T. Mernar
Corresponding author: Thomas J. Mernar, PhD, OTR; Department of Occupational Science and Occupational Therapy, Gwynedd Mercy University, 1325 Sumneytown Pike
Gwynedd Valley, PA 19437, Email: Mernar.T@gmercyu.edu
Jour Nursing Home Res 2017;3:1-9
Published online January 6, 2017, http://dx.doi.org/10.14283/jnhrs.2017.1
Abstract
Background: Admission into a skilled nursing facility can pose many challenges for new residents. Many residents possess adverse health conditions and body function and structure impairments which limit their daily activity performance and participation. Little is known about the relationships between activity, social networks, environment, and health of skilled nursing facility residents. Objectives: This study aimed to examine activity, environmental, and social network factors that significantly relate to the physical and mental health states of newly relocated skilled nursing facility residents. Design: A pre-post non-experimental correlational research design was employed during the first and second months of newly relocating to a skilled nursing facility. Setting: Eight skilled nursing facilities from the Greater Los Angeles area were used in this study. Participants: Ninety-four residents answered interviewee-administered questionnaires during their first month of stay and fifty of these residents were available to complete the questionnaire battery during their second month. Measurements: A battery of questionnaires were used to measure the residents’ perceived activity participation, importance, and performance; environmental influence; social networks; and perceived health. Results: The most importantly defined activities for residents during the first and change of first to second month were activities of daily living. Sixteen statistically significant activity and environmental predictors to both positive and negative mental and physical health were found. Conclusion: The statistically significant findings from this study can inform geriatric healthcare provider care, activity programming, and rehabilitation as to which activities and environmental elements positively and negatively relate to resident mental and physical health.
Key words: Activity, environment, health, relocation, skilled nursing facility.
Introduction
Aging can lead to a progressive and inexorable loss of function with increased vulnerability to disease, frailty, and disability (1). Impairments due to disorder and disease states can limit the capacity and ability for older adults to live safely at home. Complex health conditions coupled with insufficient environmental support can lead to hospitalization and subsequent short or long-term admission to a skilled nursing facility (SNF). According to the Centers for Medicare & Medicaid Services 2013 Nursing Home Data Compendium, there were 1.4 million Americans (2.8 % over age 65 and 10.2 % over age 85) residing in 15,643 SNFs by the end of 2012 (2). Of this population of SNF residents, 61.9% had 4 or 5 activity of daily living (ADL) impairments in bed mobility, dressing, eating, transferring and toileting, 63.4% having moderate to severe cognitive impairment, and 35% with incontinence. Among SNF residents aged 65 years and older, 19.4% had a length of stay fewer than 3 months, 24.2% stayed from 3 months to less than 1 year, and 56.4% remained for 1 year or more (3).
SNF residents face the challenges of compromised health and environmental factor constraints of the SNF institution. Limited space, privacy, comfort, and diminished access to mobility aids, self-care items, toilets, closets, and showers are common problems to SNF institutions. A study of 1,988 SNF residents in 40 SNFs in 5 states found that only 25% of the 1,988 residents had private bathrooms, 42% shared a bathroom with their roommate, and the remainder sharing with 3 or more residents. SNF residents needed to travel a range of 3 to 82 feet to reach their primary toileting room, while 13% of the residents needed to leave their room to a shared bathroom down the corridor. A tub or shower was found in 25% of the rooms and many of these did not seem to be operable (4). Studies have also shown that SNF residents have complained about their lack of freedoms of control and choice (5-6), lack of activity (7-8), and diminished social support and social networks (9-11).
To improve the quality of life and care of newly relocated SNF residents, a deeper understanding of resident activity and environmental factors that relate to physical and mental health states is needed. Several research questions were posed in this study. Do residents’ frequency of activity participation, abilities of activity performance, influence of the social and physical SNF environment, and social networks predictors relate to mental and physical health during their first month of relocation to a SNF? Are these relationships different during the second month?
Methods
Study Participants
The study population included adults aged 60 years or greater; who were newly relocated to a SNF; English speaking; scored as “independent” or “modified independence” under the “Cognitive Skills for Daily Decision Making” on the facility utilized Minimum Data Set (MDS) assessment; scored as “minimum assistance”, “extensive assistance”, or “total dependence” for at least 2 of 4 ADLs. Participants were excluded in this study if they were a direct admission from a previous SNF or if they were admitted on hospice care.
Participants were recruited from eight different SNF facilities in the Greater Los Angeles area. Permission to conduct resident interviews was obtained from each SNF administrator. Eligible subject lists were formulated by each MDS coordinator and shared with this principal investigator (PI) after the initial MDS was completed. Eligible and interested participants read or had read to them, an enlarged printed copy of a Health Insurance Portability and Accountability Act (HIPAA) authorization form and an informed consent which were later signed if they wished to participate.
Measures
Three research assistants were trained on administration of all questionnaires and each research assistant was initially supervised by this PI to ensure administrative consistency. Research assistants were blind to the study’s research questions. Upon resident request, questions on the questionnaires were read aloud to each subject and the research assistants/PI circled responses or they could circle their own responses on the questionnaires.
Once the HIPAA and informed consent was signed, a demographic background form was answered that asked questions relative to gender, decade of age, ethnicity, whether receiving occupational, physical, and/or speech therapies, previous type of residence, preference for returning to their previous residence, and choice for relocating to that SNF (preference: “You were given a choice to move here”, strategic: “You had to move because of the changing of your personal circumstances”, reluctant: “You disagreed with moving here”, or passive: “You did not question with the recommendation to move here”).
Four questionnaires were used to measure activity participation, importance, and performance; physical and social environmental climate; social networks; and perceived health. The battery of questionnaires was administered in the aforementioned order to each SNF resident between 5-28 days after admission to the SNF (baseline) and then again after 21-35 days after baseline (follow-up), if they were still present in the facility.
Activity Participation, Importance, and Performance
Because no existing tool specifically measured the perceived frequency, importance, and ability of various activities common to SNF residents, the Perceived Activity Interview (PAI) was developed. The PAI measures the perceived frequency (activity participation), importance (activity importance), and ability (activity performance) of 24 different activities common to institutional SNF living. These 24 activities were grouped into four different categories of activities that included ADL (6), activities organized and offered by SNF staff (6), play/leisure (6), and social (6). For each named activity, the respondents rated the perceived frequency of participation, importance, and performance ability. To support content validity, ADL, social, and play/leisure PAI items were categorized according to the Occupational Therapy Practice Framework II (12).
Physical and Social Environmental Climate
Environmental influence was measured using the Sheltered Care Environment Scale (SCES). The SCES is part of the larger Multiphasic Environmental Assessment Procedure developed by Moos and Lemke (13). The 54-item yes/no questionnaire obtains the resident’s and/or staff member’s appraisal of six dimensions of the physical and social environment. These dimensions include environmental cohesion, conflict, independence, self-disclosure, organization, and physical comfort of an institutional healthcare facility. Lemke and Moos reported that the SCES discriminates among different congregate elderly residences (including SNF facilities) and that the six subscales used have acceptable to high internal consistency (14).
Social Networks
The Lubben Social Network Scale (LSNS) was used as a measure of risk for social isolation. This 10-item scale contains items pertaining to family networks, friend networks, confidante relations, helping others, and living arrangements. Scores range from 0 to 60. Four ‘social isolation risk’ levels were identified: isolated (score of 0-20), high risk (score of 21-25), moderate risk (score of 26-30), and low risk (score of 31-60) (15). The LSNS has been shown to have good internal consistency with a Cronbach’s alpha of 0.76 (16).
Perceived Health
Perceived health was measured using the Short Form Health Survey (SF-12®). The SF-12® is an abbreviated version of the SF-36® Health Survey. The SF-12® measures the mental and physical health-related quality of life of adults via eight health constructs: physical functioning, role physical, bodily pain, general health, vitality, social functioning, role emotional, and mental health (17). Composite scores for both physical health (PCS) and mental health (MCS) are additional calculations made from the eight constructs. The SF-12® has been found to have acceptable convergent/discriminant validity and internal consistency when used with older adults (18).
Statistical Analyses
Mean and summary scores for the background demographic form, PAI, SCES, LSNS, and SF-12® were calculated for baseline (first month) and follow-up (second month). Backward multiple regression analyses were performed to test each research question for this study (2-tailed at the 0.05 level). Activity, environmental, and social network predictors were entered into a regression model with overall physical health (PCS) and overall mental health (MCS) separately at the first month and change of first to second month of relocation (p≤0.05). PASW Statistics 18 software was used to compute the analyses.
Results
Baseline Characteristics
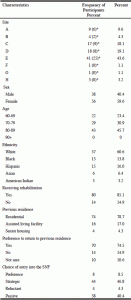
Ninety-four SNF residents participated in this study beginning at baseline during the first month of relocation to a SNF. Fifty participants remained for the follow-up time point during the second month of their stay while forty-four residents were no longer residing in their respective facility during follow-up. Facilities did not disclose specific reasons for the residents not being present during the follow-up. Eighty percent of the first month respondents came from three of the eight total SNFs. Eighty-five percent of the participants were receiving short-term rehabilitation services. Subject characteristics are depicted in Table 1.
Note. *= completed data collection during second month of stay.
Outcome Variables
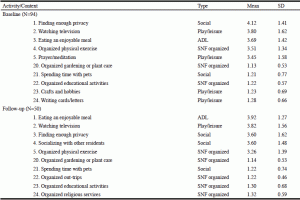
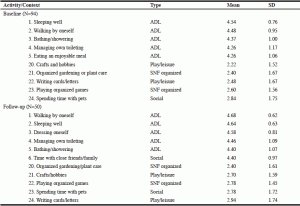
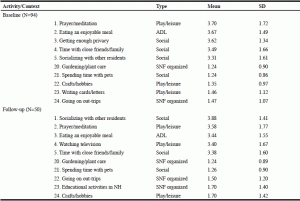
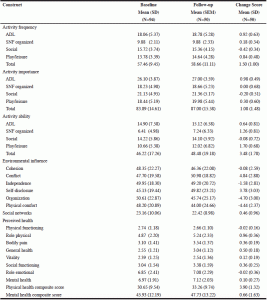
Tables 2-4 were created to record the highest and lowest mean scores of activities at baseline and follow-up for most and least frequently engaged, most and least importantly defined, and most and least able to be performed. Four out of five most frequently occurring activities of finding enough privacy, watching television, eating an enjoyable meal, and organized physical exercise were rated within a range of occurring three or more times a week to once a day at both baseline and follow-up, while gardening or plant care, spending time with pets, and attending organized educational activities were rated as occurring less than once or twice a week during the first and second month of living in a SNF (Table 2). With respect to attributed activity importance, ADL activities were rated as the most important at baseline and follow-up while crafts and hobbies, gardening and plant care, writing cards/letters, playing organized games, and spending time with pets were rated the least important at both time points (Table 3). Prayer/meditation, eating an enjoyable meal, spending time with close friends and family, and socializing with other residents were rated as most able to be performed at both time points with fair to well rated ability, while gardening and plant care, spending time with pets, going on organized out-trips, and crafts and hobbies were rated as least able to be performed at both time points with a rating of some difficulty to great difficulty (Table 4).
Note. Answers correspond to resident’s amount of perceived activity engagement within the past 7 days. Top and bottom 5 of 24 activities are listed. Scale as follows: 5=more than once a day, 4=once a day, 3=three or more times a week, 2=about once or twice a week, and 1=not at all.
Note. Answers correspond to resident’s level of perceived activity importance within the past 7 days. Top and bottom 5 of 24 activities are listed. Scale as follows: 5=very important, 4=important, 3=neutral, 2=little importance, and 1=not important.
Note. Answers correspond to resident’s perceived ability on how well they can perform these activities within the past 7 days. Top and bottom 5 of 24 activities are listed. Scale as follows: 5=very well, 4=well, 3=fair, 2=some difficulty, and 1=great difficulty.
Table 5 illustrates baseline, follow-up, and change score (post-pretest scoring for participants present for both months) data for all outcome measures. Subject scoring on the physical and social environmental climate as measured by the SCES indicate substantial challenges posed on the residents. Compared to normative data taken from more than 1,900 residents across 122 SNFs, residents participating in this study had mean scores lower in cohesion, higher in conflict, lower in institutional organization, and lower in physical comfort at both time points (13). Self-disclosure and conflict were the only constructs that slightly improved from baseline to follow-up. Social networks as measured by the LSNS indicate that residents were indicative of being at a “high risk” of social isolation. Residents available for baseline and follow-up reported mean improvements in eight of the ten constructs of perceived health as measured by the SF-12; however, these scores still denote compromised perceived health conditions.
Note. SD= standard deviation, SEM= standard error of the mean. Change score mean are post-pre test scores for each measure.
Regression Analysis Findings
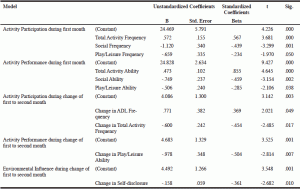
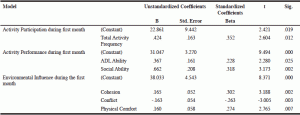
Ten predictor variables were found to be statistically significantly related to resident perceived physical health (Table 6). During the first month of relocation, it was found that the residents who were more frequently able to overall participate in activity but less participative in social and play/leisure pursuits, more able to perform activity overall but less able to perform social and play/leisure activities were found to have a significant relationship with their physical health. Residents who were more frequently participating in overall activity, more able to perform in ADLs, more socially able to perform, perceiving their environments as cohesive, physically comfortable, and with less conflict were found to have a significant relationship with their mental health. Six predictor variables were found to be statistically significantly related to resident perceived mental health (Table 7). During the change from first to the second month, 50 of the initial 94 residents remained. It was found that with these residents, improvements in ADL participation, reductions in overall activity participation, reductions in play/leisure performance, and reduced self-disclosure were found to have a significant relationship with their physical health (Table 6).
Discussion
Fifty of the ninety-four residents were available for data collection during follow-up of their second month of relocation. Eighty-five percent of those originally admitted were receiving skilled rehabilitation under Medicare indicating a likely discharge to home before the follow-up data collection period. Eighty percent of the participant population came from three of the eight SNFs. Each of these three SNFs had a large proportion of residents receiving rehabilitation services. Only fifty-five percent of the residents from these three locations were available for follow-up, indicating likely discharges to home or another level of care. This type of attrition is not surprising since the national average length of stay for a skilled nursing facility resident stay is 28 days (19). The majority of the participants were white (60%) therefore the findings from this study may not be true of all SNF residents of other ethnic backgrounds.
This study offers many important insights into understanding various activity and environmental challenges that relate to perceived health of SNF residents. The nursing facility residents from this study do not appear to be very physically or actively engaged in daily activities. Other research has produced similar findings. In a study of 308 older adults from 30 SNFs found that that the residents were often sitting in public space and not engaged in activity (23%), sleeping or dozing off in public space (10%), or eating or drinking (14%); while many were unobservable/not in public space (36%). Only 16% of the observable sample was actively engaged in activities such as walking or wheeling oneself in a wheelchair (6%) or recreating (10%) (20).
To participate in daily activities of a SNF, residents would need to have both the ability and opportunity to do so. The most frequent types of activities occurring with this sample were mostly sedentary in nature. It was not clearly understood if these frequently engaged activities were selected by the resident, if the environment supported and reinforced engagement in these types of activities, or if it was a combination of both. Gardening/plant care, spending time with pets, crafts/hobbies, and writing cards and letters were rated as least commonly engaged, least important, and least able to perform activities during the first month of relocation. Not all SNFs offer these types of activity opportunities, compared to those SNFs that have adopted principles of the Eden Alternative ™. The Eden Alternative’s™ three main aims are to eliminate loneliness, helplessness, and boredom by developing a home-like habitat (21). Generally, this is accomplished with the inclusion of receiving visits from children, caring for plants, and having companion animals. Interestingly, gardening/plant care and spending time with pets, two inclusionary activities from the Eden Alternative™, were rated as the least commonly engaged, least important, and least able to perform during the first and second month of relocation.
It was interesting to note that ADLs were rated as the most important activity at both baseline and follow-up. For the first and second months, the top five most important categorical activities were all ADLs (from a total of six self-care activities out of a list of twenty-four possible activities). ADL independence needs to be at a level conducive for a safe discharge to home or to a lesser institutionalized setting. Since the majority of these participants were receiving some form of skilled rehabilitation from time of admission, perhaps the high level of importance attributed to ADLs is related to the fact that if a resident’s self-care abilities do not improve from an institutional perspective, they may have a longer length of stay in this setting or relocate to a long-term care environment. This high level of perceived importance to ADLs is striking and has implications for nursing and occupational therapy since these professions offer resident care and enablement of ADL performance and participation.
SNF residents have disabling conditions that limit their physical, mental, social, and spiritual capacities. Within the energy reserves of each resident, a proportion of energy is expended for daily routinized activities (e.g., getting up for meals, participating with nurses in daily self-care, going to rehabilitation, etc.), with the remaining energy available for other activities. With a 74% intention to return back home, the residents from this study may not be concerning themselves with many non-therapeutic activities that may consume their time and energy. The participants of this study may be selectively avoiding activities that consume their valuable energy while focusing more on ADLs to build competence to maximize their chances for returning home. This finding may be supported in that increased engagement in importantly defined ADLs promoted improved perceived physical health. There can be usefulness of SNF staff to explain to residents that there can be health benefits to participate in activities that are outside of their time spent in rehabilitation. Short-term SNF residents, such as those sampled for this study, may avoid activities that may symbolically label them as a long-term SNF resident, such as attending bingo or resident council meetings. Short-term SNF residents may also feel that their goals and needs are different than those long-term care residents who “live” in the SNF. Participants in this study were on average at a high risk of social isolation due to their minimal contacts with their outside social networks. Residents are typically not permitted to leave SNF grounds without institutional permission, therefore, they must rely on friends and family to visit or call them (if they have access to a telephone). Although social networks were not identified as a significant predictor to perceived health, the study participants rated speaking to other residents as occurring less than one time a day on average at both baseline and follow-up.
SNF institutions have a blend of affordances and constraints that enable and disenable resident participation in importantly defined activities. Operations of the SNF are organized by State and federal regulations, administration, departmental policies and procedures, cost-effective staffing, and use of resources. It is essential for political and social forces to recognize that lack of activity or the wrong kind of activities can produce illness, isolation and despair, and can lead to death just as the right kind can enhance health and defer death (22). Although nursing facility residents are not commonly involved in decision making regarding their activities and care (23, 24), attempts need to be made, through qualitative and quantitative research inquiry, to expose problems of SNF environments as well as to reveal practical solutions identified by the SNF residents themselves.
Funding: There was no funding attained to conduct this research study.
Acknowledgments: This study was completed to fulfill the requirements for a PhD in Occupational Science at the University of Southern California. I wish to thank my committee for their guidance during this process: Jeanne Jackson, PhD, OTR/L, FAOTA; Florence Clark, PhD, OTR/L, FAOTA; Mike Carlson, PhD; Diane Parham, PhD, OTR/L, FAOTA; Kathleen Wilber, PhD; and Bin Xie, PhD. Finally, I would like to thank Yuko Ohshita, Pat Halliwell, and Diana Nessa for their data collection efforts.
Conflict of Interest: The sole author of this publication declares no conflicts of interest.
Ethical Standard: Permission to conduct this study was granted by the Institutional Review Board from the University of Southern California.
References
1. National Institute on Aging. Living long and well in the 21st century: Strategic directions for research on aging. Bethesda, MD: NIH; 2007.
2. Nursing home data compendium: 2013 edition. Centers for Medicare & Medicaid Services website. http://www.cms.gov/Medicare/Provider-Enrollment-andCertification/ CertificationandComplianc/Downloads/nursinghomedatacompendium_508.pdf. Accessed February 4, 2015.
3. The National Nursing Home Survey: 2004 overview. Centers for Disease Control and Prevention website. http://www.cdc.gov/nchs/data/series/sr_13/sr13_167.pdf. Accessed February 4, 2015.
4. Cutler LJ, Kane RA, Degenholtz HB, Miller MJ, Grant, L. Assessing and comparing physical environments for nursing home residents: Using new tools for greater research specificity. Gerontologist. 2006;46(1):42-51.
5. Port A, Barrett VW, Gurland BJ, Perez M, Riti F. Engaging nursing home residents in meaningful activities. Annals of Long-Term Care: Clinical Care and Aging. 2011;19(12):20-26.
6. Duncan-Meyers AM, Huebne, RA. Relationship between choice and quality of life among residents in long-term-care facilities. American Journal of Occupational Therapy. 2000; 54:504-508.
7. Weeks LE, Profit S, Campbell B, Graham H, Chircop A, Sheppard-LeMoine D. Participation in physical activity: Influences reported by seniors in the community and in long-term care facilities. Journal of Gerontological Nursing. 2008;34(7):36-43.
8. Voeklkl JE, Winkelhake, K, Jefferies J, Yoshioka N. Examination of a nursing home environment: Are residents engaged in recreation activities? Therapeutic Recreation Journal. 2003;37(4):300-314.
9. Grenade L, Boldy, D. Social isolation and loneliness among older people: Issues and future challenges in community and residential settings. Rehabilitation, Disability, and Aging. 2008;32(3):468-478.
10. Port C L, Gruber-Baldini AL, Burton L, et al. Resident contact with family and friends following nursing home admission. Gerontologist. 2001;41(5):589-596.
11. Zurakowski TL. The social environment of nursing homes and the health of older residents. Holistic nursing practice. 2000, July:12-23.
12. American Occupational Therapy Association. Occupational therapy practice framework: Domain and process (2nd ed.). American Journal of Occupational Therapy. 2008:62:625–683.
13. Moos R, Lemke S. Evaluating residential facilities: The Multiphasic environmental procedure. Thousand Oaks, CA: Sage; 1996.
14. Lemke S, Moos R. Measuring of social climate of congregate residences for older people: Sheltered care environment scale. Psychology and Aging. 1987; 2(1):20-29.
15. Rubinstein RL, Lubben JE, Mintzer JE. Social isolation and social support: An applied perspective. Journal of Applied Gerontology. 1994;13(1):58-72.
16. Lubben J; Gironda M. The social networks of older people: A cross-national analysis. London: Praeger; 1996.
17. Ware JE, Kosinski M, Turner-Bowker DM, Gandek B. How to score version 2 of the SF-12® health survey: With a supplement documenting version 1. Linclon, RI: QualityMetric Incorporated; 2005.
18. Jakobsson U. Using the 12-item Short Form health survey (SF-12) to measure quality of life among older people. Aging Clinical and Experimental Research. 2007;19(6):457-464.
19. Medicare Skilled Nursing Facility (SNF) Transparency Data (CY2013). Centers for Medicare and Medicaid Services website. https://www.cms.gov/Newsroom/MediaReleaseDatabase/Fact-sheets/2016-Fact-sheets-items/2016-03-09.html. Accessed November 4, 2016.
20. Mozley C, Sutcliffe C, Bagley H, et al. Towards quality care: Outcomes for older people in care homes. Burlington, VT: Ashgate Publishing Company; 2004.
21. Thomas WH. Life worth living, how someone you love can still enjoy life living in a nursing home: The Eden Alternative in action. Acton, MA: Vander Wyk & Burnham;1996.
22. Wilcock AA. Occupational science: Bridging occupation and health. Canadian Journal of Occupational Therapy. 2005;72(1):5-12.
23. Shawler C, Rowles GD, High DM. Analysis of key decision-making incidents in the life of a nursing home resident. The Gerontologist. 2001;41(5):612-622.
24. Oosterveld-Vlug MG, Pasman RW, van Gennip IE, et al. Dignity and the factors that influence it according to nursing home residents: A qualitative interview study. Journal of Advanced Nursing. 2013; 70(1):97–106.