J. Chrusciel1, S. Zid1, V. Suissa2, A. Letty3, P.-E. Hay3, D. Armaingaud3, M. Dramé4, L. Godaert5, S. Sanchez1
1. Centre Hospitalier de Troyes, Public Health Department, Troyes, France; 2. Université Paris 8, Laboratoire de Psychopathologie et Neuropsychologie, Paris, France; 3. Fondation Korian pour le Bien Vieillir, Paris, France; 4. CHU de Martinique, CIC 1424 Antilles Guyane, Fort-de-France, France; 5. CHU de Martinique, Pôle de Gériatrie Gérontologie, Fort-de-France, France. Corresponding author: Jan Chrusciel, MD, MSc, Centre Hospitalier de Troyes, Public Health Department, Troyes, France, Phone : +33 3 25 49 71 19 / Fax + 33 3 25 49 49 50. E-mail: jan.chrusciel@ch-troyes.fr
Jour Nursing Home Res 2020;6:114-119
Published online December 4, 2020, http://dx.doi.org/10.14283/jnhrs.2020.29
Abstract
Background: Entering a NH can represent considerable mental trauma in addition to an increased financial strain. An improved understanding of the psychological issues at play could help professionals to adopt a more empathic attitude. Objectives: the main objective of our study was to identify distinctive profiles of adults aged over 65 in four European countries in order to understand the difficulties associated with the transition to a nursing home. Design: Cross-sectional study and Hierarchical Cluster Analysis. Participants: Retired people from Germany, Belgium, France, and Italy aged 65 or older selected by quota sampling and contacted via an online survey, the Ipsos Poll Institute Access Panel. Methods: Cross-sectional survey. A Principal Components Analysis was performed on the answers to the questionnaire, and clusters were identified by Hierarchical Cluster Analysis using Ward’s method. Measurements: The data was collected using an Internet questionnaire. Results: A total of 4160 subjects aged 65 years or older were selected. Principal component analysis identified six well-defined groups: wealthy homeowners, flexible single people, wealthy Germans, low-income introverts, socially isolated women, Italian homebirds. Conclusions: Understanding the profiles of older Europeans could help healthcare professionals decide how to orient them towards acceptance of their new life in the nursing home.
Key words: Nursing home, successful aging, cross-sectional study, principal components analysis, hierarchical cluster analysis.
Introduction
An estimated 728,000 persons live in the various residential care structures available for older people in France (418,000 in the United Kingdom and 1.5 million in the United States). The risk of entry into a nursing home (NH) has been shown to vary according to geographical and clinical factors (1). Entry into a NH is associated with a state of frailty, and a decrease in the social environment’s ability to provide direct support (2–5), meaning life at home is no longer possible. The problem of caregiver burden is likely to increase in the years to come. The growing number of divorces, a decrease in natality (6) and a higher life expectancy are leading to a reduction in household size, which in turn reduces the potential number of caregivers (7, 8). These changes call for a re-evaluation of the current health policy regarding older people (9). The concept of home covers physical and cognitive entities and is specific to each individual (10). The place where life is lived, one’s home can extend beyond the walls of the house and include relations with loved ones and daily interactions (11). Often, the decision to enter a NH is a default choice, because the person is no longer capable of living independently despite assistance. NH entry is sometimes (12) not anticipated by the person, and often decided by their children and/or spouse. As cognitive impairment predicts entry in the NH (13–15), cognitively impaired patients sometimes do not expect such a transition and can easily be disoriented in the process (16).
Thus, entering a NH can represent considerable mental trauma in addition to an increased financial strain (17, 18). Moreover, this can happen in a context when the patient is experiencing depressive symptoms (19). The older person transitions from a situation where they were in control, to a situation where everything is decided for them by others (20). Therefore, knowledge of the profile of the future resident is important to prevent problems and misconceptions when the transition to a nursing home is nearing.
An improved understanding of the psychological issues at play could help professionals to adopt a more empathic attitude at the early stages of envisioning the transition to a nursing home (21).
Therefore, the main objective of our study was to use an on-line survey to identify clusters of people aged 65 years or older of four European countries based on their characteristics and including their attitudes regarding accommodation.
Materials and Methods
Ethical approval
Patients gave informed consent to take the survey. The survey was exempt from Institutional Review Board approval under the French Public Health law n° 2004-806 (9 August 2004).
Study population
The survey was carried out in February 2016 by a poll institute in a sample of individuals from the population of retired persons in four European countries, selected using quota sampling. A total of 4160 subjects aged 65 years or older were selected. This cross-sectional study was carried out using an internet questionnaire (Appendix 1) sent to the selected individuals in France (n=1000), Belgium (n=1076), Italy (n=1081) and Germany (n=1003). Participants took the online survey from their place of residence, using their personal computer. The reference population selected was diverse in terms of age, including both recently retired persons as well as oldest-old individuals. The characteristics used for the quota sampling method were sex, age, socio-professional category, region, city size, number of persons in the household, autonomy (dependent/independent), marital status, place of residence, income and highest educational qualification. The aims of the survey were also to obtain useful information about the different subgroups of the population (according to age, sex, income etc.).
The Ipsos© Access Panel
The questionnaires were administered via the Access Panel online service belonging to Ipsos Interactive Services©. The Access Panel is a pool of households and individuals spread homogeneously across the whole country and who regularly accept to participate in market research studies. The panel comprises over 600,000 individuals on whom detailed information has been collected in addition to the data used to establish the quotas (e.g. the size of the household, income, level of education, number of children etc.). This methodology aims to achieve adequate representativeness for the different quota. Numerous quality controls were carried out at all stages of the survey.
Quality control procedures
Quality control procedures were implemented at each stage of data collection and all the online sessions were performed using the CONFIRMIT software. This system enables automatic management of how the questionnaire scrolls (guides, filters), eliminates coding errors, displays questions or sub-questions in random order to avoid bias linked to the order of appearance of the items on the questionnaire, and ensures automated control of quotas in real time. This software meets ISO 9001 certification standards (2008 version).
Development of the questionnaire
The questionnaire was developed jointly by the Korian Foundation for Successful Ageing and IPSOS© with the assistance of a sociologist. The questionnaires contained 25 question units. The topics addressed include concepts related to attachment to the home environment. A number of sociodemographic characteristics were also recorded (age, sex, household, income, marital status, level of education). The questionnaire was professionally translated and the accuracy of the translation was confirmed by the investigators in each country.
Statistical analysis
For descriptive analysis, qualitative variables were presented as absolute frequencies with percentages. Questionnaire results were analysed using a Principal Components Analysis (PCA), which was performed based on questions 1,7, 8, 10, 14, 19, 34, 36 as active variables, while socio-demographic variables and questions 1, 3, 7, 8, 10, 11, 14, 19, 21, 24, 25, 33,34, 35, 36, 37,38 were used as illustrative variables. Clusters of residents were identified with Hierarchical Cluster Analysis using Ward’s distance. The analysis was realised using SPAD software.
Results
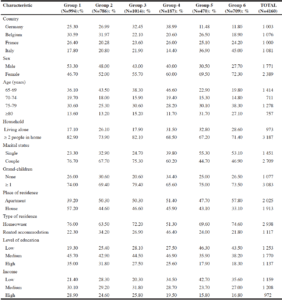
The study population comprised 4160 individuals from Germany, Belgium, France, and Italy. The characteristics of the study population are described in Table 1. Overall, 2389 (57%) were women; 1414 (34%) were aged 65 to 69, and 2709 (65%) were living maritally. A majority (2938, 70%) were homeowners, while 1253 (30%) showed signs of social precariousness including low income, and 1159 (27%) had a low level of education.
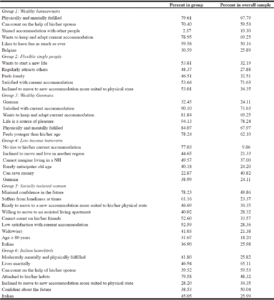
The Principal Components Analysis identified six groups whose main characteristics are described below and in Table 2:
Group 1 (N=994, 23%): well-off males with a high level of education. They were fond of their lodgings, furniture and personal belongings. They enjoyed life and felt confident about the future. This first group mainly preferred to stay at home, adapting their residence to meet their evolving needs rather than sharing accommodation with others.
Group 2 (N=786, 19%): single, flexible and young, with a high proportion of people from Germany and Belgium. Their satisfaction with, and fondness for their residence were of lesser magnitude than in Group 1. They were willing to move to accommodation that was more suitable for their physical capacity. This group was also characterised by loneliness, and less contact with those around them. They were less confident about the future due to a more pronounced anticipation of future dependency.
Group 3 (N=1014, 24%): middle-class people with a well-developed social network, living maritally and able to count on their children. They were happy and satisfied, both physically and mentally. They felt younger than their age. They were independent and lived with a sense of pleasure. As in Group 1, they were fond of their home, their furniture and their habits. This could explain their preference to adapt their current accommodation to their changing needs rather than moving.
Group 4 (N=187, 5%): People of lower income, young, and fragile with less developed networks, these people were less likely to be able to count on their spouse. They were not fulfilled, either mentally or physically. Life was a source of pleasure for only 65% in this group, compared to an average of 78%. In this group, income was lower than average. They often lived in rented accommodation, and were less attached to their residence and their habits. Consequently, they were willing to change accommodation if it meant better living conditions, and 50% would envision living in a NH.
NH: Nursing Home
Group 5 (N=470, 25%): socially isolated women. They had limited financial resources and a low level of education. They suffered from social precariousness, with few friends on whom they could count, and had physical problems that made them dependent (48%). The majority of people in this group did not consider life to be a source of pleasure, and they had less confidence in the future. They would be willing to move houses and region for an accommodation that was more suited to their needs, because they felt little attachment to their furniture, personal belongings and daily habits.
Group 6 (N=709, 17%): fond of their residence, predominantly women (72%) of Italian nationality (45%). This group presented some similarities with Group 5, in that its members were dependent and isolated. People in this group did not feel physically and mentally fulfilled. They could not save money due to their relatively low income. Only 38% of them feel confident about the future. Contrarily to Group 5, they were very attached to their habits, their furniture and their home, and consequently, were not willing to move.
Discussion
We show that there are different typologies regarding participants’ characteristics linked to accommodation and the attitude towards a change of place of living. Young, recently-retired people, living maritally, independent and fond of their routine, were more frequent among Belgian and German respondents. These groups preferred to adapt their accommodation to their changing needs rather than live in a NH. German respondents who had a more precarious social situation than their wealthier counterparts had fewer social links, and their attachment to material belongings and their accommodation was low. They showed a readiness to move or live in a NH if the living conditions were better. German nursing homes are highly regulated and have seen an improvement in quality in the last years (22, 23). Moving into a NH can be a strategy to combat loneliness, although loneliness is also prevalent in nursing homes (24).
People from Italy were well-represented in two profiles: the first comprised mainly socially-oriented individuals who were very fond of their home. Despite difficult living conditions, they preferred to remain at home rather than to live in a NH. This is consistent with cultural expectations in Southern Countries, where social support from the family is the norm (25, 26). The second profile comprised essentially isolated individuals with few social contacts. For these individuals entry into a NH could represent a solution to achieve a better quality of life.
The frequency of females in this cluster is not surprising as European statistics show that older women often live alone (27).
Our results are coherent with previous data published in the literature (28). Social isolation and loneliness can lead physically able-bodied older persons to seek out collective living arrangements, such as assisted living. Our study also reveals geographical specificities, which may be at least partially explained by different policies regarding care of older adults in society between countries in the North versus the South of Europe. In southern European countries such as Italy, the fate of incapacitated older persons depends on the family rather than on institutional solidarity (25), in contrast with northern countries like Germany or Belgium. These findings can be interpreted as evidence that culture and socio-economic factors can influence older adults’ attitude towards their place of residence (29, 30). Other factors also play an important role in a person’s ability to construct a new “home” for themselves in a NH (31). More research is needed to ascertain if the identified profiles can predict adverse outcomes surrounding the transfer to a NH (32).
Our findings also show that living maritally, which was more frequent among Belgian and German people, contributed to a happier and more fulfilling life both mentally (33) and physically. These results are coherent with previous reports that couples are better equipped to deal with household chores than a single person. Furthermore, in case of dependency, the spouse is usually the primary caregiver, thus delaying the need for entry into long-term care (34).
Strengths and Limitations of the study
Our study population comprised a sample of individuals recruited by a poll institute in four European countries. The study sample was relatively large, although it could not be fully representative of the European population of persons aged over 65 years. Respondents needed to have access to the internet, which potentially excludes some of the oldest old and participants with lower levels of education from participating. The cross-sectional nature of the study implies that we could not follow the evolution and outcomes of the identified profiles. We hypothesise that patients who declare being most attached to their residence and their habits will be most impacted when a change is needed. However, the extent to which the profiles identified in this article predict adverse outcomes, mood changes or behavioural problems surrounding entry in the nursing home has not been studied here. People from groups 4 to 6 seem particularly at risk in the period surrounding entry in the nursing home. The available data suggests that suicides often occur in the first year after entry in the nursing home, although it is unclear if anticipation is a substantial risk factor (35). As in the general population, suicide occurs predominantly in males (36).
Conclusions and Implications
Entry into a NH is often experienced as a profound rupture, and this transition should be guided and anticipated. Understanding how the characteristics of older Europeans are linked to their attitude regarding their accomodation is a first step towards helping newly arriving residents to better accept their new life in the NH. The understanding of the psychological factors at stake can create a more empathic attitude by professionals and help to improve integration.
Funding: There is no funding to disclose in connection with this study.
Acknowledgements: N/A
Ethical standards: Patients gave informed consent to take the survey. The survey was exempt from Institutional Review Board approval under the French Public Health law n° 2004-806 (9 August 2004).
Open Access: This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits use, duplication, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license and indicate if changes were made.
References
1. Himes CL, Wagner GG, Wolf DA, Aykan H, Dougherty DD. Nursing home entry in Germany and the United States. J Cross-Cult Gerontol 2000;15:99–118.
2. Gaugler JE, Kane RL, Kane RA, Clay T, Newcomer R. Caregiving and institutionalization of cognitively impaired older people: utilizing dynamic predictors of change. The Gerontologist 2003;43:219–29.
3. Bharucha AJ, Pandav R, Shen C, Dodge HH, Ganguli M. Predictors of nursing facility admission: a 12-year epidemiological study in the United States. J Am Geriatr Soc 2004;52:434–9.
4. Soto ME, Andrieu S, Gillette-Guyonnet S, Cantet C, Nourhashemi F, Vellas B. Risk factors for functional decline and institutionalisation among community-dwelling older adults with mild to severe Alzheimer’s disease: one year of follow-up. Age Ageing 2006;35:308–10. https://doi.org/10.1093/ageing/afj059.
5. Schulz R, Belle SH, Czaja SJ, McGinnis KA, Stevens A, Zhang S. Long-term Care Placement of Dementia Patients and Caregiver Health and Well-being. JAMA 2004;292:961–7. https://doi.org/10.1001/jama.292.8.961.
6. Duée M, Rebillard C. Santé et protection sociale. La dépendance des personnes âgées: une projection en 2040. In: INSEE, editor. Données sociales – La société française. Paris: INSEE; 2006. 613-619
7. Dramé M, Fierobe F, Lang P-O, Jolly D, Boyer F, Mahmoudi R, et al. Predictors of institution admission in the year following acute hospitalisation of elderly people. J Nutr Health Aging 2011;15:399–403.
8. Blanchet D, Debrand T, Dourgnon P, et al. Santé, vieillissement et retraite en Europe. Econ Stat 2007:3–18.
9. Henrard J-C. Le dispositif institutionnel d’aide et de soins aux personnes âgées. Bull Epidémiologique Hebd 2006:45–7.
10. Dahlin-Ivanoff S, Haak M, Fänge A, Iwarsson S. The multiple meaning of home as experienced by very old Swedish people. Scand J Occup Ther 2007;14:25–32. https://doi.org/10.1080/11038120601151714.
11. Oswald F, Schilling O, Wahl H-W, Fänge A, Sixsmith J, Iwarsson S. Homeward bound: Introducing a four-domain model of perceived housing in very old age. J Environ Psychol 2006;26:187–201. https://doi.org/10.1016/j.jenvp.2006.07.002.
12. Lindrooth RC, Hoerger TJ, Norton EC. Expectations among the elderly about nursing home entry. Health Serv Res 2000;35:1181–202.
13. Gaugler JE, Duval S, Anderson KA, Kane RL. Predicting nursing home admission in the U.S: a meta-analysis. BMC Geriatr 2007;7:13. https://doi.org/10.1186/1471-2318-7-13.
14. Hirono N, Tsukamoto N, Inoue M, Moriwaki Y, Mori E. [Predictors of long-term institutionalization in patients with Alzheimer’s disease: role of caregiver burden]. No To Shinkei 2002;54:812–8.
15. Yaffe K, Fox P, Newcomer R, Sands L, Lindquist K, Dane K, et al. Patient and caregiver characteristics and nursing home placement in patients with dementia. JAMA 2002;287:2090–7.
16. Thoma-Lürken T, Bleijlevens MHC, Lexis MAS, de Witte LP, Hamers JPH. Facilitating aging in place: A qualitative study of practical problems preventing people with dementia from living at home. Geriatr Nurs N Y N 2018;39:29–38. https://doi.org/10.1016/j.gerinurse.2017.05.003.
17. Digital technology to enable aging in place. Exp Gerontol 2017;88:25–31. https://doi.org/10.1016/j.exger.2016.11.013.
18. Mezuk B, Lohman M, Leslie M, Powell V. Suicide Risk in Nursing Homes and Assisted Living Facilities: 2003–2011. Am J Public Health 2015;105:1495–502. https://doi.org/10.2105/AJPH.2015.302573.
19. Harris Y, Cooper JK. Depressive symptoms in older people predict nursing home admission. J Am Geriatr Soc 2006;54:593–7. https://doi.org/10.1111/j.1532-5415.2006.00687.x.
20. Mallers MH, Claver M, Lares LA. Perceived Control in the Lives of Older Adults: The Influence of Langer and Rodin’s Work on Gerontological Theory, Policy, and Practice. The Gerontologist 2014;54:67–74. https://doi.org/10.1093/geront/gnt051.
21. Dahany M-M, Dramé M, Mahmoudi R, Novella J-L, Ciocan D, Kanagaratnam L, et al. Factors associated with successful aging in persons aged 65 to 75 years. Eur Geriatr Med 2014;5:365–70. https://doi.org/10.1016/j.eurger.2014.09.005.
22. Kottner J, Dassen T, Lahmann NA. [Pressure ulcers in German nursing homes: frequencies, grades, and origins]. Z Gerontol Geriatr 2011;44:318–22. https://doi.org/10.1007/s00391-011-0179-0.
23. Herr A, Nguyen T-V, Schmitz H. Public reporting and the quality of care of German nursing homes. Health Policy 2016;120:1162–70. https://doi.org/10.1016/j.healthpol.2016.09.004.
24. Trybusińska D, Saracen A. Loneliness in the Context of Quality of Life of Nursing Home Residents. Open Med 2019;14:354–61. https://doi.org/10.1515/med-2019-0035.
25. Uhlenberg P. International Handbook of Population Aging. Springer. New York: 2009.
26. Walker A. A European perspective on quality of life in old age. Eur J Ageing 2005;2:2–12. https://doi.org/10.1007/s10433-005-0500-0.
27. Eurostat. Ageing Europe. Looking at the lives of older peoplein the EU. 2019.
28. Rijnaard MD, van Hoof J, Janssen BM, Verbeek H, Pocornie W, Eijkelenboom A, et al. The Factors Influencing the Sense of Home in Nursing Homes: A Systematic Review from the Perspective of Residents. J Aging Res 2016;2016:1–16. https://doi.org/10.1155/2016/6143645.
29. Brownie S, Horstmanshof L, Garbutt R. Factors that impact residents’ transition and psychological adjustment to long-term aged care: a systematic literature review. Int J Nurs Stud 2014;51:1654–66. https://doi.org/10.1016/j.ijnurstu.2014.04.011.
30. Riedl M, Mantovan F, Them C. Being a Nursing Home Resident: A Challenge to One’s Identity. Nurs Res Pract 2013;2013:1–9. https://doi.org/10.1155/2013/932381.
31. Van Hoof J, Verbeek H, Janssen BM, Eijkelenboom A, Molony SL, Felix E, et al. A three perspective study of the sense of home of nursing home residents: the views of residents, care professionals and relatives. BMC Geriatr 2016;16:169. https://doi.org/10.1186/s12877-016-0344-9.
32. Snowdon J, Day S, Baker W. Why and how antipsychotic drugs are used in 40 Sydney nursing homes. Int J Geriatr Psychiatry 2005;20:1146–52. https://doi.org/10.1002/gps.1407.
33. Murphy B, Kennedy B, Martin C, Bugeja L, Willoughby M, Ibrahim JE. Health and Care Related Risk Factors for Suicide Among Nursing Home Residents: A Data Linkage Study. Suicide Life Threat Behav 2019;49:695–706. https://doi.org/10.1111/sltb.12465.
34. Arnault L, Dartigues J-F, Helmer C, Pérès K, Wittwer J. Do partners of severely disabled elderly protect against nursing home entry? Evidence from a French cohort. J Econ Ageing 2020;15:100207. https://doi.org/10.1016/j.jeoa.2019.100207.
35. Murphy BJ, Bugeja L, Pilgrim J, Ibrahim JE. Completed suicide among nursing home residents: a systematic review: Completed suicide among nursing home residents. Int J Geriatr Psychiatry 2015;30:802–14. https://doi.org/10.1002/gps.4299.
36. Mezuk B, Rock A, Lohman MC, Choi M. Suicide risk in long-term care facilities: a systematic review: Suicide in long-term care. Int J Geriatr Psychiatry 2014;29:1198–211. https://doi.org/10.1002/gps.4142.