D. Koder1, C. Kamath2
1. Specialist Mental Health Service for Older People, Sydney Local Health District; 2. Residential Business Lead, Sydney South East Residential Aged & Health Care, Uniting (NSW.ACT). Corresponding author: Deborah Koder, Specialist Mental Health Service for Older People, Sydney Local Health District, Level 7, King George V Building, Royal Prince Alfred Hospital, Missenden Road, Camperdown NSW 2050, Australia, Tel 61 02 9515-3158, Fax 61 02 9515-9801, Deborah.Koder@sswahs.nsw.gov.au
Abstract
Background: There is a dearth of research in the area of residential care for psychiatric elderly patients, despite their complex needs and the high prevalence rate of mental health problems in nursing homes. There are few accommodation alternatives specific to the needs of residents with both physical and mental health presentations. Objectives and method: A cross-sectional epidemiological study aimed to describe the characteristics of 84 residents from a residential facility caring for psychogeriatric patients via a retrospective file audit. Risk factors associated with residents being admitted to hospital were also of interest in order to assess severity of presentations and to direct resource planning. Data related to medical and psychiatric diagnoses, treatment, estimates of cognitive functioning, depression, verbal and physical aggressive behaviours, pain and falls risk were collected. Results: Based on descriptive statistics from the available data base of resident records, the profile of the average resident of this facility is aged 71, with a diagnosis of schizophrenia being treated via atypical antipsychotics, having at least one medical co-morbidity such as osteoarthritis and hypertension and has lived in the facility for six years. A significant relationship was noted between behavioural issues and both cognitive functioning and depression. There was a relatively low rate of psychiatric admission to hospital, with falls risk predicting admission to hospital, based on logistic regression analysis. Conclusion: Falls prevention programs are needed to positively impact on hospital admissions. The influence of poor cognition and depression on behavioural problems suggests there is a need to address cognitive limitations in future planning of environments and programs for older residents with mental health issues. Exercise programs may also improve mood, as well as mobility, in these residents. Attention is needed in reliably measuring aspects of care via subjective self-reports in this population.
Key words: Aged care facilities, aggression, hospital admissions, nursing homes, psychogeriatric.
Introduction
There has been a shift in providing care for psychiatric patients from State funded psychiatric institutions to more community based settings (1). As they age, the needs of mentally ill people change, with physical and cognitive co-morbidities necessitating unique care models. Research suggests while mentally ill residents in aged care facilities may be younger and have less functional impairment compared to those without chronic mental illness (2), this group display more challenging behaviours such as agitation and verbal abuse (3), often leading to hospitalization. It has been suggested that the nursing home environment may not meet the more complex needs of people with severe psychiatric symptoms (4) and that specialised facilities are required.
Background
Studies on mentally ill people living in residential care highlight the chronic nature of their illness with one study of assisted living (hostel) residents with schizophrenia citing the average length of illness being 21 years (5). Other characteristics of these residents include earlier onset, increased negative symptoms within their psychosis and increased cognitive impairment “made up of patients with the most severe and disabling disorders” (6) p.277. Whilst the impact of behavioural issues such as aggression on residents and staff has received much attention in the literature (7), with challenging behaviours significantly contributing to admissions to hospital (8), such research is typically in the context of dementia, as opposed to chronic mental illness. Similarly, there is research on hospital presentations of nursing home residents in general with an Italian study reporting an incidence of 11.6 percent of hospitalizations from nursing homes over one year (9), but study of the subset of residents with a psychiatric diagnosis is lacking (10).
Examination of psychiatric predictors in nursing home patients suggests that agitation and aggression are major causal factors leading to admission to psychiatric emergency centres. In an audit of 100 psychiatric emergency centre charts of nursing home patients, a study found a high degree of medical and psychiatric comorbidity, notably mood disorders. The most common diagnosis was dementia followed by schizophrenia, with vascular medical factors being the most prevalent medical predictor (11). Similar findings were reported in a study of 584 nursing homes in the United States: Younger age, being male, poor physical health, dementia and past drug use was associated with a threefold increased risk of psychiatric hospitalization (4). Mental health problems and their treatment can also influence falls risk, again leading to hospitalization and further disability. For example, depression was been found to be a predictor of falls in an Australian eleven year longitudinal study with investigators recommending screening for depression (12). However, falls are rarely studied within a mental health context (13). Given the high cost of in-patient care and how this would increase in proportion to patient complexity, identification and targeting of such predictors seems timely (14).
The present study
Uniting Annesley House is a home for 84 elderly residents living with mental illness located in Sydney, Australia. It is unique in being one of two aged care facilities, to date, specific to psychogeriatric residents within Australia. The residents of Uniting Annesley House are reviewed regularly by psychiatric registrars during their psychogeriatric rotation term. Residents are also seen by the community based Sydney Local Health District Specialist Mental Health Service for Older People (SMHSOP), should active case management be required for their psychiatric condition. The case management approach is the most commonly utilized variant of routine mental health clinician contact whereby case managers “undertake assessment, monitoring, planning advocacy; (their) function is clearly illness management and relapse prevention.” (15) p.1.
The first aim of the present research was to profile the current population of this aged care facility which has a predominantly chronic mental health population. Understanding the nature of the residents’ presentations and clinical needs was a major objective. Furthermore, an audit of residents also can aid future resource planning for the organizations involved.
The other study objective was to identify risk factors associated with inpatient admission of these residents. The study has the potential to better target treatment and community management by identifying influences on illness severity, as defined by need for hospital admission. By addressing such influences, such admissions may be able to be prevented thus improving outcomes for residents and promoting efficient inpatient bed use.
Methods
Participants and data collection
This cross-sectional epidemiological study design consisted of a retrospective file audit of all residents. The records were analysed and coded to identify which residents had been admitted to a psychiatric facility or general hospital within the Sydney Local Health District within a two-year period (2013-2014: a time period corresponding to the availability of reliable electronic data). All resident data of interest were coded within categories such as ICD-10 medical diagnosis (16), ICD-10 psychiatric diagnosis (16), type of psychotropic medication- including antipsychotic generation (17), number of admissions to psychiatric and general hospital facilities, age, gender and whether the resident was an active community mental health client (as defined by having an allocated case manager from the SMHSOP team at the time of data collection). Diagnoses were based on clinical assessment and/or diagnosis following admission to hospital where available. Other formal scales and monitoring tools were amongst those utilized within the current Australian government mandated Aged Care Funding Instrument (18). The Aged Care Funding Instrument (ACFI) has been the means of assessing the needs of residents within Australian residential aged care facilities and allocating government funding dependent on level of care needs since 2008. The Uniting Annesley House deputy director of nursing completes these scale ratings and there were two individuals in this position over the two year period of the present study. Cognitive skills were measured by the Psychogeriatric Assessment Scales (PAS)-Cognitive Impairment Scale (19). High scores indicate more cognitive impairment with cut-offs identifying eighty percent of cases of dementia being cited as 5; (19). Depression was measured by the Cornell Scale for Depression in Dementia (20), with a cut-off of 9 indicating the presence of depressive symptomatology. Behavioural issues were measured via adding the verbal and physical behaviours measure of the ACFI to form a total of the number of aggressive behaviours recorded every hour over a seven day period (21). The other two formal assessments where data was reliably available involved the assessment of pain (22) and falls risk (23, 24). The Brief Pain Inventory (22) examines a range of pain indices ranging from describing pain to pain management strategies. Annesley ratings required staff to ask residents to rate their average level of pain on a scale of 1 to 10 across the ratings period (in the last week) where 1 indicated slight pain, 4-6 was moderate pain, 7-9 indicated sharp pain, 10 was the worst pain. The falls risk screen was developed by the visiting physiotherapist at Annesley House. It is based on the Victorian National Ageing Institute assessment instrument-the Falls Risk Assessment-Residential Care, and contains 19 risk factors associated with falls, with a score over 10 indicating high falls risk. Items include history of falls, transfer, balance, sensory loss, nutrition and confusion (23). The items on the screen have been associated with risks identified in the literature on falls in residents of residential care facilities, such as continence and polypharmacy (24).
Residents were not actively recruited as the project involved a medical record audit.
Analysis
Data were subjected to descriptive analysis, between groups analysis of variance and direct logistic regression analysis to examine relationships between variables and predictors of admission to hospital. The SPSS version 23 statistical analysis package was used for analysis, with statistical significance values set at p < 0.01 or less. Whether a resident was admitted to hospital (either general or psychiatric) was the dependent variable for the regression analysis, with age, gender, cognition (PAS score), pain, falls risk screen score, depression (Cornell score) and behaviours (total number of aggressive behaviours in a seven day period) as independent variables. These variables were chosen both on the basis of being identified predictors in past research and the availability of reliable data.
Results
Resident Profile
Demographics
The resident population comprised of 54.8% males and 45.2 % females. Ages of residents were wide ranging (57 to 84 years of age) with the average age being 71. Similarly there was a wide variation in length of stay of residents (6 months to 25 years), with the average period of living at Uniting Annesley House being 6 years (Table 1).
Diagnoses
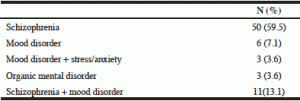
In terms of diagnosis, the resident population of Uniting Annesely House was primarily psychiatric, with schizophrenia as the main diagnosis (Table 2). Specifically, 81% of the sample had at least one psychiatric diagnosis with the most prevalent primary diagnosis being schizophrenia (59.5%). Depression featured as a diagnosis in 23.8% of residents. Co-morbid schizophrenia and mood disorder comprised 13.1% of the sample.
Multiple physical co-morbidities occurred within the resident population (84 listed in the sample), reflecting the complexity of residents’ needs. 81% of residents had a medical co-morbid condition. 29 % had three or more physical diagnoses with hypertension (21.4% of all physical diagnoses) and osteoarthritis (15.4% of all physical diagnoses) being the most common co-morbidities
Physical and psychiatric independent variable characteristics
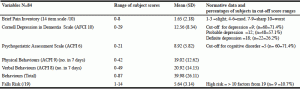
Table 3 indicated low ratings of pain amongst Annesley residents, with pain rated on average as “slight”. Overall falls risk scores were moderate with nearly 11% of the sample rated as high risk, based on falls risk score. Individual risk factor ratings were unavailable. Depression ratings were high with an average score of 12 indicating clinical levels of depression. Over 70% of the sample met ACFI cut-off criteria for depression. The population appeared to have a significant degree of cognitive impairment, based on the PAS mean of nearly 9 and 71 % of residents reaching the cut-off for having a cognitive disorder. There was an average of 21 verbal and 19 physical behaviours per resident noted across a seven day period. This suggests a high degree of behavioural issues within Annesley, with 40 noted behaviours per week on average.
Treatments
28.6% of the sample was receiving SMHSOP community services in the form of case management at the time of the study (Table 1). Case managers provided assessment of residents, together with ongoing monitoring and review of specialist mental health interventions.
In regard to anti-psychotic treatment, 67.5% of the sample was prescribed anti-psychotic medication.
Of these: 16.1% were on typical antipsychotics (for example, fluphenazine, haloperidol), with 83.9% prescribed atypical antipsychotics (for example, quetiapine, risperidone, olanzapine).
21% of the sample was prescribed antidepressant medication with 12% using hypnotics specifically for sleep.
All hospital admissions: 43% were admitted to either a general or psychiatric hospital in a two-year period with only 16.7 % of the total sample being admitted to the psychogeriatric unit. Half the residents with a psychiatric admission were being case managed by a SMHSOP community team member. Half of this psychiatric admission sample was male with the average age being 69. 71.4 % of this sample had a diagnosis of schizophrenia. Three residents had two or more psychiatric admissions over the two year period (one resident being admitted four times), none of whom were SMHSOP clients.
The number of total admissions in the past two years ranged from none to six per resident, with the average number being one admission (Table 1).
8.3% of residents were admitted due to aggression secondary to psychosis; 15.4% were admitted for other reasons that also included aggression secondary to psychosis. 6% were admitted following a fall. 18% were admitted for other reasons that included a fall.
Relationships between variables
Correlations
Relationships between variables were investigated through nonparametric Spearman’s rho correlations due to violation of linearity. Medium to strong associations were found between the number of hospital admissions and falls risk score (0.43). Significant relationships were also found concerning the total score for measures of challenging behaviour: a large correlation with both the Cornell Depression Scale score (0.50 or sharing 25 percent of the variance), and the score on the measure of cognition (0.54 or 29.16 percent shared variance with the PAS). There were no correlations reaching the 0.01 significance level involving any demographic measure. Other than number of admissions in total, there were no significant correlations involving whether a resident had been a psychiatric inpatient.
Influences on admissions to hospital (psychiatric and general)
Direct logistic regression analysis was also performed on group (admitted to hospital, not admitted to hospital) as the outcome variable, with age, gender, brief pain inventory score, depression score (Cornell), cognition (PAS), total number of behaviours and falls risk screen score as predictors. Assumptions regarding multicollinearity were not violated, based on tolerance and VIF factor diagnostics. A test of the model on 84 cases suggested that these predictors were statistically reliable in distinguishing between residents who were admitted to hospital within the two year period and residents who were not admitted ( χ2 (7, N=84) =22.64 p < 0.002). Between 23.6 and 31.7 % of the variance in admission status was explained by this set of predictor variables. The model correctly classified 71.4 % of cases. Only falls risk score (Exp (B) = 1.364) made a unique statistically significant contribution to the model, based on the Wald criteria. Patients who were admitted to hospital were nearly one and a half times more likely to have a fall.
Subsequent analysis was performed to examine the impact of type of antipsychotic on falls as measured by the falls risk scale. A one way between groups analysis of variance failed to indicate a significant effect for typical versus atypical antipsychotics and falls (F= 3.072,80; p<0.52). Post hoc comparisons were performed using the Tukey Honestly Significant Different test between the mean score for falls risk of residents not prescribed any antipsychotic medication (M = 6.78, SD = 3.238) and those prescribed atypical antipsychotics (M= 4.96 SD= 3.064; p < .05). The effect size, or actual difference in mean scores between these two groups, was small, with Eta Squared = 0.035.
Discussion
One of the main goals of this research was to examine influences on hospital admissions. Despite high psychiatric need, Uniting Annesley House residents are not typically presenting to psychiatric inpatient units. Nearly 30 % of Annesley residents were being case managed by mental health community services at the time of the study, yet half of admissions to the psychiatric inpatient unit were not clients of the community service. There is the potential for further lowering this admission rate by increasing community involvement, especially in those residents with two or more psychiatric admissions, none of whom were being seen by a SMHSOP clinician. Community case management services are well placed for timely identification of potential causes of admission to hospital such as delirium or early signs of psychosis. Medication compliance forms a significant part of a case manager’s functions which also impacts positively on psychiatric stability. The development and maintenance of a therapeutic relationship cannot be underestimated in terms of benefits to resident quality of life. The relatively higher rate of psychiatric admissions for residents who are not case managed suggests that a co-operative partnership between community mental health services and residential facilities has potential as an effective service delivery model.
However, around 43% of Uniting Annesely House residents presented to hospital for admission within a two year period, twice the comparative rate reported elsewhere (9). The most significant predictor of admission to hospital was falls risk score, suggesting that identified risk factors may not be the focus of management within the nursing home environment, despite the high degree of physical co-morbidities indicating a frail population. The admissions were predominantly linked to falls and aggression associated with exacerbation of psychosis. The latter is essentially a mental health problem that appears to be managed within the emergency department general hospital setting. Further analysis of the exact circumstances leading to these admissions (for example, bed shortages) may illuminate more appropriate alternatives to a busy emergency department for managing aggression secondary to psychosis.
Results suggested a high association between behavioural problems and both depression and cognitive dysfunction. Factoring in cognitive impairment into resource and treatment planning for this unique group may have a positive impact on challenging behaviours, particularly aggression. Poor cognitive functioning tends to be associated clinically with dementia, yet this was not a major diagnostic category, based on diagnostic criteria obtained from medical records. This is at odds with current cognitive functioning results on the PAS which indicated a large number of low functioning residents based on the cognitive screen cut-off (71.4 %). Here, poor cognitive functioning may well have been associated with the residents’ psychosis, as opposed to being a separate organic disorder per se. Another explanation may be that cognition is not being specifically targeted in assessments of residents, giving rise to a recommendation that cognitive screens be part of psychogeriatric assessment, if not already, and that clinicians be mindful of organic, as well as psychiatric, diagnoses. The measure of cognition may not be a reliable indicator of cognitive functioning, particularly in the domain of executive functioning which is most often associated with falls risk (25).
Falls risk also needs to be addressed further, given the lack of influence on type of antipsychotic medication on falls scores, suggesting falls are not related to type of antipsychotic use in the present study, a finding congruent with previous research on falls in older adults (26). The associated risk factor here may in fact lie in the cognitive domain and further research is needed in extrapolating specific falls risk factors from global risk assessments. Exercise based interventions may benefit this group, as it has been recommended for both poor cognitive functioning and depressed residents (13).
The prevalence of depression within the present sample was significant with over half of residents having Cornell scores of over 12 (probable depression). This sample has a much higher prevalence of depression compared to another Australian study of depression in nursing homes where
23% of all residents had depression based on the Cornell (27). Although the comparatively high number of residents with depression is to be expected in this psychogeriatric sample, it still underscores the need for staff training in identifying and managing depression. Issues have been raised regarding the use of the Cornell Depression Scale in Dementia in aged care facilities with little clinical follow up following administration of the screening tool (28).
Pain, age, and length of stay at Uniting Annesley House were not related to either psychiatric or general hospital admission, or other physical or behaviour problem variables. This is in contrast to other research examining predictors of hospitalization that report an association between psychiatric admission, age and gender (4). Pain scores on the Brief Pain Inventory were generally very low for an elderly population, compared to pain prevalence in nursing homes reported as being between sixty to seventy percent (29). This suggests underreporting of pain, especially given that osteoporosis was a co-morbidity in this sample. Alternatively, residents may have had difficulty identifying pain and rating it on a scale, especially for those with cognitive impairment. This raises questions regarding the reliability and validity of such self-report measures in settings with frail psychiatric patients, especially when facility funding can be reliant on scores. Similarly, the Aged Care Funding Instrument tool for measuring verbal and physical behaviours is reliant on staff observations and reliable recordings. These measures are pre-determined and the present study is carried out in its natural setting. Hence whilst a limitation of the present study is the reliability of measures, it remains representative of the industry and is a cause for concern.
Other limitations relate to the single site studied, limiting generalizability. The features of the Facility in terms of staffing ratios and experience were not examined due to the variability of these facility factors over the two year period. There is also very limited data available in regard to history of psychiatric illness, including duration of antipsychotic treatment, a predictor of falls risk based on previous research (26). Whilst previous work had been successful in studying psychiatric admissions, the present study examined all hospital admissions. This was due to the number of admissions with causal behavioural issues such as aggression being seen in general hospitals, via emergency. Details regarding the length of stay and factors relating to transfer to general hospital or psychiatric hospital would also be of value. Further research needs to target presentations to emergency departments and factors that promote treatment in a psychiatric facility.
Conclusion
Based on the present findings, there is a need to focus on resource funding and planning in the areas of falls, depression and cognitive frailty. Providing residents with a cognitively supportive physical environment appears essential in avoiding behavioural problems, and this has been addressed in the literature on management of dementia (for a review see (30)). There may be an underestimation regarding the extent of cognitive disability in residents with schizophrenia and depression and cognitive screening involving executive functions of each resident is essential. The results of such screens would add to targeting interventions in managing challenging behaviours such as aggression in psychotic patients. Development and evaluation of a falls prevention program specific to psychiatric populations would be another worthwhile outcome from the present findings, having the potential to positively impact on resident quality of life, including improved mood and decreasing hospital admissions.
The present study highlighted a low rate of admission to psychiatric hospitals. This suggests that a residential care model that specifically address the mental health needs of residents can have a positive impact on individual residents, as well as influencing broader health service usage. However the high rate of admission in general underscores the complexity of such patients where both physical and mental health needs require management in order to maximize functioning and prevent ongoing disability.
Relevance for clinical practice
Exploration of resident characteristics and treatment patterns in facilities providing accommodation and care for older people with mental illness can help accurately target care improvements within these unique settings. Furthermore, there is also the potential for this data to provide direction for planning residential services for a clinical population likely to increase in the future, given current ageing demographic projections. The present study indicates that paying attention to falls risk factors, incorporating design features that take into account poor cognition and developing programs to target low mood as important in the care of older people in psychogeriatric care facilities.
Acknowledgments: The authors acknowledge the staff and residents of Uniting Annesely House for their support with this project. The authors also acknowledge the feedback of Dr Sue Pearson, University of Tasmania and Fleur Hourihan, Uniting (NSW.ACT), regarding the interpretation of research. The authors would also like to thank Professor John Snowden and Dr Nirenjen St George from the Concord Centre of Mental Health, Sydney, Australia, for their helpful comments during the revision of this manuscript.
Funding: No financial support was received during this project.
Conflict of interest: There are no conflicts of interest.
Ethical Standard: This project received ethical approval from the Sydney Local Health District ethics review committee (Royal Prince Alfred Hospital zone).
References
1. NSW Mental Health Commission 1983. Inquiry into health services for the psychiatrically ill and developmentally disabled part 4. Services for the disturbed and confused elderly and the future role of state nursing homes. http://nswmentalhealthcommission.com.au/node/1521 Accessed 12 November 2015
2. Phillips C, Spry K. Characteristics and care of U.S. nursing home residents with a history of chronic mental illness. Can J Aging 2000; 19 Supp. 2: 1-17.
3. Fitz D, Mallya A. Discontinuation of a psychogeriatric program for nursing home residents: psychotropic medication changes and behavioural reactions. J Appl Geront 1992; 11: 50-63.
4. Becker M, Andel R, Boaz T, Howell T. The association of individual and facility characteristics with psychiatric hospitalization among nursing home residents. Int J Geriat Psychiat 2009; 24: 261-268.
5. Cadena SV. Living among strangers: the needs and functioning of persons with schizophrenia residing in an assisted living facility. Iss Ment Health Nurs 2006; 27: 25-41.
6. De Girolamo G, Bassi M. Residential facilities as the new scenario of long-term psychiatric care. Curr Opin Psychiat, 2004; 17: 275-281.
7. Cubit K, Farrell G, Robinson A, Myhill M. A survey of the frequency and impact of behaviours of concern in dementia on residential aged care staff. Austral J Ageing 2007; 26: 64-70.
8. Sampson EL, White N, Leurent B et al. Behavioural and psychiatric symptoms in people with dementia admitted to the acute hospital: prospective cohort study. Brit J Psychiat 2014; 205: 189-196.
9. Cherubini A, Eusebi P, Dell’Aquila G, et al. Predictors of hospitalization in Italian nursing home residents: the U.L.I.S.S.E. project. J Am Med Direct Assoc 2012; 13: 84.e5-84.e.10.
10. Collet J, de Vugt, ME, Verhey F, Schols J. Efficacy of integrated interventions combining psychiatric care and nursing home care for nursing home residents: A review of the literature. Int J Geriat Psychiat 2010; 25: 3-13.
11. Nejtek VA, Hardy S, Hall JR, Winter, AS. Characteristics and psychosocial predictors of psychiatric emergency centre transport and length of stay in patients with dementia and Alzheimer’s Disease: A preliminary report. J Psychiat Prac 2011; 17: 251-257.
12. Clemson L, Kendig H, Mackenzie L, Browning C. Predictors of injurious falls and fear of falling differ: An 11-year longitudinal study of incident events in older people. J Aging Healt 2015; 27: 239-256.
13. Bunn F, Dickinson A, Simpson C, et al. Preventing falls among older people with mental health problems: a systematic review. BioMedCent Nurs 2014; 13:4.
14. Sinclair C, Boyd K, Sinnott H. Advanced practice nurses in Melbourne’s hospitals: clinical coordinators in a rapid assessment medical unit. Austral J Ad Nurs 2003; 21: 42-46.
15. Australian Government Department of Health. 2006 Pathway of recovery: Preventing further episodes of mental illness.http://health.gov.au/internet/publications/publishing.nsf/Content/mental-pubs-p-mono-toc-mental-pubs-p-mono-ref Accessed 1 May 2016
16. NSW Health. Your Guide to MH-OAT: Clinicians Reference Guide to NSW Mental Health Outcomes and Assessment Tools. 2004. NSW Department of Health, North Sydney.
17. King C, Lakshimi NP, Voruganti, MD. What’s in a name: The evolution of the nomenclature of antipsychotic drugs. Rev Psychiatr Neurosci 2002; 27:168-175.
18. Australian Government Department of Social Services 2016. Aged Care Funding Instrument (ACFI) reports: https://www.dss.gov.au/our-responsibilities/ageing-and-aged-care/tools-and-resources/aged-care-funding-instrument-acfi-reports Accessed 1 April 2016
19. Jorm AF. Mackinnon AJ. Psychogeriatric Assessment Scales User’s Guide 3rd edn. 1995. ANUTECH Pty Ltd, Canberra.
20. Alexopoulos GS, Abrams RC, Young RC, Shamoian CA. Cornell Scale for Depression in Dementia. Biol Psychiat 1998; 23: 271-284.
21. Australian Government Department of Health and Ageing. Aged Care Funding Instrument (ACFI). Assessment Pack. 2007. Commonwealth of Australia, Canberra.
22. Cleeland CS, Ryan KM. Global use of the Brief Pain Inventory. Ann Acad Med Sing 1994; 23: 129-138.
23. National Ageing Research Institute. Falls Risk Assessment: Residential Care. 2003. Melbourne Health: Melbourne
24. Waldron N, Hill A, Barker A. Falls prevention in older adults: Assessment and management. Austral Fam Phys 2012; 41: 930-935.
25. Kearney FC, Harwood RH, Gladman J, Lincoln N, Masud T. The relationship between executive function and falls and gait abnormalities in older adults: A systematic review. Dem Geriat Cog Dis, 2013; 36: 20-25.
26. Mehta S, Chen H, Johnson ML , Aparasu, RR. Risk of falls and fractures in older adults using antipsychotic agents: a propensity-matched retrospective cohort study. Drugs Aging, 2010; 27: 815-829.
27. Snowdon, J, Rosengren D, Daniel F, Suyasa M Australia’s use of the Cornell scale to screen for depression in nursing homes. Austral J Ageing, 2011; 31: 33-36.
28. Davison T, Snowdon J, Castle N, et al. An evaluation of a national program to implement the Cornell Scale for Depression in Dementia into routine practice in aged care facilities. Int Psychogeriat 2012; 24: 631-641.
29. Takai Y, Yamamoto-Mitani N, Okamoto Y, Koyama K, Honda A. Literature review of pain prevalence among older residents of nursing homes. Pain Manag Nurs, 2010; 11: 209-223.
30 Fleming R, Purandare N. Long-term care for people with dementia: environmental design guidelines, Int Psychogeriat, 2010; 22: 1084-1096.