S. FIEN1, M. CLIMSTEIN2,3, T. HENWOOD4,1, E. RATHBONE1, J.W.L. KEOGH1,5,6
1. Faculty of Health Science and Medicine, Bond University, Robina, QLD, Australia; 2. Water Based Research Unit, Faculty of Health Sciences, Bond University, Gold Coast, QLD, Australia; 3. Exercise, Health and Performance Faculty Research Group, The University of Sydney, NSW, Australia; 4. Southern Cross Care, North Plympton, SA, Australia; 5. Human Potential Centre, AUT University, Auckland, New Zealand; 6. Cluster for Health Improvement, Faculty of Science, Health, Education and Engineering, University of the Sunshine Coast, Sippy Downs, QLD, Australia. Corresponding author: Samantha Fien, Faculty of Health Science and Medicine, Bond University, Robina, Australia, 4229, Ph. 0402479015, Fax: +617 5595 3524, E. samantha.fien@student.bond.edu.au
Jour Nursing Home Res 2017;3:81-87
Published online August 11, 2017, http://dx.doi.org/10.14283/jnhrs.2017.13
Abstract
Background: Falls, wounds and hospitalisation are serious adverse events that may result in reduced independence and quality of life, and contribute to higher risks of disability and death in nursing homes. Objectives: To quantify the incidence of events (falls, hospital admissions and wounds) in nursing home residents and to determine if gait speed thresholds can predict falls. Design: A prospective cohort design was used to estimate the incidence and types of adverse events. Setting: Three nursing homes on the Gold Coast/Northern New South Wales, Australia. Participants: 100 nursing home adults consented to participate in this project. Measurements: The primary outcome included the number of adverse events (falls, wounds and hospital admissions) accessed through the nursing homes records. We used negative binomial regression models adjusted for potential confounders to examine associations between gait speed group and falls suffered by residents in nursing home settings, and we reported incidence rate ratios (IRRs) with 95% CIs and the actual P-value. Results: During the six months, there were a total of 226 falls, 243 wounds, 65 hospital admissions and 29 deaths with 12% of the residents having a fall(s), wound, admitted to hospital and dying in the 6-month period. Gait speed was not a statistically significant factor that impacted adverse events. However, for every additional hospital admission there was a 28% increased rate of falling, for every additional wound there was a 7.8% increased rate of falling and for every kilogram increase in handgrip strength there was a 4.4% increase rate of falling. Residents were also found to have an increased rate of falling if they were female (65.5%) and a decreased rate of falling with a positive impairment Mini-Cog score residents were likely to have a 52% decrease in their rate of falling when compared with negative cognitive impairment. Conclusion: The incidence of adverse events in Australian nursing homes is high, suggesting that continual refinement of assessment, education, awareness and management processes are required to improve resident outcomes. In particular, falls reduction interventions appear important, as they would likely reduce the number of hospital admissions and wounds in the nursing home setting.
Key words: Adverse events, falls, hospitalisation, nursing homes, wounds.
List of Abbreviations: ADL: Activities of Daily Living; CI: Confidence interval; EWGSOP: European Working Group on Sarcopenia in Older People; IRR: Incidence Rate Ratio; Mini-Cog: Mini-Cognitive test; SARC-F: Sarcopenia Five-Item Questionnaire.
Introduction
With an ageing population and rising life expectancy rates, older adults are likely to move into nursing homes as their physical and/or cognitive function declines. Falls, hospitalisation and wounds are serious problems that result in higher risks of disability, loss of independence, reduced quality of life and mortality in nursing homes (1).
These adverse events are also proving to become very costly with falls being the leading cause of injury-related hospitalisation in adults aged 65 years or older. In those aged 85 years and over, 4% of men and 7% of women are admitted to hospital annually as result of a fall (2). As a result, the cost of falls is expected to rise to $1.4 billion in Australia by 2051. Thus, continual improvements in fall prevention programs are required in order to reduce the falls incidence rate or additional strain on the health expenditure will incur (3). One component of the high costs of falls is the need for hospital beds. In 2010, there were 240,000 hospital bed days per year related to falls in Australia, with this expected to nearly double to 450,000 hospital bed days by 2051 (2).
To the authors’ knowledge, little research has investigated the incidence of adverse events specific to falls, wounds and hospital admissions in Australian nursing home adults. A recent document on adverse events in Australian nursing home residents is a 2014-15 Australian Government report which has provided insight into older adults in hospital, however there appears to be a lack of peer-reviewed research that focuses purely upon nursing home settings (4). Residents often have multiple chronic diseases, a sarcopenic status and take multiple prescribed medications, with the interaction of these factors placing the residents at a high risk of adverse events (5, 6). Ironically, residents of nursing homes are among the least researched older adult group even though they have the highest rates for falls and hospital admissions and are among the highest consumers for prescribed medications (5).
A recent systematic review has indicated that a significant predictor of adverse events including mobility disability, cognitive decline, mortality, falls and institutionalisation for community-dwelling older adults (aged 65 and older) was low gait speeds (7). In 2012, Sterke et al. (8) sought to extrapolate the findings for community dwelling older adults to those in nursing homes by examining whether gait speed was a significant predictor of short-term falls risk in 57 nursing home residents with moderate to severe dementia in the Netherlands. Sterke et al. (8) conducted a longitudinal study and assessed the gait performance of the nursing home residents with a computer-interfaced instrumented pressure mat every three months for a period of 15 months. A reduced gait speed (OR = 1.22; 95% CI 1.04 – 1.43) and reduced mean stride length (OR = 1.19; 95% CI 1.03 – 1.40) were the strongest gait predictors for falling within three months (8). Knowing this, we wanted to investigate if in the Australian context gait speed could predict adverse events in six months with nearly double the amount of participants. Such a study would appear warranted as Keogh et al. (9) reported that a randomly selected sample of 100 nursing home resident’s mean (SD) walking speed was 0.37 (0.26) m/s, a value substantially less than a recent meta-analyses of 34 studies that reported the nursing home residents’ mean walking speeds to be 0.48 m/s (95% CI 0.40 – 0.55) (10). As very few studies have used gait speed to predict adverse events in nursing home residents, additional research utilising functional performance tasks such as gait speed to predict adverse events in Australian nursing homes appears warranted.
The primary aim was to quantify incidence of adverse events in Australian nursing home residents over a period of six months. The secondary aim was to determine if gait speed thresholds could predict the frequency of falls in nursing home residents. We hypothesized that the incidence of adverse events (i.e. falls) in Australian nursing home residents would be greater than what is commonly reported for community dwelling older adults and that gait speed thresholds could predict falls in Australian nursing home residents.
Methods
Study Participants
A prospective cohort design was used to estimate the incidence and types of adverse events experienced by 100 residents in nursing home settings for six months.
Participants were eligible for inclusion if they were: (i) aged 65 years and over, (ii) residing in a nursing home facility, (11) able to self-ambulate with or without a walking aid and (iv) could provide informed consent. The exclusion criteria included: (i) end-stage terminal and/or life expectancy <6-months (ethical reasons), (ii) two person transfer or increased falls risk during ambulation, (11) unable to communicate or follow instructions (personal needs beyond the scope of this project) and (iv) behaviours that would endanger the participant or research staff.
All participants were approached personally about participation and given the opportunity to ask questions or raise concerns about the study. A total of 100 participants supplied informed consent and took part in the study whereby the primary investigator was responsible for observing and administering all of the testing.
Recruitment and Study Design
Three nursing homes from Northern NSW/Gold Coast were approached and recruited for participation via telephone and email. A meeting was arranged with the facility Service Manager at each site; following an explanation of the procedures, purposes, benefits and associated risks of the study, potential participants were identified with the Service Manager. The primary investigator went and visited all potential participants and explained the procedures, purposes, benefits and associated risks of the study, participants also had the opportunity to ask questions. A total of 100 residents (66 females and 34 males), aged between 66 and 99, with mean (SD) 85.5 (7.2) years, provided written informed consent for the study. The final sample obtained was a convenience sample from all three nursing homes. Participant recruitment and assessment occurred over a nine-month period.
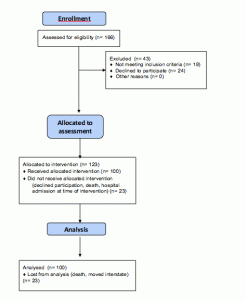
The flow of recruitment to assessment is represented in Figure 1. Ethical approval for this study was attained from the University Human Ethics Research Committee (RO 1823) and gatekeeper’s approval obtained through the nursing homes.
Adverse Events
Adverse events were defined by the World Health Organisation (12) as an injury caused by medical management or complication rather than by the underlying disease itself, and one that results in either prolonged healthcare, or disability at the time of discharge from care, or both (12). Adverse events (falls, wounds, hospital admissions and deaths) information was collected by the nursing home staff and nurses, for a total of six months post gait speed assessment. A fall was defined as unintentionally coming to rest on the ground, floor, or other lower level (13). Hospital admission was defined as an individual who met the criteria for admission to the hospital category and care type, and underwent a hospital’s admission process (documented) to receive treatment and/or care for a period of time – minimum four hours for medical admissions (4). Wounds were defined as the result of tissue damaged by trauma. This may be deliberate, as in surgical wounds of procedures, or due to accidents caused by blunt force, projectiles, heat, electricity, chemicals or friction (14).
Gait
The GaitMat II system measured the participants gait speed as they walked across a level pressure mat system that was 3.66 m (11.91 ft.) long (15). Three trials were completed at the participants’ habitual speed, with the following instructions provided to the participants, “Walk towards the end of the room in the centre of the mat at a pace that is comfortable for you”. An extra 2 m (6.56 ft.) platform was included on both ends of the GaitMat II in order to reduce the effect of acceleration or deceleration (16, 17). Participants were allowed as much rest as required between attempts, with rest periods typically being up to one minute. For safety reasons, all participants wore their own preferred footwear or walked barefoot and were spotted by the primary researcher who followed each participant with the average gait speed used for data analysis.
Other Measures
In addition, handgrip strength, the Mini-Cog test (18) and SARC-F questionnaire (19, 20) were collected for the purpose of cohort characteristics description. Nursing home facility records provided other relevant descriptors including the number of medical conditions and prescribed medications for each resident.
Data Management and Statistical Analysis
Three gait speed thresholds were defined; (i) ≥0.8 m/s; (ii) 0.61 to 0.79 m/s; ≤0.6 m/s. Baseline categorical variables like gender and gait speed group were tested using chi-square tests to determine if these characteristics were similar in the three nursing homes. Frequencies were reported for categorical variables. All continuous data were initially checked for normality prior to analysis. As data were normally distributed, descriptive statistics are presented as mean and standard deviations for continuous variables. A one-way ANOVA and post-hoc Tukey and Scheffe tests were performed to determine if statistically significant differences existed between the three nursing home facilities.
The results for falls were reported when it comes to finding a relationship between gait speed and an adverse event. Chi-square and logistic regressions were conducted to examine the relationships between gait speed and other adverse events but these did not turn out to be statistically significant.
The total number of cases of adverse events were computed, as well as the incidence as reflected by the number of residents who suffered an adverse event, out of 100 residents at risk. The counts and percentages who suffered an adverse event were also calculated by gait speed group.
A Poisson regression was run to predict the number of falls in nursing home in the last six months based on the gait speed group and the number of hospital admissions within those six months. However, the data were over dispersed and a negative binomial regression with custom parameter was performed to correct for over dispersion.
For the number of falls in the time frame of six months, we report incidence rate ratios (IRRs) with 95% CIs and the actual P-value (21). All data were analysed using SPSS statistic software (version 22) with statistical significance set at p<0.05 a priori.
Results
Participants
One hundred of the 166 (60.2%) invited, eligible adults were recruited to the study. There were no significant differences between all variables for the three nursing home cohorts in this study (P>0.05), thus the data was combined into one group for analysis. Table 1 summarises the characteristics of study participants. The average age of study participants was 85.5 (SD: 7.2) years old. The majority of participants were female (66%) and 29 deaths (15 females) occurred during the 6-month period with the average age being 85.3 (SD: 6.5) years ranging from 79 to 97 years at the time of death. The residents took an average of 14.0 (SD: 5.8) medications and had a total of 11.0 (SD: 4.9) medical conditions.
Many of the 100 participants experienced adverse events during the six months of data collection (refer to Table 2). Of the 100 participants, 73 fell during the follow-up period with 24 falling once and 49 falling two or more times. One third of the residents fell between 8:00 am and 3:59 pm (33%). Forty-two residents were admitted to hospital with the majority of these individuals (29 residents, 69%) being hospitalised once in the six-month period. The numbers of days in hospital ranged from 1 to 30 days. There were 45 residents who received treatment for wounds. The majority, (79%, n = 79) of residents had a low gait speed according to European Working Group on Sarcopenia in Older People (EWGSOP) criteria (22) that was characterized as normal (< 0.80 m/s) and 26% (n = 26) ambulated below the mean reported for nursing home residents in the local area (< 0.37 m/s) (9).
* SARC-F = Sarcopenia Five-Item Questionnaire
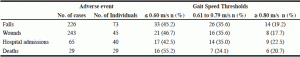
Table 2
Adverse events by gait speed thresholds after a period of six months in 100 nursing home residents
A negative binomial regression was run to predict the number of falls in nursing homes in a six-month follow up based on their baseline gait speed. Specifically, the residents were categorised into one of three gait speed groups: ≤0.6 m/s, 0.61 – 0.79 m/s and ≥0.80 m/s. The gait speed threshold of ≥0.80 m/s was used as the reference group. The results of univariable regression analyses (Table 3) indicated that hospital admissions (IRR = 1.34, 95% CI 1.11 – 1.62, P = 0.002), wounds (IRR = 1.10, 95% CI 1.03 – 1.17, P = 0.004), SARC-F (IRR = 1.07, 95% CI 1.00 – 1.15, P = 0.062), handgrip strength (IRR = 1.07, 95% CI 1.02 – 1.12, P = 0.005) and Mini-Cog (IRR = 0.59, 95% CI 0.36 – 0.97, P = 0.037) were statistically significant predictors of falls at the 0.10 significance level. In contrast, gait speed thresholds (below or equal to 0.6 m/s and 0.61 – 0.79 m/s) were not statistically significant predictors of falls in nursing homes residents (P = 0.379 and P = 0.297, respectively).
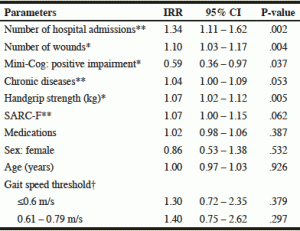
Table 3
Univariable negative binomial regression model (IRRs with 95% CIs) to predict the number of falls over six months in 100 nursing home residents
* = Statistically significant P<0.05. ** = Statistically significant P<0.1.; † = Reference group is gait speed ≥0.80 m/s; IRR = Incidence Rate Ratio; CI = Confidence Interval
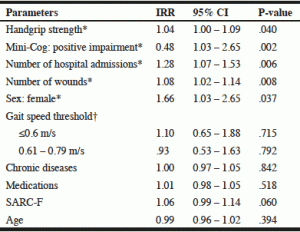
Table 4
Multivariable negative binomial regression model (IRRs with 95% CIs) to predict the number of falls over six months in 100 nursing home adults
* = Statistically significant P<0.05. † = Reference group is gait speed ≥0.80 m/s. IRR = Incidence Rate Ratio; CI = Confidence Interval
Variables that were significantly associated with a fall at the 0.10 significance level (hospital admissions, wounds and Mini-Cog) were included in a multivariable regression model, and adjusted for other covariates including age, sex and gait speed group. Results of the multivariable regression are provided in Table 4. These results indicated that hospital admissions (IRR = 1.28, 95% CI 1.07 – 1.53, P = 0.006), wounds (IRR = 1.08, 95% CI 1.02 – 1.14, P = 0.008), handgrip strength (IRR = 1.04, 95% CI 1.00- 1.09, P = 0.040), sex: female (IRR = 1.66, 95% CI 1.03 – 2.65, P = 0.037) and Mini-Cog (IRR = 0.48, 95% CI 1.03 – 2.65, P = 0.002) were statistically significant predictors of falls. Hence for every unit increase in hospital admissions, the incidence rate (or rate of falls) increases by 28%, for every unit increase in wounds; the incidence rate of falls increases by 7.8% and for every additional kilogram increase in handgrip strength the incidence rate of falls increases by 4.4%. Residents who were female had an increased risk of falling by 65.5% compared to males; residents were found to have a 51.7% decrease in the rate of falling if they scored a Mini-Cog score of positive impairment. Age, gait speed thresholds below and/or under 0.6 m/s and 0.61 – 0.79 m/s, SARC-F score, number of chronic diseases and number of medications were not statistically significant and thus did not influence the rate of falling.
Discussion
The present study reported that over a period of six months, a sample of 100 nursing home residents experienced a total of 226 falls, 243 wounds, 65 hospital admissions and 29 deaths. The rate of these adverse events happening within nursing homes appeared substantially greater than what is reported for community dwelling older adults (7).
The frequency of these adverse events provides an ongoing challenge in the nursing home setting. For example, the rate of falls in nursing home males were seven times higher than those living in the community in 2009-10; whilst the equivalent comparison for females was five times higher (5). The results of the current study and findings reported within the literature for older adults (23, 24) show that females may be 65.5% more likely to fall than compared to males; suggesting that females should be the focus of fall prevention programmes in nursing homes.
In Australia, Everett and Powell (25) found skin tears constituted 41% of known wounds amongst a nursing home that contained 347 residents (with an average age of 80 years) with an average of 22 skin tears occurring each month. During the six months of the current prospective study, 45% of residents experienced a wound, higher than that of Everett and Powell which had 38% of residents experiencing a skin tear in six months (25). Wounds experienced by up to 50% of residents in nursing home settings is a major concern due to the associated link of pain, risk of infection, decreased functional ability and poor quality of life (26). Thus, wounds needs to be recognised as a major health issue in nursing homes due to residents having a high risk of suffering from wounds such as skin tears, pressure ulcers and chronic leg ulcers (27).
In regards to hospital admissions, older adults accounted for 41% of Australian patients admitted into hospital in 2014-15 (4). In particular, a growing concern is that the number of older adults (aged 85 years and older) admitted into hospital each year (5.8%) is higher than the population growth for this age group (4.1%) (4). It has also been highlighted that adverse events such as falls and wounds may lead to longer hospital stays and may even contribute to in-hospital deaths (28). In 2009-10, approximately one in five falls that resulted in hospitalisation were reported to have occurred in a nursing home setting (5). Further findings suggest that the rates of fall-related injury cases in nursing homes remain nearly six times higher than community-dwelling adults (29-31).
In contrast to findings in several other studies (32, 33), we found that those residents who were classified as having a positive cognitive impairment in the Mini- Cog score had a 51.7% reduction in falling when compared to those who scored a negative cognitive impairment score. While such a result was initially unexpected, this may reflect a fact that residents who are classified as being cognitively impaired are more closely monitored by nurses and staff and require more assistance (i.e. assisted transfer walking to dinner table) when compared to those who are not cognitively impaired.
The substantially greater rate of adverse events in nursing home than community dwelling settings for older adults is not an unexpected finding. However it does continue to raise the question of how to minimise the incidence and severity of these events in the nursing home facilities. One factor that may be implicated in this number of adverse events in nursing home facilities is the age of the residents (85.7, SD: 7.1 years), number of medical conditions (11.0, SD: 4.9) and number of prescribed medications (14.0, SD: 5.8). Currently, two thirds of Australians aged over 75 years take five or more prescribed medications, an outcome referred to as “polypharmacy”. Depending upon the setting and definition used, 20-70% of older adults use at least one medication that is either harmful or unnecessary (34), with polypharmacy increasingly becoming the norm in nursing home settings. Unfortunately; polypharmacy has been shown to increase the risk of medication errors, falls, confusion, frailty, loss of independence, hospitalisation and mortality (34). As age is a non-modifable risk factor for falls, reductions in polypharmacy and/or number of medical conditions may reduce these adverse effects. Non-pharmacological approaches such as exercise programs involving progressive resistance, balance and/or cardiovascular exercise may provide such benefits (34, 35).
Another approach that may assist nursing home staff reduce the severity and incidence of these adverse events is to screen their residents based on factors that are predictive of these adverse events. Prior to conducting the study, one such simple factor to screen nursing home residents was gait speed. This approach was based on a systematic review in community-dwelling older adults (aged 65 and older) that indicated low gait speed was a significant predictor of a range of adverse events, including mobility disability, cognitive decline, mortality, falls and institutionalisation in community dwelling adults (7). The potential use of gait speed to predict adverse events in nursing home residents was also supported by Sterke et al. (8) who identified reduced gait speed and stride length as significant predictors of falls over the following three months for a group of 57 nursing home residents with dementia.
As a result of the over-dispersion identified in the initial Poisson analysis, the best approach according to the nature of the data was a negative binomial regression analysis to further examine the relationship between potential risk factors and falls in our sample.
Our multivariable analysis found that for every additional hospital admission, the incidence rate (or rate of falls) increases by 28%; for every additional wound, the incidence rate of falls increases by 7.8% and for every additional kilogram increase in handgrip strength the incidence rate of falls increases by 4.4%. Residents who were female had an increased risk of falling by 65.5% when compared to males. Residents who scored a positive impairment on the Mini-Cog had a reduced rate of falls by 51.7% compared with those who were negatively impaired. Such results suggest that continuing improvements in fall prevention programs are required in the Australian nursing home context so to minimise the high social, economic and care burden associated with falls-related hospitalisation and wound care. As suggested in a recent meta-analysis by Lee and Kim (36), to prevent these adverse outcomes from occurring programs that combine exercise and fall interventions that challenge balance should be targeted at high and low falls risk older adults in nursing home facilities.
Study Limitations
Some limitations must also be acknowledged. Due to the study being conducted in a small geographical area within Australia, the results may not be generalizable to other parts of the world. Additionally, in contrast to Sterke et al. (8) who quantified gait speed every three months over a period of 15 months, the present study only assessed gait speed at the beginning of the six-month follow-up.
Conclusion
This study identified the high incidence of adverse events in regards to falls, wounds and hospital admissions in Australian nursing home residents over a period of six months. To reduce the frequency and/or severity of these adverse outcomes, population-based intervention programs should be targeted at the population at risk. As the number of hospital admissions, wounds and handgrip strength increases the risk of falls, with females and Mini-Cog scores classifying positive cognitive impairment with a decrease rate of of falling, a combination of exercise and fall interventions that challenge balance should be targeted to reduce falls in older adults in nursing home facilities. This is especially important for the residents for whom the nursing staff may consider to be at lower risk of falls (those with higher strength and cognitive function). These higher functioning residents may be more physically active and monitored less closely than those with reduced strength and cognitive function. Thus, additional research is needed to better understand the mechanisms underlying our results; with the implication being that different approaches may be needed to minimise the risk of adverse falls-related events in higher and lower functioning nursing home residents.
Acknowledgments: We would like to thank the management, staff and residents of the nursing home settings for their assistance and participation in this project.
Funding: There was no funding attained to conduct this research study.
Conflict of Interest: The authors of this publication declare no conflicts of interest.
Ethical Standard: Permission to conduct this study was granted by the University Human Ethics Research Committee and respective gatekeepers at the nursing home settings.
References
1. Pagan M, Trip H, Burrell B, & Gillon D. Wound programmes in residential aged care: a systematic review. Wound Practice and Research. 2015;23(2).
2. Australian Government. Aged care in Australia: Part I – policy, demand and funding CEPAR research brief. 2014;ARC Centre of Excellence in Population Ageing Research(Date Published 10th April 2014).
3. Tariq H, Kloseck M, et al. An exploration of risk for recurrent falls in two geriatric care settings. BMC Geriatrics. 2013;13(106).
4. Australian Institute of Health and Welfare. Admitted patient care 2014-15: Australian hospital statistics. Health services series no 68. 2016;Cat. no. HSE 172.:Canberra: AIHW.
5. Australian Institute Health and Welfare. Hospitalisations due to falls by older people, Australia 2009-10. Injury research and statistics series no. 70. Canberra: AIHW. 2013;Cat. no. INJCAT 146.
6. Sluggett JK, Ilomaki J, Seaman KL, Corlis M, & Bell JS. Medication management policy, practice and research in Australian residential aged care: current and future directions. Pharmacol Res. 2017;116:27-35.
7. Abellan Van Kan G, Rolland Y, Andrieu S, Bauer J, Beauchet O, Bonnefoy M, et al. Gait speed at usual pace as a predictor of adverse outcomes in community-dwelling older people an international academy on nutrition and aging (IANA) task force. JNHA: Clinical Neurosciences. 2009;13:881-9.
8. Sterke CS, van Beeck EF, Loonman CWN, Kressig RW, van der Cammen TJM. An electronic walkway can predict short-term fall risk in nursing home residents with dementia. Gait Posture. 2012;36(1):95-101.
9. Keogh JW, Senior H, Beller EM, Henwood T. Prevalence and risk factors for low habitual walking speed in nursing home residents: an observational study. Arch Phys Med Rehabil. 2015;96(11):1993-99.
10. Kuys SS, Peel NM, Klein K, Slater A, Hubbard RE. Gait speed in ambulant older people in long term care: a systematic review and meta-analysis. JAMDA. 2013:1-7.
11. Judge JO, Davis RBI, & Ounpuu S. Step length reductions in advanced age: the role of ankle and hip kinetics. J Gerontol A Biol Sci Med Sci. 1996;51:M303-M12.
12. Brennan TA, Leape LL, Laird NM, Hebert L, Localio AR, Lawthers AG, et al. Incidence of adverse events and negligence in hospitalized patients: results of the harvard medical practice study I. N Engl J Med. 1991;324(6):37-376.
13. Lamb SE, Jorstad-Stein EC, Hauer K, & Becker C. Development of a common outcome data set for fall injury prevention trials: the prevention of falls network europe consensus. J Am Geriatr Soc. 2005;53:1618-22.
14. Ashton J, Morton N, Beswick S, Barker V, Blackburn F, Wright C, et al. Wound care guidelines. Primary Care Trust, Bolton NHS. 2008.
15. McDonough AL, Batavia M, Chen FC, Kwon S, Ziai J. The validity and reliability of the GAITRite system’s measurements: a preliminary evaluation. Arch Phys Med Rehabil. 2001;82(3):419-25.
16. Kressig RW, Gregor RJ, Oliver A, Waddell D, Smith W, O-Grady M, et al. Temporal and spatial features of gait in older adults transitioning to frailty. Gait Posture. 2004;20(1):30-5.
17. Fien S, Henwood T, Climstein, M., & Keogh, J. W. L. Feasibility and benefits of group based exercise in residential aged care adults: a pilot study for the GrACE programme. PeerJ. 2016;4:e2018(eCollection 2016).
18. Borson S, Scanlan JM, Watanabe J, Tu SP, Lessig M. Improving identification of cognitive impairment in primary care. Int J Geriatr Psychiatry. 2006;21(4):349-55.
19. Malmstrom TK, & Morley JE. SARC-F: A simple questionnaire to rapidly diagnose sarcopenia. JAMDA. 2013;14(8):1-2.
20. Cao L, Chen S, Zou C, Ding X, Gao L, Liao Z, et al. A pilot study of the SARC-F scale on screening sarcopenia and physical disability in the Chinese older people. J Nutr Health Aging. 2014;18(3):277-83.
21. Huang AR, Mallet L, Rocherfort CM, Euguale T, Buckeridge DL, & Tamblyn R. Medication –related falls in older people: causative factors and management. Drugs Aging. 2012;29(5):359-76.
22. Cruz-Jentoft AJ, Baeyens JP, Bauer JM, Boirie Y, Cederholm T, Landi F, et al. Sarcopenia: European consensus on definition and diagnosis: report of the European Working Group on Sarcopenia in Older People. Age Ageing. 2010;39(4):412-23.
23. Wei F, Hester AL. Gender difference in falls among adults treated in emergency departments and outpatient clinics. J Gerontol Geriatric Res. 2014;3:152.
24. Gale CR, Cooper C, Sayer AA. Prevalence and risk factors for falls in older men and women: the english longitudinal study of ageing. Age and Ageing. 2016;45:789-94.
25. Edwards H, Finlayson K, Shuter P, Parker C, Jensen R, & Finlayson K. Improving wound management for residents in residential age care facilities: national dissemintation and implementation of the evidence based champions for skin integrity program EBPAC – Champions for Skin Integrity National Dissemination Project (EBPAC-CSI Stage 2) 2015.
26. Anand SC, Dean C, Nettleton R, & Praburaj DV. Health-related quality of life tools for venoud-ulcerated patients. Br J Nurs. 2003;12(1):48-59.
27. Edwards H, Chang A, & Finlayson K. Creating champions for skin integrity: final report Queensland, University of Technology: Brisbane 2010.
28. Szlejf C, Farfel JM, Curiati JA, de Barros Couto Junior E, Jacob-Filho W, & Azevedo RS. Medical adverse events in elderly hospitalized patients: a prospective study. Clinics. 2012;67(11):1247-52.
29. Gibson RE, Harden M, Bylesm J., & Ward J. Incidence of falls and fall-related outcomes among people in aged-care facilities in the lower-hunter region, NSW. New South Wales Public Health Bulletin. 2008;19:166-9.
30. Bradley C. Hospitalisations due to falls by older people, Australia 2008-09. Injury research and statistics series no. 62. Canberra: AIHW. 2012b;Cat. no. INJCAT 138.
31. Bradley C, & Pointer S. Hospitalisations due to falls by older people, Australia 2006-07. Injury research and statistics series no. 57. Canberra: AIHW. 2012;Cat. no. INJCAT 133.
32. Muir SW, Gopaul K, Montero-Odasso M. The role of cognitive impairment in fall risk among older adults: a systematic review and meta analysis. Age and Ageing. 2012;41:299-308.
33. Nazir A, Muelle C, Perkins A, Arling G. Falls and nursing home residents with cognitive impairment: new insights into quality measures and interventions JAMDA. 2012;13(9):819.e1-.e6.
34. National Stakeholders. Outcome statement: national stakeholders’ meeting on quality use of medicines to optimise ageing in older australians National Stakeholders Meeting: Quality Use of Medicines to Optimise Ageing in Older Australians. 2016.
35. Bird M-L, Pittaway JK, Cuisick I, Rattray M, Ahuja KDK. Age-related changes in physical fall risk factors: results from a 3 year follow-up of community dwelling older adults in Tasmania, Australia. Int J Environ Res Public Health. 2013;10:5989-97.
36. Lee SH, & Kim HS. Exercise interventions for preventing falls among older people in care facilities: a meta-analysis. Worldviews Evid Based Nurs. 2016;14(1):74-80.