C. Hugo1, N. Cockburn2, P. Ford2, S. March2, E. Isenring1
1. Faculty of Health Sciences and Medicine, Bond University, Australia; 2. The University of Queensland, School of Dentistry, UQ Oral Health Centre, Herston Rd, Brisbane, QLD 4006, Australia. Corresponding author: Cherie Hugo, Faculty of Health Sciences and Medicine, Bond University, Australia, cherie.hugo@student.bond.edu.au
Jour Nursing Home Res 2016;2:118-122
Published online November 4, 2016, http://dx.doi.org/10.14283/jnhrs.2016.18
Abstract
Objective: As previous studies have used a variety of outcome measures and assessment tools, the relationship between nutrition and oral health in residents of aged care facilities is unclear. The aim of this study was to investigate the association of oral health status and oral health-related quality of life (OHRQol) with nutritional status among residents of aged care facilities using validated assessment tools. Design: Prospective cross-sectional clinical investigation of 65 aged care residents (>65 years). Setting: Two residential aged care facilities from Southeast Queensland, Gold Coast region, Australia. Measurements: An aged care dietitian conducted nutritional assessments using the Subjective Global Assessment (SGA). An oral health therapist performed assessments using the Oral Health Assessment Tool (OHAT) and geriatric oral health assessment index (GOHAI). Results: Of the 65 older adults, almost two thirds (62%; n=38) were malnourished; (55%; n=34 moderately malnourished and 7%; n=4 severely malnourished). Using OHAT, 82% (n=41) needed a dental referral. Malnutrition was strongly associated with poor OHRQoL (p=0.007). Edentulous (no teeth) participants were more likely to limit their contact with others due to their dentures (p=0.025) and in turn, negatively impact OHRQoL. More people who had decayed or broken natural teeth (77%) (p=0.041) had trouble eating firm foods than those who had healthy natural teeth (23%). Modified diet texture was associated with poor nutritional status (p<0.001). Access to dentists in RACFs was an identified barrier to both optimal oral health and nutritional status. Conclusion: Both malnutrition and poor oral health were common in this sample of aged care residents which contributed to poor OHRQoL. Our findings show the SGA, OHAT and GOHAI instruments are appropriate and acceptable for assessing nutrition and oral health in this population. Further research needs to investigate if early and regular oral health assessments and treatments can improve or minimise deterioration in nutritional status in aged care residents. Recommendations for future practice include increasing training and education of RACFs in terms of oral health care and its connection with nutritional status and quality of life, increased access to dental professionals in RACFs and the importance of concurrent referrals to dietitians when dental issues are identified.
Key words: Oral health, oral health-related quality of life, malnutrition.
Introduction
Approximately one in seven Australians (15%) are aged over 65 years, with rates predicted to triple over the next 50 years (1). The Australian prevalence of older adults is comparable to Canada (16%) and US (14%), but behind Japan (26%), Italy (21%), Germany (21%), Sweden (20%) and the UK (18%)(2). With ageing comes increased healthcare costs and often an increased reliance on health services, including residential aged care facilities (RACFs) (3).
The oral health of older people living in care has been widely recognised as inadequate (4-6). Historically, dental service provision has been sparse and problematic for RACF residents (5, 7). Barriers to caring for oral health in RACFs include having inadequate resources and time to support oral health needs, dental practitioners not feeling confident in providing care in the aged care environment and nurses having low levels of motivation and knowledge in providing oral care (4). There is evidence to suggest poor oral health has implications for general systemic health (8, 9), however the association between oral health and nutritional status is unclear. Poor oral health in aged care residents impacts on daily functioning and overall quality of life (8, 10). Measures of health are complex and the relationship with quality of life is often overlooked. The health-related quality of life conceptual model describes that at one end of the continuum there are biological measures and on the other symptoms, functioning, general health perceptions and overall quality of life (11). Previous studies have indicated that oral health quality of life (OHRQoL) factors can negatively impact dietary intake, but no studies have investigated the link between all three domains of oral health, nutrition and quality of life (11-13).
A systematic review (14) of the association between malnutrition and oral health status in the elderly living in long-term care facilities highlighted “tentative evidence” of an independent association between oral health and malnutrition but pointed out the lack of methodological robustness and the importance of using validated assessments. Of the included studies in the review only three out of the 16 studies used a validated assessment tool (14). Due to the absence of agreed measures and the multifactorial nature of both poor oral health along with a range of confounding factors, interpretation of the current evidence is difficult (14). The aim of this study was to undertake a preliminary investigation into the association of oral health status and oral health-related quality of life with nutritional status using validated assessment tools in aged care residents. To our knowledge this is the first study to use the combination of a validated nutrition assessment tool, oral health assessment and oral health assessment quality of life tool (14).
Methods
Participants
Data were collected from January to March 2015 in two RACFs in Southeast Queensland, Australia. Participants were recruited by convenience sampling. The RACF manager along with the research team distributed consent forms to residents and written informed consent was obtained from interested participants or their power of attorney where appropriate. Those identified by the clinical manager with severe and acute illness were excluded.
Outcome measures
Demographic information of participants was collected which included the resident’s age, gender, medical status, current medications as well as level of dependency on others for daily oral hygiene. Social Economic profiling of the facilities was calculated using the Socio-Economic Indexes for Areas guide(15).
A thorough analysis of the participant’s nutritional status was completed by an experienced RACF accredited practising dietitian. The previously validated and reliable Subjective Global Assessment (SGA) nutritional assessment tool was used to evaluate the resident’s medical history, weight changes, dietary intake, gastrointestinal symptoms, functional capacity and a physical examination. A rating of well nourished (A), moderately malnourished (B) or severely malnourished (C) was given overall and in each domain measured in the SGA (16, 17).
The Oral Health Assessment Tool (OHAT) was used by a qualified dental professional (oral health therapist) to assess the oral health of the residents (18). A ranking of healthy (0), changes (1), or unhealthy (2) was recorded for the status of the lips, tongue, gums/tissues, saliva, natural teeth, dentures, oral cleanliness and dental pain. Scores from each category were added, giving a total score of 0 (healthy) to 16 (extensive oral health problems). Additionally, a summary oral health assessment score between 0 and 3 was recorded.
• 0 = participants who had all healthy scores
• 1 = ≥1 changes score in any category
• 2 = ≥1 unhealthy score in categories less likely to impact on function (lips, tongue and oral cleanliness)
• 3 = ≥1 unhealthy score in the categories more likely to impact on function (gums and tissues, saliva, natural teeth, dentures and pain).
A score of 3 indicated that the participant required referral to a dental professional for a problem that may be impacting on oral function (functional impact).
The residents’ oral health-related quality of life (OHRQoL) was assessed using the Geriatric Oral Health Assessment Index (GOHAI)(19). This validated and reliable questionnaire comprised of 12 questions assessing dimensions of physical function, discomfort or pain, behavioural and psychological impacts of oral health (19). Total scores ranged between 12 and 60, with a higher score indicating better oral health. Residents with a GOHAI score of 12-57 were identified as needing dental care and those with a score more than 57 indicated no impact from oral conditions (10, 19).
Statistical analysis
Statistical analysis was performed in SPSS Version 22.0 (IBM Corp, Armonk, United States of America)(20). Continuous variables were tested for normality. Normally distributed continuous variables are presented as mean (SD) and categorical variables as percentage and counts. Chi Square tests were used for bivariate associations between categorical variables. Independent t tests were used to determine differences in continuous variables per categorical variable. P value of <0.05 designated statistical significance.
Ethical consideration
This study was reviewed and approved by the University of Queensland Medical Research Ethics Committee (project no. 2014000794) and Bond University Research ethics committee (project no. RO1883A). Participants and their guardians provided written informed consent.
Results
Participant characteristics
A convenience sample of 65 participants took part in this study (27% of the total RACF’s resident population). Of the 65 participants, 13 were unable to have the dental assessment completed, 16 were unable to have the OHRQoL assessment completed and 3 were unable to have the nutrition assessment completed which resulted in 50 of the participants (77%) completing all assessments. Inability to gather required data was the result of participant illness and/or unplanned circumstances.
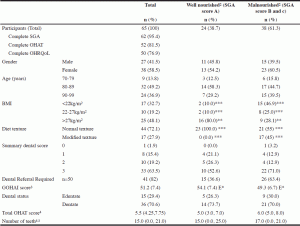
Demographic, nutrition and oral health characteristics of participants can be found in Table 1. There were more female participants (n=38) in the study compared with males (n=27). Females were also significantly older at 87.9 years (SD 4.7) (vs. 84.3 years (SD 7.2) (p=0.033). The ages of participants ranged between 70 and 99 years with the majority being greater than 80 years.
1. Using Subjective Global Assessment (SGA)(17) where “A” indicates nourished and “B”and “C” indicates malnourished; 2. Chi Square Test performed and Fisher’s Exact Test(E) when cell sizes were <5; * = p value significant at <0.05; **=p value significant at <0.005; ***=p value significant at ≤0.001; **statistically significant, p<0.001; 3. Mean (SD); 4. Median (IQR1, IQR3); 5. Including edentate participants;
Nutrition of residents
Almost two thirds (62%) of the residents were malnourished (55% moderately and 7% severely malnourished). Females were significantly lighter than males (59.5kg±12.9 vs. 83.6kg±15.7; p<0.001). BMI differences between genders were statistically significant (p =0.002) with the male mean BMI at 29.3kg/m2 (SD 4.8) compared to females at 23.7kg/m2 (SD 5.4).
Despite most of the participants assessed as malnourished, nearly half (48.1%, n=25) were found to have a BMI greater than 27kg/m2 (categorised as overweight/obese for residents greater than 65 years). Interestingly, 9 of the 25 overweight/obese residents (36%) were found to be moderately malnourished. Over 40% of residents (n=26) were assessed as having inadequate dietary intake and around 50% (n=31) of participants showing weight loss in the past fortnight (compared to 15% in the 6 months prior).
While the majority of participants did not have any gastrointestinal symptoms, the most common symptoms experienced were poor appetite (32%, n=20) and nausea (21%, n=13). Females experienced significantly more gastrointestinal symptoms (nausea p=0.012 and vomiting p=0.05) compared to males. Significantly more residents identified as being malnourished reported anorexia (p=0.001), poor dietary intake (p<0.001) and weight loss in the past fortnight (p<0.001). Modified diet texture influenced a number of nutrition variables including the overall malnutrition (p<0.001), poor dietary intake history (p<0.001), anorexia (p=0.022) and weight loss history in the past 2 weeks (p=0.007). There were significantly more participants with an adequate diet intake history on a normal texture diet (73%, n= 32) compared to those whose diet texture was modified (18%, n= 3) (p<0.001).
Oral health of residents
The median OHAT score was 5.5. From the dental assessment summary scores, 82% of participants (n=41) required a dental referral; 19% of participants (n=10) required referral for reasons not likely to cause functional impacts and 64% (n=33) required referral for reasons likely to impact on normal oral functions like mastication and swallowing. The median number of teeth was 15 and 71% (n=36) of participants had some teeth remaining. From the oral health assessment, 89% (n=46) of participants had inadequate oral cleanliness.
Oral Health-Related Quality of Life (OHRQoL)
The mean total score for the OHRQoL assessment was 51.4 (SD 7.3); a maximum score of 60 indicating good OHRQoL. Participants who were malnourished had poorer OHRQoL than those who were well nourished. The overall results for the GOHAI can be categorised according to their domains.
• Functional limitations: 58% had difficulties biting/chewing food, 24% found it uncomfortable to swallow and in 22% speaking was affected.
• Pain and discomfort domains: 58% had discomfort when eating, 8% use medications to relieve pain and 31% have sensitive teeth.
• Psychological impact domains: 74% were unhappy with appearance, 10% were worried or concerned about their teeth, 35% were nervous of self-conscious and 25% were uncomfortable eating in front of people.
• Behavioural impact domains: 29% limit kinds or amounts of food and 6% limit contact with other due to their teeth.
Impact of oral health on nutrition
Compared to well-nourished residents (53%), more malnourished residents (71%) had oral health issues causing functional impacts such as mastication and swallowing difficulties. A similar proportion of well-nourished and malnourished residents were dentate and malnourished residents had a higher median number of teeth. More people who had decayed or broken natural teeth (86%) had trouble eating firm foods than those who had healthy natural teeth (14%). There were significantly more participants who were malnourished (73% n=22) who had difficulty eating firm foods compared to those who were well-nourished (32% n=6) (p= 0.004). Modified diet texture was associated with domains tested in oral health and OHRQoL assessments. 58% (n=22) of participants with a normal diet texture had unhealthy changes to their teeth compared to 100% (n=12) of participants who had a modified texture diet (p=0.006). The majority (68%, n=13) of well-nourished participants reported never having trouble eating firm foods, comparatively the majority (70%, n= 19) of moderately malnourished participants did have difficulty with firm foods (p=0.01).
Discussion
This study describes the nutrition and oral health status for a sample of aged care residents in Australia using validated and reliable assessment tools and qualified practitioners. Dental problems and malnutrition were common in this population. Approximately two thirds of our participants were moderately to severely malnourished, which falls in line with National figures indicating that 50-80% of aged care residents are malnourished (17, 21). Our results show higher proportions of malnourished aged care residents have functional oral health impacts. The majority of our participants who had trouble eating firm foods had unhealthy changes to their natural teeth. Poor oral health and xerostomia have previously been associated with reduced chewing function and avoidance of firm foods (22). When aged care residents change their diet due to oral health problems their nutrition may suffer in terms of ability to adequately meet micro- and macro-nutrient requirements. There was an observed reduction in quality of life and increased proportion of functionally impared elderly who were malnourished. Our observations are consistent with previous studies that have indicated that poor dental status and OHRQoL factors can influence meal times and loneliness which in turn can negatively impact dietary intake (12, 13, 22, 23).
The quality of this study overall was enhanced by the using valid and reliable assessment tools and lacked strength in the sample size due to a low response rate. Utilizing valid and reliable assessment tools adds to the robustness of the study and is crucial in testing correlations. In addition to this, the health related quality of life conceptual framework was used to incorporate another domain (OHRQoL) that may influence oral health and nutrition in this group and not just biological and functional measures. Our preliminary findings highlight the appropriateness of the SGA tool for assessment of nutritional status and the OHAT and GOHAI tools for assessment of oral health and quality of life. Future studies with a larger sample size should utilize these tools to reduce confounding factors and determine if there is a correlation between oral health and nutrition in aged care residents.
Our oral health assessment results however differed to the comparison population described by Chalmers et al. (2009) in multiple domains. Compared to national results, our participants had higher oral health results (indicating poorer oral health), with the mean OHAT score being 5.87 compared to 2.71 (7). The national study by Chalmers et al. (2009) used trained nurses for the assessment of residents, whereas our study used a dental professional (7). While training nurses in dental health is important for recognition and referral of problems, under-reporting of oral health problems by nurses is likely to influence these results. Future studies should utilize oral health professionals and dietitians for assessments to reduce under-reporting and strengthen study results. In RACFs under-reporting and incorrect assessments can result in fewer referrals to dental professionals as well as an increased risk of nutritional issues. This reinforces the importance of training and education in aged care facilities for carers and nurses as a vast majority of participants from this study required referral to a dental practitioner.
Malnutrition adversely impacts health outcomes including increased risk of pressure injuries and falls, hospital admission, death and poorer quality of life (17, 24). With many contributors to the increased risk of malnutrition among the institutionalised elderly (17, 21), improvement and maintenance of oral health is essential to the residents’ nutritional status (22). It has been recommended that dental practitioners play an important role in the nutritional care of the elderly (10, 12). Extending on this, RACF staff as well as dental practitioners should also proactively recognise and refer aged care residents with poor oral health for dietitian assessment.
Conclusion
Both malnutrition and poor oral health were common in this sample of residents and key issues included dry mouth, anorexia, dental pain, problems consuming firm foods and diet texture. Diet texture was associated with dietary intake and nutritional status. Access to dentists in RACFs was an identified barrier to both optimal oral health and nutritional status. Standardisation of validated assessment tools used in this research area would assist with comparison across studies and improve our understanding of the relationship between malnutrition, poor oral health and ageing. Further research also needs to investigate if early and regular oral health assessments and treatments can improve or minimise deterioration in nutritional status in aged care residents. Recommendations for future practice include increasing training and education of RACFs in terms of oral health care and its connection with nutritional status and quality of life, increased access to dental professionals in RACFs and the importance of concurrent referrals to dietitians when dental issues are identified.
Conflicts of interest: No conflicts of interest.
References
1. Statistics ABo. 4430.0 – Disability, Ageing and Carers, Australia: Summary of Findings, 2012. 2012.
2. The World Bank – http://data.worldbank.org/indicator/SP.POP.65UP.TO.ZS?order=wbapi_data_value_2014+wbapi_data_value+wbapi_data_value-last&sort=asc. Population ages 65 and above. 2015.
3. Australian Institute of H, Welfare. Residential aged care in Australia, 2010-11: a statistical overview. Canberra: Australian Institute of Health and Welfare; 2012.
4. Hearn L, Slack-Smith L. Oral health care in residential aged care services: barriers to engaging health-care providers. Australian Journal of Primary Health. 2014.
5. Hopcraft MS, Morgan MV, Satur JG, Wright FAC. Dental service provision in Victorian residential aged care facilities. Australian Dental Journal. 2008;53(3):239-45.
6. Paley GA, Slack-Smith L, O’Grady M. Oral health care issues in aged care facilities in Western Australia: resident and family caregiver views. Gerodontology. 2009;26(2):97-104.
7. Chalmers JM SA, Carter KD, King PL & Wright C,. Caring for oral health in Australian residential care. Dental statistics and research series no 48 Cat no DEN 193. Canberra: AIHW; 2009.
8. Gil-Montoya JA, de Mello ALF, Barrios R, Gonzalez-Moles MA, Bravo M. Oral health in the elderly patient and its impact on general well-being: a nonsystematic review. Clinical interventions in aging. 2015;10:461.
9. van der Putten G-J, De Visschere L, Van Der Maarel-Wierink C, Vanobbergen J, Schols J. The importance of oral health in (frail) elderly people–a review. European Geriatric Medicine. 2013;4(5):339-44.
10. Gil-Montoya JA, Subirá C, Ramón JM, González-Moles MA. Oral Health-Related Quality of Life and Nutritional Status. Journal of public health dentistry. 2008;68(2):88-93.
11. Wilson IB, Cleary PD. Linking clinical variables with health-related quality of life. A conceptual model of patient outcomes. Jama. 1995;273(1):59-65.
12. Cousson PY, Bessadet M, Nicolas E, Veyrune JL, Lesourd B, Lassauzay C. Nutritional status, dietary intake and oral quality of life in elderly complete denture wearers. Gerodontology. 2012;29(2):e685-e92.
13. Palmer CA. Gerodontic nutrition and dietary counseling for prosthodontic patients. Dental clinics of North America. 2003;47(2):355-71.
14. Van Lancker A, Verhaeghe S, Van Hecke A, Vanderwee K, Goossens J, Beeckman D. The association between malnutrition and oral health status in elderly in long-term care facilities: a systematic review. International journal of nursing studies. 2012;49(12):1568.
15. Statistics ABo. Socio-Economic Indexes for Areas. 2011.
16. Detsky AS, McLaughlin JR, Baker JP, Johnston N, Whittaker S, Mendelson RA, et al. What is subjective global assessment of nutritional status? Journal of Parenteral and Enteral Nutrition. 1987;11(1):8-13.
17. Watterson C, Fraser A, Banks M, Isenring E, Miller M, Silvester C, et al. Evidence based practice guidelines for the nutritional management of malnutrition in adult patients across the continuum of care. Nutrition & Dietetics. 2009;66:S1-34.
18. Chalmers J, Johnson V, Tang JH-C, Titler MG. Evidence-based protocol: oral hygiene care for functionally dependent and cognitively impaired older adults. Journal of gerontological nursing. 2004;30(11):5-12.
19. Atchison KA, Dolan TA. Development of the Geriatric Oral Health Assessment Index. Journal of dental education. 1990;54(11):680-7.
20. IBM Corp. IBM SPSS Statistics, Version 22.0. . Armonk, NY: IBM Corp2013.
21. Banks M, Ash S, Bauer J, Gaskill D. Prevalence of malnutrition in adults in Queensland public hospitals and residential aged care facilities. Nutrition & Dietetics. 2007;64(3):172-8.
22. Budtz-Jørgensen E, Chung J-P, Rapin C-H. Nutrition and oral health. Best Practice & Research Clinical Gastroenterology. 2001;15(6):885-96.
23. Raynaud-Simon A, Lesourd B. Malnutrition in the elderly. Clinical consequences. Presse médicale (Paris, France : 1983). 2000;29(39):2183.
24. Banks MD. Economic analysis of malnutrition and pressure ulcers in Queensland hospitals and residential aged care facilities. 2008.