use of the SW Tool among their CNAs. The SNF quality improvement project sought to meet the demand for (1) the culture of accountability for CNAs by using the SW Tool and (2) the need for data and metrics to monitor progress after implementing the INTERACT program. Therefore, this study focused on the relationship between CNAs using the SW Tool and transfer rates back to a hospital for readmission. Because CNAs provide nearly 90% of daily care in SNFs (13), they are uniquely positioned to identify early signs or symptoms of a resident’s declining status (15).
Based on the SW Tool, when SNF patients require further assessment, INTERACT provides a Situation, Background, Assessment, and Recommendation (SBAR) communication form and progress note to be used by licensed nurses. This tool also helps licensed nurses to organize necessary information before calling medical providers. Without the SW Tool, there is a chance of misreporting changes in a resident’s condition in a SNF. Timely communication of critical information, such as that facilitated by the SW Tool, fosters team work, mutual professional understanding, and respect (14). However, in the facility in this study, the SW Tool often was not used consistently, leading to a lack of data-driven information about its effectiveness. Licensed nurses typically waited for CNAs to voluntarily report resident status changes before conducting an assessment. CNAs were unsure of the value of the SW Tool and its intended benefits; therefore, the SW Tool had been inconsistently used by CNAs. The facility readmission rate was nearly 50% in the baseline period in 2013.
As a Quality Improvement (QI) project, there was a need for evaluation of CNAs’ utilization of the SW Tool in regards to timely management and impact on hospital transfer rates for readmission. The objectives were (a) describe the effects of the INTERACT SW Tool among admission patients and (b) correlate outcomes of using the SW Tool with 30-day transfer rates for hospital readmission.
Methods
Setting
The study setting was a SNF in a large Midwestern urban area in the United States, composed of mostly lower socioeconomic status communities. According to citydata.com, median household income was $28,235 per year, and the unemployed percentage was above state average.
The 234-bed SNF provides short- and long-term care to residents. It has three units, averaging 91% occupancy. The one skilled nursing unit, with 80 beds, was selected for this study. The resident patient population (N = 80) included new and readmitted Medicare/Medicaid and long-/short-term stay residents on the skilled study nursing unit. Patient population in this setting was composed of 97% African-Americans: 56% male whose average age was 61 years, and 44% female whose average was 65 years.
The University of Illinois at Chicago Internal Review Board (IRB) approved a Claim of Exemption (#2015-0280). The study facility granted permission to review de-identified data.
Sample
The study sample consisted of nursing staff that had been working in the skilled nursing unit (N = 32), including licensed registered and practical nurses (n = 11) and CNAs (n = 21). The skilled nursing unit was included for the study because most admissions, readmissions, and discharge patients were in this study unit. All CNAs and licensed nurses (regardless of their educational level) were educated about the new protocol for use of the SW Tool between July and November 2014.
Instruments
The instrument used was the SW Tool (Figure 1).
Approach: Review of the Stop and Watch Tool
Since January 2013, the INTERACT program (including the SW Tool) has been adopted but inconsistently implemented on the study unit. CNAs were educated by nursing administrators, especially the assistant nursing director, who was a champion of the INTERACT program implementation. After a year and half, the Quality Improvement Committee discussed redesign of the INTERACT program because facility readmission rates were nearly 50%.
This project implemented a revised INTERACT protocol, including (1) identification of admission/readmission patients and (2) daily monitoring of use of the SW Tool. During the project, CNAs were encouraged to communicate any resident status changes to licensed nurses, who then assessed the resident and reported changes to medical providers.
Admission patients included all new and readmitted hospital discharged residents. The list of identified admission patients who needed SW Tool monitoring was placed in front of the nursing station on the CNAs’ assignment sheet and on the nurses’ medication cart before 10 a.m. daily. The SW Tool monitoring program was completed on all three shifts, including weekends.
For this project, QI facilitators obtained buy-in from key stakeholders and performed need-based assessment. They chose the one metric SW Tool process to monitor progress, incorporating standard CNAs’ care principles into existing flow of daily work.
Procedure
1. Admission patients were monitored daily (all shifts) by CNAs using the SW Tool (in file card form) for a mandatory 30 days.
2. The CNAs reported each admission patient’s condition using the SW Tool.
3. If no changes were noted, CNAs wrote «no change» on the SW Tool file card.
4. The documented file card (SW Tool) was submitted to nurses for signature.
5. Upon receiving a signature from the licensed nurses, communication was completed about admission patients’ condition.
6. Whenever a change was reported, the licensed nurses would assess the admission patients’ condition for follow-up care and report changes to the medical provider using the SBAR tool.
7. The process time of using the SW Tool was less than 5 minutes, and it was completed during or by the end of each shift.
Education
1. An education session was held at each monthly CNA staff meeting, with information on how to identify changes in residents’ condition.
2. Weekly in-service meetings continued with the Assistant Nursing Director and all unit managers, with reminders about daily utilization of the SW Tool by CNAs.
3. Daily stand-up meetings were held within the unit, with the Assistant Nursing Director, unit managers, all nurses, and CNAs on duty discussing any status changes among admission/readmission patients.
4. This daily meeting also became a reminder for CNAs to consistently use the SW Tool among the admission patients.
Data Collection
From July to November 2014, the study unit data were examined on admission patients and CNA SW Tool use.
Among the 80 patients, their payers were Medicare (14%), Medicaid (63%), and private insurance (23%). Their diagnoses included heart failure, acute myocardial infarction, and stroke (24%); infection (19%); respiratory problems (11%); end-stage renal disease/hemodialysis (10%); and hip and knee problems and diabetic problems (36%). To determine the relation of using the SW Tool with 30-day transfer rates for hospital readmission, the monthly status of listed patients was monitored as follows.
1) The total numbers of SW Tool (file card form) use from each day, evening, and night shift were retrieved and tallied each month (Table 1).
2) SW Tool use levels were divided into three categories by the total numbers of monthly SW Tool use between minimum = 0 and maximum = 90 (30 days x 3 shifts).
3) The total use of SW Tool levels (defined as “SW-Yes”) were graded as follows: less than or equal to 4 times = 0, 5 to 9 times = 1, and 10 times or more = 2.
4) For the main outcome evaluation (i.e., the number of transfers within 30 days), data were classified into three transfer status groups: no transfer = 0; planned transfer = 1, and unplanned transfer = 2.
5) Variables for analyses of the relation with 30-day transfer rates were as follows: (a) Total numbers of SW Tool use among the listed admission patients versus number of 30-day patient transfers; (b) “SW-YES” as numbers of SW Tool reports per each patient per shift (day, evening, and night) versus number of 30-day patient transfers; c) “SW–SBAR,” which was used as a measure of communication level and measured in each shift’s SW Tool record status, versus number of 30-day patient transfers; and d) If all shifts were recorded, communication level = 1; if any shift was marked «0,» this status was measured as no direct communication. It was also interpreted as follow-up care if a note or SBAR was made by licensed or registered nurses after receiving a CNA’s SW Tool file card notification.
Completion of the SW Tool demonstrated communication from CNAs to licensed nurses of clinical alerts to determine the necessity of further evaluation by the nurse (14).
Data Analysis
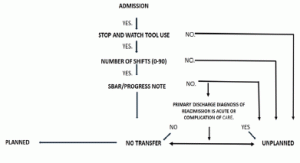
Data were analyzed for differences in 30-day readmissions before and after implementation of the new protocol and education of SW Tool use. De-identified demographic data were obtained for the study period. Data analysis was conducted as shown (Fig. 2), with three outcome measures: (1) total number of SW Tool uses by CNAs for day, evening, and night shifts for 30 days; (2) SW Tool use frequency relationship to 30-day transfer rates; and (3) SW Tool communication frequency (defined as “SW-SBAR”) relationship to 30-day transfers. Statistics included descriptive statistics, correlations with bivariate tests, independent samples t tests, and Monte Carlo Exact Chi-square tests. SPSS was used (Version 22, Chicago IL). The overall main outcome of interest was the relation of SW Tool use to 30-day transfer rates (Fig. 3). Because Fisher’s exact test only works for a 2 x 2 table, we used Monte Carlo Exact Chi-square tests in SPSS.
Results
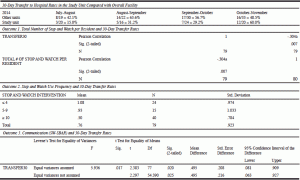
Correlation test results showed significant association between the two independent variables: 30-day hospital transfers and total number of SW Tool uses per resident (p = 0.007, Pearson Correlation = -0.304). This can be interpreted as a prediction: for every 1% increase in CNAs SW Tool use, 30-day transfers were reduced 0.3% (Table 2, Outcome 1). If Stop and Watch Tool utilization is increased by 10 times, within a 30-day period, hospital readmission rates will decrease by 3%. We have calculated NNT = 1/ ARR =1/ (34%-50%) =6.
The relation of the SW Tool to 30-day transfers was proportional as numbers increased. (i.e., if CNAs used the SW Tool more than 10 times in 30 days for the monitored patients, transfers decreased; Table 2, Outcome 2).
Direct communication (i.e., SW Tool file card submission with licensed nurses’ signature) was shown to be associated with reduction in 30-day transfer rates twice as much (Mean = .057) as no direct communication (Mean = 1.07; Table 2). It was also associated with a reduction in 30-day transfers (t = 2.297, p = .025; Table 2, Outcome 3).
The facility 30-day transfer rates were compared with the study unit for four months (Table 2). The study unit showed a nearly 30% lower 30-day readmission rate than the overall facility, except for the months of October and November 2014. In November, an exceptional month, an increased readmission rate was speculated, which may be related to confounding factors, such as seasonal influences; changes in weather and flu season. These seasonal influences frequently caused respiratory infections such as pneumonia. Readmission/admission rates also varied during end-of-the-year holidays. Overall, changes in SW Tool use were associated with changes in 30-day transfer rates.
Correlation is significant at the 0.01 level (2-tailed).
Discussion
This study examined the results of a retrospective data analysis in one unit of a SNF. Among the study months of July through November, September (p = .008) and October (p = .001) showed clear associations between SW Tool use and 30-day transfers. Compared to no use (SW-YES score = 0), SW Tool use (SW-Yes = 1 or 2) was associated with an increase in non-transfers (transfer score = 0). This implies that 30-day hospital readmission rates can be reduced by using the SW Tool. Another result of this project was improved knowledge among CNAs as demonstrated by adopting appropriate use of the SW Tool and participating in daily meetings on each shift.
As noted, this is the first study after the implementation of the INTERACT program in the study SNF in compliance with the Quality Assurance & Performance Improvement (QAPI) recommendations from CMS. Consistent use was not enforced because there was concern that using the SW Tool might be an additional burden to CNAs. This could be a barrier to implementing a new SW Tool protocol. However, scrutiny of readmission rates may instill a sense of urgency to implement a process change: there is certainly a desire to provide quality care. SNFs have always been highly regulated but not always well-staffed. It is key to incorporate the SW Tool practice into existing SNF work flow by assigning responsible CNAs to ensure accountability.
The study provided important evidence of the SW Tool’s role in aiding efforts to reduce transfer rates. Through this study, the QI project team learned several lessons: (1) CNAs’ participation in using the SW Tool had a strong correlation to 30-day transfers to hospitals; (2) timely communication related to patient care was associated with a reduction in 30-day hospital transfer rates when staff implemented the SW Tool correctly.
It can be concluded that increased frequency of SW Tool use is related to lower transfer rates—if CNAs use it more than 10 times among the residents who are at risk of readmissions in 30 days. Findings indicate that consistent use of the SW Tool is required for positive outcomes.
Licensed nurses are mainly occupied with daily tasks such as medication and computer charting. It is difficult to notice changes in residents’ condition in a timely manner; CNAs’ observations and reporting through SW Tool utilization could prevent episodes of missing reports of patient conditions during or at the end of the shift. Timely reporting in turn can produce increased timely care and reduced transfer rates in SNFs. Communication of changes in residents’ condition without missing reports promoted teamwork among nurses in the SNF environment. Continuous education and reinforcement is essential while using the SW Tool among CNAs on every shift.
In general, CNAs’ daily practice has not been recognized despite their workload. Through SW Tool use, their work was recognized and valued. It is noteworthy that CNAs were willing to record residents’ complaints or unusual behaviors that were not itemized on the SW Tool file card. This indicates CNAs’ enthusiasm and genuine concern of health care practice. Also, in this study unit, SW Tool file cards became a basis of discussion regarding care plans during shift stand-up meetings with multidisciplinary team members. Presenting monthly unit results of SW Tool use to CNAs, who are the direct care providers, could be empowering. Empowerment creates an encouraging work environment and culture among CNAs, nurses, and residents, resulting in positive outcomes (16).
There are several limitations with this retrospective data analysis of a pilot study. The small sample size may hinder generalizability. A larger sample size may show stronger associations between SW Tool use and 30-day transfers. It was difficult using aggregated data retrospectively to follow up and distinguish correctly between admission diagnosis and transfer diagnosis for the planned or unplanned readmission to hospitals. There was no real-time staff survey among CNAs and nurses who participated during the analyzed period for further evaluation of the project effects.
Conclusion
Quality improvement projects are important for improving both care-givers’ performance and patient outcomes in SNFs. This study demonstrated encouraging results for implementing consistent use of the SW Tool, which could result in significant cost-saving, improve resident quality of life, decrease hospital transfers, and enhance person-centered care. It is imperative to develop a team approach to decrease hospital readmissions by increasing timely communication of patients’ changes in condition in SNFs. In the study unit, quality was influenced more often by the system-process than the individual players. Adoption of new tools or programs is challenging. Solutions were found through interaction and communication among SNF staff. When direct communication was achieved between CNAs and licensed nurses, transfer status decreased overall by nearly half. Hospital readmission is risky and costly to nursing home residents. Prevention of unnecessary hospital transfer (readmission) is beneficial to SNF residents because it reduces potentially negative physical, emotional, and psychological effects from hospital complications and infections (17). Prevention of readmissions also improves the quality of care and processes and reduces health care system costs (2, 17, 18).
Acknowledgments: The authors thank Kevin Grandfield, Publication Manager, for editorial assistance and Chang G. Park, PhD, Senior Biostatistician/Assistant Research Professor for data review at the University of Illinois College of Nursing Department of Biobehavioral Health Science.
Conflicts of interest: There are no conflicts of interest include academic, personal, or political relationships; employment; consultancies or honoraria; and financial connections and funding related to this project or manuscript..
Ethical standards: The content of this paper represents original work/opinion that verifies the accuracy of the content.
References
1. Grabowski DC, O’Malley AJ, Barhydt NR. The costs and potential savings associated with nursing home hospitalizations. Health Aff (Millwood). 2007; 26(6):1753-1761.
2. Walsh E, Freiman M, Haber S, Bragg A, Ouslander J, Wiener J. Cost drivers for dually eligible beneficiaries: Potentially avoidable hospitalizations from nursing facility, skilled nursing facility, and home and community-based services waiver programs. 2010; http://www.cms.gov/Research-Statistics-Data-and-Systems/Statistics-Trends-and-Reports/Reports/downloads/costdriverstask2.pdf.
3. Graverholt B, Forsetlund L, Jamtvedt G. Reducing hospital admissions from nursing homes: A systematic review. BMC Health Serv Res. 2014; 14:36.
4. Krumholz HM, Nuti SV, Downing NS, Normand SL, Wang Y. Mortality, hospitalizations, and expenditures for the Medicare population aged 65 years or older, 1999-2013. JAMA. 2015; 314(4):355-365.
5. Medicare Payment Advisory Commission. Skilled nursing facility services. Report to the congress. Washington, DC: MedPAC; 2016.
6. Rau J. Medicare to penalize 2,217 hospitals for excess readmissions. Kaiser Health News. August 13, 2012.
7. Centers for Medicare & Medicaid Services. QAPI five elements. 2014; http://www.cms.gov/Medicare/Provider-Enrollment-and-Certification/QAPI/nhqapi.html. Accessed May 1, 2015.
8. Holahan J, Schoen, C., McMorrow, S. The potential savings from enhanced chronic care management policies. 2011; http://www.urban.org/uploadedpdf/412453-The-Potential-Savings-from-Enhanced-Chronic-Care-Management-Policies-Brief.pdf. Accessed June 4, 2015.
9. INTERACT. Interact T.E.A.M. n.d.; http://interactteam.org/ Accessed May 1, 2015.
10. Ouslander JG, Lamb G, Tappen R, et al. Interventions to reduce hospitalizations from nursing homes: Evaluation of the INTERACT II collaborative quality improvement project. J Am Geriatr Soc. 2011; 59(4):745-753.
11. Tena-Nelson R, Santos K, Weingast E, Amrhein S, Ouslander J, Boockvar K. Reducing potentially preventable hospital transfers: Results from a thirty nursing home collaborative. J Am Med Dir Assoc. 2012; 13(7):651-656.
12. Ouslander JG, Perloe M, Givens JH, Kluge L, Rutland T, Lamb G. Reducing potentially avoidable hospitalizations of nursing home residents: Results of a pilot quality improvement project. J Am Med Dir Assoc. 2009; 10(9):644-652.
13. Galloro V. Staffing outlook grim. High turnover expected to continue in skilled nursing, assisted living. Mod Healthc. 2001; 31(8):64.
14. Ouslander JG, Bonner A, Herndon L, Shutes J. The interventions to reduce acute care transfers (interact) quality improvement program: An overview for medical directors and primary care clinicians in long term care. J Am Med Dir Assoc. 2014; 15(3):162-170.
15. Pfefferle SG, Weinberg DB. Certified nurse assistants making meaning of direct care. Qual Health Res. 2008; 18(7):952-961.
16. Gruss V, McCann, JJ, Edelman, P, Farran, CJ. Job stress among nursing home certified nursing assistants: Comparison of empowered and none empowered work environments. Alzheimers Care Q. 2004;5(3):207–216.
17. American Health Care Association. Hospital readmissions. n.d.; http://www.ahcancal.org/quality_improvement/qualityinitiative/Pages/Hospital-Readmissions.aspx. Accessed June 4, 2015.
18. Jencks SF, Williams MV, Coleman EA. Rehospitalizations among patients in the Medicare fee-for-service program. N Eng J Med. 2009; 360(14):1418-1428.