O. Farrer1, A. Yaxley1, K. Walton2, R. Milte3, M. Miller1
1. Nutrition and Dietetics, Flinders University, GPO Box 2100 Adelaide, South Australia 5001, Australia; 2. School of Medicine, University of Wollongong, Northfields Avenue, Wollongong NSW 2522, Australia; 3. Rehabilitation, Aged and Extended Care, Flinders University, GPO Box 2100 Adelaide, South Australia 5001, Australia; NHMRC Cognitive Decline Partnership Centre, Sydney, NSW. Corresponding author: Prof Michelle Miller, Nutrition and Dietetics, Flinders University, GPO Box 2100 Adelaide, South Australia 5001, Michelle.miller@flinders.edu.au; Ph: +61 8 8204 5328; Fax +61 8 8204 6406
Jour Nursing Home Res 2017;3:50-53
Published online April 7, 2017, http://dx.doi.org/10.14283/jnhrs.2017.8
Abstract
Background: Historically, diabetic diets are typically limited in carbohydrate, energy and food choices and may limit overall oral intake in older adults with diabetes. Objective: This study aims to evaluate the extent to which Australian residential aged care facilities still offer a diabetic diet, the rationale for providing and composition of this diet, and with consideration for implications this may have for residents with diabetes. Design: A web-based survey about current food service practices, menu design and specifically about meal provision for residents with diabetes was emailed to participants. Participation was voluntary. Setting: Web based survey to Australian residential aged care facilities. Participants: 2075 food service managers or staff of similar responsibility within the organisation. Results: More than half of the respondents (n=121, 59%) still provide a diabetic diet because it has historically always been offered or as advised by their dietitian. Respondents frequently offered a menu comprising food restriction rather than the liberalised diet promoted by current recommendations. Conclusions: Findings from this study demonstrate that there is inconsistency in practices. Dietary restriction is still a feature of diabetes management which may increase risk of malnutrition and affect resident quality of life. There does appear to be a need for widely endorsed aged care specific guidelines for best practice.
Key words: Diabetic diet, food service, menu, residential aged care.
Introduction
Australia’s population is getting older, with approximately 14% of the population being over the age of 65 years and 1.9% over the age of 85years (1). Globally diabetes diagnosis is epidemic and as type 2 diabetes is more prevalent in the ageing population, which by 2050 is set to rise to 25% of the worlds’ population, this presents significant challenges to healthcare systems such as residential aged care (RAC) (2). Diabetes is mainly managed through diet and lifestyle interventions, supported by medication where needed (3) although there is debate as to the appropriate dietary approach for older adults with diabetes. Individualised dietary prescriptions are highly recommended (4) but how this is managed in an institutional food service system can vary.
Historically institutions like RAC have provided a diabetic diet largely based on healthy eating recommendations used in community setting. This diet would have likely included an energy restriction to promote healthy weight management and reflected a low fat, high fibre eating philosophy with emphasis on exclusion of foods with added sugar such as desserts, sweets and full sugar beverages. More recently it has been recognised that this style of diet (5) may promote malnutrition amongst aged care residents (6). This concern for malnutrition prompted a review of current practice by the American Diabetic Association (7), American Dietetic Association (8) and more recently an international document (2013) from the International Diabetes Federation (4) which all agreed that traditional diabetic diets offer no benefit in glycaemic management and are potentially overly restrictive.
Anecdotally it is known that changes in practice in response to the position statement and IDF guidelines has been received with mixed responses with some facilities continuing to offer a diabetic diet. However, the extent to which this is the case and the level of dietary restriction being imposed is hitherto unknown.
As part of a wider study examining the philosophy and experience of a diabetic diet in RAC; the aims of this study were to evaluate the extent to which a special diet for residents with diabetes is still being provided. Subsequently, for those institutions continuing to provide this diet we sought to understand more about the rationale and the composition of what is being provided and consider the implications this may have for older adults with diabetes.
Methods
This anonymous cross-sectional questionnaire was a two phase design to gather information from food service managers in Australian RAC. The initial phase involved piloting a web based questionnaire for ease of use and acceptability of question context and wording. The final questionnaire was approved by the Social and Behavioural ethics committee, for Flinders University and distributed to named aged care manager emails purchased from an Australian marketing agency with an invitation for the food service manager or other suitable person to complete.
Questionnaire Structure
The questionnaire was created on website host Survey Monkey® (Palo Alto, Calif, USA). The website provided a means to keep the responses confidential throughout the process. The questionnaire incorporated 25 questions specific to this study and was divided into four parts: demographics, the food service system, the menu and finally specific questions on special diets, particularly for diabetes management. An additional four conditional release questions were only revealed to those facilities indicating that they did provide a diabetic menu to probe the way in which these meals were ordered, the quantity of diabetes-specific meals prepared per day and a series of statements related to food options available or unavailable on the diabetic menu when compared to the standard menu.
In addition, both RAC who provide a therapeutic diabetic diet and those that did not, were asked for insight into the philosophy behind their practice. The questionnaire was delivered to 2075 valid personal email addresses for managers in Australian RAC. Data were retrieved from Survey Monkey® and analysed using IBM Statistics Package for the Social Sciences (SPSS) version 22. Descriptive statistics were used to describe the sample whereas chi square calculations were used to determine differences in responses to categorical variables between facilities that provide a diabetic diet and those that do not and also the provision of core food groups as provided in the current diabetic diet.
Results
Of the 2075 questionnaires sent out to RACF management emails, n= 205 were commenced and 201 were completed in full (9.8% response rate). Incomplete questionnaires provided answers to all sections other than the therapeutic diabetic diet composition questions and therefore have still been included for analysis of results. Data from non-responders other than the facility name and email address was not available and therefore not included in data analysis. General demographic results for responders are shown in Table 1 and divided by state and territory.
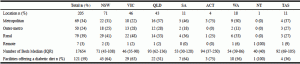
Table 1
Total respondent demographics by state and territory and n (%) facilities still providing a diabetic diet
Abbreviations: IQR = interquartile range; n = number.
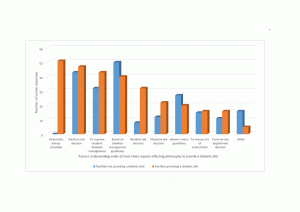
Figure 1
Contributing factors to RACF philosophy in providing a therapeutic diabetic diet vs decisions influential in not providing a diabetic diet for Australian residential aged care survey repondents
NB: Respondents were asked to tick as many responses from the categories as applied to their service
The Menu
More than half of the facilities (n =142; 69%) reported using menu guidelines or standards for review or design of the menu although none of the guidelines noted have diabetes specific guidance. Most frequently cited guidelines were generic dietitian (n=53; 26%) or aged care guidelines (n =19; 9%) or HACCP/Food safe standards (n =30; 15%). In addition a smaller number of facilities, (n=5; 2%) quoted using recommendations from an independent aged care consultancy company (www.oscarhospitality.com.au) and to a lesser extent (n=4; 2%) the ‘Best Practice Food and Nutrition Manual for Aged Care Facilities (9).
Diabetic Diet
A total of 121 (59%) RACF reported offering a special diet for diabetes management which was generally provided automatically on admission (n=65; 54%). In other cases the diet was available if prescribed by either the dietitian (n=20; 17%), the medical team (n=15; 12%) or requested by the resident or family (n=6; 5%). A further (n=4; 3%) respondents commented that their menu had been tailored to be suitable for all residents including those with diabetes and did not offer a separate ordering process but still identified as offering a ‘diabetic’ menu in the questionnaire responses.
Table 2 provides an overview of the meal exclusions and additions that occur in facilities providing a diabetic diet and how this compares to the facilities’ standard menu. One way chi square testing suggests a significant difference in provision of all core and discretionary food groups for a diabetic diet when compared to the standard facility menu and between facilities (p= <0.05, Table 2).
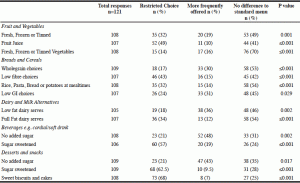
Table 2
Overview of typical food restrictions and additions that represent the current ‘diabetic diet’ as compared to the standard menu offered to all other residents in Australian
Abbreviations: n = number, GI = glycemic index
In particular the following known characteristics of a traditional institutional diabetic diet were explored:
Rice, pasta, potato or breads and cereals at mealtimes
Approximately a third of RACF reported limiting mealtime serves of starchy breads and cereals for residents with diabetes 32% (n=35), while 14% (n=15) reported offering them more regularly to residents with diabetes than those without.
No added sugar/low sugar diet
Residents with diabetes were more likely to be offered a restricted choice of sugar sweetened beverages (n=60; 57%) and more regularly offered a no sugar option (n=52; 48%) than those residents without diabetes. In addition, residents on a diabetic diet are less likely to be offered sweet biscuits and cakes (n=73; 68%) or desserts and condiments containing sugar (n=68; 62.5%). Fruit and fruit juice are also more likely to be restricted for residents with diabetes, n=35 (32%) and n=52 (49%) facilities respectively.
Low fat and calorie restricted diet
Residents on a diabetic diet are more likely to be offered low fat dairy serves 36% (n=38) or this is reported as a standard practice for all residents (n=48, 46%). Low calorie desserts 43% (n=47) and beverages 48% (n=52) are also offered more often to diabetic residents in respondent facilities with a therapeutic diabetic diet.
Philosophy for diabetes management
Figure 1 outlines the rationale provided by respondents for why a therapeutic diabetic diet was offered as compared to facilities that did not provide it. For facilities offering a diabetic diet the primary reason cited was it being historically always offered (n=51; 42%); and/or a dietitian led decision (n=47; 39%) which is believed to improve diabetes management (n=43; 36%) or in reference to diabetes guidelines (n=40; 33%). Conversely those facilities (n=80) that do not offer a therapeutic menu suggest this is also predominantly a dietitian led decision (n=43; 54%) in reference to diabetes guidelines (n=50; 63%) and for improved diabetes management (n=32; 40%).
Discussion
In the last two decades there has been significant discussion in the literature regarding liberalisation of dietary recommendations for all adults with diabetes (4). Subsequently, there has been concern for the continued use of the more restrictive style diabetic diet for management of older adults (4, 7, 8) in institutional care particularly as malnutrition is so prevalent in this setting.
The results from this study suggest that more than half of the survey respondents (59%) still offer a therapeutic diabetic diet such as this, to their residents. The decision to offer a separate therapeutic menu seems to be as a result of long held practices and perception of diabetes management from key personnel managing the menu design and unspecified menu guidelines.
Aged care guidelines which include information on nutrition (4, 8, 9) are available and although are non-specific in their recommendations, all consistently refer to there being no need for a separate diabetic diet or restriction of food items. However these guidelines are not mandated or widely promoted to health professionals or food service staff working in an aged care setting (10) which might also contribute to significant difference in practices between facilities.
Concern for continued use of a diabetic diet is that it has implications for the adequate dietary intakes of residents with diabetes, particularly if more aligned with historical carbohydrate and energy restrictions (11). Although the evidence for the alternative liberalised diet and diabetes management is weak (12) the restriction of core food groups such as fruit and breads and cereals, does not resemble best practice recommendations (13). The diabetic diets described in this study do still appear to be consistent with the theme of restriction particularly foods with added sugar, starchy carbohydrates and full fat items. The restriction of fruit, fruit juice, sweetened and starchy foods raises concern for adequate intake of vitamins, minerals, fibre and calories in the diet overall and in general, dietary restriction is proposed to increase risk of dissatisfaction with the diet, reduce oral intake and impact on quality of life (14, 15).
In summary, the findings of this study, although only an exploratory snapshot of what is occurring Australia wide, do support what is known anecdotally, that there is diversity in practice when it comes to food service and diabetes management in residential aged care. This study has provided insight into what residents are being offered and the philosophy for doing so. Going forward, it is clear that aged care specific menu guidelines that are endorsed Australia wide are needed to promote consistent practice and better nutrition outcomes for older adults with diabetes.
Conflict of Interest: The authors have no conflict of interest to declare.
Funding: Rachel Milte is supported by funding provided by the National Health and Medical Research Council (NHMRC) Partnership Centre on Dealing with Cognitive and Related Functional Decline in Older People (grant no. GNT9100000). The contents of the published materials are solely the responsibility of the Administering Institution, Flinders University, and the individual authors identified, and do not reflect the views of the NHMRC or any other Funding Bodies or the Funding Partners.
References
1. Australian Institute of Health and Welfare. Residential aged care in Australia 2010–11: a statistical overview Canberra: AIHW, 2012.
2. Knickman JR, Snell EK. The 2030 problem: caring for aging Baby Boomers. Health Services Research. 2002 2002/08//:849+.
3. The Royal Australian College of General Practitioners and Diabetes Australia. General practice management of type 2 diabetes – 2014-2015. Melbourne: 2014. .
4. International Diabetes Federation. Global Guideline for Managing Older People with Type 2 Diabetes IDF, Brussels, 2013.
5. Buckler DA, Kelber ST, Goodwin JS. The use of dietary restrictions in malnourished nursing-home patients. Journal of the American Geriatrics Society. 1994;42(10):1100-2.
6. Evidence based practice guidelines for the nutritional management of malnutrition in adult patients across the continuum of care. Nutrition & Dietetics. 2009;66:S1-S34.
7. American Diabetes Association. Nutrition Recommendations and Interventions for Diabetes: A position statement of the American Diabetes Association. Diabetes Care. 2008;31(Supplement 1):S61-S78.
8. Niedert K. ADA reports. Position of the American Dietetic Association: liberalization of the diet prescription improves quality of life for older adults in long-term care. Journal of the American Dietetic Association. 2005;105(12):1955-65.
9. Bartl R, Bunney C. Best practice food and nutrition manual for aged care facilities,. 2004.
10. Williams P. DAA. Scoping Project Literature Review: Development of nutrition and menu planning standards for residential aged care facilities in Australia and New Zealand.2012. 3/8/2016]. Available from: http://daa.asn.au/wp-content/uploads/2011/07/Scoping-Project-Literature-Review-Updated-Version-February-2012.pdf.
11. Darmon P, Kaiser MJ, Bauer JM, Sieber CC, Pichard C. Restrictive diets in the elderly: Never say never again? Clin Nutr 2010;29(2):170-4.
12. Farrer O, Yaxley A, Walton K, Healy E, Miller M. Systematic review of the evidence for a liberalized diet in the management of diabetes mellitus in older adults residing in aged care facilities. Diabetes Res Clin Pract. 2015;108(1):7-14.
13. Diabetes Outreach. Healthy eating & diabetes: A guide for aged care facilities. South Australia: 2012.
14. Coulston AM, Mandelbaum D, Reaven RM. Dietary management of nursing home residents with non-insulin-dependent diabetes mellitus. Am Journ of Clin Nutr. 1990;51(1):67-71.
15. Tariq S, Karcic E, Thomas D, Thomson K, Philpot C, Chapel D, et al. The use of a no-concentrated-sweets diet in the management of type 2 diabetes in nursing homes. J Am Diet Assoc. 2001;101(12):1463-6.
