K.L. Lapane1, C.E. Dubé1, B.M. Jesdale1
1. University of Massachusetts Medical School, Worcester, MA, USA. Corresponding author: Kate L. Lapane, PhD MS, Associate Dean, Clinical and Population Health Research, Professor– Department of Quantitative Health Sciences, University of Massachusetts Medical School, 55 Lake Avenue North, Worcester, MA 01655, Phone: 508-856-8965, Fax: (508) 856-8993, email: Kate.Lapane@umassmed.edu
Jour Nursing Home Res 2016;2:110-117
Published online October 28, 2016, http://dx.doi.org/10.14283/jnhrs.2016.17
Abstract
In 2012, nursing homes were considered the most dangerous workplaces in the United States. While other industries have guidelines that limit manual lifting of stable objects to ≤50 pounds, the same is not so in the nursing home industry where residents requiring physical assistance may weigh over 250 pounds and where the prevalence of obesity among residents is increasing. Safe patient handling legislation in nursing homes has been enacted in nine of the United States since 2005 (Hawaii, Illinois, Maryland, Minnesota, New Jersey, New York, Ohio, Rhode Island, and Texas). This paper reviews the problem of worker injuries in nursing homes, describes the legislation passed to address the problem, and reviews the data available on the effectiveness of the legislation. No national studies evaluating the effectiveness of safe patient handling state policies on nursing home injuries exists, although the National Institute on Occupational Safety and Health has recently funded a national evaluation.
Key words: Nursing homes, worker injuries, safe patient handling, legislation.
Introduction
Nursing homes have one of the highest occupational illness and injury rates in the United States (higher than coal mines, steel and paper mills, warehousing and trucking) (1). From 1984 to1995, the reported injury rate for workers in the nursing home sector increased by 57 percent (2); this has been trending downward in recent years (3). Although the reasons for the downward trend remain unknown, it may be directly or indirectly affected by trends in improved quality in nursing homes (4), improved staffing levels (5), reduced staffing turnover (6), disincentives to report worker injuries because of job insecurity (7, 8) and interventions specifically aimed at reducing worker injuries in nursing homes (9). In 2014, nursing homes were deemed to be among the most dangerous workplaces in the United States according to the Bureau of Labor Statistics, with a rate of 7.1 recordable cases per 100 FTEs.3 Heavy manual handling is a key risk factor for work-related musculoskeletal disorders of the back, neck, and upper extremities and nursing homes rank among the top five industries for compensable injuries and disorders of this type. Nursing homes rank highest for sprains, strains, and tears (10) and back injuries (11).
Many back injuries are considered preventable by means including improved job design (12). Despite this, the cost of back injuries in the American health care industry exceeds $7 billion annually which represents an estimated 5%-15% of the total cost of back injuries across all occupations (13). Nursing assistants have among the highest rates of sprains, strains, and tears of all occupations in the United States (14). This comes as no surprise when the realities of the nursing home context are considered. In most industries, guideline-concordant manual lifting of stable objects is limited to 50 pounds or less (15). Nursing home residents—who may move or shift unexpectedly, have pain or wounds, be precariously attached to equipment or tubing, or who may even actively resist efforts to assist them—may weigh 250 pounds or more with those weighing 100 pounds considered “light” (13). In a typical 8-hour workday, a nurse may manually lift an estimated cumulative weight of 1.8 tons (17). Further compounding this problem is the ongoing American obesity epidemic. In 2011-2012, 34.9% of adults in the United States were obese (18). The nursing home industry has not been immune to this epidemic (19), and the increasing trend in the prevalence of obesity is unlikely to reverse in the foreseeable future (20).
This article reviews information regarding worker injuries in nursing home settings, shining a spotlight on a serious issue in the nursing home sector. We review the issues that make the problem of worker injuries particularly challenging in the nursing home sector. Briefly, we conducted a literature search in PubMed using combinations of words for each of the major headings covered in the manuscript. We restricted the search to include only papers published in English. We also reviewed the reference lists of articles identified through the PubMed search to see if there were additional references germane to the topics included in the review. We also consider the special circumstances of workers who are at particular risk for injury in the nursing home setting. The impact of staff turnover on the problem of worker safety in this setting is considered, and we then provide a review of potential solutions to the problem with a focus on safe patient handling legislation. We also review what little has been reported on the effectiveness of the legislative solution and conclude with a summary of ongoing evaluations of the legislative approaches to reducing worker injuries in nursing homes.
Significance of worker injuries in the nursing home setting
Currently, 1.4 million people reside in nursing homes (21), with ~1.3 million staff providing direct skilled nursing and nursing-related care. Nursing home direct care staff members include registered nurses (RNs), licensed practical nurses (LPNs), licensed vocational nurses (LVNs), certified nursing assistants (CNAs), and nurses aides-in-training (22). Nursing homes employ ~8% of RNs and one-third of LPN and LVNs nationwide (23). More than half of nursing home nursing staff are CNAs (24), who are responsible for helping frail and disabled older adults carry out the most basic activities of daily life. Nationally, CNAs have a rate of musculoskeletal injuries (197.3 per 10,000 FTEs) over five times as high as the national average (35.4 per 10,000 FTEs) (1, 10).
Caring for nursing home residents is challenging. About half of all residents are unable to independently transfer (e.g., from bed to chair) or require total or extensive assistance (25) and residents often move unexpectedly (13). Types of resident handling that may result in worker injury include manual lifting, repositioning in bed, catching patients when they fall, transporting from one location to another, and providing assistance for toileting, etc (20, 26).
As previously mentioned, nursing homes are dangerous places to work (3). Forty-four percent of such injuries are due to lifting, with extensive worker’s compensation and medical treatment costs (27). More than half of nursing assistant injuries are due to overexertion (28). Even with two staff members manually handling a patient, substantial risk of injury exists (22). Recurring injuries due to repeated lifting can result in scarring and cumulative damage (3). Risk factors for injury include 1) force required; 2) repetition and frequency; and 3) awkward postures that place stress on the body (29, 30).
When the realities of the nursing home context are considered, the risk to caregivers should come as no surprise. The prevalence of nursing home resident obesity has more than doubled in the past 20 years (15), and in 2008 it was estimated that ~25% of all residents were obese (31). Work factors (e.g., working the night shift) have also been linked to increased risk of low back pain-related sick leave among CNAs (22) and with variation in safe patient handling implementation (33). Adverse nursing work schedules have been linked to musculoskeletal problems (34). The importance of injury risk among nursing home workers is highlighted by the Occupational Safety and Health Administration recent directive targeting “ergonomic stressors in patient lifting” as an important hazard to worker safety (35).
Marginalized populations working in nursing homes
When we consider who is at risk for injury in this setting it is clear that they are largely vulnerable. Nursing staff in nursing homes are disproportionately women (>90%) (36). Compared to men, women may be more susceptible to back injuries with lower load exposures (37). On average, women are smaller in stature and have lower body mass. Differences in both innate strength and altered body positioning in response to heavier loads have potential to cause more harm to women than men under similar circumstances (38, 39). While the majority of RNs and LPN/LVNs are non-Hispanic white (88% and 78%, respectively), nearly half of CNAs are racial minorities (38.7% black, 7.9% other), almost 10% are Hispanic, and 20% are immigrants (31). More than three-quarters of CNAs have a high school education or less (31). Federal law requires that state-approved CNA training programs include a minimum of only 75 hours of instruction, with almost half of states requiring the minimum and about one third of states requiring over 100 hours. Missouri requires the most training at 175 hours (40). CNAs make little more than the minimum wage (41) with nearly three-quarters of CNAs reporting household incomes less than $30,000, almost half with a history of receiving public assistance like food stamps, and 16.5% having lacked health insurance (23). Low wages and inadequate benefits may well contribute to the high rate of turnover among nursing home CNAs (20, 34). Compounding the risk to these vulnerable workers is a workers’ compensation system where benefits have been slashed over recent years in 33 states in the United States, reducing benefits, creating new hurdles to obtaining medical care, or making it more difficult to qualify for benefits. Indeed, the Occupational Safety and Health Administration of the United States Department of Labor has characterized the workers’ compensation system as “broken”, with employers now supporting only about 20% of the cost of workplace injuries through workers’ compensation. This forces injured workers, their families, and taxpayers to subsidize the vast majority of lost income and medical care costs (42). This has occurred despite the fact that employers are paying the lowest rates for workers’ compensation insurance than at any time in the past 35 years and insurers’ profits in 2013 are the highest they had been in over 10 years (43). At the same time, injured workers have limited options for recourse as, under current worker compensation laws, workers who suffer preventable, disabling, work-related injuries have are prohibited from suing their employers for lack of lift equipment even if this has led to their disability (10, 36).
Staff turnover exacerbates the problem of worker injuries
In the nursing home setting, staff turnover is high. Thirty-eight percent of nursing home staff report intentions to leave their position within 2 years (44). The instability of the nursing home workforce often contributes to extreme workloads, insufficient training, and high accident and injury rates (45-47). Efforts to reduce staff turnover in nursing homes may indeed improve worker safety as new staff are particularly vulnerable to accidents during their initial period of employment (48). Making matters worse, worker injury also contributes to the well-documented staff shortage (49). This results in a vicious cycle as staff shortages result in overworked staff which in turn leads to higher injury rates which results in increasing staff turnover and shortages (50).
Potential solutions to reduce injuries
Many back injuries are considered preventable by improved job design. In the health care sector, use of mechanical lift equipment is effective in back injury prevention (1, 29). The National Institute for Occupational Safety and Health National Occupational Research Agenda (51) and the American Nurses Association (52) have identified models of care to address unsafe practices in healthcare settings. These effective solutions do involve a financial cost to the institution. Purchase of equipment such as portable lifts and transfer sheets, staff training, adopting a “minimal lift” policy to eliminate manual lifting, and establishing “lift teams” with proper training and equipment to rotate around the facility all require potentially significant initial investment (53). However, it is estimated that costs related to these improvements can be recovered in less than 5 years (49) as a result of reduced workers’ compensation costs (54), reduced staff injury costs (55), and reduction in costs related to patient pressure ulcers (56). Further savings are realized in reducing turnover as hiring and training costs for replacement staff has been estimated ~$92,442 per nurse in 2000 (57).
There is no federal legislation specifically regarding safe patient handling and mobility, although federal legislators introduced a bill in each session since 2009 (58). The most recent bill has been referred to the Subcommittee on Health where it currently remains (59). The United States lags behind other industrialized nations where manual lifting of patients is prohibited, including in Canada, England, the Netherlands, Switzerland, Ireland, Finland, and Australia (60).
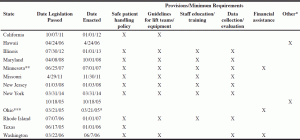
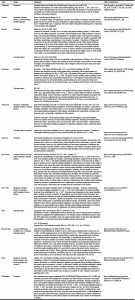
Table 1 summarizes enacted safe patient handling legislation at the state level. Twelve states have passed legislation related to safe patient handling, of which 9 states explicitly include nursing homes. In three states (California, Missouri, Washington), substantial numbers of nursing homes implemented safe patient handling programs. At the state level, nursing home-specific safe patient handling legislation varies in scope and strength. Six states (Illinois, Maryland, Minnesota, New Jersey, New York, and Rhode Island) require nursing homes to have comprehensive programs that implement safe patient handling policies that include guidelines for securing appropriate equipment and training, data collection, and evaluation. Ohio provided interest-free loans to nursing homes wishing to install lift equipment (61), although this was repealed in June of 2015. New York provided funding to select health care facilities enrolled in its two-year safe patient handling demonstration program (62), and the 2014-15 New York state budget included a provision requiring general hospitals and other health care facilities to establish facility-specific safe patient handling programs by January 1, 2017 (63). Hawaii passed legislation that adopted a resolution supporting the American Nurses Association’s Handle With Care® campaign, but with no regulatory requirements (63, 64). Table 2 shows detailed summaries of the legislation and links to the actual legislation.
Shaded states explicitly extend legislation to nursing homes. *Includes demonstration projects and resolutions; ** Revised 2015 *** Repealed 6/30/15
Effectiveness of safe patient handling legislation
Although safe patient handling legislation has been in effect since 2005, publicly-available evaluations of its impact on healthcare worker injuries are scarce. Evaluations of staff injuries by state agencies or legislative committees in Ohio and New York show promising results. In Ohio, nursing homes with state funding to install ergonomic interventions saw a 37% decrease in the incidence rate of cumulative trauma disorders among workers, a 39% decrease in days lost due to injury, and a 26% decrease in restricted days due to injury (65), although they did not examine these trends relative to facilities that did not get grant funding. Evaluation of the impact of legislation in New York focused on five case studies demonstrating a dramatic reduction in lost work days due to patient handling injuries in these selected facilities (66). Despite the fact that six of the nine states’ legislation targeting nursing home workers called for data collection and evaluation, we were unable to identify any other reports evaluating the impact of these legislative acts.
In Washington state an evaluation of workers in acute care hospitals found that from 2007-2009, compared to Idaho (a state where no safe patient handling legislation existed), Washington acute care hospital workers reported a higher proportion of reported routine use of lift and other safe patient handling equipment. In fact, the proportion reporting equipment use in Idaho decreased over the same period (p< .009) (67). However, the declining trend in compensable injury rates in this sector was indistinguishable from the declining rate across all industrial sectors.
An analysis by Public Citizen found dramatic declines in the number of health care and social assistance workers reporting musculoskeletal injuries resulting in days away from work in many, but not all, states with safe patient handling legislation (68). This analysis grouped workers in nursing homes and hospitals with a large number of other health care and social services workers together, and did not account for changes in the number of workers in the sector over time.
The relation between nursing home organizational factors and worker injuries has been studied. Organizational characteristics of the nursing homes—including staffing, training, equipment availability, and organization of work—can affect work load (69). Other nursing home characteristics associated with higher reports of staff injury rates include not-for-profit status, belonging to a chain, higher average occupancy, more RNs, and lower quality of care (70). It is unlikely that legislation would be equally effective for all nursing homes as the variability in organizational characteristics of individual nursing homes is likely to substantially modify legislation effects (71). Understanding the profile of nursing homes which require interventions beyond legislative initiatives to improve worker safety is important.
Conclusion
Safe patient handling legislation is one approach to reduce worker injuries in the health care sector. Nine states have passed legislation related to safe patient handling in nursing homes since 2005, with two states currently considering legislative initiatives to protect against injury owing to manual patient lifting. Some promising results have emerged from single state evaluations. Given the importance of the problem, the toll on the lives of nursing home workers and residents, and spiraling economic costs, national studies of the impact of such legislation on reducing musculoskeletal injury specifically among nursing home staff are warranted. We are currently in the midst of a two-year evaluation funded by National Institute for Occupational Safety and Health. As part of this research project, we are cross-linking information from the Occupational Safety and Health Administration Data Initiative (72) with resident level information from the Centers for Medicare and Medicaid Services Minimum Data Set, and facility level information captured by the Certification and Survey Provider Enhanced Reporting system. Extensive administrative data sources collected in the nursing home sector by federal mandate make possible the current research. The research will estimate the effect of state-level safe patient handling legislation on nursing home worker injury rates. In addition, the research will identify characteristics of those nursing homes which may require additional interventions beyond safe patient handling legislation to effectively reduce worker injury rates. We hypothesize that safe patient handling legislation reduces worker injury rates in nursing homes, and that organizational characteristics of the nursing homes (e.g., size, staffing patterns, profit orientation) will impact the effectiveness of state legislation on the rate of worker injuries.
The population is aging and it is highly unlikely that the obesity epidemic will reverse in the near future. Staffing shortages (including nurses, nursing assistants, and other direct care nursing home staff such as occupational therapists) are projected to continue and intensify as Baby Boomers age and require more healthcare services, aging nurses retire, capacity for training new nurses and other direct care staff and the supply of trained nursing assistants and other direct care nursing home staff does not keep up with projected demand (34, 73). There is no evidence that lost workers compensation benefits will be restored or staff turnover challenges in nursing homes will be effectively addressed. These issues will likely exacerbate the issue of worker injuries in nursing homes. Understanding whether legislation is an effective strategy, what specific components of legislation are more effective than others, and whether nursing homes require intervention above and beyond what legislation can be expected to achieve is critical to protect our nursing home workers.
Funding Sources and related paper presentations: This work was funded by a grant to Dr. Lapane from the National Institute For Occupational Safety And Health (1R21OH010769-01A1). There are no related paper presentations to report.
Acknowledgments: We are grateful for Camilla Pimentel’s help in tracking down the information needed to construct the tables presented in this paper.
References
1. Bureau of Labor Statistics. Nonfatal occupational injuries and illnesses requiring days away from work, 2012. Available at: www.bls.gov Accessed 1/19/14.
2. Service Employees International Union SEI. Caring till it hurts: How Nursing Home Work is Becoming the Most Dangerous Job in America. 2nd edition; 1997.
3. U.S. Bureau of Labor Statistics, U. S. Department of Labor. Employer-Reported Workplace Injuries and Illnesses—2014. 2015. Available at: http://www.bls.gov/news.release/pdf/osh.pdf Accessed 5/31/2016.
4. American Health Care Association Reimbursement and Research Department. Trends in Publicly Reported Nursing Facility Quality Measures; Accessed July 11,2016.
5. Castle NG, Engberg J, Mendeloff J, Burns R. A national view of workplace injuries in nursing homes. Health Care Manage Rev 2009;34(1):92-103.
6. Lerner NB, Johantgen M, Trinkoff AM, Storr CL, Han K. Are nursing home survey deficiencies higher in facilities with greater staff turnover. J Am Med Dir Assoc 2014;15(2):102-7.
7. Trinkoff AM, Johantgen M, Muntaner C, Le R. Staffing and Worker Injury in Nursing Homes. American Journal of Public Health 2005;95(7):1220-1225.
8. Okechukwu CA, Bacic J, Velasquez E, Hammer LB. Marginal structural modelling of associations of occupational injuries with voluntary and involuntary job loss among nursing home workers. Occup Environ Med 2016;73(3):175-82.
9. Stanev S, Bailer J, Straker JK, Mehdizadeh S, Park RM, Li H. Worker injuries and safety equipment in Ohio nursing homes. J Gerontol Nurs 2012;38(6):47-56.
10. U.S. Bureau of Labor Statistics, U. S. Department of Labor. Table R5. Incidence rates for nonfatal occupational injuries and illnesses involving days away from work, per 10,000 full-time workers by industry and selected natures of injury or illness, private industry, 2014. 2015. Available at: http://www.bls.gov/iif/oshwc/osh/case/ostb4371.pdf Accessed 5/31/2016.
11. U.S. Bureau of Labor Statistics, U. S. Department of Labor. Table R6. Incidence rates for nonfatal occupational injuries and illnesses involving days away from work, per 10,000 full-time workers by industry and selected parts of body affected by injury or illness, private industry, 2014. 2015. Available at: http://www.bls.gov/iif/oshwc/osh/case/ostb4372.pdf Accessed 5/31/2016.
12. Edlich RF, Hudson MA, Buschbacher RM, Winters KL, Britt LD, Cox MJ, Becker DG, et al. Devastating injuries in healthcare workers: description of the crisis and legislative solution to the epidemic of back injury from patient lifting. J Long Term Eff Med Implants 2005; 15(2): 225-41.
13. Collins JW. CDC Congressional Testimony: Safe patient handling lifting standards for a safer American workforce, May 11, 2010. Centers for Disease Control and Prevention. Available at: http://www.cdc.gov/washington/testimony/2010/t20100511.htm Accessed 1/23/14.
14. U.S. Bureau of Labor Statistics, U.S. Department of Labor. Table R98. Incidence rates for nonfatal occupational injuries and illnesses involving days away from work per 10,000 full-time workers by occupation and selected nature of injury or illness, private industry, 2014. 2015. Available at: http://www.bls.gov/iif/oshwc/osh/case/ostb4464.pdf Accessed 5/31/2016.
15. Cal/OSHA Consultation Service, Research and Education Unit, Division of Occupational Safety and Health, California Department of Industrial Relations. Ergonomic Guidelines for Manual Material Handling. California Department of Industrial Relations, 2007. Available at: http://www.cdc.gov/niosh/docs/2007-131/ Accessed 1/29/14.
16. Massachusetts Nurses Association. Safe Patient Handling, December 2005. Available at: http://www.massnurses.org/nursing-resources/position-statements/safe-patient-handling Accessed 1/29/14.
17. DuBoise J, Donahue T. Taking the pain out of patient handling. American Nurse Today 2006; December: 37-43.
18. Ogden CL, Carroll MD, Kit BK, Flegal KM. Prevalence of childhood and adult obesity in the United States, 2011-2012. JAMA 2014;311(8):806-14.
19. Lapane KL, Resnik L. Obesity in nursing homes: an escalating problem. J Am Geriatr Soc 2005;53:1386-91.
20. Felix HC, Bradway C, Chisholm L, Pradhan R, Weech-Maldonado R. Prevalence of moderate to severe obesity among U.S. Nursing home residents, 2000–2010. Res Gerontol Nurs 2015;8:173–178.
21. Harrington C, Carrillo H, Blank BW, et al. Nursing facilities, staffing, residents and facilities deficiencies, 2004 through 2009 [online]. Available from URL: http://pascenter.org/documents/OSCAR_complete_2010.pdf
22. American Health Care Association (AHCA). 2011 AHCA Staffing Survey Report. 2012. Available at: http://www.ahcancal.org/research_data/staffing/Documents/2011%20Staffing%20Survey%20Report.pdf. Accessed 2/4/2014.
23. Health Resources and Services Administration (HRSA). The U.S. Nursing Workforce: Trends in Supply and Education. Washington, DC: HRSA, April 2013.
24. Marras WS, Davis KG, Kirking BC, et al. A comprehensive analysis of low-back disorder risk and spinal loading during the transferring and repositioning of patients using different techniques. Ergonomics 1999;42:904–26.
25. Centers for Disease Control and Prevention. National Nursing Home Survey, Nursing Home Current Residents, June 2008. http://www.cdc.gov/nchs/data/nnhsd/Estimates/nnhs/Estimates_FunctionalStatus_Tables.pdf#Table14 . Accessed 1/22/14.
26. Pompeii LA, Lipscomb HJ, Shoenfisch AL, et al. Musculoskeletal injuries resulting from patient handling tasks among hospital workers. Am J Ind Med 2009; 52:571-8.
27. Cohen-Mansfield J, Culpepper WJ, Carter P. Nursing staff back injuries: prevalence and costs in long term care facilities. AAOHN Journal 1996;44:9-17.
28. U.S. Department of Health and Human Services (HHS). Understanding Direct Care Workers: A Snapshot of Two of America’s Most Important Jobs. Washington, DC: HHS, March 2011.
29. Fragala, G. Ergonomics: How to Contain On-the-Job Injuries in Health Care. Oakbrook Terrace IL: Joint Commission on Accreditation of Healthcare Organizations. 1996.
30. U.S. Department of Labor Occupational Safety and Health Administration. Guidelines for Nursing Homes Ergonomics for the Prevention of Musculoskeletal Disorders OSHA 3182, 2003 (Revised March 2009). Available at: https://www.osha.gov/ergonomics/guidelines/nursinghome/final_nh_guidelines.html Accessed 1/29/14.
31. Zhang N, Li Y, Temkin-Greener H. Prevalence of obesity in New York nursing homes: associations with facility characteristics. Gerontologist 2013;53(4):567-81.
32. Erickson W, Bruusgaard, D, Knardahl, S. Work factors as predictors of intense or disabling low back pain; a prospective study of nurses’ aides. Occup Environ Med 2004;61:398-404.
33. http://ltcombudsman.org/uploads/files/library/deficiencies-09-14.pdf, Accessed 5/31/16.
34. Trinkoff AM, Brady B. Nielsen K. Workplace prevention and musculoskeletal injuries in nurses. J Nurs Adm 2003;33(3):153-8.
35. Michaels D. National emphasis program (NEP) for programmed inspections of nursing and residential care facilities. OSHA Instruction, US Department of Labor, 04-05-2012. Available at https://www.osha.gov/OshDoc/Directive_pdf/CPL_03-00-016.pdf Accessed 1/23/14.
36. U.S. Department of Health and Human Services (HHS). Understanding Direct Care Workers: A Snapshot of Two of America’s Most Important Jobs. Washington, DC: HHS, March 2011.
37. Institute of Medicine (IOM). Musculoskeletal Disorders and the Workplace: Low Back Pain and Upper Extremities. Washington DC: National Academies Press 2001. Available at: http://www.nap.edu/catalog.php?record_id=10032 Accessed 1/28/14.
38. Krupenevich R, Rider P, Domire Z, DeVita P. Males and females respond similarly to walking with a standardized, heavy load. Mil Med 2015;180(9):994-1000.
39. Ciriello VM, Snook SH. Survey of manual handling tasks. International Journal of Industrial Ergonomics 1999;23:149-156.
40. Office of Inspector General. State Nurse Aide Training: Program Information and Data. Office of Evaluation and Inspections, OEI-05-01-00031, August 2002. Available at: http://oig.hhs.gov/oei/reports/oei-05-01-00031.pdf Accessed 3/14/16.
41. Stone RI, Wiener J. Who will care for us? Addressing the Long-Term Care Workforce Crisis. USDHHS 2001. Available at: https://aspe.hhs.gov/basic-report/who-will-care-us-addressing-long-term-care-workforce-crisis Accessed 3/17/16.
42. Occupational Safety and Health Administration. Adding Inequality to Injury: The Cost of Failing to Protect Workers on the Job. June 2015. Available at: http://www.dol.gov/osha/report/20150304-inequality.pdf Accessed 3/1/16.
43. Grabell M, Nerkes H. The demolition of workers’ comp: over the past decase, states have slashed workers’ compensation benefits, denying injured workers help when they need it most and shifting the costs of workplace accidents to taxpayers. ProPublica, Insult to Injury. Available at: https://www.propublica.org/article/the-demolition-of-workers-compensation Accessed 3/2/16.
44. Zhang Y, Punnett L, Gore R; CPH-NEW Research Team. Relationships among employees’ working conditions, mental health, and intention to leave in nursing homes. J Appl Gerontol 2014;33(1):6-23.
45. Boyer J, Galizzi M, Cifuentes M, d’Errico A, Gore R, Punnett L, Slatin C, et al. Ergonomic and socioeconomic risk factors for hospital workers’ compensation injury claims. Am J Ind Med 2009;52:551-62.
46. Institute for the Future of Aging Services. The Long-Term Care Workforce: Can the Crisis be Fixed? Problems, Causes and Options. Washington DC: American Association of Homes and Services for the Aging, 2007. Available at: http://www.leadingage.org/uploadedFiles/Content/About/Center_for_Applied_Research/Center_for_Applied_Research_Initiatives/LTC_Workforce_Commission_Report.pdf Accessed 3/1/16.
47. Citizens for Long Term Care. Long-Term Care Financing and the Long-Term Care Workforce Crisis: Causes and Solutions. Washington DC: Citizens for Long Term Care, 2003. Available at: http://phinational.org/research-reports/long-term-care-financing-and-long-term-care-workforce-crisis-causes-and-solutions Accessed 3/1/16.
48. Burt CDB. New employee accident rates. In: Risk Factors and Management Strategies. Switzerland: Springer, 2015, pp 9-22.
49. Occupational Safety & Health Administration. Safe patient handling. OSHA Quick Takes, Safety and Health Topics: Healthcare. Available at: https://www.osha.gov/SLTC/healthcarefacilities/safepatienthandling.html Accessed 1/23/14.
50. Oregon OSHA. Sate Patient Handling: A Worthy Investment. Available at: www.orosha.org/ppt/safe_patient_handling.pps Accessed 3/16/16.
51. Collins JW, Nelson A, Sublet V. Safe Lifting and Movement of Nursing Home Residents. Centers for Disease Control and Prevention, National Institute for Occupational Safety and Health. Available at: http://www.cdc.gov/niosh/docs/2006-117/pdfs/2006-117.pdf Accessed 1/23/14.
52. American Nurses Association. Safe Patient Handling and Mobility: Interprofessional National Standards. Silver Spring MD: American Nurses Association, 2013.
53. Occupational Health and Safety Administration. Safe Patient Handling Programs: Effectiveness and Cost Savings. Available at: https://www.osha.gov/Publications/OSHA3279.pdf Accessed 3/16/16.
54. Stenger K, Montgomery LA, Briesemeister E. Creating a culture of change through implementation of a safe patient handling program. Critical Care Nursing Clinics of North America 2007;19(2): 213-222.
55. Lancman R, Wright KLT, Gottfried R. 2011. Safe Patient Handling in New York: Short Term Costs Yield Long Term Results. See assembly.state.ny.us/comm/WorkPlaceSafe/20110527a/index.pdf.
56. Celona J, Hall E, Forte J. Making a business case for safe handling. Presented at the 2010 West Coast Safe Patient Handling and Movement Conference. September 2010; San Diego, California. As cited in: Gallagher SM, Charney W, McGinley LD. 2010. Clinical nursing education series: Rethinking lift teams. Bariatric Times 7(11): 18-23.
57. Hatcher BJ (ed), Bleich MR, Connolly C, Davis K, Hewlett PO, Hill KS. Wisdom at Work: The Importance of the Older and Experienced Nurse in the Workplace. Robert Wood Johnson Foundation 2006. Available at: http://www.rwjf.org/content/dam/supplementary-assets/2006/06/wisdomatwork.pdf Accessed 3/16/16.
58. https://www.congress.gov/bill/111th-congress/house-bill/2381, Accessed May 31, 2016.
59. U.S. House. 113th Congress, 1st Session. H.R.2480.IH, Nurse and Health Care Worker Protection Act.
60. AOHP OSHA Alliance Implementation Team. Beyond Getting Started: A Resource Guide for Implementing a Safe Patient Handing Program in the Acute Care Setting, Second Edition. Wexford PA: AOHP, 2011. Available at: http://www.prismmedicalinc.com/cmss_files/attachmentlibrary/Beyond%20Getting%20Started.pdf Accessed 3/17/16.
61. Ohio Rev. Code Sec. 4121.48. Available at: http://codes.ohio.gov/orc/4121.48. Accessed 1/5/14.
62. New York State Assembly Bill No.: S04929 Available at: http://assembly.state.ny.us/leg/?default_fld=&bn=S04929&term=2005&Summary=Y&Actions=Y&Text=Y Accessed 3/1/16.
63. American Nursing Association. Safe Patient Handling and Mobility (SPHM). Updated June 15, 2015. http://www.nursingworld.org/MainMenuCategories/Policy-Advocacy/State/Legislative-Agenda-Reports/State-SafePatientHandling Accessed 3/2/16.
64. de Castro AB. «Handle With Care®: The American Nurses Association’s Campaign to Address Work-Related Musculoskeletal Disorders» Online Journal of Issues in Nursing.2004; 9 (3), Manuscript 2. Available: www.nursingworld.org/MainMenuCategories/ANAMarketplace/ANAPeriodicals/OJIN/TableofContents/Volume92004/No3Sept04/HandleWithCare.aspx
65. Ohio Bureau of Workers’ Compensation. Ergonomics Best Practices for Extended-Care Facilities. Available at: https://www.bwc.ohio.gov/downloads/brochureware/publications/ExtCareSafeGrant.pdf. Accessed 1/13/14.
66. Safe Patient Handling Workgroup, New York State Department of Health. Report to the Commissioner of Health. (undated). Available at: http://www.health.ny.gov/statistics/safe_patient_handling/docs/sph_report.pdf Accessed 5/31/2016.
67. Silverstein, B.; Schurke, J. Washington State Department of Labor and Industries’ SHARP Program: Implementation of Safe Patient Handling in Washington State Hospitals. Olympia, WA: Safely and Health Assessment & Research for Prevention; 2010. http://www.lni.wa.gov/safety/research/files/safepatienthandlingrpt2010.pdf Accessed 3/16/16
68. Keith Wrightson, Taylor Lincoln, Susan Harley, Brett Sanoian. Uplifting an Industry? State-Based Safe Patient Handling Laws Have Yielded Improvements But Are Not Adequately Protecting Health Care Workers. 2015. Available at: http://www.citizen.org/documents/state-health-care-worker-safety-laws-uplifting-industry.pdf Accessed 5/31/2016.
69. Garg A, Owen B. An ergonomic approach to preventing back injuries from patient lifting. PTSM Series 1994;2:15-22.
70. Castle NG, Engberg J, Mendeloff J, Burns R. A national view of workplace injuries in nursing homes. Health Care Manage Rev 2009;34:92-203.
71. Kurowski A, Gore R, Buchholz B, Punnett L. Differences among nursing homes in outcomes of a safe resident handling program. J Healthc Risk Manag 2012;32(1):35-51.
72. US Government Accountability Office. Workplace Safety and Health: Enhancing OSHA’s Records Audit Process Could Improve the Accuracy of Worker Injury and Illness Data. GAO, 10-10, 2009. Available at: http://www.gao.gov/products/GAO-10-10 Accessed 3/2/16.
73. American Association of Colleges of Nursing. Fact Sheet: Nursing Shortage. AACN 2014. Available at: http://www.aacn.nche.edu/media-relations/fact-sheets/nursing-shortage Accessed 3/17/16.