D.M. Wilson1, R.R. Brow2, R. Playfair2
1. Faculty of Nursing, University of Alberta, Edmonton, Alberta, Canada T6G 1C9, Canada; 2. Registered Nurse, C/O Faculty of Nursing, University of Alberta Canada. Corresponding author: Donna M. Wilson, Faculty of Nursing, University of Alberta, Edmonton, Alberta, Canada T6G 1C9, Tele (780) 492-5574, fax 492-2551, donna.wilson@ualberta.ca
Jour Nursing Home Res 2017;3:16-21
Published online March 3, 2017, http://dx.doi.org/10.14283/jnhrs.2017.3
Abstract
The need for nursing homes is increasing rapidly now with accelerating population aging and other socio-demographic developments. No indicators currently exist to specify the number of nursing home beds that should be available to meet population requirements. To meet this gap, descriptive-comparative information was gathered on the number of nursing home beds that exist in 10 Canadian provinces and 15 high-income countries and other relevant information. Major differences were found in bed numbers relative to population age structures, with a set of three median indicators (109.4, 17.5, and 4.5) developed to identify the mid-range number of citizens of all ages per nursing home bed, citizens aged 65+ per nursing home bed, and citizens aged 80+ per nursing home bed. Indicators such as these enable comparisons of actual to optimal. The devised set of three indicators should raise nursing attention to nursing home bed accessibility, and further policy and planning for the nursing home expansion required with population aging.
Key words: Nursing homes, residential continuing care facilities, aged care facilities, long-term care, accessibility, benchmarking, policy analysis.
Highlights:
• Indicators allow for measuring the current state against a preferred or optimal state.
• Only a small proportion of older people require long-term institutional type care.
• Ensuring nursing home beds are available when needed is highly important.
• This data analysis created three sets of age-based indicators to use in planning nursing homes.
Introduction
Extended lifespans have resulted in an aging population. A small proportion of people in every country are so physically or cognitively disabled that they require ongoing supportive care (1-3). Most receive this care in the home, and with this care provided primarily if not solely by family members (4-7). Others receive this care in facilities designed for people who require assistance with instrumental and basic activities of daily living (2, 8). Many different types of supportive care facilities exist today, but only some provide 24-hour skilled nursing care; with these variably identified internationally as nursing homes, long-term care facilities, auxiliary hospitals, continuing-care homes, supportive-care facilities, skilled care homes, designated assisted living facilities, and aged care facilities (9). For instance, the Canadian province of Ontario has nursing homes or long-term care homes that are “designed for people who require the availability of 24-hour nursing care and supervision, sometimes within a secure (lock-down) setting. In general, long-term care homes offer more personal care and support than that offered by retirement homes or supportive housing. Long-term care homes are licensed and authorized as government-regulated residences and receive government funding from the Ministry of Health and Long-Term Care.”(10, para 6) In Canada, 4.5% of older people live in nursing homes that are designed to provide 24-hour skilled nursing care (8).
In the province of Alberta, where the authors live, the term “nursing home” is used to designate a facility that provides 24-hour nursing care for people with dependency care needs, with the term “nursing home” subsequently used in this report as a way of differentiating these homes from other care facility types. Nursing homes differ from lodges, assisted living facilities, seniors’ housing complexes, and other facilities that do not offer skilled nursing care, medical care, personal care, and other supportive care services around the clock (2). This distinction is important, as nursing home residents are often highly or completely dependent on their caregivers (7). For instance, most nursing home residents now suffer from significant senescence as a result of advanced aging (7). Unstable health is also common, with many nursing home residents suffering from one or more late-stage illnesses that require continual monitoring and management (4, 11). In Canada, the average age of nursing home residents now is 85, and the most common health problems impacting them are bladder incontinence, dementia, and musculoskeletal diseases (12). Nursing homes now are also increasingly providing onsite palliative or end-of-life care (9, 13, 14).
Nursing homes can be found in all developed countries and many developing countries. An increase in nursing homes and nursing home beds has been expected for some time now in keeping with population aging (1, 2, 15). However, with population aging accelerating as the large babyboom generation has started to reach age 65, planning ahead is critically important to ensure that all older people needing nursing home-level care will be able to receive it as soon as possible after it becomes necessary (11). If nursing home beds are not available, their care will primarily take place in home or hospital. Family caregiver exhaustion, inappropriate hospital admissions, and extended hospital stays are common outcomes of nursing home bed shortages (11, 16). A study of waiting in hospital for nursing home placement also revealed the concern that people waiting indefinitely in hospital for a nursing home bed have a low quality of life; with this in part due to a lack of staff who are educationally prepared to care for them (16).
At the same time, excess nursing home beds are problematic for population health and multiple other reasons. People who move into a nursing home prematurely tend to lose their independence capacities. Moreover, the cost of building and maintaining nursing homes, as well as the cost of providing nursing and supportive care there is higher than the cost of providing care in the home (7, 16). Unfortunately, no indicators exist to suggest or mandate the number of nursing home beds that should be available to meet population needs. This report outlines the development of some possible indicators.
Methods
Any project to develop nursing home bed indicators must be aware of major cross-border differences in the nomenclature of nursing homes, as well as historic and current local or country-specific factors impacting nursing homes. For instance, since 1984, the Canada Health Act has mandated public funding for medically-necessary healthcare services in Canada regardless of where this care is provided. Medically-necessary healthcare services are therefore provided on-site and elsewhere at no cost to Canadian nursing home residents. This provision occurs regardless of whether they reside in a public or private nursing home, but all nursing home residents must still pay out-of-pocket the “hotel” cost portion of their residential care facility. This fee is designed to cover overhead accommodation expenses and on-site services such as meals and housekeeping. Every Canadian province sets a daily fee rate for their public nursing homes; in Alberta, this fee currently ranges from $51.10 to $62.25 dollars per day for a shared or private room (17).
Every Canadian province determines the number and thus availability of nursing home beds through building, expanding, or closing public nursing homes; and through directly or indirectly encouraging or restricting the private nursing home sector (11). Other developed countries also appear to have considerable flexibility in relation to the size of their nursing home sector. No policies mandating nursing home bed numbers were found worldwide in the late 1990s (2).
To develop indicators, credible information on nursing home numbers, nursing home bed numbers, population age structure numbers, and population age demographics were sought in 2015 through university library database and Internet searches. Country and province specific information was subsequently obtained from health departments and other government or non-government information sources. As this project was not a research study, but instead a review of publicly-available information, institutional research ethics approval was not required.
This search for information was first performed for Canada’s 10 provinces and then other similar high-income developed countries. The 27 countries listed in a 2011 OECD report on nursing homes and the 10 countries listed in Ribbe et al.’s 1997 comparison of long-term care systems were first checked for information (2, 3). Not all had accessible and current or relatively current information. In total, relatively current (within 2 years of 2015) and comparative information was found for 15 countries, mostly European ones, and 10 provinces, but not Canada as a whole.
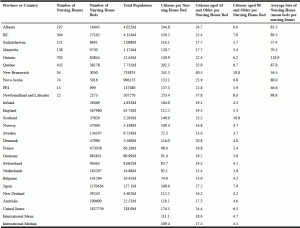
After verifying the numbers gathered for each province and country (see Table 1), a decision was made to calculate the number of citizens per nursing home bed in each province and country using the practical rational that a nursing home bed can only be used by one occupant at a time. This decision varies from the current practice of ratios, such as beds per 1,000 persons or 10,000 persons. Three calculations were made for each province and country, one in relation to their total population (i.e. number of citizens per bed) and two in relation to old-age demographics; the number of persons aged 65 and older per bed, and the number of persons aged 80 and older per bed. Nursing homes are more typically used by very-old persons, although some beds are used by younger persons (6-8). For instance, a study in Alberta found nearly 5% of nursing home residents were under the age of 65 and another 5% aged 65 to 80 (18).
a. Data sources listed below.
The calculated figures for each jurisdiction were then compared and found to differ greatly. Consequently, a median number and an average number across the 15 countries for each of the three age groups was devised as indicators for benchmarking purposes. Canada was excluded, as no nation-wide number of beds could be located and verified, and summing the number of provincial beds was not used to devise a national number out of concern for compounded error.
Benchmarking with indicators is widely done now to permit comparisons of actual against one or more measures (19). As such, the devised nursing home bed indicators could potentially be used to reveal a deficit or an excess in nursing home bed numbers. Benchmarking has become extremely important, with benchmarking a single event leading to major change, or repeated at regular intervals for continued monitoring to identify needed adjustments or other actions over time (19).
Regardless, the information provided in Table 1 must be viewed as approximate given the considerable cross-border diversity as to which beds are classified as nursing home beds. In addition, this indicator-development exercise gathered the most current publicly-available nursing home information, information that often reflected numbers dated one or two years. Nursing home bed numbers change over time, sometimes rapidly as a result of nursing home closures and new homes being built or expanding existing ones. Moreover, it must be recognized that populations change from year to year in age demographic and other characteristics.
Results and Discussion
As illustrated in the Table, major differences in actual and population-relative nursing home bed numbers were found across the 25 jurisdictions. In Canada, the difference in calculated citizens of all ages per nursing home bed ranged from 116.1 in Saskatchewan to 244.7 in Alberta, and internationally from 72.4 in Sweden to 174.5 in the United States of America. In addition, citizens aged 65+ per bed ranged in number from 17.7 in both Saskatchewan and Manitoba to 40.5 in New Brunswick, and internationally from 13.6 in Sweden to 27.2 in Japan. Moreover, citizens aged 80 and older per nursing home bed ranged within Canada from 5.4 in Manitoba to 10.8 in New Brunswick, and internationally from 3.7 in Sweden to 10.8 in Scotland.
Although these bed differences across the 10 Canadian provinces and 15 countries are considerable, this is not the first time that large variances in nursing home availability or use has been noticed. In 1997, a comparative study of 10 mainly European countries revealed widely ranging institutionalization rates; with 2% to 5% of citizens aged 65+ in these countries living in nursing homes, and with this diversity said to be due “at least in part to differences in the organization and financing of long-term care services, in the amount of responsibility assumed in the care for disabled elderly people by each sector and the availability of long-term care beds.” (2, p. 3)
As indicated above, a decision was made to calculate three sets of means and three sets of medians as diverse citizen-to-bed figures in the 10 provinces and 15 countries were found, and using the information gained from the 15 countries only, as pan-Canadian information could not be located. The extreme diversity in nursing home beds across Canadian provinces and the fact that each province has the independent ability to plan nursing home and other healthcare services suggests indicators derived from whole country figures are more valid. Both a mean and median were calculated for the three age demographic groups. Among the 15 countries, the mean/median citizens of all ages per nursing home bed was 111.1 and 109.4 respectively. The mean/median citizens aged 65+ per nursing home bed was 18.6 and 17.5 respectively. The mean/median citizens aged 80+ per nursing home bed was 4.7 and 4.5 respectively.
All three sets of mean or median figures could potentially be used as indicators for benchmarking purposes (18). However, the median indicators are more valid, as averages are easily skewed by a few high or low outliers. Little spread between the means and medians were noted however. Moreover, the median indicators for citizens aged 80+ per nursing home bed may be the most relevant for nursing home benchmarking purposes, as residents are typically 80 years of age or older (18). However, as population aging has focused attention on people aged 65 and older, the median indicators for people aged 65+ may also be useful. For instance, a 2011 OECD report on long-term care beds in 27 countries focused on beds per 1,000 persons aged 65+, with an average of 50 beds per 1,000 persons aged 65+ (or 1 bed for every 20 such persons) calculated using 2009 data (3). No median figure was provided. The current exercise in indicator development found the mean number of citizens aged 65+ per nursing home bed across the 15 countries was 18.6 (median=17.5).
All three sets of indicators may therefore be useful, and particularly as each jurisdiction is likely to have considerable diversity in their need for and use of nursing home beds as a result of country-specific or region-specific age structure, socio-demographic, health, and health system differences. The case of Scotland illustrates this point, as Scotland was found to have 140.0 citizens of all ages per nursing home bed (compared to the international median of 109.4), 23.5 citizens aged 65+ per nursing home bed (compared to the international median of 17.5), and 10.8 citizens aged 80+ (compared to the international median of 4.5) per nursing home bed. All three comparisons reveal a low number of nursing home beds in Scotland. However, it is possible that older people in Scotland may have less need for residential care as supportive care in the home through district nursing has been a health system priority there (20, 21). In contrast, high hospitalization rates and long hospital stays in Japan (22, 23), help explain why Japan has the least available nursing home beds among the 15 countries for citizens aged 65+ and the second least available nursing home beds for citizens aged 80+. Japan is the “oldest” country in the world now, with one of every four citizens aged 65 or older and with many of these aged 80 and older (24). Similarly, the United States of America has the highest ratio of citizens of all ages per nursing home bed (174.5) and also high ratios of citizens aged 65+ and 80+ per nursing home bed. These comparisons indicate research is needed to determine why this low number of nursing home beds exists, so as to determine the impact of this low number of nursing home beds (25).
These indicators may also be useful for benchmarking in Canada. The finding that the province of Alberta leads Canada in having the least available nursing homes for citizens of all ages is notable, with Alberta’s 244.7 citizens per bed comparing starkly against the devised international median indicator of 109.4. Alberta has had a long-standing policy preference to support aging in place, a euphemism for staying at home (26). Yet, long waits for nursing home admission have been problematic for many years in Alberta, with inappropriate hospital admissions, extended hospital stays, and family caregiver exhaustion highly concerning outcomes (7, 16). The province of Alberta has the “youngest” population in Canada (27), with supportive care options for older people overlooked as compared to acute healthcare services for younger people.
It is also relevant to note that the accessibility and use of nursing homes likely varies considerably within each region or country (25). The three sets of indicators do not account for differences in population density, nursing home geographic placement issues, and other relevant matters. As such, it is important to recognize that mismatched local-area population needs and nursing bed numbers are possible even if a region or country has a higher number of nursing home beds than indicated. This issue is highlighted by an analysis of nursing home beds in the Canadian province of Newfoundland and Labrador, which revealed major differences from one region to another in nursing home bed use by persons aged 75+ (11). A related consideration is rural/urban age differences, a matter of concern in many countries as rural areas typically have a much higher proportion of older people than urban areas (28).
Before concluding, it is important to note that nursing homes often differ in size. Information on the number of beds per nursing home in all 10 Canadian provinces was available and is reported in Table 1. A nursing home average bed size was calculated for each province, and these averages were then compared across the 10 provinces. Nursing homes ranged in average size from a low of 56.5 beds in the province of New Brunswick (the province that led the country in least available nursing home beds for citizens aged 65+ and citizens aged 80+) to a high of 118.9 beds in Ontario. The province of Ontario was thus not only found to have the largest nursing homes in terms of average size, but also more nursing homes than in other provinces. To some degree, these findings are understandable, as Ontario has a large population and is highly urbanized, so large nursing homes in metropolitan areas could be expected.
However, it is also important to know that Ontario set a policy goal in 1998 to expand and build new nursing homes over an eight year period, with the aim of adding 20,000 more nursing home beds in the province (29). The intended doubling in bed numbers did not occur, despite a policy target of 100 beds per 1,000 individuals aged 75+ (29). The current exercise to develop indicators for benchmarking purposes revealed the current number of Ontario nursing home beds is comparatively low now in Canada in relation to all three median indicators. Ontario may need to plan to increase the size of its nursing home sector or alternatively justify their low comparative number of nursing home beds. It is possible that Ontario has positive old-age health and wellness outcomes as a result of accessible and effective home-based or community-based care services such as home hospice care and hospital at home services that support aging in place, rehabilitation and chronic care in place, and possibly also dying in place.
Conclusions
Population-linked nursing home bed numbers were found to be highly diverse across 15 developed countries and 10 Canadian provinces, a diversity that suggests reduced availability of beds in some cases and excesses in others. These large differences require additional study and discussion as it is of great concern that dependent older persons may not be receiving the nursing care that they require. This is not an easy task, as 24-hour care can be provided in a nursing home and in other places. What is clear though is that most governments are actively seeking to find ways to better meet the supportive care needs of older persons; ways that are humane and efficient, if not economical. This exercise, which resulted in three sets of median indicators for benchmarking purposes, may help further this policy and planning through focusing nursing attention on the relative or “right” number of nursing home beds for distinct age-based population groups.
Conflict of interest: None to declare.
Appendix
Data Sources
(1) http://www12.statcan.gc.ca/census-recensement/2011/as-sa/fogs-spg/select-Geo-Choix.cfm?
(2)http://data.worldbank.org/indicator/AG.LND.TOTL.K2
(3) http://www.scotland.gov.uk/Resource/Doc/923/0010669.pdf
(4) http://www.ahw.gov.ab.ca/IHDA_Retrieval/redirectToURL.do
(5) http://www12.statcan.gc.ca/nhs-enm/2011/as-sa/fogs-spg/Pages/FOG
(6) http://www12.statcan.gc.ca/nhs-enm/2011/as-sa/fogs-spg/Pages/FOG
(7) http://www12.statcan.gc.ca/nhs-enm/2011/as-sa/fogs-spg/Pages/FOG
(8) http://www12.statcan.gc.ca/nhs-enm/2011/as-sa/fogs-spg/Pages/FOG
(9) http://www12.statcan.gc.ca/nhs-enm/2011/as-sa/fogs-spg/Pages/FOG
(10) http://www12.statcan.gc.ca/nhs-enm/2011/as-sa/fogs-spg/Pages/FOG.
(11) http://www12.statcan.gc.ca/nhs-enm/2011/as-sa/fogs-spg/Pages/FOG
(12) http://www12.statcan.gc.ca/nhs-enm/2011/as-sa/fogs-spg/Pages/FOG.
(13) http://www12.statcan.gc.ca/nhs-enm/2011/as-sa/fogs-spg/Pages/FOG
(14) https://www.cia.gov/library/publications/the-world-factbook/rankorder/2119rank.html
(15) http://www.scotlandscensus.gov.uk/ods-web/standard-outputs.html
(16) http://www12.statcan.gc.ca/census-recensement/2011/dp-pd/prof/details/page
(17) http://www12.statcan.gc.ca/census-recensement/2011/dp-pd/prof/details/page
(18) http://www12.statcan.gc.ca/census-recensement/2011/dp-pd/prof/details/page
(19) http://www12.statcan.gc.ca/census-recensement/2011/dp-pd/prof/details/page
(20) http://www12.statcan.gc.ca/census-recensement/2011/dp-pd/prof/details/page
(21) http://www12.statcan.gc.ca/census-recensement/2011/dp-pd/prof/details/page.
(22) http://www12.statcan.gc.ca/census-recensement/2011/dp-pd/prof/details/page.
(23) http://www12.statcan.gc.ca/census-recensement/2011/dp-pd/prof/details/page.
(24) http://www12.statcan.gc.ca/census-recensement/2011/dp-pd/prof/details/page
(25) http://www12.statcan.gc.ca/census-recensement/2011/dp-pd/prof/details/page
(26) http://stats.oecd.org/viewhtml.aspx
(27) http://data.worldbank.org/indicator/SP.POP.65UP.TO.ZS
(28) http://www.scotlandscensus.gov.uk/ods-web/area.html#!
(29) http://stats.oecd.org/index.aspx#
(30) Number of Long term care Beds in institutions and hospitals per 1000 population over 6. Number of long term care beds then calculated using most recent available population over 65. http://www.oecd-ilibrary.org/docserver/download/8113161ec078.
(31) Page 9 http://www.albertahealthservices.ca/Publications/ahs-pub-2013-2014-annual-report.pdf
(32) Canadian Healthcare Facilities Volume 20, 2013, Canadian Healthcare Association. (Beds and facilities defined as long term care beds with full nursing care counted)
(33) Page 68 – http://www.healthcarecan.ca/wp-content/uploads/2012/11/CHA_LTC_9-22-09_eng.pdf (Note that data is from 2007 version of Canadian Healthcare Association. (2007). Guide to Canadian Healthcare Facilities, 2007-2008. Vol. 15. Ottawa: CHA Press)
References
1. Brown HL, Bub L. Care transitions across the continuum: improving geriatric competence. Geriatr Nurs. 2016;37:68-70.
2. Ribbe MW, Ljunggren G, Steel K, et al. Nursing homes in 10 nations: a comparison between countries and settings. Age Aging. 1997;26(Suppl 2):3-12. doi: 10.1093/ageing/26.suppl_2.3
3. Organization of Economic Co-operation and Development. Long-term Care Beds in Institutions and Hospitals. Health at a Glance 2013: OECD Indicators, 2013. Paris: OECD Publishing. Available from : http://www.oecd-ilibrary.org/docserver/download/8113161e.pdf Accessed 24.06.16.
4. Bishop CE. (1999). Where are the missing elders? The decline in nursing home use, 1985 and 1995. Health Affair. 1999;18(4):146-155. doi: 10.1377/hlthaff.18.4.146
5. Stajduhar KI. Burdens of family caregiving at the end of life. Clin Invest Med. 2013;36(3):E121-E127.
6. Statistics Canada. Elder Care: What We Know Today, 2009. Available from: http://www.statcan.gc.ca/pub/11-008-x/2008002/article/10689-eng.htm. Accessed 24.06.16.
7. Wilson DM, Birch S, Cohen J, et al. Home care developments in the Canadian province of Alberta with regionalization. Glob J Health Sci. 2011;3(1):3-8. doi: 10.5539/gjhs.v3n1p3
8. Statistics Canada. Living Arrangements of Seniors, 2015. Available from: https://www12.statcan.gc.ca/census-recensement/2011/as-sa/98-312-x/98-312-x2011003_4-eng.cfm. Accessed 24.06.16.
9. Australian Institute of Health & Welfare. Use of Aged Care Services Before Death, 2015. Available from: http://www.aihw.gov.au/publication-detail/?id=60129550413. Accessed 24.06.16.
10. Ontario Retirement Communities Association. Senior Living Options, 2016. Available from: http://www.orcaretirement.com/retirement-living/seniors-living-options/. Accessed 24.06.16.
11. Hughes N, McDonald J, Barrett B, et al. Planning the restructuring of long-term care: The demand, need and provision of institutional care beds in Newfoundland and Labrador. Health Manage Forum. 2008;21(2):6-13.
12. Canadian Institute for Health Information. When a Nursing Home is Home: How do Canadian Nursing Homes Measure up on Quality? Continuing Care Reporting System (CCRS) Analyses in Brief and Analytic Reports, 2013. Available from: https://secure.cihi.ca/estore/productFamily.htm?pf=PFC2033. Accessed 24.06.16.
13. Houttekier D, Cohen J, Surkyn J, et al. Study of recent and future trends in place of death in Belgium using death certificate data: A shift from hospitals to care homes. BMC Public Health. 2011;11(1): 228-237. doi: 10.1186/1471-2458-11-228
14. Wilson DM, Truman C, Thomas R, et al. The rapidly changing location of death in Canada, 1994-2004. Soc Sci Med. 2009;68(10):1752-1758. doi: 10.1016/j.socscimed.2009.03.006
15. Wiener JM, Tilly J. Population ageing in the United States of America: Implications for public programmes. Int J Epidemiol. 2002;31(4):776-781. doi: 10.1093/ije/31.4.776
16. Wilson DM, Vihos J, Hewitt JA, et al. Examining waiting placement in hospital: Utilization and the lived experience. Glob J Health Sci. 2014;6(2):12-22. doi: 10.5539/gjhs.v6n2p12
17. Alberta Health. Continuing Care – Accommodation Charges, 2016. Available from: http://www.health.alberta.ca/services/continuing-care-accommodation-charges.html. Accessed 24.06.16.
18. Wilson D, Truman C. Long-term-care residents. Concerns identified by population and care trends. Can J Public Health. 2004;95(5):382-386.
19. Ettorchi-Tardy A, Levif M, Michel P. Benchmarking: A methods for continuous quality improvement in health. Healthcare Policy. 2012;7(4):e101-e119.
20. Steel D, Cylus J. United Kingdom (Scotland). Health System Review, 2012. A European Observatory on Health Systems and Policies report on health systems in transition. Available from: http://www.euro.who.int/__data/assets/pdf_file/0008/177137/E96722-v2.pdf. Accessed 24.06.16.
21. The Scottish Government. Modernizing Nursing in the Community, 2012. Available from:http://www.gov.scot/Publications/2012/07/9145/1. Accessed 24.06.16.
22. Gleysteen WH. Report of a one-day conference: Making universal health care affordable. How Japan does it, 1993. Available from: https://www.nyu.edu/projects/rodwin/lessons.html. Retrieved 24.06.16.
23. Tatara K, Okamotao E. Japan. Health System Review, 2009. A European Observatory on Health Systems and Policies report on health systems in transition. Available from: http://www.euro.who.int/__data/assets/pdf_file/0011/85466/E92927.pdf. Accessed 25.06.16.
24. United Nations. World Population Ageing, 2015. Available from: http://www.un.org/en/development/desa/population/publications/pdf/ageing/WPA2015_Report.pdf. Accessed 24.06.16.
25. Centers for Disease Control and Prevention. Long-term Care Services in the United States – 2013 Overview, 2013. Available from: http://www.cdc.gov/nchs/data/nsltcp/long_term_care_services_2013.pdf. Accessed 24.06.16.
26. Alberta Health. Continuing Care Strategy, 2008. Available from: http://www.health.alberta.ca/initiatives/continuing-care-strategy.html. Accessed 24.06.16.
27. Statistics Canada. Population by Age and Sex, 2012. Available from: http://www.statcan.gc.ca/pub/91-215-x/2012000/part-partie2-eng.htm. Accessed 24.06.16.
28. Keating N, Swindle J, Fletcher S. Aging in rural Canada: A retrospective and review. Can J Aging. 2011;30(3):323-338. doi: http://dx.doi.org/10.1017/S0714980811000250
29. Ministry of Health and Long-term Care. 3-04 – Long-term care facilities activity, 2002. Available from: http://www.auditor.on.ca/en/reports_en/en02/304en02.pdf. Accessed 24.06.16.