I. Binot1,2, N. Tavassoli3,4, E. Berard5,6, A. Perrin3, S. Bismuth7, E. Giovanni7, A. Lafourcade7, B. Vellas3,4,6, Y. Rolland3,4,6
1. Department of Geriatric Medicine, Amiens University Hospital, France; 2. Laboratory of Functional Neurosciences EA4559, Amiens University Hospital, France; 3. Toulouse Gerontopole, Department of Internal Medicine and Clinical Gerontology, Toulouse University Hospital, France; 4. Regional Team on Aging and Prevention of Dependency (ERVPD), Toulouse Gerontopole, Toulouse University Hospital, France; 5. Epidemiology Department, Toulouse University Hospital, France; 6. INSERM UMR 1027, Toulouse III University, Toulouse, France; 7. University Department of General Practitioners, Toulouse III University, Toulouse, France. Corresponding author: Ingrid Binot. North Hospital, Department of Geriatric Medicine, Amiens University Hospital, Place Victor Pauchet – 80054 Amiens cedex 1, Fax: 33.3.22.45.53.30, Phone: 33.3.22.45.57.20. E-mail: binot.ingrid@chu-amiens.fr
Jour Nursing Home Res 2017;3:28-37
Published online March 3, 2017, http://dx.doi.org/10.14283/jnhrs.2017.5
Abstract
Background: Transfer of residents from nursing home (NH) to emergency department (ED) can be inappropriate or potentially avoidable. Objectives: To determine the rate of inappropriate (IT) or potentially avoidable (PAT) transfers of NH residents to ED and to identify the factors associated with these transfers. Setting: Two emergency departments of Toulouse University Hospital, France. Design: All residents arriving at the ED during one week were included. Data were collected, the day of the resident’s transfer, by face to face interviews with the ED’s practitioner and by phone call to the general practitioner (GP) or the health professional in the NH who decided the transfer. An independent panel of experts in geriatrics, pharmacy, emergency and family medicine assessed the appropriateness and potentially avoidable profile of transfers. Results: Fifty-four residents were included. 43% (n=23) considered as IT and 48% (n=26) as PAT. The main factors associated with IT was a low score on basic ADL (Activities of Daily Living) (p=0.03), the need of physician to be reassured about the resident’s pathology (p=0.03) and a lack of technical support in the NH (p=0.03). Iatrogenic medication was found in 44% of the resident with PAT. Before the transfer to ED and after the return in NH, there was a significant increase in diagnosis of dementia (p=0.01) and a non-significant decline in residents’ functional status (ADL score) (p=0.05). Conclusion: This pilot study suggested that factors associated with IT and PAT are related to the clinical characteristics of the residents, the isolation of the NH and the poor quality of prescription. Some factors seem accessible to improvement.
Key words: Nursing home, emergency department, inappropriate transfer, potentially avoidable transfer.
Introduction
In France, Europe or North America, yearly rate of hospitalization of nursing home (NH) residents is around 30% and most of the transfers lead to an emergency department admission (ED) (1, 2). With numerous co-morbidities, high polypharmacy, poor physical function and significant cognitive impairment, acute changes in the resident health status are complex situations that frequently exceed NH’s resources and lead to transfer residents to the hospital (3, 4). During the past decade, various reports have highlighted the questionable risk/benefit balance of NH resident’s hospitalization (5, 6). Beside the advantages of ED care (access to human’s expertise and laboratory test, radiological exam and follow-up), ED admission is an uncomfortable and scary experience for NH residents. It increases the risk of iatrogenic events such as falls, pressure ulcers, delirium, nosocomial infections, and functional decline (7-10). These events increase the length of stay at the hospital, the healthcare costs (6, 11) and reduce the quality of life. Moreover, the reason to transfer residents to ED might be questionable. Indeed, growing evidences support that many transfers to ED are inappropriate or potentially avoidable (1, 5, 6, 11). Therefore, the rate of inappropriate or potentially avoidable hospitalizations of the NH residents has become an indicator of poor quality of care in NH and targets for quality improvement (6).
Inappropriate or potentially avoidable hospitalizations are usually defined using the Ambulatory Care Sensitive Diagnosis (ACSD) (5). The ACSD lists disorders such as urinary tract infection, pneumonia, or dehydration that may have been cared without loss of chance in the NH (without requiring a transfer to the hospital), or potentially avoidable conditions by appropriate care such as vaccination or better management of chronic diseases upstream acute events. However, the transfer may be appropriate (severe acute heart failure for instance) but potentially avoidable (poor preventive treatment in the NH) (8). Although the use of the ACSD is fairly widespread, this tool has some limitations. It is not specific to the transfer to an ED and does not take into account the characteristics and some special conditions of NH residents (12).
Another approach to define appropriateness of a hospital transfer is to perform a Structured Implicit record Review (SIR) (1). It supposes that an expert panel takes account the circumstances in the NH before the resident’s transfer to the hospital and the patient’s benefit after the hospitalization. Appropriateness of a hospital transfer is widely variable from 13,1% to 67% (11, 13) depending on whether the rating relies on a list of diseases, the panel expert’s judgment, the general practitioners’ or ED physicians’ opinion. Many authors emphasize the lack of consensus to define appropriateness of a NH resident’s hospitalization.
A large number of factors can influence the rate of hospitalization of the NH residents. Intrinsic factors like sociodemographic and resident’s health characteristics (poor general condition (7), additional co-morbidities (14), higher level of dependency (15), cognitive impairment (16), neuropsychiatric symptoms (17) and extrinsic factors associated with the NH (dearth of health care professionals trained to evaluate and manage geriatric population, easy access on-site to a primary care clinician or an urgent laboratory result (18, 19)) or the staff and the families (lack of education or collegial decisions about the realistic goal for care and advance care planning (6)).
Most of the factors associated to inappropriate or potentially avoidable hospitalizations have been generally found upstream the ED’s admission and efficient interventions targeted actions in NH (6, 20). A recent systematic review showed that the geographic variations in the rates of inappropriate or potentially avoidable hospitalizations were driven by the primary care quality and secondary care access (21).
These results emphasize the need to study and analyze the nature of transfers to ED of NH residents. To our knowledge, only few studies described the residents’ entire transfer, including events in NH leading up to the transfer, the ED admission and their return to NH (22, 23).
The aim of this pilot study is to determine the rate of inappropriate and potentially avoidable transfers of NH residents to ED and to identify the factors associated with them. We also try to describe the resident’s characteristics from the NH to the ED and back to the NH. Our hypothesis is that a large number of transfers to the ED are inappropriate, related to NH’s organizational factors and associated with a significant functional decline.
Materials and methods
This pilot study was conducted by the Toulouse Gerontopole and the University Department of Family Medicine in association with the Department of Epidemiology (Unity of Research INSERM, UMR 1027).
Data collection
During one full week (7days/7days, 24 hours/24 hours) all patients transferred from NH to the two ED of the Toulouse University Hospital (Purpan and Rangueil) were included in the study. Two fellows in family medicine collected data on-site in both ED. By a phone call to NH in the day of transfer, were collected residents’ characteristics seven day before the transfer to ED medical history, level of dependency according to the Activities of Daily Living’s Scale (ADL), pain, behavioral disturbances, fever,… and the circumstances around the transfer (who decided the transfer, accessibility to the general practitioner’s advice, medical protocol for emergency conditions). The general practitioner (GP) or the health professional that decided the transfer to the ED was also interviewed by phone on his/her knowledge about the patient, reasons of his/her decision to transfer the patient to the ED.
During the patient’s admission to the ED, data were collected from the patient’s medical record (reason of admission, accessibility to patient’s data, medical history, treatments or anticipated prescriptions, time between patient’s admission and his support by a physician). The ED physicians who examined the patients were also interviewed on their opinion about the reasons of the patients’ transfer to the ED in absence of criteria of gravity and their perception about the appropriateness of the transfer.
Seven days after the return of residents to their NH, a fellow in family medicine phoned the NH’s referent nurse to know the circumstances around the return (delay to see the GP after returning to the NH, presence of prescriptions and supervisory guidance, feasibility of the management of the somatic condition in the NH). The general practitioner or the health professional that decided the transfer to the ED was also interviewed (opinion about appropriateness of his/her decision to transfer the resident to the ED).
Moreover, the incidence of residents’ functional decline (loss of 0.5 points or more in the ADL score) and diagnosis of dementia between before the transfer to ED and after the return in NH was calculated.
Defining inappropriate and potentially avoidable resident’s transfers
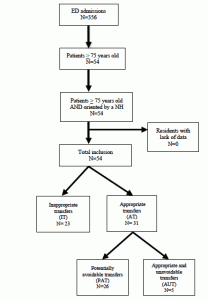
Three months after the inclusion, an expert panel of geriatricians and emergency physicians determined if the residents’ transfers to ED were inappropriate or potentially avoidable (Figure 1).
Inappropriate Transfer (IT) to ED is a clinical situation that could be managed by other means than transfer to ED without loss of opportunity for the resident. In our study IT to ED was defined in the FINE pilot study as “the absence of somatic and psychiatric emergency conditions” and/or “palliative care known before decision to transfer” and/or “the presence of advance directives of non-hospitalization in the resident’s medical chart”. If none of these criteria was present, the transfer to ED was appropriate.
In a second time, among the Appropriate Transfers (AT) to ED, the group of experts had to consider which transfers to ED were potentially avoidable. Potentially avoidable transfers (PAT) to ED are due to potentially avoidable conditions by appropriate care upstream the acute events, such as vaccination or better management of chronic diseases. The PAT to ED were defined by referring to the Ambulatory Care Sensitive Conditions (ACSC-9) list. However, as the ACSC is not specifically dedicated for ED transfer of NH resident, the list was completed by conditions frequently reported in NH residents and which were potentially avoidable (fall, fracture, iatrogenic drug effect, inadequate treatment, suboptimal palliative treatment).
Finally when a transfer to ED was neither an IT nor a PAT, it was considered as an Appropriate and Unavoidable Transfer (AUT).
In order to define the factors associated with the IT or PAT to ED, four groups were compared. The group IT was compared to the group AT and the group PAT was compared to the group AUT (Figure 2).
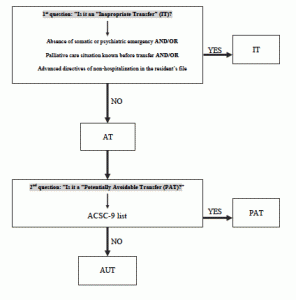
Figure 2
Procedure used to screen inappropriate, appropriate, potentially avoidable, and appropriate and unavoidable residents’ transfers to ED
IT = Inappropriate Transfer; AT = Appropriate Transfer; PAT= Potentially Avoidable Transfer; AUT= Appropriate and Unavoidable Transfer »
Statistical analysis
The statistical analysis of the factors associated to the IT and PAT was performed by STATA® software package (StataCorp LP, College station, TX, USA, eleven version). The continuous variables were expressed in mean and standard deviation. The mean comparison was performed with the Student’s t-test and the Wilcoxon rank sum test if the distribution was not normal. The categorical variables were expressed in number and frequencies. The Chi2 test « χ2 » was used to compare categorical variables and the Ficher test, if the frequency was lower than 5. The significant threshold was five percent. In this pilot study, the results with a significant threshold lower than 0.20 have been discussed.
Results
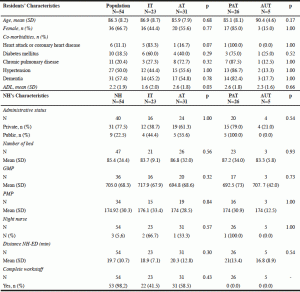
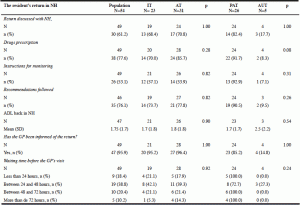
During one week, from 3 to 9 December 2012, 54 residents from NH were included in the both ED of the Toulouse University Hospital (34 in Purpan and 20 in Rangueil ED). Their mean age was 86.3 (±8.2) years and the majority (66.7%) of the population was women (n=36) (Table 1).
ADL, Activities of Daily Living scale (score from 0 to 6: 0=totally dependent, 6= fully autonomous, a total score got by the addition of the items walking, washing yourself, eating, going to the toilet, continence, getting dressed ‘scores); AT, Appropriate Transfer; AUT, Appropriate and Unavoidable Transfer; ED, Emergency Department; GMP, Gir Moyen Pondéré [reflects the load of the residents’ dependency evaluated on the AGGIR score, French scale to determine residents’ dependency, more the GMP score is high (>700), more dependent are the residents]; IT, Inappropriate Transfer; NH, Nursing Home; PAT: Potentially Avoidable Transfer; PMP, Pathos Moyen Pondéré [measures the level of benefits to support medical care in NH, more the PMP score is high (>150), more the level of the level of benefits to support medical care is high]; SD, standard deviation.
According to experts’ panel judgment, 43% (23/54) of transfers were qualified “Inappropriate (IT)” and 57% (31/54) “Appropriate (AT)”. Among the 31 transfers qualified as “Appropriate”, 84% (26/31) were judged “Potentially avoidable (PAT)” and 16% (5/31) “Appropriate and Unavoidable (AUT)” (Figure 1). Among the 54 residents, the most frequent potentially avoidable disorders were “iatrogenic drug effect” (n=24, 44%), “falls” (n=19, 35%) and “inadequate treatment” (n=8, 15%).
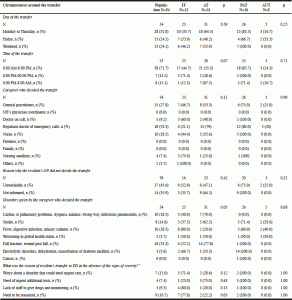
Conditions of the transfer in Nursing Homes (Table 2)
As reported in the table 2, most residents were transferred to ED from Monday to Thursday from 8:00 to 8:00 p.m. In most of cases (33%), the regulator doctor of the emergency calls decided to transfer the resident, following by the GP (28%) and the nurse (18%). The main reason for transferring the resident to ED without the GP’s advice was the impossibility to contact the GP in 44% of cases. The main cause of resident’s transfer to ED was “fall, post-fall injury or suspicion of fracture” (33%). A nurse was present during the night in only three NH among all the NH that sent the 54 residents included. There was a medical protocol for emergency conditions in about half of the cases (48%) and it was mostly applied (91%).
AT, Appropriate Transfer; AUT, Appropriate and Unavoidable Transfer; GP, General Practitioner; IT, Inappropriate Transfer; NH, Nursing Home; PAT, Potentially Avoidable Transfer.
Resident’s admission at Emergency Departments (Table 3)
In ED, the access to the residents’ history of disorders and co-morbidities was possible in one out of two cases. Most of the information which had to be sought was the cognitive status (54%) and the level of dependence (39%). According to ED physician’s opinion, if resident was transferred without signs of severity, the main reasons of the transfer were “to be reassured about signs of severity” and “the need of urgent additional tests”. According to ED physician’s perception, 77% of transfers were “Inappropriate” and 37% were “Potentially Avoidable”.
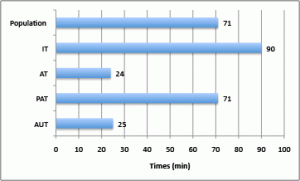
After the ED’s nurse evaluation of the severity signs at the admission, the mean waiting time between admission and the ED physician’s visit ranged from 25 min for an AUT to 90 min for an IT. For the PAT, this time was 72 min. Residents from NH had to wait on overage 72 min before the ED physician’s visit (Figure 3). In one out of two cases, residents returned in NH after ED in the 24 hours.
AT, Appropriate Transfer; AUT, Appropriate and Unavoidable Transfer; ED, Emergency Department; GP, General Practitioner; IT, Inappropriate Transfer; NH, Nursing Home; PAT, Potentially Avoidable Transfer.
IT = Inappropriate Transfer; AT = Appropriate Transfer; PAT= Potentially Avoidable Transfer; AUT= Appropriate and Unavoidable Transfer »
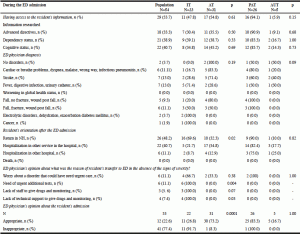
Back to the NH (Table 4)
NH agreement about the residents’ return was discussed in 62% of cases. The NH received from ED a prescription in 38 cases (77.6%) and instructions for monitoring in 26 cases (53.1%). Staff in NH followed recommendations in 76.1% of cases. The GP was informed about the resident’s return in NH in 95.9% of cases. One resident out of two was examined by the GP within 48 hours after his return to NH.
Moreover, before the transfer to ED and after the return in NH, there was a significant increase in diagnosis of dementia (from 52% of residents before the transfer to ED to 75% of residents back in the NH, p=0.01) and a non-significant decline in residents’ functional status (from a mean ADL score of 1.7±1.7 before the transfer to ED to a mean ADL score of 2.1±1.7, p=0.05).
ADL, Activities of Daily Living; AT, Appropriate Transfer; AUT, Appropriate and Unavoidable Transfer; ED, Emergency Department; GP, General Practitioner; IT, Inappropriate Transfer; NH, Nursing Home; PAT, Potentially Avoidable Transfer.
Inappropriate versus Appropriate transfers to ED
There is no difference between two groups concerning age, sex, co-morbidities, and characteristics of NH (Table 1). The IT were more frequent when residents had less autonomy on the ADL scale (p=0.03) (Table 1) and when the answer to the question “Why the resident was transferred without signs of severity?” was “need to be reassured” (p=0.03) (Table 2).
According to table 3, the IT were more frequent when residents returned in NH after ED (p=0.02). When ED physician’s opinion about “What was the reason of resident’s transfer to ED in the absence of the signs of severity?” was “the need of urgent additional tests”, the IT were more frequent (p=10-4). When ED physician qualified the resident’s transfer to ED of “Inappropriate”, that was mostly an IT according to expert’s group (p=10-4).
At the limit of the significance level (p<0.2), more IT seemed to be associated with a transfer between 8:00 PM to 00:00 AM (p=0.07), and with the causes of transfer “digestive infection, hyperthermia and urinary catheter” (p=0.05) (Table 2). When ED physician’s opinion about “What was the reason of resident’s transfer to ED in the absence of the signs of severity?” was “the lack of technical capacities” (p=0.03) or “the lack of human resources” (p=0.07), IT were more frequent than AT to ED according to expert’s group (Table 3).
Potentially Avoidable versus Appropriate and Unavoidable transfers to ED
There is no difference between two groups concerning age, sex, co-morbidities, and characteristics of NH (Table 1). At the limit of the significance level (p<0.2), the causes of transfer “electrolyte disorders, dehydration and exacerbation of diabetes mellitus” were associated with more PAT (p=0.08) (Table 3).
Discussion
In our pilot study, 43% of transfers were qualified as “IT” and 57% as “AT”. Among the AT, 84% were judged as “PAT” and only 16% as “AUT” (45% and 9% of the whole population respectively).
The prevalence of IT (43%) and PAT (45%) to ED reported in our study is within the large range reported in the literature (2, 11, 13). Ouslander et al. (11) found that 67% of the hospitalizations were “Potentially avoidable”. In this study, the authors did not targeted ED admission and did not distinguished inappropriate or potentially avoidable transfers to the hospital. Moreover, a panel expert determined the appropriateness of hospitalizations by using a structured implicit record review (SIR). The lack of consensus to define and to attest inappropriate or potentially avoidable transfers to ED explains these heterogeneous results. It may also be explained by the various health care organizations of the different countries. However, inappropriate or potentially avoidable transfers to ED seem to be close to 50%. Finally, appropriate and unavoidable resident transfers from NH occurs one out of ten admissions in ED. These results should increase the interest on the subject.
Despite a small sample size in our pilot study, some factors were turned out to be associated with IT or PAT. They were mostly located within the NH, before the ED admission.
In our study, the level of dependency (ADL score) was significantly associated with IT. This result is in coherence with literature’s data. Among 8,815 beneficiaries from the Medicare Current Beneficiary Survey (MCBS), Schüssler et al. (15) found that more dependent were people more likely they were to experiment a “potentially avoidable hospitalization”. It seems that residents with a higher dependence are a more vulnerable population in regards to inappropriate transfers to ED.
Moreover, in our study, we noted a non-significant increase of disability on the ADL scale for residents back in the NH. Sourdet al. (24) reported in a population of 503 patients, aged 75 years and older, with a length of stay of minimum 2 days in hospital, an incidence of 18.1% (91 cases) of functional decline (loss of 0.5 points or more in the ADL score) between the time of hospital admission and discharge. Among these cases, 60 cases of iatrogenic disability (11.9%), related to health care management issues and the hospital environment were identified. This result supports the idea that the alternatives to hospitalization of NH’s resident should be developed.
Some intrinsic factors like co-morbidities (14) or cognitive status (16) were fairly associated with potentially avoidable hospitalization in a few studies. However, these residents’ characteristics were not found in our study.
Regarding the extrinsic factors identified in our study to be associated to IT, two trends stood out: the health professional who the transfer decision and the condition of access to primary care in NH.
In our study, in 33% of cases, the regulator doctor of the emergency calls made the decision to transfer the residents. More IT seemed to be associated with a transfer between 8:00 PM to 00:00 AM. It means that many acute events can occur in out-of-hours of the GP (25). Many of residents in NH have a complex and long medical story. However, it is often a physician of emergency medical services, without any knowledge of patient’s medical history, who has to make the decision of patient’s transfer in a short time (26-28).
In addition to a small sample size, there are some other limitations in our study. We didn’t have any information to conclude about the adequacy between the number of staff and the care needed by the acute event. But we can argue that during an acute event, the needs of staff is growing to provide treatment and monitoring to the resident who feels ill and to manage the needs of all the others residents. We cannot also conclude about the qualitative aspect of the care given. Other authors point the lack of staff in NH with a specific expertise and training in the management of geriatric persons and syndromes (29).
In our study, the causes of transfer “electrolyte disorder, dehydration and exacerbation of diabetes mellitus” showed a trend to be associated with more IT. The most frequent “preventable disorders” were “iatrogenic medication” (44%), “falls” (35%) and “without appropriate treatment” (15%). By extension, these results lead to two important observations. In one hand, the resident’s disorders with IT do not finally require the ED’s level of care. In the other hand, a geriatric expertise, upstream and when needed, and some simple tests like a standard laboratory result, could be helpful. By targeting 3 nursing homes that had the highest number of multiple admissions, Liske et al. (30) showed that geriatrician input into NH, had a significant impact on transfer from NH to ED (Χ2= 6.261, p < 0.05). These observations are in agreement with previous conclusions: the main factor of inappropriate transfers to ED is the primary care quality and secondary care access6.
In our study, the ED physician’s opinion was pertinent. When ED physician’s opinion about the transfer was “Inappropriate”, that was an inappropriate transfer most of the time (p=10-4). Thus, they seemed to have a good knowledge about the NH difficulties, in contrary to the conclusion of a Canadian study where the ED staff is not familiar with the NH resident’s care (22).
The time between admission by nurse and the ED physician’s clinical examination was variable. This time was more than three times longer for IT (90 min) comparing to AUT (25 min). Information about the residents’ medical history was sufficient in one out of two cases. We suggest that the time spent to search information could explain the length of time between the admission and the ED physician’s examination. This observation refers to the lack of pertinent information transmissions between physicians, NH and ED (22). This length of time could have also contributed to the discomfort of the most dependent residents and their global deterioration. At last, PAT were logically more frequent when residents returned in NH after ED (p=0,02).
In return to NH, there were indications for medication, treatment and monitoring, but only one out of two residents were examined by the GP in the 48 hours. Although we do not have any information about the residents’ need to be visited before 48 hours, this observation concerns again the primary care quality and secondary care access for residents in NH (6).
We used a statistical method to identify the factors associated to IT and PAT, in contrary to many others studies that used declarative method. But for identifying statistically significant factors associated with IT, we need a larger sample size. Residents should be included in a multi-center study and at several periods of the year. Other intrinsic factors should be taken into account like malnutrition and neuropsychiatric symptoms. Qualitative (evaluation of the practices in NH) and quantitative (number of GP or other specialists’ visits, number of readmission in ED) data about the care given upstream and during the acute event in the NH could be helpful. Furthermore, it would be interesting to estimate the economic impact of the costs associated to PAT compared to AT (transports, time spent for items of ADL score).
The lack of consensus to define and assess IT or PAT to ED contributes to the heterogeneity of the result. It may be some factors associated with IT or PAT from NH to ED but also from ED to medical units (needs of a geriatric evaluation or a hospitalization) or to NH (lack of information about human and technical resources in NH). The identification of these factors let us to develop efficient strategies in NH and ED to prevent the residents’ deterioration due to their transfer.
Conflict of Interest: All participating authors declare that they have no competing financial interests.
Ethical Standard: This text had been submitted to independent reviewers to reinforce the ethical standards that have been respected by the authors.
References
1. Rolland Y, Andrieu S, Crochard A Goni S, Hein C, Vellas B. Psychotropic drug consumption at admission an discharge of nursing home residents. J Am Med Dir Assoc 2012; 13: 407.
2. Saliba D, Kington R, Buchanan J, Bell R, Wang M, Lee M, et al. Appropriateness of the decision to transfer nursing facility residents to hospital. J Am Geriatr Soc 2000; 48:154–163.
3. Arendts G, Howard K. The interface between residential aged care and the emergency department: a systematic review. Age Ageing 2010; 39:306–12.
4. Wang HE, Shah MN, Allman RM, Kilgore M. Emergency department visits by nursing home residents in the United States. J Am Geriatr Soc 2011; 59:1864–72.
5. Grabowski DC, O’Malley AJ, Barhydt NR. The costs and potential savings associated with nursing home hospitalizations. Health Aff 2007; 26:1753– 1761.
6. Ouslander JG, Berenson RA. Reducing unnecessary hospitalizations of Nursing Home Residents. NEJM 2011; 365:1165-67.
7. Grabowski DC, Stewart KA, Broderick SM, Coots LA. Predictors of nursing home hospitalization: a review of the literature. Medical Care Research & Review 2008; 65:3–39.
8. Sari AB, Cracknell A, Sheldon TA. Incidence, preventability and consequences of adverse events in older people: results of a retrospective case-note review. Age Ageing 2008; 37:265-9.
9. Rothschild JM, Bates DW, Leape LL. Preventable medical injuries in older patients. Arch Intern Med 2000; 160: 2717-28.
10. Lafont C, Gérard S, Voisin T, Pahor M, Vellas B; Members of I.A.G.G./A.M.P.A Task Force. Reducing «iatrogenic disability» in the hospitalized frail elderly. J Nutr Health Aging. 2011; 15: 645-60.
11. Ouslander JG, Lamb G, Perloe M Givens JH, Kluge L, Rutland T, et al. Potentially avoidable hospitalizations of nursing home residents: frequency, causes, and costs J Am Geriatr Soc. 2010 Apr;58(4):627-35.
12. Ouslander JG , Maslow K. Geriatrics and the Triple Aim: Defining Preventable Hospitalizations in the Long-Term Care Population. J Am Geriatr Soc. 2012; 60:2313-8.
13. Finn J C, Flicker L, Mackenzie E. Interface between residential aged care facilities and a teaching hospital emergency department in Western Australia. MJA 2006; 184:432-435.
14. Payne RA, Abel GA, Guthrie B, Mercer SW. The effect of physical multimorbidity, mental health conditions and socioeconomic deprivation on unplanned admissions to hospital: a retrospective cohort study. CMAJ 2013; 185:E221-8.
15. Schüssler-Fiorenza Rose SM, Stineman MG, Pan Q, Bogner H, Kurichi JE, Streim JE, et al. Potentially Avoidable Hospitalizations amon People at Different Activity of Daily Living Limitation Stages. Health Serv Res. 2016 doi: 10.1111/1475-6773.12484.
16. Becker MA, Boaz TL, Andel R, Gum AM, Papadopoulos AS. Predictors of preventable nursing home hospitalizations: the role of mental disorders and dementia. Am J Geriatr Psychiatr 2010; 18:475-82.
17. Davydow DS1, Zivin K, Katon WJ, Pontone GM, Chwastiak L, Langa KM, et al. Neuropsychiatric Disorders and Potentially Preventable Hospitalizations in a Prospective Cohort Study of Older Americans. J Gen Intern Med. 2014; 29:1362-71.
18. Ashcraft AS, Champion JD. Nursing home resident symptomatology triggering transfer: avoiding unnecessary hospitalizations. Nurs Res Pract. 2012; 2012:495103.
19. Young Y, Barhydt NR, Broderick S, Colello AD, Hannan EL. Factors associated with potentially preventable hospitalization in nursing home residents in New York State: a survey of directors of nursing. J Am Geriatr Soc 2010; 58:901-7.
20. Van Loenen T, Van den Berg MJ, Westert GP. Organizational aspects of primary care related to avoidable hospitalization: a systematic review. Fam Pract. 2014; 31:502-16.
21. Busby J, Purdy S, Hollingworth W. A systematic review of the magnitude and cause of geographic variation in unplanned hospital admission rates and length of stay for ambulatory care sensitive conditions. BMC Health Services Research 2015; 15:324.
22. McCloskey RM, van den Hoonaard D. Nursing home residents in emergency departments: a Foucauldian analysis. J Adv Nurs. 2007; 59:186-94.
23. McCloskey RM. A Qualitative Study on the Transfer of Residents Between a Nursing Home and an Emergency Department J Am Geriatr Soc 2011; 59:717–724.
24. Sourdet S, Lafont C, Rolland Y, Nourhashemi F, Andrieu S, Vellas B. Preventable Iatrogenic Disability in Elderly Patients During Hospitalization. J Am Med Dir Assoc. 2015 Aug; 16:674-81.
25. Gruneir A, Bell CM, Bronskill SE. Frequency and pattern of emergency department visits by long-term care residents – a population based study. J Am Geriatr Soc 2010; 58:510-7.
26. Bellelli G, Frisoni GB, Barbisoni P, Boffelli S, Rozzini R, Trabucchi M. The management of adverse clinical events in nursing homes: a 1-year survey study. J Am Geriatr Soc 2001; 49:915-25.
27. Arendts G, Dickson C, Howard K, Quine S. Transfer from residential aged care to emergency departments: an analysis of patient outcomes. Intern Med J. 2012; 42:75-82.
28. Evans G. Factors influencing emergency hospital admissions from nursing and residential homes: positive results from a practice-based audit.J Eval Clin Pract. 2011;17:1045-9.
29. Hanger HC, Fletcher V, Sidwell A. Acute medical admissions for older people from residential care facilities: are they appropriate? N Z Med J. 2011; 124:24-32.
30. Lisk R, Yeong K, Nasi A, Baxter M, Mandal B, Nari R. Geriatrician input into nursing homes reduces emergency hospital admissions. Archives of Gerontology and Geriatrics 2012; 55:331–337.